Abstract
Introduction
Elderly patients with femoral neck fractures (FNFs) undergoing hemiarthroplasty usually have poor physical condition. The main aim of this study was to identify risk factors for blood transfusion in these patients and construct a nomogram to intuitively predict the requirement of transfusion. The secondary purpose was to examine the relationship between blood transfusion and complications within 30 days post-operatively. Our hypothesis was that chronic kidney disease (CKD) and hypoalbuminemia may increase the requirement of transfusion.
Methods
Data of 414 elderly patients undergoing hemiarthroplasty for FNFs were retrospectively collected. Univariate and multiple regression analysis were performed to identify independent risk factors for blood transfusion, which were used to construct a nomogram subsequently. The discrimination and calibration of the nomogram model were assessed with concordance index (C-index), the area under receiver operating characteristic curve (AUC), and calibration curve. Furthermore, the complications of blood transfusion within 30 days post-operatively were also analyzed.
Results
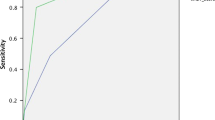
Out of 414 patients, 127 (30.7%) received a blood transfusion. Independent risk factors for blood transfusion included CKD, hypoalbuminemia, pre-operative anaemia, general anaesthesia, higher American Society of Anesthesiologists score, more intraoperative blood loss, and longer surgical time. Increased hidden blood loss, deep vein thrombosis, superficial wound infection, and prolonged hospital stays were more common in transfused patients. The C-index of the nomogram model was 0.848 (95% CI = 0.811–0.885), and the AUC value was 0.859. The calibration curve showed a good consistency between the actual transfusion and the predicted probability.
Discussion
We observed a transfusion rate of 30.7% in elderly FNF patients undergoing hemiarthroplasty. CKD and hypoalbuminemia were firstly identified as independent risk for blood transfusion. In addition, blood transfusion can increase the occurrence of early post-operative complications.
Conclusion
Targeted pre-operative intervention, such as optimizing CKD and correcting hypoalbuminemia is essential and highly regarded.




Similar content being viewed by others
Data availability
The data contributing to this article may be made available upon request by sending an e-mail to the first author.
References
Gullberg B, Johnell O, Kanis JA (1997) World-wide projections for hip fracture. Osteoporos Int 7:407–413. https://doi.org/10.1007/pl00004148
Sircana G, Cauteruccio M, Oliva MS, Piccirillo N, Pesare E, Minutillo F, Ziranu A (2020) Fibrin sealant reduces need for transfusions after hip hemiarthroplasty for femoral neck fractures. Injury 51 Suppl 3:S23-s27. https://doi.org/10.1016/j.injury.2020.05.026
Guo WJ, Wang JQ, Zhang WJ, Wang WK, Xu D, Luo P (2018) Hidden blood loss and its risk factors after hip hemiarthroplasty for displaced femoral neck fractures: a cross-sectional study. Clin Interv Aging 13:1639–1645. https://doi.org/10.2147/CIA.S174196
Liodakis E, Antoniou J, Zukor DJ, Huk OL, Epure LM, Bergeron SG (2016) Major complications and transfusion rates after hemiarthroplasty and total hip arthroplasty for femoral neck fractures. J Arthroplasty 31:2008–2012. https://doi.org/10.1016/j.arth.2016.02.019
Morris R, Rethnam U, Russ B, Topliss C (2017) Assessing the impact of fracture pattern on transfusion requirements in hip fractures. Eur J Trauma Emerg Surg 43:337–342. https://doi.org/10.1007/s00068-016-0655-8
Woon CYL, Moretti VM, Schwartz BE, Goldberg BA (2017) Total hip arthroplasty and hemiarthroplasty: US national trends in the treatment of femoral neck fractures. Am J Orthop 46:E474-e478
Danninger T, Rasul R, Poeran J, Stundner O, Mazumdar M, Fleischut PM, Poultsides L, Memtsoudis SG (2014) Blood transfusions in total hip and knee arthroplasty: an analysis of outcomes. ScientificWorldJournal 2014:623460. https://doi.org/10.1155/2014/623460
Ashworth A, Klein AA (2010) Cell salvage as part of a blood conservation strategy in anaesthesia. Br J Anaesth 105:401–416. https://doi.org/10.1093/bja/aeq244
Hart A, Khalil JA, Carli A, Huk O, Zukor D, Antoniou J (2014) Blood transfusion in primary total hip and knee arthroplasty. Incidence, risk factors, and thirty-day complication rates. J Bone Joint Surg Am 96:1945–1951. https://doi.org/10.2106/JBJS.N.00077
Shander A, Hofmann A, Ozawa S, Theusinger OM, Gombotz H, Spahn DR (2010) Activity-based costs of blood transfusions in surgical patients at four hospitals. Transfusion 50:753–765. https://doi.org/10.1111/j.1537-2995.2009.02518.x
Yu X, Wang Z, Shen Y, Liu Z, Wang H, Zhang S, Gan J, Xue F, Han W, Shi X, Hu Y, Wang L, Li N, Wu P, Yang C, Jiang J (2020) Population-based projections of blood supply and demand, China, 2017–2036. Bull World Health Organ 98:10–18. https://doi.org/10.2471/BLT.19.233361
Wang JQ, Chen LY, Jiang BJ, Zhao YM (2020) Development of a nomogram for predicting blood transfusion risk after hemiarthroplasty for femoral neck fractures in elderly patients. Med Sci Monit 26:e920255. https://doi.org/10.12659/MSM.920255
Coresh J, Selvin E, Stevens LA, Manzi J, Kusek JW, Eggers P, Van Lente F, Levey AS (2007) Prevalence of chronic kidney disease in the United States. JAMA 298:2038–2047. https://doi.org/10.1001/jama.298.17.2038
Moramarco S, Morciano L, Morucci L, Messinese M, Gualtieri P, Carestia M, Ciccacci F, Orlando S, Buonomo E, Legramante JM, De Lorenzo A, Palombi L (2020) Epidemiology of hypoalbuminemia in hospitalized patients: a clinical matter or an emerging public health problem? Nutrients 12.https://doi.org/10.3390/nu12123656
Levey AS, Eckardt KU, Tsukamoto Y, Levin A, Coresh J, Rossert J, De Zeeuw D, Hostetter TH, Lameire N, Eknoyan G (2005) Definition and classification of chronic kidney disease: a position statement from Kidney Disease: Improving Global Outcomes (KDIGO). Kidney Int 67:2089–2100. https://doi.org/10.1111/j.1523-1755.2005.00365.x
(2002) K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Am J Kidney Dis 39:S1–266.
Sehat KR, Evans RL, Newman JH (2004) Hidden blood loss following hip and knee arthroplasty. Correct management of blood loss should take hidden loss into account. J Bone Joint Surg Br 86:561–565
Gross JB (1983) Estimating allowable blood loss: corrected for dilution. Anesthesiology 58:277–280. https://doi.org/10.1097/00000542-198303000-00016
Lin PC, Hsu CH, Huang CC, Chen WS, Wang JW (2012) The blood-saving effect of tranexamic acid in minimally invasive total knee replacement: is an additional pre-operative injection effective? J Bone Joint Surg Br 94:932–936. https://doi.org/10.1302/0301-620X.94B7.28386
Wang J, Zhao Y, Jiang B, Huang X (2021) Development of a nomogram to predict post-operative transfusion in the elderly after intramedullary nail fixation of femoral intertrochanteric fractures. Clin Interv Aging 16:1–7. https://doi.org/10.2147/CIA.S253193
Peduzzi P, Concato J, Kemper E, Holford TR, Feinstein AR (1996) A simulation study of the number of events per variable in logistic regression analysis. J Clin Epidemiol 49:1373–1379. https://doi.org/10.1016/s0895-4356(96)00236-3
Hollis S, Campbell F (1999) What is meant by intention to treat analysis? Survey of published randomised controlled trials. BMJ 319:670–674. https://doi.org/10.1136/bmj.319.7211.670
Augustin ID, Yeoh TY, Sprung J, Berry DJ, Schroeder DR, Weingarten TN (2013) Association between chronic kidney disease and blood transfusions for knee and hip arthroplasty surgery. J Arthroplasty 28:928–931. https://doi.org/10.1016/j.arth.2013.02.004
Chen J, Zhang F, Liu CY, Yuan QM, Di XS, Long SW, Shang HC, Jia YS (2020) Impact of chronic kidney disease on outcomes after total joint arthroplasty: a meta-analysis and systematic review. Int Orthop 44:215–229. https://doi.org/10.1007/s00264-019-04437-4
Graves A, Yates P, Hofmann AO, Farmer S, Ferrari P (2014) Predictors of perioperative blood transfusions in patients with chronic kidney disease undergoing elective knee and hip arthroplasty. Nephrology (Carlton) 19:404–409. https://doi.org/10.1111/nep.12239
Girvent M, Maestro S, Hernández R, Carajol I, Monné J, Sancho JJ, Gubern JM, Sitges-Serra A (1998) Euthyroid sick syndrome, associated endocrine abnormalities, and outcome in elderly patients undergoing emergency operation. Surgery 123:560–567. https://doi.org/10.1067/msy.1998.87238
Cauteruccio M, Vitiello R, Perisano C, Covino M, Sircana G, Piccirillo N, Pesare E, Ziranu A, Maccauro G (2020) Euthyroid sick syndrome in hip fractures: evaluation of post-operative anemia. Injury 51 Suppl 3:S9-s12. https://doi.org/10.1016/j.injury.2020.07.006
Adunsky A, Lichtenstein A, Mizrahi E, Arad M, Heim M (2003) Blood transfusion requirements in elderly hip fracture patients. Arch Gerontol Geriatr 36:75–81. https://doi.org/10.1016/s0167-4943(02)00059-6
Sessler DI (2008) Temperature monitoring and perioperative thermoregulation. Anesthesiology 109:318–338. https://doi.org/10.1097/ALN.0b013e31817f6d76
Borghi B, Casati A, Iuorio S, Celleno D, Michael M, Serafini P, Pusceddu A, Fanelli G (2002) Frequency of hypotension and bradycardia during general anesthesia, epidural anesthesia, or integrated epidural-general anesthesia for total hip replacement. J Clin Anesth 14:102–106. https://doi.org/10.1016/s0952-8180(01)00362-2
Morcos MW, Jiang F, McIntosh G, Ahn H, Dea N, Abraham E, Paquet J, Natara A, Johnson M, Manson N, Fisher C, Rampersaud R, Thomas K, Hall H, Weber M (2019) Predictive factors for discharge destination following posterior lumbar spinal fusion: a Canadian Spine Outcome and Research Network (CSORN) Study. Glob Spine J 9:403–408. https://doi.org/10.1177/2192568218797090
Sershon RA, Fillingham YA, Malkani AL, Abdel MP, Schwarzkopf R, Padgett DE, Vail TP, Della Valle CJ (2021) Independent risk factors for transfusion in contemporary revision total hip arthroplasty. J Arthroplasty 36:2921–2926. https://doi.org/10.1016/j.arth.2021.03.032
Kapadia BH, Banerjee S, Issa K, McElroy MJ, Harwin SF, Mont MA (2013) Pre-operative blood management strategies for total knee arthroplasty. J Knee Surg 26:373–377. https://doi.org/10.1055/s-0033-1357492
Petis SM, Lanting BA, Vasarhelyi EM, Naudie DDR, Ralley FE, Howard JL (2017) Is there a role for pre-operative iron supplementation in patients preparing for a total hip or total knee arthroplasty? J Arthroplasty 32:2688–2693. https://doi.org/10.1016/j.arth.2017.04.029
Voorn VM, van der Hout A, So-Osman C, Vliet Vlieland TP, Nelissen RG, van den Akker-van Marle ME, Dahan A, Marang-van de Mheen PJ, van Bodegom-Vos L (2016) Erythropoietin to reduce allogeneic red blood cell transfusion in patients undergoing total hip or knee arthroplasty. Vox Sang 111:219–225. https://doi.org/10.1111/vox.12412
Abdel MP, Chalmers BP, Taunton MJ, Pagnano MW, Trousdale RT, Sierra RJ, Lee YY, Boettner F, Su EP, Haas SB, Figgie MP, Mayman DJ (2018) Intravenous versus topical tranexamic acid in total knee arthroplasty: both effective in a randomized clinical trial of 640 patients. J Bone Joint Surg Am 100:1023–1029. https://doi.org/10.2106/JBJS.17.00908
Moo IH, Chen JYQ, Pagkaliwaga EH, Tan SW, Poon KB (2017) Bone wax is effective in reducing blood loss after total knee arthroplasty. J Arthroplasty 32:1483–1487. https://doi.org/10.1016/j.arth.2016.12.028
Pawaskar A, Salunke AA, Kekatpure A, Chen Y, Nambi GI, Tan J, Sonawane D, Pathak S (2017) Do autologous blood transfusion systems reduce allogeneic blood transfusion in total knee arthroplasty? Knee Surg Sports Traumatol Arthrosc 25:2957–2966. https://doi.org/10.1007/s00167-016-4116-z
Karkouti K, Callum JL, Acker JP, Yip P, Rao V (2017) Red Cell Transfusion-associated hemolysis in cardiac surgery: an observational cohort study. Anesth Analg 124:1986–1991. https://doi.org/10.1213/ANE.0000000000001807
De la Garza RR, Gelfand Y, Benton JA, Longo M, Echt M, Yanamadala V, Yassari R (2020) Rates, risk factors, and complications of red blood cell transfusion in metastatic spinal tumor surgery: an analysis of a prospective multicenter surgical database. World Neurosurg 139:e308–e315. https://doi.org/10.1016/j.wneu.2020.03.202
Acknowledgements
We appreciate the contribution of all patients, the investigators, and the medical staff.
Funding
This study was supported by the Non-profit Central Research Institute Fund of the Chinese Academy of Medical Sciences [2019PT320001].
Author information
Authors and Affiliations
Contributions
Yingze Zhang and Wei Chen contributed to the study conception and design. Material preparation and data collection were performed by Xiangtian Deng, Xiaodong Cheng, and Hongzhi Hu. Yonglong Li analyzed and interpreted the data. The first draft of the manuscript was written by Jian Zhu and Xiangtian Deng. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This retrospective study was approved by the Third Hospital of Hebei Medical University, and all participants provided written informed consents.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Consent to publish was obtained from the patient detailed in this study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhu, J., Hu, H., Deng, X. et al. Risk factors analysis and nomogram construction for blood transfusion in elderly patients with femoral neck fractures undergoing hemiarthroplasty. International Orthopaedics (SICOT) 46, 1637–1645 (2022). https://doi.org/10.1007/s00264-022-05347-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-022-05347-8