Abstract
Purpose
Tourniquets are routinely used in high tibial osteotomy (HTO). However, research on the necessity of tourniquets during HTO is lacking. This study was designed to investigate the necessity of tourniquets in HTO.
Methods
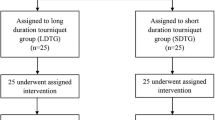
This was a prospective study that included patients who underwent HTO at the same hospital. The patients were randomised into Group A (non-tourniquet, n = 45) and Group B (tourniquet, n = 45). Same surgical techniques and haemostatic methods were used in the two groups.
Results
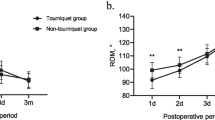
All patients were followed up for more than three months. There was no difference in operation time, and no intra-operative vascular or nerve damage occurred in either group. The hospital stay was shorter in group A than in group B (p < 0.05). There was no difference in post-operative blood loss, haemoglobin or haematocrit (p > 0.05). The post-operative visual analogue scale (VAS) pain scores and calf swelling were lower in group A (p < 0.05), and the early knee range of motion was higher in group A (p < 0.05). The use of morphine and the incidence of thigh complications were also lower in group A (p < 0.05). There was no difference in the VAS and knee function between the two groups at three months post-operatively (p > 0.05).
Conclusion
Tourniquet use during HTO does not reduce post-operative blood loss, operation time or intra-operative complications, but not using a tourniquet shortens the hospital stay and reduces the post-operative usage of morphine and tourniquet-related complications, which promotes early recovery of knee function.




Similar content being viewed by others
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Change history
19 January 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00264-021-05297-7
References
Hernigou P, Giber D, Dubory A, Auregan JC (2020) Safety of simultaneous versus staged bilateral opening-wedge high tibial osteotomy with locked plate and immediate weight bearing. Int Orthop 44(1):109–117. https://doi.org/10.1007/s00264-019-04385-z
Lee SH, Seo HY, Lim JH, Kim MG, Seon JK (2021) Higher survival rate in total knee arthroplasty after high tibial osteotomy than that after unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06641-5
Schuster P, Gesslein M, Schlumberger M, Mayer P, Mayr R, Oremek D, Frank S, Schulz-Jahrsdorfer M, Richter J (2018) Ten-year results of medial open-wedge high tibial osteotomy and chondral resurfacing in severe medial osteoarthritis and varus malalignment. Am J Sports Med 46(6):1362–1370. https://doi.org/10.1177/0363546518758016
Kim KI, Kim HJ, Kim GB, Bae SH (2018) Tranexamic acid is effective for blood management in open-wedge high tibial osteotomy. Orthop Traumatol Surg Res 104(7):1003–1007. https://doi.org/10.1016/j.otsr.2018.07.019
Palanisamy JV, Das S, Moon KH, Kim DH, Kim TK (2018) Intravenous tranexamic acid reduces postoperative blood loss after high tibial osteotomy. Clin Orthop Relat Res 476(11):2148–2154. https://doi.org/10.1097/CORR.0000000000000378
Li S, Lu Q, Guo X, Zhang M, Miao Z, Luo D, Liu P (2020) Intravenous combined with topical tranexamic acid administration has no additional benefits compared with intravenous administration alone in high tibial osteotomy: a retrospective case-control study. Orthop Surg 12(2):515–523. https://doi.org/10.1111/os.12652
Yao RZ, Gao WQ, Wang BW, Wang GL, Wu CX, A-Mu YD, (2019) Efficacy and safety of tranexamic acid in reducing blood loss of lower extremity osteotomy in peri-acetabulum and high tibia: a systematic review and meta-analysis. Orthop Surg 11(4):545–551. https://doi.org/10.1111/os.12515
Yi S, Tan J, Chen C, Chen H, Huang W (2014) The use of pneumatic tourniquet in total knee arthroplasty: a meta-analysis. Arch Orthop Trauma Surg 134(10):1469–1476. https://doi.org/10.1007/s00402-014-2056-y
Ozkunt O, Sariyilmaz K, Gemalmaz HC, Dikici F (2018) The effect of tourniquet usage on cement penetration in total knee arthroplasty: a prospective randomized study of 3 methods. Medicine (Baltimore) 97(4):e9668. https://doi.org/10.1097/MD.0000000000009668
Ryu KJ (2016) CORR Insights((R)): Does tourniquet use in TKA affect recovery of lower extremity strength and function? A randomized trial. Clin Orthop Relat Res 474(1):78–80. https://doi.org/10.1007/s11999-015-4436-1
Heller S, Chen A, Restrepo C, Albert E, Hozack WJ (2015) Tourniquet release prior to dressing application reduces blistering following total knee arthroplasty. J Arthroplasty 30(7):1207–1210. https://doi.org/10.1016/j.arth.2015.02.035
Xie J, Ma J, Yao H, Yue C, Pei F (2016) Multiple boluses of intravenous tranexamic acid to reduce hidden blood loss after primary total knee arthroplasty without tourniquet: a randomized clinical trial. J Arthroplasty 31(11):2458–2464. https://doi.org/10.1016/j.arth.2016.04.034
Huang Z, Xie X, Li L, Huang Q, Ma J, Shen B, Kraus VB, Pei F (2017) Intravenous and topical tranexamic acid alone are superior to tourniquet use for primary total knee arthroplasty: a prospective, randomized controlled trial. J Bone Joint Surg Am 99(24):2053–2061. https://doi.org/10.2106/JBJS.16.01525
Yue C, Kang P, Yang P, Xie J, Pei F (2014) Topical application of tranexamic acid in primary total hip arthroplasty: a randomized double-blind controlled trial. J Arthroplasty 29(12):2452–2456. https://doi.org/10.1016/j.arth.2014.03.032
Motycka T, Eggerth G, Landsiedl F (2000) The incidence of thrombosis in high tibial osteotomies with and without the use of a tourniquet. Arch Orthop Trauma Surg 120(3–4):157–159. https://doi.org/10.1007/s004020050034
Suh DW, Kyung BS, Han SB, Cheong K, Lee WH (2018) Efficacy of tranexamic acid for hemostasis in patients undergoing high tibial osteotomy. J Knee Surg 31(1):50–55. https://doi.org/10.1055/s-0037-1600091
Li S, Yang J, Watson C, Lu Q, Zhang M, Miao Z, Luo D, Liu P (2020) Drainage relieves pain without increasing post-operative blood loss in high tibial osteotomy: a prospective randomized controlled study. Int Orthop 44(6):1037–1043. https://doi.org/10.1007/s00264-020-04530-z
Nadler SB, Hidalgo JH, Bloch T (1962) Prediction of blood volume in normal human adults. Surgery 51(2):224–232
Matziolis D, Perka C, Hube R, Matziolis G (2011) Influence of tourniquet ischemia on perioperative blood loss after total knee arthroplasty. Orthopade 40(2):178–182. https://doi.org/10.1007/s00132-010-1727-9
Guler O, Mahirogullari M, Isyar M, Piskin A, Yalcin S, Mutlu S, Sahin B (2016) Comparison of quadriceps muscle volume after unilateral total knee arthroplasty with and without tourniquet use. Knee Surg Sports Traumatol Arthrosc 24(8):2595–2605. https://doi.org/10.1007/s00167-015-3872-5
Dennis DA, Kittelson AJ, Yang CC, Miner TM, Kim RH, Stevens-Lapsley JE (2016) Does tourniquet use in TKA affect recovery of lower extremity strength and function? A randomized trial. Clin Orthop Relat Res 474(1):69–77. https://doi.org/10.1007/s11999-015-4393-8
Jimenez JJ, Iribarren JL, Lorente L, Rodriguez JM, Hernandez D, Nassar I, Perez R, Brouard M, Milena A, Martinez R, Mora ML (2007) Tranexamic acid attenuates inflammatory response in cardiopulmonary bypass surgery through blockade of fibrinolysis: a case control study followed by a randomized double-blind controlled trial. Crit Care 11(6):R117. https://doi.org/10.1186/cc6173
Zhou K, Wang H, Li J, Wang D, Zhou Z, Pei F (2017) Non-drainage versus drainage in tourniquet-free knee arthroplasty: a prospective trial. Anz J Surg 87(12):1048–1052. https://doi.org/10.1111/ans.14183
Aglietti P, Baldini A, Vena LM, Abbate R, Fedi S, Falciani M (2000) Effect of tourniquet use on activation of coagulation in total knee replacement. Clin Orthop Relat Res 371:169–177. https://doi.org/10.1097/00003086-200002000-00021
Hernandez AJ, Almeida AM, Favaro E, Sguizzato GT (2012) The influence of tourniquet use and operative time on the incidence of deep vein thrombosis in total knee arthroplasty. Clinics (Sao Paulo) 67(9):1053–1057. https://doi.org/10.6061/clinics/2012(09)12
Martin R, Birmingham TB, Willits K, Litchfield R, Lebel ME, Giffin JR (2014) Adverse event rates and classifications in medial opening wedge high tibial osteotomy. Am J Sports Med 42(5):1118–1126. https://doi.org/10.1177/0363546514525929
Acknowledgements
The authors are grateful to the patients that were willing to participate in the study.
Funding
This work was funded by the Natural Science Foundation of Shandong Province (ZR2020MH278), the Horizontal project of Shandong University (12671818) and the Rongxiang Regenerative Medicine Foundation of Shandong University (2019SDRX-17).
Author information
Authors and Affiliations
Contributions
All authors contributed to either the conception, design, data collection or analysis. Songlin Li, Wenwei Qian and Peilai Liu were responsible for conception and design of the study. Songlin Li, Xiangshuai Zhang and Qunshan Lu drafted the manuscript. Mingxing Liu, Desu Luo, Kaifei Han and Lei Li contributed to data collection. Songlin Li, Mingxing Liu, YangYu and Zhuang Miao contributed to manuscript preparation and data analysis. Peilai Liu and Wenwei Qian contributed to revision of the manuscript. All authors read and approved the final manuscript. Wenwei Qian and Peilai Liu contribute equally to the work and should be regarded as co-corresponding authors.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This trial was approved by the ethics committee of a local hospital (KYLL-2019042) and registered at ClinicalTrials.gov, number NCT-04992533.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original version of this article was revised. The correct copyright should be “The Author(s) under exclusive licence to SICOT aisbl.”
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Li, S., Zhang, X., Liu, M. et al. Not using a tourniquet is superior to tourniquet use for high tibial osteotomy: a prospective, randomised controlled trial. International Orthopaedics (SICOT) 46, 823–829 (2022). https://doi.org/10.1007/s00264-021-05246-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-021-05246-4