Abstract
Purpose
The study compared a novel imageless robotic-assisted total knee arthroplasty (RATKA) and conventional TKA by considering (1) radiological outcomes, (2) outliers of radiological outcomes, and (3) learning curve.
Methods
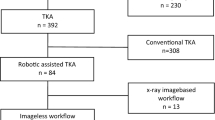
This prospective randomized controlled study performed by a single surgeon evaluated 152 patients (152 knees): 75 patients undergoing RATKA and 77 patients undergoing conventional TKA. Mechanical alignment, radiological implant positioning, and outliers were analyzed for radiological outcomes. Cumulative summation (CUSUM) analysis was used to assess the learning curve for operative time in RATKA.
Results
The RATKA had significantly better accuracy of knee alignment and component positioning than conventional TKA. The hip-knee-ankle axis and implant position outliers were significantly lower in the RATKA, with 94.7% of patients had achieved an overall mechanical alignment within 3° of a neutral mechanical axis. Changes in posterior condylar offset and joint line were significantly lower in the RATKA. A learning curve of seven cases for operative time was obtained for the RATKA.
Conclusion
The imageless RATKA has better alignment accuracy with a short learning curve; thus, it presents an attractive option for TKA.




Similar content being viewed by others
Data availability
All data and material pertaining to the study are made available upon request.
References
Sharkey PF, Lichstein PM, Shen C, Tokarski AT, Parvizi J (2014) Why are total knee arthroplasties failing today–has anything changed after 10 years? J Arthroplasty 29(9):1774–1778. https://doi.org/10.1016/j.arth.2013.07.024
Fehring TK, Odum S, Griffin WL, Mason JB, Nadaud M (2001) Early failures in total knee arthroplasty. Clin Orthop Relat Res 392:315–318. https://doi.org/10.1097/00003086-200111000-00041
Rodriguez JA, Bhende H, Ranawat CS (2001) Total condylar knee replacement: a 20-year followup study. Clin Orthop Relat Res 388:10–17
Thiengwittayaporn S, Fusakul Y, Kangkano N, Jarupongprapa C, Charoenphandhu N (2016) Hand-held navigation may improve accuracy in minimally invasive total knee arthroplasty: a prospective randomized controlled trial. Int Orthop 40(1):51–57. https://doi.org/10.1007/s00264-015-2848-x
Agarwal N, To K, McDonnell S, Khan W (2020) Clinical and radiological outcomes in robotic-assisted total knee arthroplasty: a systematic review and meta-analysis. J Arthroplasty 35(11):3393-3409.e3392. https://doi.org/10.1016/j.arth.2020.03.005
Kayani B, Konan S, Tahmassebi J, Pietrzak JRT, Haddad FS (2018) Robotic-arm assisted total knee arthroplasty is associated with improved early functional recovery and reduced time to hospital discharge compared with conventional jig-based total knee arthroplasty: a prospective cohort study. Bone Joint J 100(7):930–937. https://doi.org/10.1302/0301-620x.100b7.Bjj-2017-1449.R1
Kayani B, Konan S, Ayuob A, Onochie E, Al-Jabri T, Haddad FS (2019) Robotic technology in total knee arthroplasty: a systematic review. EFORT Open Rev 4(10):611–617. https://doi.org/10.1302/2058-5241.4.190022
Vaidya NV, Deshpande AN, Panjwani T, Patil R, Jaysingani T, Patil P (2020) Robotic-assisted TKA leads to a better prosthesis alignment and a better joint line restoration as compared to conventional TKA: a prospective randomized controlled trial. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06353-2
Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the knee society clinical rating system. Clin Orthop Relat Res 248:13–14
Murray DW, Fitzpatrick R, Rogers K, Pandit H, Beard DJ, Carr AJ, Dawson J (2007) The use of the Oxford hip and knee scores. J Bone Joint Surg Br 89(8):1010–1014. https://doi.org/10.1302/0301-620X.89B8.19424
Feller JA, Bartlett RJ, Lang DM (1996) Patellar resurfacing versus retention in total knee arthroplasty. J Bone Joint Surg Br 78(2):226–228
Boeckstyns ME, Backer M (1989) Reliability and validity of the evaluation of pain in patients with total knee replacement. Pain 38(1):29–33. https://doi.org/10.1016/0304-3959(89)90069-9
Doyle DJ, Goyal A, Bansal P, Garmon EH (2021) American society of anesthesiologists classification. In: StatPearls [Internet]. StatPearls Publishing, Treasure Island (FL)
Bellemans J, Banks S, Victor J, Vandenneucker H, Moemans A (2002) Fluoroscopic analysis of the kinematics of deep flexion in total knee arthroplasty. Influence of posterior condylar offset. J Bone Joint Surg Br 84(1):50–53. https://doi.org/10.1302/0301-620x.84b1.12432
Colebatch AN, Hart DJ, Zhai G, Williams FM, Spector TD, Arden NK (2009) Effective measurement of knee alignment using AP knee radiographs. Knee 16(1):42–45. https://doi.org/10.1016/j.knee.2008.07.007
Vanin N, Panzica M, Dikos G, Krettek C, Hankemeier S (2011) Rotational alignment in total knee arthroplasty: intraoperative inter- and intraobserver reliability of Whiteside’s line. Arch Orthop Trauma Surg 131(11):1477–1480. https://doi.org/10.1007/s00402-011-1329-y
Dai Y, GB, CH (2018) Learning curve in computer-assisted total knee arthroplasty: a CUSUM analysis. CAOS 2018. The 18th Annual Meeting of the International Society for Computer Assisted Orthopaedic Surgery. EasyChair. https://doi.org/10.29007/wzh3
Kayani B, Konan S, Huq SS, Tahmassebi J, Haddad FS (2019) Robotic-arm assisted total knee arthroplasty has a learning curve of seven cases for integration into the surgical workflow but no learning curve effect for accuracy of implant positioning. Knee Surg Sports Traumatol Arthrosc 27(4):1132–1141. https://doi.org/10.1007/s00167-018-5138-5
Song EK, Seon JK, Yim JH, Netravali NA, Bargar WL (2013) Robotic-assisted TKA reduces postoperative alignment outliers and improves gap balance compared to conventional TKA. Clin Orthop Relat Res 471(1):118–126. https://doi.org/10.1007/s11999-012-2407-3
Babazadeh S, Dowsey MM, Swan JD, Stoney JD, Choong PF (2011) Joint line position correlates with function after primary total knee replacement: a randomised controlled trial comparing conventional and computer-assisted surgery. J Bone Joint Surg Br 93(9):1223–1231. https://doi.org/10.1302/0301-620x.93b9.26950
Liow MH, Chin PL, Tay KJ, Chia SL, Lo NN, Yeo SJ (2014) Early experiences with robot-assisted total knee arthroplasty using the DigiMatchTM ROBODOC® surgical system. Singapore Med J 55(10):529–534. https://doi.org/10.11622/smedj.2014136
Watanabe T, Abbasi AZ, Conditt MA, Christopher J, Kreuzer S, Otto JK, Banks SA (2014) In vivo kinematics of a robot-assisted uni- and multi-compartmental knee arthroplasty. J Orthop Sci 19(4):552–557. https://doi.org/10.1007/s00776-014-0578-3
Kayani B, Konan S, Pietrzak JRT, Haddad FS (2018) Iatrogenic bone and soft tissue trauma in robotic-arm assisted total knee arthroplasty compared with conventional jig-based total knee arthroplasty: a prospective cohort study and validation of a new classification system. J Arthroplasty 33(8):2496–2501. https://doi.org/10.1016/j.arth.2018.03.042
Yang HY, Seon JK, Shin YJ, Lim HA, Song EK (2017) Robotic total knee arthroplasty with a cruciate-retaining implant: a 10-year follow-up study. Clin Orthop Surg 9(2):169–176. https://doi.org/10.4055/cios.2017.9.2.169
Cho KJ, Seon JK, Jang WY, Park CG, Song EK (2019) Robotic versus conventional primary total knee arthroplasty: clinical and radiological long-term results with a minimum follow-up of ten years. Int Orthop 43(6):1345–1354. https://doi.org/10.1007/s00264-018-4231-1
Liow MHL, Goh GS, Wong MK, Chin PL, Tay DK, Yeo SJ (2017) Robotic-assisted total knee arthroplasty may lead to improvement in quality-of-life measures: a 2-year follow-up of a prospective randomized trial. Knee Surg Sports Traumatol Arthrosc 25(9):2942–2951. https://doi.org/10.1007/s00167-016-4076-3
Sodhi N, Khlopas A, Piuzzi NS, Sultan AA, Marchand RC, Malkani AL, Mont MA (2018) The learning curve associated with robotic total knee arthroplasty. J Knee Surg 31(1):17–21. https://doi.org/10.1055/s-0037-1608809
Acknowledgements
The authors thank Ms. Thikampa Wichai, for their help in collecting and organizing the data analyzed in this report.
Funding
This project was supported by the Faculty of Medicine Vajira Hospital, Navamindradhiraj University Research Fund, Thailand (grant numbers 10–63).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by ST, PU, and NH. The first draft of the manuscript was written by ST, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
The study has been performed in compliance with the Helsinki Declaration, has been approved by the ethical committee of Navamindradhiraj University (COA012/2563), and registered on ClinicalTrials.gov (NCT04307251).
Consent to participate/consent for publication
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Thiengwittayaporn, S., Uthaitas, P., Senwiruch, C. et al. Imageless robotic-assisted total knee arthroplasty accurately restores the radiological alignment with a short learning curve: a randomized controlled trial. International Orthopaedics (SICOT) 45, 2851–2858 (2021). https://doi.org/10.1007/s00264-021-05179-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-021-05179-y