Abstract
Purpose
Hypoxia is a well-known complication in cemented arthroplasty; however, it is not known whether the level of hypoxia is related to the intramedullary pressure or to the age of the patient; therefore, we studied the intramedullary pressure and level of hypoxia in patients undergoing cemented arthroplasty.
Methods
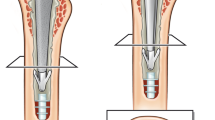
A prospective study was performed during cemented arthroplasties in 25 patients with an average age of 66.2 ± 12.1 years old. The intramedullary pressure (IMP) was measured by placing a pressure transducer within the bone while simultaneously measuring the pulse oximetry arterial oxygen saturation (SpO2), pulse, and blood pressure. These variables were obtained immediately after spinal anaesthesia, five minutes after cementation, and 15 minutes after prosthesis insertion.
Results
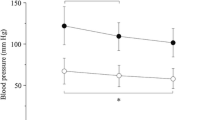
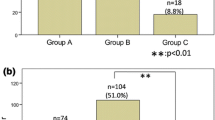
One hundred percent of patients had hypoxia at some level, but 83% of elderly patients (older than 66.5 years) had hypoxia (SpO2 <94%) as compared to only 23% of younger patients (p = 0.006). In the group of young patients, IMP was roughly increased 32 times as compared with baseline level, with as consequences a decrease of 4% of SpO2 (from 98.3 to 94.15%); in the elderly group, the IMP was only increased 20 times, but a decrease of 6% of SpO2 (from 97.25 to 91%) was observed.
Conclusions
This series demonstrated higher hypoxia in elderly healthy patients despite a paradoxical lower femoral increase of intramedullary pressure as compared with younger patients. This hypoxia is probably not only related to the cement but also to the patient’s age with decline of maximum oxygen uptake capacity and increase bone porosity.
Clinical trials
ClinicalTrials.gov Identifier: NCT03930537 https://clinicaltrials.gov/ct2/show/NCT03930537




Similar content being viewed by others
References
Sierra RJ, Timperley JA, Gie GA (2009) Contemporary cementing technique and mortality during and after Exeter total hip arthroplasty. J Arthroplasty 24(3):325–332
Talsnes O, Vinje T, Gjertsen JE, Dahl OE, Engesaeter LB, Baste V, Pripp AH, Reikeras O (2013) Perioperative mortality in hip fracture patients treated with cemented and uncemented hemiprosthesis: a register study of 11,210 patients. Int Orthop 37(6):1135–1140
Garland A, Gordon M, Garellick G, Karrholm J, Skoldenberg O, Hailer NP (2017) Risk of early mortality after cemented compared with cementless total hip arthroplasty: a nationwide matched cohort study. Bone Joint J 99-b(1):37–43
Donaldson AJ, Thomson HE, Harper NJ et al (2009) Bone cement implantation syndrome. Brit J Anaesth 102:12–22
Lindahl H, Oden A, Garellick G, Malchau H (2007) The excess mortality due to periprosthetic femur fracture: a study from the Swedish national hip arthroplasty register. Bone 40(5):1294–1298
Dale H, Børsheim S, Kristensen TB, Fenstad AM, Gjertsen JE, Hallan G, Lie SA, Furnes O (2020) Fixation, ksex, and age: highest risk of revision for uncemented stems in elderly women—data from 66,995 primary total hip arthroplasties in the Norwegian Arthroplasty Register. Acta Orthop Feb 91(1):33–41. https://doi.org/10.1080/17453674.2019.1682851
Olsen F, Hård Af Segerstad M, Nellgård B, Houltz E, Ricksten SE (2020) The role of bone cement for the development of intraoperative hypotension and hypoxia and its impact on mortality in hemiarthroplasty for femoral neck fractures. Acta Orthop 91(3):293–298. https://doi.org/10.1080/17453674.2020.1745510
Dale H, Børsheim S, Kristensen TB, Fenstad AM, Gjertsen JE, Hallan G, Lie SA, Furnes O (2020) Perioperative, short-, and long-term mortality related to fixation in primary total hip arthroplasty: a study on 79,557 patients in the -Norwegian Arthroplasty Register. Acta Orthop 91(2):152–158. https://doi.org/10.1080/17453674.2019.1701312
Kotyra M, Houltz E, Ricksten S-E (2010) Pulmonary haemodynamics and right ventricular function during cemented hemiarthroplasty for femoral neck fracture: pulmonary haemodynamics and right ventricular function. Acta Anaesthesiol Scand 54(10):1210–1216
Pitto RP, Koessler M, Kuehle JW (1999) Comparison of fixation of the femoral component without cement and fixation with use of a bone-vacuum cementing technique for the prevention of fat embolism during total hip arthroplasty. A prospective, randomized clinical trial. J Bone Joint Surg Am. 81(6):831–843
Smith PN, Leditschke A, McMahon D, Sample RR, Perriman D, Prins A, Brüssel T, Li RW (2008) Monitoring and controlling intramedullary pressure increase in long bone instrumentation: a study on sheep. J Orthop Res 26(10):1327–1333. https://doi.org/10.1002/jor.20564
Song Y, Goodman SB, Jaffe RA (1994) An in vitro study of femoral intramedullary pressures during hip replacement using modern cement technique. Clin Orthop Relat Res 302:297–304
Hallin G, Modig J, Nordgren L, Olerud S (1974) The intramedullary pressure during the bone marrow trauma of total hip replacement surgery. Ups J MedSci 79(1):51–54. https://doi.org/10.3109/03009737409178390
Rothberg DL, Kubiak EN, Peters CL, Randall RL, Aoki SK (2013) Reducing the risk of bone cement implantation syndrome during femoral arthroplasty. Orthopedics 36:e463–e467. https://doi.org/10.3928/01477447-20130327-23
Dunne NJ, Orr JF (2000) Development of a computer model to predict pressure generation around hip replacement stems. Proc Inst Mech Eng H. 214(6):645–658. https://doi.org/10.1243/0954411001535679
Stein MS, Feik SA, Thomas CD, Clement JG, Wark JD (1999) An automated analysis of intracortical porosity in human femoral bone across age. J Bone Miner Res 14(4):624–632. https://doi.org/10.1359/jbmr.1999.14.4.624
Hernigou P (2020) Bone marrow in orthopaedics (part II): a three hundred and seventy million-year saga from the Devonian to the coronavirus disease 2019 pandemic-osteonecrosis; transplantation; “human chimera”; stem cells, bioreactors, and coronavirus disease. Int Orthop 9:1–19. https://doi.org/10.1007/s00264-020-04843-z
Rasch-Halvorsen Ø, Hassel E, Langhammer A, Brumpton BM, Steinshamn S (2019) The association between dynamic lung volume and peak oxygen uptake in a healthy general population: the HUNT study. BMC Pulm Med 19(1):2. https://doi.org/10.1186/s12890-018-0762-x
Janssens JP, Pache JC, Nicod LP (1999) Physiological changes in respiratory function associated with ageing. Eur Respir J. 13:197–205
Johnson BD, Dempsey JA (1991) Demand vs. capacity in the aging pulmonary system. Exerc Sport Sci Rev. 19:171–210
Lenke LG, White DK, Kemp JS, Bridwell KH, Blanke KM, Engsberg JR (2002) Evaluation of ventilatory efficiency during exercise in patients with idiopathic scoliosis undergoing spinal fusion. 27(18):2041–2045. https://doi.org/10.1097/00007632-200209150-00014
Imam MA, Shehata MSA, Elsehili A, Morsi M, Martin A, Shawqi M, Grubhofer F, Chirodian N, Narvani A, Ernstbrunner L (2019) Contemporary cemented versus uncemented hemiarthroplasty for the treatment of displaced intracapsular hip fractures: a meta-analysis of forty-two thousand forty-six hips. Int Orthop 43(7):1715–1723. https://doi.org/10.1007/s00264-019-04325-x
Phypers BJ, Robiony-Rogers D, Pickering RM, Garden AL (2011) Test-retest reliability of the oxygen uptake efficiency slope in surgical patients. Anaesthesia Aug 66(8):659–666. https://doi.org/10.1111/j.1365-2044.2011.06714.x
Martin R, Leighton RK, Petrie D, Ikejiani C, Smyth B (1996) Effect of proximal and distal venting during intramedullary nailing. Clin Orthop 332:80–89
Availability of data and materials
ClinicalTrials.gov ID: NCT03930537
Author information
Authors and Affiliations
Contributions
SU: Surgery
MS, SK, VP, and AA: Data collection
PH: Study design, redaction, iconography
FU: Statistics
MC: Redaction
Corresponding author
Ethics declarations
Ethics approval
All procedures were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study
Consent to participate
Informed consent was obtained from all individual participants included in the study
Consent for publication
Participants have given consent for data publication.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ukaj, S., Veslko, M., Krasniqi, S. et al. Cemented stems in healthy elderly patients result in higher hypoxia despite a paradoxical lower femoral increase of intramedullary pressure. International Orthopaedics (SICOT) 45, 915–922 (2021). https://doi.org/10.1007/s00264-021-04955-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-021-04955-0