Abstract
Purpose
The study objective was to compare the clinical results of reverse total shoulder arthroplasty (rTSA) and anatomical total shoulder arthroplasty (aTSA) in patients with osteoarthritis and intact rotator cuff. We hypothesised that the clinical results using rTSA would be comparable with those obtained with aTSA in this group of patients.
Methods
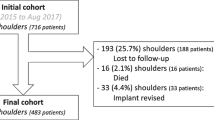
The study included 51 patients with shoulder osteoarthritis and intact rotator cuff who underwent rTSA or aTSA. The range of motion, Constant–Murley score and strength in external rotation were recorded pre-operatively and at the two year follow-up. Subjective post-operative results were measured using the subjective shoulder value (SSV) score and a satisfaction questionnaire.
Results
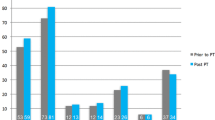
The post-operative improvement was significant in both groups, subjectively and concerning all parameters of the Constant–Murley score. Post-operatively, no significant difference was noted between the two groups for active anterior elevation (AAE), active external rotation (ER), internal rotation (IR) or Constant–Murley score (67 ± 12 in the rTSA group vs 71 ± 11 in the aTSA group). An exception was the Constant–Murley range of motion sub-score, which was better in the aTSA group (p = 0.028). No significant complications necessitating revision surgery were encountered.
Discussion
Our findings are consistent with previous studies showing good results of rTSA with shoulder osteoarthritis and intact rotator cuff with a good restoration of the IR, similar to that obtained with aTSA.
Conclusion
The rTSA is a valid option for shoulder osteoarthritis and intact rotator cuff in older adult patients.







Similar content being viewed by others
References
Sandow MJ, David H, Bentall SJ (2013) Hemiarthroplasty vs total shoulder replacement for rotator cuff intact osteoarthritis: how do they fare after a decade? J Shoulder Elb Surg 22:877–885. https://doi.org/10.1016/j.jse.2012.10.023
Roberson TA, Bentley JC, Griscom JT, Kissenberth MJ, Tolan SJ, Hawkins RJ et al (2017) Outcomes of total shoulder arthroplasty in patients younger than 65 years: a systematic review. J Shoulder Elb Surg 26:1298–1306. https://doi.org/10.1016/j.jse.2016.12.069
Raiss P, Bruckner T, Rickert M, Walch G (2014) Longitudinal observational study of total shoulder replacements with cement: fifteen to twenty year follow-up. J Bone Joint Surg Am 96:198–205. https://doi.org/10.2106/JBJS.M.00079
Young AA, Walch G, Pape G, Gohlke F, Favard L (2012) Secondary rotator cuff dysfunction following total shoulder arthroplasty for primary glenohumeral osteoarthritis: results of a multicenter study with more than five years of follow-up. J Bone Joint Surg Am 94:685–693. https://doi.org/10.2106/JBJS.J.00727
Wall B, Nové-Josserand L, O'Connor DP, Edwards TB, Walch G (2007) Reverse total shoulder arthroplasty: a review of results according to etiology. J Bone Joint Surg Am 89:1476–1485. https://doi.org/10.2106/JBJS.F.00666
Mulieri P, Dunning P, Klein S, Pupello D, Frankle M (2010) Reverse shoulder arthroplasty for the treatment of irreparable rotator cuff tear without glenohumeral arthritis. J Bone Joint Surg Am 92:2544–2556. https://doi.org/10.2106/JBJS.I.00912
Hasler A, Fornaciari P, Jungwirth-Weinberger A, Jentzsch T, Wieser K, Gerber C (2019) Reverse shoulder arthroplasty in the treatment of glenohumeral instability. J Shoulder Elb Surg 28:1587–1594. https://doi.org/10.1016/j.jse.2019.02.001
Shields E, Wiater JM (2019) Patient outcomes after revision of anatomic total shoulder arthroplasty to reverse shoulder arthroplasty for rotator cuff failure or component loosening: a matched cohort study. J Am Acad Orthop Surg 27:e193–e198. https://doi.org/10.5435/JAAOS-D-17-00350
Alentorn-Geli E, Wanderman NR, Assenmacher AT, Sperling JW, Cofield RH, Sánchez-Sotelo J (2018) Anatomic total shoulder arthroplasty with posterior capsular plication versus reverse shoulder arthroplasty in patients with biconcave glenoids: a matched cohort study. J Orthop Surg 26:1–8. https://doi.org/10.1177/2309499018768570
Steen BM, Cabezas AF, Santoni BG, Hussey MM, Cusick MC, Kumar AG et al (2015) Outcome and value of reverse shoulder arthroplasty for treatment of glenohumeral osteoarthritis: a matched cohort. J Shoulder Elb Surg 24:1433–1441. https://doi.org/10.1016/j.jse.2015.01.005
Bacle G, Nové-Josserand L, Garaud P, Walch G (2017) Long-term outcomes of reverse total shoulder arthroplasty: a follow-up of a previous study. J Bone Joint Surg Am 99:454–461. https://doi.org/10.2106/JBJS.16.00223
Mizuno N, Denard R, Raiss P, Walch G (2013) Reverse total shoulder arthroplasty for primary glenohumeral osteoarthritis in patients with a biconcave glenoid. J Bone Joint Surg Am 95:1297–1304. https://doi.org/10.2106/JBJS.L.00820
Wright MA, Keener JD, Chamberlain AM (2019) Comparison of clinical outcomes after anatomic total shoulder arthroplasty and reverse shoulder arthroplasty in patients 70 years and older with glenohumeral osteoarthritis and an intact rotator cuff. J Am Acad Orthop Surg 28:e222–e229. https://doi.org/10.5435/JAAOS-D-19-00166
Goutallier D, Postel JM, Bernageau J, Lavau L, Voisin MC (1994) Fatty muscle degeneration in cuff ruptures. Pre- and post-operative evaluation by CT scan. Clin Orthop Relat Res 304:78–83
Bercik MJ, Kruse K, Yalizis M, Gauci MO, Chaoui J, Walch G (2016) A modification to the Walch classification of the glenoid in primary glenohumeral osteoarthritis using three-dimensional imaging. J Shoulder Elb Surg 25:1601–1606. https://doi.org/10.1016/j.jse.2016.03.010
Friedman RJ, Hawthorne KB, Genez BM (1992) The use of computerized tomography in the measurement of glenoid version. J Bone Joint Surg Am 74:1032–1037
Kidder J, Rouleau D, Pons-Villanueva J, Dynamidis S, DeFranco M, Walch G (2010) Humeral head posterior subluxation on CT scan: validation and comparison of 2 methods of measurement. Tech Shoulder Elb Surg 11:72–76. https://doi.org/10.1097/BTE.0b013e3181e5d742
Walch G, Moraga C, Young A, Castellanos-Rosas J (2012) Results of anatomic non-constrained prosthesis in primary osteoarthritis with biconcave glenoid. J Should Elbow Surg 21:1526–1533. https://doi.org/10.1016/j.jse.2011.11.030
Merolla G, De Cupis M, Walch G, De Cupis V, Fabbri E, Franceschi F et al (2020) Pre-operative factors affecting the indications for anatomical and reverse total shoulder arthroplasty in primary osteoarthritis and outcome comparison in patients aged seventy years and older. Int Orthop 44:1131–1141. https://doi.org/10.1007/s00264-020-04501-4
Jackson JD, Cil A, Smith J, Steinmann SP (2010) Integrity and function of the subscapularis after total shoulder arthroplasty. J Shoulder Elb Surg 19:1085–1090. https://doi.org/10.1016/j.jse.2010.04.001
Shields E, Ho A, Wiater JM (2017) Management of the subscapularis tendon during total shoulder arthroplasty. J Shoulder Elb Surg 26:723–731. https://doi.org/10.1016/j.jse.2016.11.006
Oh JH, Shin SJ, McGarry MH, Scott JH, Heckmann N, Lee TQ (2014) Biomechanical effects of humeral neck-shaft angle and subscapularis integrity in reverse total shoulder arthroplasty. J Shoulder Elb Surg 23:1091–1098. https://doi.org/10.1016/j.jse.2013.11.003
Kiet TK, Feeley BT, Naimark M, Gajiu T, Hall SL, Chung TT et al (2015) Outcomes after shoulder replacement: comparison between reverse and anatomic total shoulder arthroplasty. J Shoulder Elb Surg 24:179–185. https://doi.org/10.1016/j.jse.2014.06.039
Lädermann A, Denard PJ, Boileau P, Farron A, Deransart P, Terrier A et al (2015) Effect of humeral stem design on humeral position and range of motion in reverse shoulder arthroplasty. Int Orthop 39:2205–2213. https://doi.org/10.1007/s00264-015-2984-3
Herrmann S, König C, Heller M, Perka C, Greiner S (2011) Reverse shoulder arthroplasty leads to significant biomechanical changes in the remaining rotator cuff. J Orthop Surg Res 6. https://doi.org/10.1186/1749-799X-6-42
Rol M, Favard L, Berhouet J (2019) Factors associated with internal rotation outcomes after reverse shoulder arthroplasty. Orthop Traumatol Surg Res 105:1515–1519. https://doi.org/10.1016/j.otsr.2019.07.024
Bigdon SF, Bolliger L, Albers CE, Collin P, Zumstein MA (2019) Subscapularis in reverse total shoulder arthroplasty. J Shoulder Elb Arthroplast 3:1–8. https://doi.org/10.1177/2471549219834192
Kiet TK, Feeley BT, Naimark M, Gajiu T, Hall SL, Chung TT et al (2015) Outcomes after shoulder replacement: comparison between reverse and anatomic total shoulder arthroplasty. J Shoulder Elb Surg 24:179–185. https://doi.org/10.1016/j.jse.2014.06.039
Cox RM, Padegimas EM, Abboud JA, Getz CL, Lazarus MD, Ramsey ML et al (2018) Outcomes of an anatomic total shoulder arthroplasty with a contralateral reverse total shoulder arthroplasty. J Shoulder Elb Surg 27:998–1003. https://doi.org/10.1016/j.jse.2017.12.005
Krithikadatta J (2014) Normal distribution. J Conserv Dent 17:96–97. https://doi.org/10.4103/0972-0707.124171
De Winter JCF (2013) Using the Student’s t-test with extremely small sample sizes. Pract Assessment Res Eval 18. https://doi.org/10.7275/e4r6-dj05
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Laurent Nové-Josserand receives royalties from 3S Ortho.
The other authors declare that they have no conflicts of interest.
Ethics approval
Approval was obtained from the ethics committee of the Scientific Committee of the GCS Ramsay Santé for Education and Research. Ethics approval number: COS-RGDS-2020-01-004-NOVE JOSSERAND-L.
Consent
All study participants provided informed consent.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Haritinian, EG., Belgaid, V., Lino, T. et al. Reverse versus anatomical shoulder arthroplasty in patients with intact rotator cuff. International Orthopaedics (SICOT) 44, 2395–2405 (2020). https://doi.org/10.1007/s00264-020-04754-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-020-04754-z