Abstract
Background
Several operative techniques exist for Achilles tendinopathy. The purpose of our study was to compare the clinical and functional outcomes of flexor hallucis longus (FHL) transfer and V-Y advancement for the treatment of chronic insertional Achilles tendinopathy.
Methods
Retrospective chart review from 2010 to 2016 of patients that underwent FHL transfer or V-Y advancement for chronic insertional Achilles tendinopathy. Outcome measures were compared for these two procedures.
Results
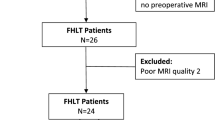
In total, 46 patients (49 ankles) with a mean age of 55.0 (range 33–73) years. Mean follow-up time 44.7 +/− 25.5 months. FHL group had 21 patients (21 ankles) with 89% satisfaction, 14% complication rate, final VAS of 0.4, final VISA-A of 89.1, subjective strength improvement following surgery of 78%, and 94% would recommend the procedure. V-Y group had 25 patients (28 ankles) with 74% subjective satisfaction, 21% complication rate, final VAS of 1.4, final VISA-A of 78.4, subjective strength improvement following surgery of 67%, and 84% would recommend the procedure. There was no significant difference in any of the results rates between the two groups (p > .05).
Conclusion
V-Y advancement is comparable to FHL transfer for the operative management of insertional Achilles tendinopathy. Though our results trend towards less satisfactory results following V-Y advancement, we found high satisfaction rates with similar functional outcomes and complication rates in both operative groups. We suggest considering V-Y advancement as a viable option for the primary treatment of chronic insertional Achilles tendinopathy in patients who may not be an ideal candidate for FHL transfer.



Similar content being viewed by others
References
Rahm S, Spross C, Gerber F et al (2013) Operative treatment of chronic irreparable Achilles tendon ruptures with large flexor hallucis longus tendon transfers. Foot ankle Int 34:1100–1110. https://doi.org/10.1177/1071100713487725
Hunt KJ, Cohen BE, Davis WH et al (2015) Surgical treatment of insertional Achilles tendinopathy with or without flexor Hallucis longus tendon transfer: a prospective, randomized study. Foot ankle Int 36:998–1005. https://doi.org/10.1177/1071100715586182
DeOrio MJ, Easley ME (2008) Surgical strategies: insertional Achilles tendinopathy. Foot Ankle Int 29:542–550. https://doi.org/10.3113/FAI.2008.0542
Wapner KL, Pavlock GS, Hecht PJ et al (1993) Repair of chronic Achilles tendon rupture with flexor hallucis longus tendon transfer. Foot Ankle 14:443–449
Silver RL, de la Garza J, Rang M (1985) The myth of muscle balance. A study of relative strengths and excursions of normal muscles about the foot and ankle. J Bone Joint Surg Br 67:432–437
Kissel CG, Blacklidge DK, Crowley DL (1994) Repair of neglected Achilles tendon ruptures—procedure and functional results. J Foot Ankle Surg 33:46–52
Abraham E, Pankovich AM (1975) Neglected rupture of the Achilles tendon. Treatment by V-Y tendinous flap. J Bone Joint Surg Am 57:253–255
Ponnapula P, Aaranson RR (2010) Reconstruction of Achilles tendon rupture with combined V-Y Plasty and gastrocnemius-soleus fascia turndown graft. J Foot Ankle Surg 49:310–315. https://doi.org/10.1053/j.jfas.2010.02.021
Elias I, Besser M, Nazarian LN, Raikin SM (2007) Reconstruction for missed or neglected Achilles tendon rupture with V-Y lengthening and flexor hallucis longus tendon transfer through one incision. Foot ankle Int 28:1238–1248. https://doi.org/10.3113/FAI.2007.1238
Carlsson AM (1983) Assessment of chronic pain. I. Aspects of the reliability and validity of the visual analogue scale. Pain 16:87–101. https://doi.org/10.1016/0304-3959(83)90088-X
Robinson JM, Cook JL, Purdam C et al (2001) The VISA-A questionnaire: a valid and reliable index of the clinical severity of Achilles tendinopathy. Br J Sports Med 35:335–341. https://doi.org/10.1136/bjsm.35.5.335
Tashjian RZ, Hur J, Sullivan RJ, Campbell JT (2003) Flexor hallucis longus transfer for repair of chronic Achilles tendinopathy. Foot Ankle Int 24:673–676. https://doi.org/10.1177/107110070302400306
Schon LC, Shores JL, Faro FD et al (2013) Flexor hallucis longus tendon transfer in treatment of Achilles tendinosis. J Bone Jt Surg Am 95:54–60. https://doi.org/10.2106/JBJS.K.00970
Monroe MT, Dixon DJ, Beals TC et al (2000) Plantarflexion torque following reconstruction of Achilles tendinosis or rupture with flexor hallucis longus augmentation. Foot ankle Int 21:324–329. https://doi.org/10.1177/107110070002100409
Wilcox DK, Bohay DR, Anderson JG (2000) Treatment of chronic Achilles tendon disorders with flexor hallucis longus tendon transfer/augmentation. Foot Ankle Int 21:1004–1010. https://doi.org/10.1046/j.1460-9584.2001.0261a.x
Martin RL, Manning CM, Carcia CR, Conti SF (2005) An outcome study of chronic Achilles tendinosis after excision of the Achilles tendon and flexor hallucis longus tendon transfer. Foot Ankle Int 26:691–697. https://doi.org/10.1177/107110070502600905
Cottom JM, Hyer CF, Berlet GC, Lee TH (2008) Flexor hallucis tendon transfer with an interference screw for chronic Achilles tendinosis: a report of 62 cases. Foot Ankle Spec 1:280–287. https://doi.org/10.1177/1938640008322690
McCormack J, Underwood F, Slaven E, Cappaert T (2015) The minimum clinically important difference on the VISA-A and LEFS for patients with insertional Achilles tendinopathy. Int J Sports Phys Ther 10:639–644
Iversen JV, Bartels EM, Langberg H (2012) The Victorian institute of sports assessment-Achilles questionnaire (VISA-A)—a reliable tool for measuring Achilles tendinopathy. Int J Sports Phys Ther 7:76–84. https://doi.org/10.1007/s40279-013-0096-z
Sayana MK, Maffulli N (2007) Eccentric calf muscle training in non-athletic patients with Achilles tendinopathy. J Sci Med Sport 10:52–58. https://doi.org/10.1016/j.jsams.2006.05.008
Coull R, Flavin R, Stephens MM (2003) Flexor hallucis longus tendon transfer: evaluation of postoperative morbidity. Foot ankle Int 24:931–934. https://doi.org/10.1177/107110070302401211
Hoenig JM, Heisey DM (2001) The abuse of power: the pervasive fallacy of power calculations for data analysis. Am Stat 55:19–24. https://doi.org/10.1198/000313001300339897
Acknowledgements
This work was presented at the Alabama Orthopaedic Society (AOS) 2017 but never published in the final form. We would also like to thank Girish Motwani, M.D., for his contributions to this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Institutional review board approval was obtained prior to this study.
Informed consent
For this type of study, formal consent was not required.
Rights and permissions
About this article
Cite this article
Staggers, J.R., Smith, K., de C. Netto, C. et al. Reconstruction for chronic Achilles tendinopathy: comparison of flexor hallucis longus (FHL) transfer versus V-Y advancement. International Orthopaedics (SICOT) 42, 829–834 (2018). https://doi.org/10.1007/s00264-018-3834-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-018-3834-x