Abstract
Purpose
Three-dimensional bioactive scaffolds are useful tools for stem cell implant in tissue-engineering. For chondral and subchondral repair, the chondroinductive and osteoinductive property of a scaffold is a major challenge. The scaffolds that aim to osteogenic differentiation have been well studied. However, cartilage cells can hardly be induced for osteogenesis, and monophase scaffolds cannot ideally repair both cartilage and subchondral defects at the same time.
Methods
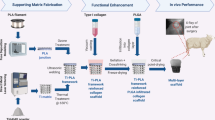
We developed a novel biphase composite scaffold and observe its application osteochondral defects. We combined the advantages of silk-fibroin/chitosan (SF/CS) scaffold in chondrogenic differentiation and the silk-fibroin/chitosan/nano-hydroxyapatite (SF/CS/nHA) scaffold in osteogenic differentiation and bone regeneration, and synthesized a SF/CS-SF/CS/nHA scaffold, which contained both the chondrocytic phase (SF/CS) and the osteoblastic phase (SF/CS/nHA).
Results
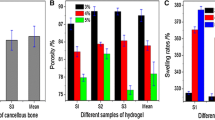
The biphase scaffold exhibited a porosity ratio around 90% and a water absorption ratio about 822%. A similar degradation property to traditional monophase scaffolds was observed. Bone mesenchymal stem cells (BMSCs) showed a good proliferation on this scaffold. Expression of two types of collagen was inducable for BMSCs on the scaffold. Neoformative extracellular matrix integrated with the scaffold was observed by the scanning electron microscope. When implanted in the lesion site in the rabbit femur with cartilage injury, mixing and filling function were exerted by the cell-scaffold constructs (CSCs). Micro-CT scanning revealed both chondral and subchondral layers were repaired. Moreover, type I and II collagens were both expressed in the implanted CSCs.
Conclusions
Chondral and subchondral repair can be achieved using the biphase scaffold implant that permits both chondrogenesis and osteogenesis from BMSCs. This approach has the potential to be clinically used for tissue engineering implantation.





Similar content being viewed by others
References
Langer R, Vacanti JP (1993) Tissue engineering. Science 260(5110):920–926
Thangavelu MRRN, Adithan A A C, Jong-Hoon K, Thotapalli Parvathaleswara S (2016) Reengineered graft copolymers as a potential alternative for the bone tissue engineering application by inducing osteogenic markers expression and biocompatibility. Colloids Surf B: Biointerfaces 143:15–26. doi:10.1016/j.colsurfb.2016.03.021
Li X, Yuan Z, Wei X, Li H, Zhao G, Miao J, Wu D, Liu B, Cao S, An D, Ma W, Zhang H, Wang W, Wang Q, Gu H (2016) Application potential of bone marrow mesenchymal stem cell (BMSCs) based tissue-engineering for spinal cord defect repair in rat fetuses with spina bifida aperta. J Mater Sci Mater Med 27(4):77. doi:10.1007/s10856-016-5684-7
Gentile P, Nandagiri VK, Daly J, Chiono V, Mattu C, Tonda-Turo C, Ciardelli G, Ramtoola Z (2016) Localised controlled release of simvastatin from porous chitosan-gelatin scaffolds engrafted with simvastatin loaded PLGA-microparticles for bone tissue engineering application. Mater Sci Eng C Mater Biol Appl 59:249–257. doi:10.1016/j.msec.2015.10.014
Orth P, Madry H (2015) Advancement of the Subchondral bone plate in translational models of osteochondral repair: implications for tissue engineering approaches. Tissue Eng B Rev 21(6):504–520. doi:10.1089/ten.TEB.2015.0122
Schroeder JE, Mosheiff R (2011) Tissue engineering approaches for bone repair: concepts and evidence. Injury 42(6):609–613. doi:10.1016/j.injury.2011.03.029
Kobayashi M, Spector M (2009) In vitro response of the bone marrow-derived mesenchymal stem cells seeded in a type-I collagen-glycosaminoglycan scaffold for skin wound repair under the mechanical loading condition. Mol Cell Biomech 6(4):217–227
Maraldi T, Riccio M, Pisciotta A, Zavatti M, Carnevale G, Beretti F, La Sala GB, Motta A, De Pol A (2013) Human amniotic fluid-derived and dental pulp-derived stem cells seeded into collagen scaffold repair critical-size bone defects promoting vascularization. Stem Cell Research & Therapy 4(3):53. doi:10.1186/scrt203
Wang Z, Li M, Yu B, Cao L, Yang Q, Su J (2012) Nanocalcium-deficient hydroxyapatite-poly (e-caprolactone)-polyethylene glycol-poly (e-caprolactone) composite scaffolds. Int J Nanomedicine 7:3123–3131. doi:10.2147/IJN.S31162
Silva SS, Motta A, Rodrigues MT, Pinheiro AF, Gomes ME, Mano JF, Reis RL, Migliaresi C (2008) Novel genipin-cross-linked chitosan/silk fibroin sponges for cartilage engineering strategies. Biomacromolecules 9(10):2764–2774. doi:10.1021/bm800874q
Gobin AS, Froude VE, Mathur AB (2005) Structural and mechanical characteristics of silk fibroin and chitosan blend scaffolds for tissue regeneration. J Biomed Mater res a 74(3):465–473. doi:10.1002/jbm.a.30382
Bhardwaj N, Kundu SC (2012) Chondrogenic differentiation of rat MSCs on porous scaffolds of silk fibroin/chitosan blends. Biomaterials 33(10):2848–2857. doi:10.1016/j.biomaterials.2011.12.028
Chen JP, Chen SH, Lai GJ (2012) Preparation and characterization of biomimetic silk fibroin/chitosan composite nanofibers by electrospinning for osteoblasts culture. Nanoscale res Lett 7(1):170. doi:10.1186/1556-276X-7-170
Budiraharjo R, Neoh KG, Kang ET (2012) Hydroxyapatite-coated carboxymethyl chitosan scaffolds for promoting osteoblast and stem cell differentiation. J Colloid Interface Sci 366(1):224–232. doi:10.1016/j.jcis.2011.09.072
Qi XN, Mou ZL, Zhang J, Zhang ZQ (2014) Preparation of chitosan/silk fibroin/hydroxyapatite porous scaffold and its characteristics in comparison to bi-component scaffolds. J Biomed Mater res a 102(2):366–372. doi:10.1002/jbm.a.34710
Arahira T, Todo M (2014) Effects of proliferation and differentiation of mesenchymal stem cells on compressive mechanical behavior of collagen/beta-TCP composite scaffold. J Mech Behav Biomed Mater 39:218–230. doi:10.1016/j.jmbbm.2014.07.013
Bornes TD, Jomha NM, Mulet-Sierra A, Adesida AB (2015) Hypoxic culture of bone marrow-derived mesenchymal stromal stem cells differentially enhances in vitro chondrogenesis within cell-seeded collagen and hyaluronic acid porous scaffolds. Stem Cell Res Ther 6:84. doi:10.1186/s13287-015-0075-4
Brix M, Kaipel M, Kellner R, Schreiner M, Apprich S, Boszotta H, Windhager R, Domayer S, Trattnig S (2016) Successful osteoconduction but limited cartilage tissue quality following osteochondral repair by a cell-free multilayered nano-composite scaffold at the knee. Int Orthop 40(3):625–632. doi:10.1007/s00264-016-3118-2
Araki S, Imai S, Ishigaki H, Mimura T, Nishizawa K, Ueba H, Kumagai K, Kubo M, Mori K, Ogasawara K, Matsusue Y (2015) Improved quality of cartilage repair by bone marrow mesenchymal stem cells for treatment of an osteochondral defect in a cynomolgus macaque model. Acta Orthop 86(1):119–126. doi:10.3109/17453674.2014.958807
Filardo G, Kon E, Perdisa F, Balboni F, Marcacci M (2014) Autologous osteochondral transplantation for the treatment of knee lesions: results and limitations at two years’ follow-up. Int Orthop 38(9):1905–1912. doi:10.1007/s00264-014-2322-1
Verhaegen J, Clockaerts S, Van Osch GJ, Somville J, Verdonk P, Mertens P (2015) TruFit plug for repair of Osteochondral defects-where is the evidence? Systematic review of literature. Cartilage 6(1):12–19. doi:10.1177/1947603514548890
Niethammer TR, Holzgruber M, Gulecyuz MF, Weber P, Pietschmann MF, Muller PE (2017) Matrix based autologous chondrocyte implantation in children and adolescents: a match paired analysis in a follow-up over three years post-operation. Int Orthop 41(2):343–350. doi:10.1007/s00264-016-3321-1
De Caro F, Bisicchia S, Amendola A, Ding L (2015) Large fresh osteochondral allografts of the knee: a systematic clinical and basic science review of the literature. Arthroscopy 31(4):757–765. doi:10.1016/j.arthro.2014.11.025
Astur DC, Arliani GG, Binz M, Astur N, Kaleka CC, Amaro JT, Pochini A, Cohen M (2014) Autologous osteochondral transplantation for treating patellar chondral injuries: evaluation, treatment, and outcomes of a two-year follow-up study. J Bone Joint Surg am 96(10):816–823. doi:10.2106/JBJS.M.00312
Seo JY, Ha KY, Kim YH, Ahn JH (2016) Foreign body reaction after implantation of a device for intervertebral assisted motion. J Korean Neurosurg Soc 59(6):647–649. doi:10.3340/jkns.2016.59.6.647
Grassel S, Lorenz J (2014) Tissue-engineering strategies to repair chondral and osteochondral tissue in osteoarthritis: use of mesenchymal stem cells. Curr Rheumatol rep 16(10):452. doi:10.1007/s11926-014-0452-5
Volz M, Schaumburger J, Frick H, Grifka J, Anders S (2017) A randomized controlled trial demonstrating sustained benefit of autologous matrix-induced Chondrogenesis over microfracture at five years. Int Orthop 41(4):797–804. doi:10.1007/s00264-016-3391-0
Hofmann S, Knecht S, Langer R, Kaplan DL, Vunjak-Novakovic G, Merkle HP, Meinel L (2006) Cartilage-like tissue engineering using silk scaffolds and mesenchymal stem cells. Tissue Eng 12(10):2729–2738. doi:10.1089/ten.2006.12.2729
Jakobsen RB, Shahdadfar A, Reinholt FP, Brinchmann JE (2010) Chondrogenesis in a hyaluronic acid scaffold: comparison between chondrocytes and MSC from bone marrow and adipose tissue. Knee Surg Sports Traumatol Arthrosc 18(10):1407–1416. doi:10.1007/s00167-009-1017-4
Zavan B, Giorgi C, Bagnara GP, Vindigni V, Abatangelo G, Cortivo R (2007) Osteogenic and chondrogenic differentiation: comparison of human and rat bone marrow mesenchymal stem cells cultured into polymeric scaffolds. Eur J Histochem 51(Suppl 1):1–8
Stadler N, Trieb K (2016) Osteochondritis dissecans of the medial femoral condyle: new cell-free scaffold as a treatment option. Orthopade 45(8):701–705. doi:10.1007/s00132-016-3267-4
Algul D, Gokce A, Onal A, Servet E, Dogan Ekici AI, Yener FG (2016) In vitro release and in vivo biocompatibility studies of biomimetic multilayered alginate-chitosan/beta-TCP scaffold for osteochondral tissue. J Biomater Sci Polym Ed 27(5):431–440. doi:10.1080/09205063.2016.1140501
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest.
Funding
The research was financially supported by the Science and technology plan projects in Guizhou province (grant number:[2016]1420).
The research was financially supported by a grant from the National Natural Science Foundation of China (grant number: 81,660,367).
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Ruan, Sq., Yan, L., Deng, J. et al. Preparation of a biphase composite scaffold and its application in tissue engineering for femoral osteochondral defects in rabbits. International Orthopaedics (SICOT) 41, 1899–1908 (2017). https://doi.org/10.1007/s00264-017-3522-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-017-3522-2