Abstract
Purpose
The purpose of this study was to review all cases of patients submitted to Westin’s tenodesis, who had calcaneus feet secondary to myelomeningocele sequel, in order to evaluate the anatomical change provided by surgery and also to verify, in a long-term follow-up, the inversion of the deformity depending on the patient’s age.
Methods
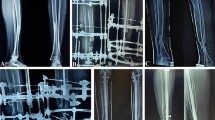
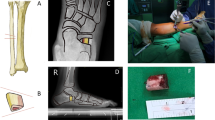
In this longitudinal retrospective study, all medical records of patients with myelomeningocele sequelae submitted to Westin’s tenodesis from 1993 to 2013 in a public university hospital were reviewed. Patients were contacted for new clinical and radiographic evaluations after a minimum of 36 months after surgery. The calcaneotibial angle was measured and the shortening of the fibula was calculated as the "intermalleolar height".
Results
The study was based on 16 children (26 feet), aged 84.27 months on average at the time of tenodesis. The calcaneotibial angle increased significantly post-operatively, from 63.77 degrees on average to 70.54 degrees. Intermalleolar height and valgus ankle did not change significantly. Most patients had plantigrade feet after surgery, without pressure ulcers, and were able to use orthoses.
Conclusion
Westin’s tenodesis, with or without other associated procedures, can correct or improve the calcaneus and valgus ankle deformity in patients with myelomeningocele sequelae. There was no association of the surgical result with age at the time of surgery. There was no inversion of the deformity in equinus during the follow-up time.




Similar content being viewed by others
References
Westin GW (1965) Tendon transfers about the foot, ankle, and hip in the paralyzed lower extremity. J Bone Joint Surg Am 47(7):1430–1443
Westin GW, Dingeman RD, Gausewitz SH (1988) The results of tenodesis of tendo achilles to the fibula for paralytic pes calcaneus. J Bone Joint Surg Am 70(3):320–328
Fucs PM, Svartman C, Santili C, De Assumpção RM, de Almeida Leite LF, Quialheiro LS et al (2007) Results in the treatment of paralytic calcaneus-valgus feet with the Westin technique. Int Orthop 31(4):555560
Bliss DG, Menelaus MB (1986) The results of transfer of tibialis anterior to the heel in patients who have a myelomeningocele. J Bone Joint Surg Am 68(8):1258–1264
Hayes JT, Gross HP, Dow S (1964) Surgery for paralytic defects secondary to myelomeningocele and myelodysplasia. J Bone Joint Surg Am 46:1577–1597
Akbar M, Bresch B, Seyler TM, Wenz W, Bruckner T, Abel R et al (2009) Management of orthopaedic sequelae of congenital spinal disorders. J Bone Joint Surg Am 91(Suppl 6):87–100
Swaroop VT, Dias L (2011) Orthopaedic management of spina bifida-part II: foot and ankle deformities. J Child Orthop 5(6):403–414
Park KB, Park HW, Joo SY, Kim HW (2008) Surgical treatment of calcaneal deformity in a select group of patients with myelomeningocele. J Bone Joint Surg Am 90(10):2149–2159
Frischhut B, Stöckl B, Landauer F, Krismer M, Menardi G (2000) Foot deformities in adolescents and young adults with spina bifida. J Pediatr Orthop B 9(3):161–169
Sharrard WJ, Gorsfield I (1968) The management of deformity and paralysis of the foot in myelomeningocele. J Bone Joint Surg (Br) 50(3):456–465
Sharrard WJ (1967) Paralytic deformity in the lower limb. J Bone Joint Surg (Br) 49(4):731–747
Janda JP, Skinner SR, Barto PS (1984) Posterior transfer of tibialis anterior in low-level myelodysplasia. Dev Med Child Neurol 26(1):100–103
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
PLATAFORMA BRASIL (http://aplicacao.saude.gov.br/plataformabrasil)
Funding
No funding was received for this study.
Conflict of interest
All authors declare they have no competing interests.
Additional information
This study was conducted at the Orthopaedic Department, Santa Casa Medical School and Hospitals, São Paulo, Brazil.
Rights and permissions
About this article
Cite this article
Yamada, H.H., Fucs, P.M. Long-term results of fibular-Achilles tenodesis (Westin’s tenodesis) for paralytic pes calcaneus: is hypercorrection avoidable? A longitudinal retrospective study. International Orthopaedics (SICOT) 41, 1641–1646 (2017). https://doi.org/10.1007/s00264-017-3458-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-017-3458-6