Abstract
Purpose
We aimed to identify the incidence and preventability rate of adverse events (AEs) occurring in a specialty orthopaedic unit.
Methods
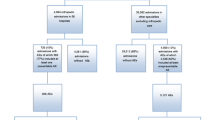
Four thousand nine hundred and six consecutive in-patient admissions over six months in an orthopaedic unit were prospectively analysed. The total indoor patient capacity was segregated into 25-bed units each, and AEs were recorded on a daily basis by two observers. Each event was assessed by allotting a causation score (1–6), with a score of ≥ 4 implying a systemic/individual failure of healthcare provision. A preventability score (1–6) was allotted and scores ≥ 4 were considered to be preventable.
Results
Four hundred and sixty-seven patients (9.5 %) suffered a total of 529 AEs, including 127 readmissions; 49 patients suffering multiple events. Three hundred and thirty-three (62.9 %) events had a causation score of ≥ 4, indicating a failure of healthcare delivery systems. Three hundred and one (56.8 %) events could have been prevented with better regulation and adherence to management protocols. Hospital-acquired infections were the most common event, with surgical-site infection in 102 cases (19.2 and 2 % overall) and catheter-associated urinary tract infections noted in 45 (8.5 %) patients. Medical events included seven deep vein thrombosis, two pulmonary embolisms, five myocardial infarctions and one stroke. AEs occurred 56.3 % in the ward, 4.3 % in the intensive care unit (ICU), 6.2 % in the emergency room, and 9.0 % in the operating theatre.
Conclusion
This prospective study documented an adverse event rate of 9.5 %, of which 56 % were preventable. AEs occurred in all stages of treatment care, emphasising the need for vigilance during the entire treatment process.
Similar content being viewed by others
References
Thomas EJ, Studdert DM, Runciman WB, Webb RK, Sexton EJ, Wilson RM, Gibberd RW, Harrison BE, Brennan TA (2000) A comparison of iatrogenic injury studies in Australia and the USA I: context, methods, casemix, population, patient and hospital characteristics. Int J Qual Health Care 12(5):371–378
Leape LL, Brennan TA, Laird N, Lawthers AG, Localio AR, Barnes BA, Hebert L, Newhouse JP, Weiler PC, Hiatt H (1991) The nature of adverse events in hospitalized patients: results of the Harvard Medical Practice Study II. N Engl J Med 324(6):377–384
Brennan TA, Leape LL, Laird NM, Hebert L, Localio AR, Lawthers AG, Newhouse JP, Weiler PC, Hiatt HH (1991) Incidence of adverse events and negligence in hospitalized patients: results of the Harvard Medical Practice Study I. N Engl J Med 324(6):370–376
Thomas EJ, Studdert DM, Burstin HR, Orav EJ, Zeena T, Williams EJ, Howard KM, Weiler PC, Brennan TA (2000) Incidence and types of adverse events and negligent care in Utah and Colorado. Med Care 38(3):261–271
Wilson RM, Runciman WB, Gibberd RW, Harrison BT, Newby L, Hamilton JD (1995) The quality in Australian health care study. Med J Austral 163(9):458–471
Kable AK, Gibberd RW, Spigelman AD (2002) Adverse events in surgical patients in Australia. Int J Qual Health Care 14(4):269–276
Davis P, Lay-Yee R, Briant R, Ali W, Scott A, Schug S (2003). Adverse events in New Zealand public hospitals II: preventability and clinical context. NZ Med J (online), 116(1183)
Baker GR, Norton PG, Flintoft V, Blais R, Brown A, Cox J, Etchells E, Ghali WA, Hébert P, Majumdar SR, O’Beirne M (2004) The Canadian adverse events study: the incidence of adverse events among hospital patients in Canada. Can Med Assoc J 170(11):1678–1686
deVries EN, Ramrattan MA, Smorenburg SM, Gouma DJ, Boermeester MA (2008) The incidence and nature of in-hospital adverse events: a systematic review. Qual Saf Health Care 17(3):216–223
Thomas EJ, Studdert DM, Newhouse JP, Zbar BI, Howard KM, Williams EJ, Brennan TA (1999) Costs of medical injuries in Utah and Colorado. Inquiry, 255–264
Vincent C, Neale G, Woloshynowych M (2001) Adverse events in British hospitals: preliminary retrospective record review. BMJ 322(7285):517–519
Forster AJ, Asmis TR, Clark HD, Al Saied G, Code CC, Caughey SC, Baker K, Watters J, Worthington J, Van Walraven C (2004) Ottawa Hospital Patient Safety Study: incidence and timing of adverse events in patients admitted to a Canadian teaching hospital. Can Med Assoc J 170(8):1235–1240
Neale G, Woloshynowych M, Vincent C (2001) Exploring the causes of adverse events in NHS hospital practice. J R Soc Med 94(7):322–330
Unbeck M, Muren O, Lillkrona U (2008) Identification of adverse events at an orthopedics department in Sweden. Acta Orthop 79(3):396–403
Sadat-Ali M, Abdallah S, Mohammed Q (2012) Identification of adverse events in orthopaedic practice: a step towards quality care. Acta Orthop Belg 78(5):582
Öhrn A, Elfström J, Tropp H, Rutberg H (2012) What can we learn from patient claims? a retrospective analysis of incidence and patterns of adverse events after orthopaedic procedures in Sweden. Patient Saf Surg 6(2), P.1
Bellomo R, Goldsmith D, Russell S, Uchino S (2002) Postoperative serious adverse events in a teaching hospital: a prospective study. Med J Aust 176(5):216–218
Michel P, Quenon JL, de Sarasqueta AM, Scemama O (2004) Comparison of three methods for estimating rates of adverse events and rates of preventable adverse events in acute care hospitals. BMJ 328(7433):199
Sari ABA, Sheldon TA, Cracknell A, Turnbull A (2007) Sensitivity of routine system for reporting patient safety incidents in an NHS hospital: retrospective patient case note review. BMJ 334(7584):79
O’Neil AC, Petersen LA, Cook EF, Bates DW, Lee TH, Brennan TA (1993) Physician reporting compared with medical-record review to identify adverse medical events. Ann Intern Med 119(5):370–376
Wong DA, Herndon JH, Canale ST, Brooks RL, Hunt TR, Epps HR, Fountain SS, Albanese SA, Johanson NA (2009) Medical errors in orthopaedics. J Bone Joint Surg 91(3):547–557
Smits M, Zegers M, Groenewegen PP, Timmermans DRM, Zwaan L, Van der Wal G, Wagner C (2010) Exploring the causes of adverse events in hospitals and potential prevention strategies. Qual Saf Health Care 19(5):1–7
Anderson DJ, Sexton DJ, Kanafani ZA, Auten G, Kaye KS (2007) Severe surgical site infection in community hospitals: epidemiology, key procedures, and the changing prevalence of methicillin-resistant Staphylococcus aureus. Infect Contrl Hospital Epidemiol 28(09):1047–1053
Cruse P (1981) Wound infection surveillance. Rev Infect Dis 3(4):734–737
Scott RD (2009) The direct medical costs of healthcare-associated infections in US hospitals and the benefits of prevention. Division of Healthcare Quality Promotion National Center for Preparedness, Detection, and Control of Infectious Diseases, Centers for Disease Control and Prevention
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
Ganga Orthopaedic Research & Education Foundation, Coimbatore.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical considerations
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Rajasekaran, S., Ravi, S. & Aiyer, S.N. Incidence and preventability of adverse events in an orthopaedic unit: a prospective analysis of four thousand, nine hundred and six admissions. International Orthopaedics (SICOT) 40, 2233–2238 (2016). https://doi.org/10.1007/s00264-016-3282-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-016-3282-4