Abstract
Purpose
In autologous osteochondral transplantation, the edges of the harvested plug are particularly susceptible to mechanical or thermal damage to the chondrocytes. We hypothesised that the applied harvesting device has an impact on chondrocyte vitality.
Methods
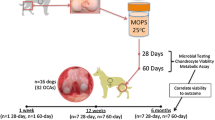
Both knees of five blackhead sheep (ten knees) underwent open osteochondral plug harvesting with three different circular harvesting devices (osteoarticular transfer system harvester [OATS; diameter 8 mm; Arthrex, Munich, Germany], diamond cutter [DC; diameter 8.35 mm; Karl Storz, Tuttlingen, Germany] and hollow reamer with cutting crown [HRCC; diameter 7 mm; Dannoritzer, Tuttlingen, Germany]) from distinctly assigned anatomical sites of the knee joint. The rotary cutters (DC and HRCC) were either used with (+) or without cooling (−). Surgical cuts of the cartilage with a scalpel blade were chosen as control method. After cryotomy cutting, chondrocyte vitality was assessed using fluorescence microscopy and a Live/Dead assay.
Results
There were distinct patterns of chondrocyte vitality, with reproducible accumulations of dead chondrocytes along the harvesting edge. No statistical difference in chondrocyte survivorship was seen between the OATS technique and the control method, or between the HRCC+ technique and the control method (P > 0.05). The DC+, HRCC− and DC− techniques yielded significantly lower chondrocyte survival rates compared with the control method (P < 0.05).
Conclusions
Chondrocyte survival in osteochondral cylinders depends on the applied harvesting technique. The use of rotary cutters without cooling yielded worst results, while the traditional OATS punch and rotary cutters with cooling achieved comparable rates of chondrocyte vitality.




Similar content being viewed by others
References
Badekas T, Takvorian M, Souras N (2013) Treatment principles for osteochondral lesions in foot and ankle. Int Orthop 37:1697–1706. doi:10.1007/s00264-013-2076-1
Biant LC, Bentley G, Vijayan S, Skinner JA, Carrington RW (2014) Long-term results of autologous chondrocyte implantation in the knee for chronic chondral and osteochondral defects. Am J Sports Med 42:2178–2183. doi:10.1177/0363546514539345
Buda R, Vannini F, Castagnini F, Cavallo M, Ruffilli A, Ramponi L, Pagliazzi G, Giannini S (2015) Regenerative treatment in osteochondral lesions of the talus: autologous chondrocyte implantation versus one-step bone marrow derived cells transplantation. Int Orthop 39:893–900. doi:10.1007/s00264-015-2685-y
Chiang H, Liao CJ, Hsieh CH, Shen CY, Huang YY, Jiang CC (2013) Clinical feasibility of a novel biphasic osteochondral composite for matrix-associated autologous chondrocyte implantation. Osteoarthr Cartil 21:589–598. doi:10.1016/j.joca.2013.01.004
Evans PJ, Miniaci A, Hurtig MB (2004) Manual punch versus power harvesting of osteochondral grafts. Arthroscopy 20:306–310. doi:10.1016/j.arthro.2004.01.012
Filardo G, Kon E, Perdisa F, Balboni F, Marcacci M (2014) Autologous osteochondral transplantation for the treatment of knee lesions: results and limitations at two years’ follow-up. Int Orthop 38:1905–1912. doi:10.1007/s00264-014-2322-1
Gagala J, Tarczynska M, Gaweda K (2013) Clinical and radiological outcomes of treatment of avascular necrosis of the femoral head using autologous osteochondral transfer (mosaicplasty): preliminary report. Int Orthop 37:1239–1244. doi:10.1007/s00264-013-1893-6
Hangody L, Vasarhelyi G, Hangody LR, Sukosd Z, Tibay G, Bartha L, Bodo G (2008) Autologous osteochondral grafting—technique and long-term results. Injury 39(Suppl 1):S32–S39. doi:10.1016/j.injury.2008.01.041
Horas U, Pelinkovic D, Herr G, Aigner T, Schnettler R (2003) Autologous chondrocyte implantation and osteochondral cylinder transplantation in cartilage repair of the knee joint. A prospective, comparative trial. J Bone Joint Surg Am 85-A:185–192
Huntley JS, Bush PG, McBirnie JM, Simpson AH, Hall AC (2005) Chondrocyte death associated with human femoral osteochondral harvest as performed for mosaicplasty. J Bone Joint Surg Am 87:351–360
Karataglis D, Green MA, Learmonth DJ (2006) Autologous osteochondral transplantation for the treatment of chondral defects of the knee. Knee 13:32–35
Kircher J, Patzer T, Magosch P, Lichtenberg S, Habermeyer P (2009) Osteochondral autologous transplantation for the treatment of full-thickness cartilage defects of the shoulder: results at nine years. J Bone Joint Surg (Br) 91:499–503. doi:10.1302/0301-620X.91B4.21838
Kock NB, Hannink G, van Kampen A, Verdonschot N, van Susante JL, Buma P (2011) Evaluation of subsidence, chondrocyte survival and graft incorporation following autologous osteochondral transplantation. Knee Surg Sports Traumatol Arthrosc 19:1962–1970. doi:10.1007/s00167-011-1650-6
McGregor AJ, Amsden BG, Waldman SD (2011) Chondrocyte repopulation of the zone of death induced by osteochondral harvest. Osteoarthr Cartil 19:242–248. doi:10.1016/j.joca.2010.11.008
Petri M, Broese M, Simon A, Liodakis E, Ettinger M, Guenther D, Zeichen J, Krettek C, Jagodzinski M, Haasper C (2013) CaReS (MACT) versus microfracture in treating symptomatic patellofemoral cartilage defects: a retrospective matched-pair analysis. J Orthop Sci 18:38–44. doi:10.1007/s00776-012-0305-x
Petri M, Ettinger M, von Falck C, Hawi N, Jagodzinski M, Haasper C (2013) Reconstruction of osteochondral defects by combined bone grafting and a bilayer collagen membrane as a sandwich technique. Orthop Rev (Pavia) 5, e36. doi:10.4081/or.2013.e36
Sasaki K, Matsumoto T, Matsushita T, Kubo S, Ishida K, Tei K, Akisue T, Kurosaka M, Kuroda R (2012) Osteochondral autograft transplantation for juvenile osteochondritis dissecans of the knee: a series of twelve cases. Int Orthop 36:2243–2248. doi:10.1007/s00264-012-1648-9
Vogt S, Siebenlist S, Hensler D, Weigelt L, Ansah P, Woertler K, Imhoff AB (2011) Osteochondral transplantation in the elbow leads to good clinical and radiologic long-term results: an 8- to 14-year follow-up examination. Am J Sports Med 39:2619–2625. doi:10.1177/0363546511420127
Weigelt L, Siebenlist S, Hensler D, Imhoff AB, Vogt S (2015) Treatment of osteochondral lesions in the elbow: results after autologous osteochondral transplantation. Arch Orthop Trauma Surg 135:627–634. doi:10.1007/s00402-015-2204-z
Woelfle JV, Reichel H, Nelitz M (2013) Indications and limitations of osteochondral autologous transplantation in osteochondritis dissecans of the talus. Knee Surg Sports Traumatol Arthrosc 21:1925–1930. doi:10.1007/s00167-013-2483-2
Acknowledgments
The surgical materials for this study were donated by Arthrex (Munich, Germany), Karl Storz (Tuttlingen, Germany) and Dannoritzer (Tuttlingen, Germany).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Benedikt Hafke and Maximilian Petri contributed equally to this work
Rights and permissions
About this article
Cite this article
Hafke, B., Petri, M., Suero, E. et al. Chondrocyte survival in osteochondral transplant cylinders depends on the harvesting technique. International Orthopaedics (SICOT) 40, 1553–1558 (2016). https://doi.org/10.1007/s00264-015-3065-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-015-3065-3