Abstract
Background
Femoral neck fractures are frequent in the elderly population and lead to high morbidity and mortality. Hemiarthroplasty is an established surgical procedure for displaced intracapsular femoral neck fractures. Post-operative infection is frequent and is potentially devastating for the patient and the healthcare services. The goal of this study was to identify the risk factors of infection after hemiarthroplasty and help adapt our surgical practice.
Methods
A systematic review of the literature was performed in July 2015 by two authors using the MedLine, PubMed and Cochrane databases. We used the MeSH keywords “hip hemiarthroplasty” AND “infection” to identify risk factors and methods of prevention for surgical site infection after hemiarthroplasty. Following the search, two authors independently performed the first stage based on titles and abstracts.
Results
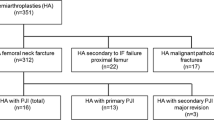
Thirty-seven articles were selected. Review and analysis of the references was performed to find other articles of interest. Thirteen articles were selected to analyse. According to literature, the surgical site infection (SSI) rate after hip hemiarthroplasty (HHA) is between 1.7 and 7.3 %. Pre-operative comorbidities (obesity, liver disease, advanced age), operative conditions (junior surgeon, uncemented stems, time of surgery) and post-operative management (length of hospitalisation, haematoma, prolonged wound drainage and two urinary catheterisations) were identified as risk factors of surgical site infection. Authors describe conditions to decrease the incidence of these complications and underline the importance of “a specialised hip team” that provides fast care and helps decrease the duration of hospitalisation.
Conclusions
Careful patient management for hemiarthroplasty is vital and may decrease the incidence of surgical site infection, which is associated with high morbidity and high procedure cost. Our review suggests that there are specific correctable risk factors for SSIs after HHA. Being able to identify these risk factors leads to better care because of SSI prevention in patients undergoing HHAs after femoral neck fractures. To improve the outcomes, some methods of prevention of surgical site infection are available: before, during and after the operation.
Study design
Review of literature. Level of evidence: IV

Similar content being viewed by others
References
Schmidt AH, Swiontkowski MF (2002) Femoral neck fractures. Orthop Clin N Am 33(1):97–111, viii
Nather A, Seow CS, Iau P, Chan A (1995) Morbidity and mortality for elderly patients with fractured neck of femur treated by hemiarthroplasty. Injury 26(3):187–190
Sullivan NP, Hughes AW, Halliday RL, Ward AL, Chesser TJ (2015) Early complications following cemented modular hip hemiarthroplasty. Open Orthop J 9:15–19. doi:10.2174/1874325001509010015
Sprowson AP, Jensen CD, Gupta S, Parsons N, Murty AN, Jones SM, Inman D, Reed MR (2013) The effect of high dose antibiotic impregnated cement on rate of surgical site infection after hip hemiarthroplasty for fractured neck of femur: a protocol for a double-blind quasi randomised controlled trial. BMC Musculoskelet Disord 14:356. doi:10.1186/1471-2474-14-356
Gao H, Liu Z, Xing D, Gong M (2012) Which is the best alternative for displaced femoral neck fractures in the elderly?: A meta-analysis. Clin Orthop Relat Res 470(6):1782–1791. doi:10.1007/s11999-012-2250-6
Bhandari M, Devereaux PJ, Einhorn TA, Thabane L, Schemitsch EH, Koval KJ, Frihagen F, Poolman RW, Tetsworth K, Guerra-Farfan E, Madden K, Sprague S, Guyatt G, Investigators H (2015) Hip fracture evaluation with alternatives of total hip arthroplasty versus hemiarthroplasty (HEALTH): protocol for a multicentre randomised trial. BMJ Open 5(2):e006263. doi:10.1136/bmjopen-2014-006263
Liu Y, Tao X, Wang P, Zhang Z, Zhang W, Qi Q (2014) Meta-analysis of randomised controlled trials comparing unipolar with bipolar hemiarthroplasty for displaced femoral-neck fractures. Int Orthop 38(8):1691–1696. doi:10.1007/s00264-014-2355-5
Schneppendahl J, Grassmann JP, Petrov V, Bottner F, Korbl B, Hakimi M, Betsch M, Windolf J, Wild M (2012) Decreasing mortality after femoral neck fracture treated with bipolar hemiarthroplasty during the last twenty years. Int Orthop 36(10):2021–2026. doi:10.1007/s00264-012-1600-z
Varley J, Parker MJ (2004) Stability of hip hemiarthroplasties. Int Orthop 28(5):274–277. doi:10.1007/s00264-004-0572-z
Clohisy JC, Calvert G, Tull F, McDonald D, Maloney WJ (2004) Reasons for revision hip surgery: a retrospective review. Clin Orthop Relat Res 429:188–192
Alazzawi S, Sprenger De Rover WB, Brown J, Davis B (2012) The conversion rate of bipolar hemiarthroplasty after a hip fracture to a total hip arthroplasty. Clin Orthop Surg 4(2):117–120. doi:10.4055/cios.2012.4.2.117
Gjertsen JE, Lie SA, Vinje T, Engesaeter LB, Hallan G, Matre K, Furnes O (2012) More re-operations after uncemented than cemented hemiarthroplasty used in the treatment of displaced fractures of the femoral neck: an observational study of 11,116 hemiarthroplasties from a national register. J Bone Joint Surg (Br) 94(8):1113–1119. doi:10.1302/0301-620X.94B8.29155
Fichman SG, Makinen TJ, Vincent A, Lozano B, Safir O, Kuzyk PR (2015) Complications following conversion of a hip hemiarthroplasty to a total hip arthroplasty. Int Orthop. doi:10.1007/s00264-015-2827-2
Burgers PT, Van Lieshout EM, Verhelst J, Dawson I, de Rijcke PA (2014) Implementing a clinical pathway for hip fractures; effects on hospital length of stay and complication rates in five hundred and twenty six patients. Int Orthop 38(5):1045–1050. doi:10.1007/s00264-013-2218-5
Warwick D, Hubble M, Sarris I, Strange J (1998) Revision of failed hemiarthroplasty for fractures at the hip. Int Orthop 22(3):165–168
Tidermark J, Ponzer S, Svensson O, Soderqvist A, Tornkvist H (2003) Internal fixation compared with total hip replacement for displaced femoral neck fractures in the elderly. A randomised, controlled trial. J Bone Joint Surg (Br) 85(3):380–388
Rogmark C, Johnell O (2006) Primary arthroplasty is better than internal fixation of displaced femoral neck fractures: a meta-analysis of 14 randomized studies with 2,289 patients. Acta Orthop 77(3):359–367. doi:10.1080/17453670610046262
Edwards C, Counsell A, Boulton C, Moran CG (2008) Early infection after hip fracture surgery: risk factors, costs and outcome. J Bone Joint Surg (Br) 90(6):770–777. doi:10.1302/0301-620X.90B6.20194
Blewitt N, Mortimore S (1992) Outcome of dislocation after hemiarthroplasty for fractured neck of the femur. Injury 23(5):320–322
Cordero-Ampuero J, de Dios M (2010) What are the risk factors for infection in hemiarthroplasties and total hip arthroplasties? Clin Orthop Relat Res 468(12):3268–3277. doi:10.1007/s11999-010-1411-8
Gaynes RP (1997) Surveillance of nosocomial infections: a fundamental ingredient for quality. Infect Control Hosp Epidemiol 18(7):475–478
Ridgeway S, Wilson J, Charlet A, Kafatos G, Pearson A, Coello R (2005) Infection of the surgical site after arthroplasty of the hip. J Bone Joint Surg (Br) 87(6):844–850. doi:10.1302/0301-620X.87B6.15121
Wright RW, Brand RA, Dunn W, Spindler KP (2007) How to write a systematic review. Clin Orthop Relat Res 455:23–29. doi:10.1097/BLO.0b013e31802c9098
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097. doi:10.1371/journal.pmed.1000097
Wright JG, Swiontkowski MF, Heckman JD (2003) Introducing levels of evidence to the journal. J Bone Joint Surg Am 85-A(1):1–3
Dale H, Skramm I, Lower HL, Eriksen HM, Espehaug B, Furnes O, Skjeldestad FE, Havelin LI, Engesaeter LB (2011) Infection after primary hip arthroplasty: a comparison of 3 Norwegian health registers. Acta Orthop 82(6):646–654. doi:10.3109/17453674.2011.636671
Jameson SS, Jensen CD, Elson DW, Johnson A, Nachtsheim C, Rangan A, Muller SD, Reed MR (2013) Cemented versus cementless hemiarthroplasty for intracapsular neck of femur fracture—a comparison of 60,848 matched patients using national data. Injury 44(6):730–734. doi:10.1016/j.injury.2012.10.031
Leonardsson O, Karrholm J, Akesson K, Garellick G, Rogmark C (2012) Higher risk of reoperation for bipolar and uncemented hemiarthroplasty. Acta Orthop 83(5):459–466. doi:10.3109/17453674.2012.727076
Lau AC, Neo GH, Lee HC (2014) Risk factors of surgical site infections in hip hemiarthroplasty: a single-institution experience over nine years. Singap Med J 55(10):535–538
Cumming D, Parker MJ (2007) Urinary catheterisation and deep wound infection after hip fracture surgery. Int Orthop 31(4):483–485. doi:10.1007/s00264-006-0227-3
Johnson B, Starks I, Bancroft G, Roberts PJ (2012) The effect of care bundle development on surgical site infection after hemiarthroplasty: an 8-year review. J Trauma Acute Care Surg 72(5):1375–1379. doi:10.1097/TA.0b013e318245267c
Acklin YP, Widmer AF, Renner RM, Frei R, Gross T (2011) Unexpectedly increased rate of surgical site infections following implant surgery for hip fractures: problem solution with the bundle approach. Injury 42(2):209–216. doi:10.1016/j.injury.2010.09.039
Duckworth AD, Phillips SA, Stone O, Moran M, Breusch SJ, Biant LC (2012) Deep infection after hip fracture surgery: predictors of early mortality. Injury 43(7):1182–1186. doi:10.1016/j.injury.2012.03.029
Harrison T, Robinson P, Cook A, Parker MJ (2012) Factors affecting the incidence of deep wound infection after hip fracture surgery. J Bone Joint Surg (Br) 94(2):237–240. doi:10.1302/0301-620X.94B1.27683
Shah SN, Wainess RM, Karunakar MA (2005) Hemiarthroplasty for femoral neck fracture in the elderly surgeon and hospital volume-related outcomes. J Arthroplasty 20(4):503–508. doi:10.1016/j.arth.2004.03.025
Frihagen F, Madsen JE, Aksnes E, Bakken HN, Maehlum T, Walloe A, Nordsletten L (2007) Comparison of re-operation rates following primary and secondary hemiarthroplasty of the hip. Injury 38(7):815–819. doi:10.1016/j.injury.2006.09.020
Lora-Tamayo J, Euba G, Ribera A, Murillo O, Pedrero S, Garcia-Somoza D, Pujol M, Cabo X, Ariza J (2013) Infected hip hemiarthroplasties and total hip arthroplasties: differential findings and prognosis. J Infect 67(6):536–544. doi:10.1016/j.jinf.2013.07.030
del Toro MD, Nieto I, Guerrero F, Corzo J, del Arco A, Palomino J, Nuno E, Lomas JM, Natera C, Fajardo JM, Delgado J, Torres-Tortosa M, Romero A, Martin-Rico P, Muniain MA, Rodriguez-Bano J, group P-SR (2014) Are hip hemiarthroplasty and total hip arthroplasty infections different entities? The importance of hip fractures. Eur J Clin Microbiol Infect Dis 33(8):1439–1448. doi:10.1007/s10096-014-2091-1
Haley RW (1985) Surveillance by objective: a new priority-directed approach to the control of nosocomial infections. The National Foundation for Infectious Diseases lecture. Am J Infect Control 13(2):78–89
Southwell-Keely JP, Russo RR, March L, Cumming R, Cameron I, Brnabic AJ (2004) Antibiotic prophylaxis in hip fracture surgery: a metaanalysis. Clin Orthop Relat Res 419:179–184
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR (1999) Guideline for Prevention of Surgical Site Infection, 1999. Centers for Disease Control and Prevention (CDC) Hospital Infection Control Practices Advisory Committee. Am J Infect Control 27(2):97–132, quiz 133-134; discussion 196
Leong G, Wilson J, Charlett A (2006) Duration of operation as a risk factor for surgical site infection: comparison of English and US data. J Hosp Infect 63(3):255–262. doi:10.1016/j.jhin.2006.02.007
Rotter R (2012) Hip fractures—surgical experience reduces the infection rate. Z Orthop Unfall 150(2):135
Parker MJ, Pryor GA, Myles JW (1994) The value of a special surgical team in preventing complications in the treatment of hip fractures. Int Orthop 18(3):184–188
Cooke EM, Coello R, Sedgwick J, Ward V, Wilson J, Charlett A, Ward B, Pearson A (2000) A national surveillance scheme for hospital associated infections in England. Team of the Nosocomial Infection National Surveillance Scheme. J Hosp Infect 46(1):1–3. doi:10.1053/jhin.2000.0801
Trebse R, Pisot V, Trampuz A (2005) Treatment of infected retained implants. J Bone Joint Surg (Br) 87(2):249–256
Byren I, Bejon P, Atkins BL, Angus B, Masters S, McLardy-Smith P, Gundle R, Berendt A (2009) One hundred and twelve infected arthroplasties treated with ‘DAIR’ (debridement, antibiotics and implant retention): antibiotic duration and outcome. J Antimicrob Chemother 63(6):1264–1271. doi:10.1093/jac/dkp107
Toms AD, Davidson D, Masri BA, Duncan CP (2006) The management of peri-prosthetic infection in total joint arthroplasty. J Bone Joint Surg (Br) 88(2):149–155. doi:10.1302/0301-620X.88B2.17058
Fitzgerald RH Jr (1995) Infected total hip arthroplasty: diagnosis and treatment. J Am Acad Orthop Surg 3(5):249–262
Senthi S, Munro JT, Pitto RP (2011) Infection in total hip replacement: meta-analysis. Int Orthop 35(2):253–260. doi:10.1007/s00264-010-1144-z
Bori G, Munoz-Mahamud E, Cune J, Gallart X, Fuster D, Soriano A (2014) One-stage revision arthroplasty using cementless stem for infected hip arthroplasties. J Arthroplasty 29(5):1076–1081. doi:10.1016/j.arth.2013.11.005
Yoo JJ, Kwon YS, Koo KH, Yoon KS, Kim YM, Kim HJ (2009) One-stage cementless revision arthroplasty for infected hip replacements. Int Orthop 33(5):1195–1201. doi:10.1007/s00264-008-0640-x
Ilchmann T, Zimmerli W, Ochsner PE, Kessler B, Zwicky L, Graber P, Clauss M (2015) One-stage revision of infected hip arthroplasty: outcome of 39 consecutive hips. Int Orthop. doi:10.1007/s00264-015-2833-4
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Noailles, T., Brulefert, K., Chalopin, A. et al. What are the risk factors for post-operative infection after hip hemiarthroplasty? Systematic review of literature. International Orthopaedics (SICOT) 40, 1843–1848 (2016). https://doi.org/10.1007/s00264-015-3033-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-015-3033-y