Abstract
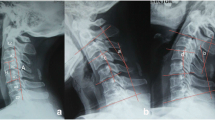
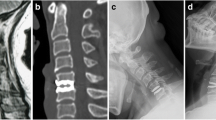
We reviewed patients with cervical disc prosthesis replacement for single-level cervical disc disease to evaluate its clinical effect and maintenance of cervical spine motion. Fifteen patients underwent Bryan artificial cervical disc replacement and were followed-up for at least 24 months. No neurological or vascular complications were observed during or after operation. JOA, VAS, and NDI scores showed statistical significant improvement in our follow-up. The procedure achieved an 87% (13/15) satisfactory rate at 24-month evaluations according to Odom’s criteria. The range of motion (ROM) of the cervical spine, treated segment, adjacent segment, and functional spinal unit (FSU) decreased at early follow-up, but they recovered to the preoperative level at 12- and 24-month follow-up. Also, preoperative lordosis of the cervical spine and FSU were not only maintained but also even improved during the 24-month follow-up. No obvious degeneration of adjacent discs were found at MRI. There were no cases of prosthesis subsidence or extrusion. The cervical disc prosthesis showed a good clinical outcome; it also restored ROM of the cervical spine and reestablished cervical curvature in our 24-month follow-up. But to be sure of its long term effect, a longer follow-up is needed.
Résumé
Nous avons revu les patients ayant bénéficié d’une prothèse cervicale de disque, placée à un seul niveau ceci afin d’évaluer le bénéfice clinique et la persistance de la mobilité cervicale. 15 patients ayant bénéficié d’une prothèse de disque de type Bryan ont été suivis avec un minimum de 24 mois. Aucune complication neurologique ou vasculaire n’a été observée durant l’intervention. Le score de la JOA et le score douleur VAS et le score NDI ont montré de façon significative une amélioration au dernier suivi de ces patients, le taux de satisfaction étant de 87% (13/15) à 24 mois selon les critères de Odomi. La mobilité de la colonne cervicale (FSU) après un limitation passagère précoce est entièrement récupérée à un niveau identique au niveau pré-opératoire entre 12 et 24 mois de suivi. La lordose préopératoire de la colonne cervicale et la mobilité segmentaire FSU non seulement sont maintenues mais sont aussi améliorées durant ces 24 mois de suivi. Nous n’avons pas observé de dégénérescence des disques adjacents à la prothèse discale à l’IRM. Il n’y a pas eu de tassements ou d’extrusion de la prothèse discale. Cette prothèse et les disques cervicaux ont un bon devenir clinique qui permettent de restaurer la mobilité de la colonne cervicale, de rétablir la courbure cervicale à 24 mois de suivi, mais néanmoins, un suivi à long terme est nécessaire.


Similar content being viewed by others
References
Ahrengart L, Sahlin K, Lindgren U (1987) Myositis ossification after total hip replacement and perioperative muscle ischemia. J Arthroplasty 2:65–69
Anderson PA, Rouleau JP (2004) Intervertebral disc arthroplasty. Spine 29:2779–2786
Anderson PA, Sasso RC, Rouleau JP et al (2004) The Bryan cervical disc: wear properties and early clinical results. Spine J 4:303S–309S
Baba H, Furusawa N, Imura S et al (1993) Late radiographic findings after anterior cervical fusion for spondylotic myeloradiculopathy. Spine 18:2167–2173
Chang UK, Kim DH, Lee MC et al (2007) Changes in adjacent-level disc pressure and facet joint force after cervical arthroplasty compared with cervical descectomy and fusion. J Neurosurg Spine 7:33–39
Cherubino P, Benazzo F, Borromeo U et al (1990) Degenerative arthritis of the adjacent spinal joints following anterior cervical spinal fusion: clinicoradiologic and statistical correlations. Ital J Orthop Traumatol 16:533–543
DePalma AF, Rothman RH, Lewinnek GE, Canale ST (1972) Anterior interbody fusion for severe cervical disc degeneration. Surg Gynecol Obstet 134:755–758
Dohler JR, Kahn MR, Hughes SP (1985) Instability of the cervical spine after anterior interbody fusion. A study on its incidence and clinical significance in 21 patients. Arch Orthop Trauma Surg 104:247–250
Goffin J, Calenbergh FV, Loon JV et al (2003) Intermediate follow-up after treatment of degenerative disc disease with the Bryan cervical disc prosthesis: single-level and bi-level. Spine 28:2673–2678
Gore DR, Sepic SB (1984) Anterior cervical fusion for degenerated or protruded discs. A review of one hundred forty-six patients. Spine 9:667–671
Hilibrand AS, Carlson GD, Palumbo MA et al (1999) Radiculopathy and myelopathy at segments adjacent to the site of a previous anterior cervical arthrodesis. J Bone Joint Surg Am 81:519–528
Hunter LY, Braunstein EM, Bailey RW (1980) Radiographic changes following anterior cervical fusion. Spine 5:399–401
Katsuura A, Hukuda S, Saruhashi Y et al (2001) Kyphotic malalignment after anterior cervical fusion is one of the factors promoting the degenerative process in adjacent intervertebral levels. Eur Spine J 10:320–324
Kim SW, Shin JH, Arbatin JJ et al (2008) Effects of a cervical disc prosthesis on maintaining sagittal alignment of the functional spinal unit and overall sagittal balance of the cervical spine. Spine 17:20–29
Lafuente J, Casey AT, Perzold A et al (2005) The Bryan cervical disc prosthesis as an alternative to arthrodesis in the treatment of cervical spondylosis. J Bone Surg Br 87:508–512
Leung C, Casey AT, Goffin J et al (2005) Clinical significance of heterotopic ossification in cervical disc replacement: a prospective multicenter clinical trail. Neurosurgery 57:759–763
McGrory BJ, Klassen RA (1994) Arthrodesis of the cervical spine for fractures and dislocations in children and adolescents. A long-term follow-up study. J Bone Joint Surg Am 76:1606–1616
Nabhan A, Ahlhlm F, Shariat K et al (2007) The Pro-Disc prosthesis: clinical and radiological experience 1 year after surgery. Spine 32:1935–1941
Pickett GE, Mitsis DK, Sekhon LH et al (2004) Effects of a cervical disc prosthesis on segmental and cervical spine alignment. Neurosurg Focus 17:E5
Sekhon LH (2004) Cervical arthroplasty in the management of spondylotic myelopathy: 18-month results. Neurosurg Focus 15:E8
Wang Y, Zhang X, Xiao S et al (2006) Clinical report of cervical arthroplasty in management of spondylotic myelopathy in Chinese. J Orthop Surg 1:13
Weinhoffer SL, Guyer RD, Herbert M et al (1995) Intradiscal pressure measurements above an instrumented fusion. A cadaveric study. Spine 20:526–531
Wigfield C, Gill S, Nelson R, Langdon I et al (2002) Influence of an artificial cervical joint compared with fusion on adjacent-level motion in the treatment of degenerative cervical disc disease. J Neurosurg 96:17–21
Wu W, Thuomas KA, Hedlund R et al (1996) Degenerative changes following anterior cervical discectomy and fusion evaluated by fast spin-echo MR imaging. Acta Radiol 37:614–617
Yoon DH, Yi S, Shin HC et al (2006) Clinical and radiographic results following cervical arthroplasty. Acta Neurochir 148:943–950
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yang, Y.C., Nie, L., Cheng, L. et al. Clinical and radiographic reports following cervical arthroplasty: a 24-month follow-up. International Orthopaedics (SICOT) 33, 1037–1042 (2009). https://doi.org/10.1007/s00264-008-0571-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-008-0571-6