Abstract
Backgound
Literature reports suggest that the host immune system may control Malignant Pleural Mesothelioma (MPM) growth, although its activity is limited by regulatory mechanisms. In this retrospective study, we analyzed the levels of pro-inflammatory (IL-1, IL-6, TNF), immune-regulatory (IL-10) and Th1/CTL-related cytokines (IL-12p70, IFN-γ) in the pleural exudate and their relationship with overall survival (OS) in MPM.
Methods
Cytokines were quantified by multiplexed immunoassay. Concentrations were dichotomized with respect to the median value. Correlation between cytokine level and OS was assessed using univariate (Kaplan–Meier curves) and multivariate (Cox regression) analyses.
Results
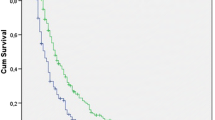
Regarding outcome, tumor histology, therapies undergone and IFN-γ were independent prognostic factors of OS in a 72 MPM training cohort. Notably, high concentrations of IFN-γ halved death probability (HR of high vs low IFN-γ concentration = 0.491, 95%CI 0.3–0.8, p = 0.007). Also in patients with epithelioid histology and those receiving at least one line of therapy, high IFN-γ level was an independent factor predictive of OS (HR of high vs low IFN-γ concentration were 0.497, p = 0.007 and 0.324, p = 0.006, respectively). However, these data were not confirmed in a 77 MPM validation cohort, possibly due to the low IFN-γ levels encountered in this population, and the heterogeneous distribution of disease stages between the training and the validation cohorts. None of the other cytokines showed any effect on survival.
Conclusions
High level of IFN-γ in pleural effusion may be associated with better survival in MPM patients and potentially serve as a prognostic biomarker. Larger prospective studies are needed to ascertain this hypothesis.



Similar content being viewed by others
References
Carbone M, Adusumilli PS, Alexander HR et al (2019) Mesothelioma: scientific clues for prevention, diagnosis, and therapy. CA Cancer J Clin 69:402–429. https://doi.org/10.3322/caac.21572
de Gooijer CJ, Borm FJ, Scherpereel A, Baas P (2020) Immunotherapy in malignant pleural mesothelioma. Front Oncol 10:187. https://doi.org/10.3389/fonc.2020.00187
Maio M, Scherpereel A, Calabrò L et al (2017) Tremelimumab as second-line or third-line treatment in relapsed malignant mesothelioma (DETERMINE): a multicentre, international, randomised, double-blind, placebo-controlled phase 2b trial. Lancet Oncol 18:1261–1273. https://doi.org/10.1016/S1470-2045(17)30446-1
Scherpereel A, Mazieres J, Greillier L et al (2019) Nivolumab or nivolumab plus ipilimumab in patients with relapsed malignant pleural mesothelioma (IFCT-1501 MAPS2): a multicentre, open-label, randomised, non-comparative, phase 2 trial. Lancet Oncol 20:239–253. https://doi.org/10.1016/S1470-2045(18)30765-4
Okada M, Kijima T, Aoe K et al (2019) Clinical efficacy and safety of nivolumab: results of a multicenter, open-label, single-arm, japanese phase ii study in malignant pleural mesothelioma (MERIT). Clin Cancer Res 25:5485–5492. https://doi.org/10.1158/1078-0432.CCR-19-0103
Disselhorst MJ, Quispel-Janssen J, Lalezari F et al (2019) Ipilimumab and nivolumab in the treatment of recurrent malignant pleural mesothelioma (INITIATE): results of a prospective, single-arm, phase 2 trial. Lancet Respir Med 7:260–270. https://doi.org/10.1016/S2213-2600(18)30420-X
Hegmans JP, Veltman JD, Lambers ME et al (2010) Consolidative dendritic cell-based immunotherapy elicits cytotoxicity against malignant mesothelioma. Am J Respir Crit Care Med 181:1383–1390. https://doi.org/10.1164/rccm.200909-1465OC
Aerts JGJV, de Goeje PL, Cornelissen R et al (2018) Autologous dendritic cells pulsed with allogeneic tumor cell lysate in mesothelioma: from mouse to human. Clin Cancer Res 24:766–776. https://doi.org/10.1158/1078-0432.CCR-17-2522
Cornelissen R, Hegmans JPJJ, Maat APWM et al (2016) Extended tumor control after dendritic cell vaccination with low-dose cyclophosphamide as adjuvant treatment in patients with malignant pleural mesothelioma. Am J Respir Crit Care Med 193:1023–1031. https://doi.org/10.1164/rccm.201508-1573OC
Robinson BW, Robinson C, Lake RA (2001) Localised spontaneous regression in mesothelioma–possible immunological mechanism. Lung Cancer 32:197–201. https://doi.org/10.1016/s0169-5002(00)00217-8
Yamada N, Oizumi S, Kikuchi E et al (2010) CD8+ tumor-infiltrating lymphocytes predict favorable prognosis in malignant pleural mesothelioma after resection. Cancer Immunol Immunother 59:1543–1549. https://doi.org/10.1007/s00262-010-0881-6
Anraku M, Cunningham KS, Yun Z et al (2008) Impact of tumor-infiltrating T cells on survival in patients with malignant pleural mesothelioma. J Thorac Cardiovasc Surg 135:823–829. https://doi.org/10.1016/j.jtcvs.2007.10.026
Salaroglio IC, Kopecka J, Napoli F et al (2019) Potential diagnostic and prognostic role of microenvironment in malignant pleural mesothelioma. J Thorac Oncol 14:1458–1471. https://doi.org/10.1016/j.jtho.2019.03.029
Blum Y, Meiller C, Quetel L et al (2019) Dissecting heterogeneity in malignant pleural mesothelioma through histo-molecular gradients for clinical applications. Nat Commun 10:1333. https://doi.org/10.1038/s41467-019-09307-6
Sottile R, Tannazi M, Johansson MH et al (2019) NK- and T-cell subsets in malignant mesothelioma patients: baseline pattern and changes in the context of anti-CTLA-4 therapy. Int J Cancer 145:2238–2248. https://doi.org/10.1002/ijc.32363
Mosser DM, Edwards JP (2008) Exploring the full spectrum of macrophage activation. Nat Rev Immunol 8:958–969. https://doi.org/10.1038/nri2448
Chéné A-L, d’Almeida S, Blondy T et al (2016) Pleural effusions from patients with mesothelioma induce recruitment of monocytes and their differentiation into M2 macrophages. J Thorac Oncol 11:1765–1773. https://doi.org/10.1016/j.jtho.2016.06.022
Lievense LA, Cornelissen R, Bezemer K et al (2016) Pleural effusion of patients with malignant mesothelioma induces macrophage-mediated t cell suppression. J Thorac Oncol 11:1755–1764. https://doi.org/10.1016/j.jtho.2016.06.021
Chu GJ, van Zandwijk N, Rasko JEJ (2019) The immune microenvironment in mesothelioma: mechanisms of resistance to immunotherapy. Front Oncol 9:1366. https://doi.org/10.3389/fonc.2019.01366
Hmeljak J, Sanchez-Vega F, Hoadley KA et al (2018) Integrative molecular characterization of malignant pleural mesothelioma. Cancer Discov 8:1548–1565. https://doi.org/10.1158/2159-8290.CD-18-0804
Acknowledgements
We thank Stefania Martini for excellent technical assistance and the Azienda Ospedaliera di Alessandria Biorepository “Alessandria Biobank” for providing the validation cohort
Funding
This work was supported by grants from the Italian Ministry of Health (GR-2013–02356568, Ricerca Corrente and 5 × 1000 Funds).
Author information
Authors and Affiliations
Contributions
Study concept and design, and study supervision: SF, MF, Recruitment of MPM patients: SR, PF, PD, PAC, Acquisition, analysis or interpretation of data: BD, GC, SF, MF, Manuscript drafting: BD, GC, SF, MF, Statistical analyses: BD, Critical revision of the manuscript for important intellectual content: SF, All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The author declares there is no conflict of interest.
Ethical approval
The local Ethical Committee (Azienda Sanitaria Locale n.5 La Spezia) approved the study (P.R. 207REG2014). All procedures performed in the study were in accordance with the Declaration of HELSINKI.
Informed consent
All patients provided a signed informed consent before enrollment.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Dozin, B., Carbotti, G., Roncella, S. et al. Assessment of interferon-γ in pleural fluid as a prognostic factor of survival in malignant pleural mesothelioma. Cancer Immunol Immunother 70, 3349–3355 (2021). https://doi.org/10.1007/s00262-021-02965-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-021-02965-w