Abstract
Background
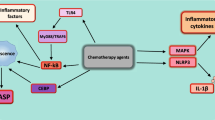
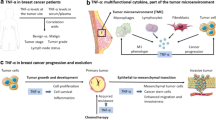
Interleukin (IL)-38 was discovered in 2001 and is a member of the IL-1 family of cytokines. IL-38 shows anti-inflammatory activity in several inflammatory diseases. In lung adenocarcinoma, we previously demonstrated that high IL-38 expression in tumor cells was associated with poor prognosis. However, the role of IL-38 in the tumor microenvironment has not been clarified.
Methods
IL-38-plasmid-transfected Lewis lung carcinoma cells (LLC-IL38) and empty vector-transfected LLC cells (LLC-vector) were established. Cell proliferation in vitro and tumor growth in vivo were examined, and immunohistochemical staining was used to assess tumor-infiltrating lymphocytes (TILs). A CD8+ lymphocyte depletion model was established to show the association between IL-38 and CD8+ lymphocytes. Moreover, we examined the association between IL-38 expression and CD8+ TILs in human samples, analyzing immunohistochemical staining in 226 patients with radically resected lung adenocarcinoma.
Results
Tumor growth of LLC-IL38 in vivo was significantly increased compared with that of LLC-vector, although cell proliferation of LLC-IL38 in vitro was lower than that of LLC-vector. CD8+ TILs were significantly decreased in LLC-IL38 tumor compared with LLC-vector tumor. The difference in tumor growth between LLC-IL38 and LLC-vector became insignificant after depletion of CD8+ lymphocytes. In immunohistochemical staining in tissues from patients with lung adenocarcinoma, multivariate analysis showed high IL-38 expression was an independent negative predicter of high density of CD8+ TILs.
Conclusion
We demonstrated that high IL-38 expression in tumor cells was significantly associated with reduction of CD8+ TILs and tumor progression. These results suggest that IL-38 could be a therapeutic target for lung cancer.





Similar content being viewed by others
Data availability
The data used to support the findings of our study are available from the corresponding author upon reasonable request.
Abbreviations
- LLC-vector:
-
Empty-vector-transfected LLC cells
- IL:
-
Interleukin
- IFN-γ:
-
Interferon-γ
- IL-36R:
-
IL-36 receptor
- LLC-IL38:
-
IL-38-plasmid-transfected LLC cells
- LLC:
-
Lewis lung carcinoma
- MDSCs:
-
Myeloid-derived suppressor cells
- NK:
-
Natural killer
- NSCLC:
-
Non-small cell lung cancer
- PD-1:
-
Programmed cell death-1
- PD-L1:
-
Programmed cell death-ligand 1
- RT:
-
Reversed transcription
- Tregs:
-
Regulatory T cells
- TILs:
-
Tumor-infiltrating lymphocytes
- TNF-α:
-
Tumor necrosis factor-α
References
Ferlay J, Colombet M, Soerjomataram I, Mathers C, Parkin DM, Pineros M, Znaor A, Bray F (2019) Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int J Cancer 144:1941–1953
Borghaei H, Paz-Ares L, Horn L, Spigel DR, Steins M, Ready NE, Chow LQ, Vokes EE, Felip E, Holgado E, Barlesi F, Kohlhäufl M, Arrieta O, Burgio MA, Fayette J, Lena H, Poddubskaya E, Gerber DE, Gettinger SN, Rudin CM, Rizvi N, Crinò L, Blumenschein GR Jr, Antonia SJ, Dorange C, Harbison CT, Graf Finckenstein F, Brahmer JR (2015) Nivolumab versus docetaxel in advanced nonsquamous non-small-cell lung cancer. N Engl J Med 373:1627–1639
Herbst RS, Baas P, Kim DW, Felip E, Perez-Gracia JL, Han JY, Molina J, Kim JH, Arvis CD, Ahn MJ, Majem M, Fidler MJ, de Castro G, Jr GM, Lubiniecki GM, Shentu Y, Im E, Dolled-Filhart M, Garon EB (2016) Pembrolizumab versus docetaxel for previously treated, PD-L1-positive, advanced non-small-cell lung cancer (KEYNOTE-010): a randomised controlled trial. Lancet 387:1540–1550
Rittmeyer A, Barlesi F, Waterkamp D, Park K, Ciardiello F, von Pawel J, Gadgeel SM, Hida T, Kowalski DM, Dols MC, Cortinovis DL, Leach J, Polikoff J, Barrios C, Kabbinavar F, Frontera OA, De Marinis F, Turna H, Lee JS, Ballinger M, Kowanetz M, He P, Chen DS, Sandler A, Gandara DR (2017) Atezolizumab versus docetaxel in patients with previously treated non-small-cell lung cancer (OAK): a phase 3, open-label, multicentre randomised controlled trial. Lancet 389:255–265
Sacher AG, Gandhi L (2016) Biomarkers for the clinical use of PD-1/PD-L1 inhibitors in non-small-cell lung cancer: a review. JAMA Oncol 2:1217–1222
Lin H, Ho AS, Haley-Vicente D, Zhang J, Bernal-Fussell J, Pace AM, Hansen D, Schweighofer K, Mize NK, Ford JE (2001) Cloning and characterization of IL-1HY2, a novel interleukin-1 family member. J Biol Chem 276:20597–20602
Bensen JT, Dawson PA, Mychaleckyj JC, Bowden DW (2001) Identification of a novel human cytokine gene in the interleukin gene cluster on chromosome 2q12-14. J Interferon Cytokine Res 21:899–904
Tominaga M, Okamoto M, Kawayama T, Matsuoka M, Kaieda S, Sakazaki Y, Kinoshita T, Mori D, Inoue A, Hoshino T (2017) Overexpression of IL-38 protein in anticancer drug-induced lung injury and acute exacerbation of idiopathic pulmonary fibrosis. Respir Investig 55:293–299
van de Veerdonk FL, Stoeckman AK, Wu G, Boeckermann AN, Azam T, Netea MG, Joosten LA, van der Meer JW, Hao R, Kalabokis V, Dinarello CA (2012) IL-38 binds to the IL-36 receptor and has biological effects on immune cells similar to IL-36 receptor antagonist. Proc Natl Acad Sci USA 109:3001–3005
Vigne S, Palmer G, Martin P, Lamacchia C, Strebel D, Rodriguez E, Olleros ML, Vesin D, Garcia I, Ronchi F, Sallusto F, Sims JE, Gabay C (2012) IL-36 signaling amplifies Th1 responses by enhancing proliferation and Th1 polarization of naive CD4 T cells. Blood 120:3478–3487
Ding L, Wang X, Hong X, Lu L, Liu D (2017) IL-36 cytokines in autoimmunity and inflammatory disease. Oncotarget 9:2895–2901
Chu M, Chu IM, Yung EC, Lam CW, Leung TF, Wong GW, Wong CK (2016) Aberrant expression of novel cytokine IL-38 and regulatory T lymphocytes in childhood asthma. Molecules. https://doi.org/10.3390/molecules21070933
Takenaka S, Kaieda S, Kawayama T, Matsuoka M, Kaku Y, Kinoshita T, Sakazaki Y, Okamoto M, Tominaga M, Kanesaki K, Chiba A, Miyake S, Ida H, Hoshino T (2015) IL-38: a new factor in rheumatoid arthritis. Biochem Biophys Rep 4:386–391
Takada K, Okamoto T, Tominaga M, Teraishi K, Akamine T, Takamori S, Katsura M, Toyokawa G, Shoji F, Okamoto M, Oda Y, Hoshino T, Maehara Y (2017) Clinical implications of the novel cytokine IL-38 expressed in lung adenocarcinoma: possible association with PD-L1 expression. PLoS ONE 12:e0181598
Wang F, Zhang W, Wu T, Chu H (2018) Reduced interleukin-38 in non-small cell lung cancer is associated with tumour progression. Open Biol. https://doi.org/10.1098/rsob.180132
Ostroumov D, Fekete-Drimusz N, Saborowski M, Kuhnel F, Woller N (2018) CD4 and CD8 T lymphocyte interplay in controlling tumor growth. Cell Mol Life Sci 75:689–713
Zeng DQ, Yu YF, Ou QY, Li XY, Zhong RZ, Xie CM, Hu QG (2016) Prognostic and predictive value of TILs for clinical therapeutic research in patients with NSCLC. Oncotarget 7:13765–13781
Geng Y, Shao Y, He W, Hu W, Xu Y, Chen J, Wu C, Jiang J (2015) Prognostic role of tumor-infiltrating lymphocytes in lung cancer: a meta-analysis. Cell Physiol Biochem 37:1560–1571
Han Y, Mora J, Huard A, da Silva P, Wiechmann S, Putyrski M, Schuster C, Elwakeel E, Lang G, Scholz A, Scholz T, Schmid T, de Bruin N, Billuart P, Sala C, Burkhardt H, Parnham MJ, Ernst A, Brüne B, Weigert A (2019) IL-38 ameliorates skin inflammation and limits IL-17 production from γδ T Cells. Cell Rep 27:835–846
Bhat P, Leggatt G, Waterhouse N, Frazer IH (2017) Interferon-gamma derived from cytotoxic lymphocytes directly enhances their motility and cytotoxicity. Cell Death Dis 8:e2836
Schoenborn JR, Wilson CB (2007) Regulation of interferon-gamma during innate and adaptive immune responses. Adv Immunol 96:41–101
Giovarelli M, Santoni A, Jemma C, Musso T, Giuffrida AM, Cavallo G, Landolfo S, Forni G (1988) Obligatory role of IFN-gamma in induction of lymphokine-activated and T lymphocyte killer activity, but not in boosting of natural cytotoxicity. J Immunol 141:2831–2836
Balkwill F (2009) Tumour necrosis factor and cancer. Nat Rev Cancer 9:361–371
Lejeune FJ (2002) Clinical use of TNF revisited: improving penetration of anti-cancer agents by increasing vascular permeability. J Clin Invest 110:433–435
Chang SH, Mirabolfathinejad SG, Katta H, Cumpian AM, Gong L, Caetano MS, Moghaddam SJ, Dong C (2014) T helper 17 cells play a critical pathogenic role in lung cancer. Proc Natl Acad Sci USA 111:5664–5669
Kryczek I, Banerjee M, Cheng P, Vatan L, Szeliga W, Wei S, Huang E, Finlayson E, Simeone D, Welling TH, Chang A, Coukos G, Liu R, Zou W (2009) Phenotype, distribution, generation, and functional and clinical relevance of Th17 cells in the human tumor environments. Blood 114:1141–1149
Martin-Orozco N, Muranski P, Chung Y, Yang XO, Yamazaki T, Lu S, Hwu P, Restifo NP, Overwijk WW (2009) T helper 17 cells promote cytotoxic T cell activation in tumor immunity. Immunity 31:787–798
Acknowledgements
We thank Saori Tsurumaru, Emi Kamiya, Asuka Nakamura, Miki Nakashima, Yuko Kubota and Natsumi Maeda (Junior Laboratory Animal Technician) for their invaluable help with in vitro examination, tissue processing and animal experiments. We also thank Cathel Kerr, BSc, PhD, from Edanz Group (www.edanzediting.com/ac) for editing a draft of this manuscript.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
Conception and design: FK, KT, TT, MM. Development of methodology: FK, TA, KT, TT. Acquisition of data: FK, TA, YY, YO, KK, YO, KT, SW. Analysis and interpretation of data: FK, TA, KT, TO, AO, TT, MS, YO, TH, MM. Writing, review, and/or revision of manuscript: FK, TT, TH, MM. Study supervision: TT, MS, YO, TH, MM.
Corresponding author
Ethics declarations
Conflict of interest
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kinoshita, F., Tagawa, T., Akamine, T. et al. Interleukin-38 promotes tumor growth through regulation of CD8+ tumor-infiltrating lymphocytes in lung cancer tumor microenvironment. Cancer Immunol Immunother 70, 123–135 (2021). https://doi.org/10.1007/s00262-020-02659-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-020-02659-9