Abstract
Background
Single-agent pembrolizumab represents the standard first-line option for metastatic non-small-cell lung cancer (NSCLC) patients with a PD-L1 (programmed death-ligand 1) expression of ≥ 50%.
Methods
We conducted a multicenter retrospective study aimed at evaluating the clinicopathologic correlates of pembrolizumab effectiveness in patients with treatment-naïve NSCLC and a PD-L1 expression of ≥ 50%.
Results
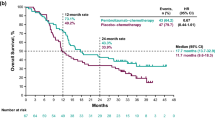
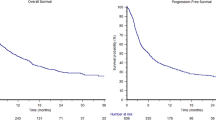
One thousand and twenty-six consecutive patients were included. The objective response rate (ORR) was 44.5% (95% CI 40.2–49.1), while the median progression free survival (PFS) and overall survival (OS) were 7.9 months (95% CI 6.9–9.5; 599 events) and 17.2 months (95% CI 15.3–22.3; 598 censored patients), respectively. ECOG-PS ≥ 2 (p < 0.0001) and bone metastases (p = 0.0003) were confirmed to be independent predictors of a worse ORR. Former smokers (p = 0.0002), but not current smokers (p = 0.0532) were confirmed to have a significantly prolonged PFS compared to never smokers at multivariate analysis. ECOG-PS (p < 0.0001), bone metastases (p < 0.0001) and liver metastases (p < 0.0001) were also confirmed to be independent predictors of a worse PFS. Previous palliative RT was significantly related to a shortened OS (p = 0.0104), while previous non-palliative RT was significantly related to a prolonged OS (p = 0.0033). Former smokers (p = 0.0131), but not current smokers (p = 0.3433) were confirmed to have a significantly prolonged OS compared to never smokers. ECOG-PS (p < 0.0001), bone metastases (p < 0.0001) and liver metastases (p < 0.0001) were also confirmed to be independent predictors of a shortened OS. A PD-L1 expression of ≥ 90%, as assessed by recursive partitioning, was associated with significantly higher ORR (p = 0.0204), and longer and OS (p = 0.0346) at multivariable analysis.
Conclusion
Pembrolizumab was effective in a large cohort of NSCLC patients treated outside of clinical trials. Questions regarding the effectiveness in clinical subgroups, such as patients with poorer PS and with liver/bone metastases, still remain to be addressed. We confirmed that the absence of tobacco exposure, and the presence of bone and liver metastasis are associated with worse clinical outcomes to pembrolizumab. Increasing levels of PD-L1 expression may help identifying a subset of patients who derive a greater benefit from pembrolizumab monotherapy.




Similar content being viewed by others
Availability of data and materials
The datasets used during the present study are available from the corresponding author upon reasonable request.
References
Reck M, Rodríguez-Abreu D, Robinson AG et al (2016) Pembrolizumab versus chemotherapy for PD-L1-positive non-small-cell lung cancer. N Engl J Med 375(19):1823–1833
Reck M, Rodríguez-Abreu D, Robinson AG et al (2019) Updated analysis of KEYNOTE-024: pembrolizumab versus platinum-based chemotherapy for advanced non-small-cell lung cancer with PD-L1 tumor proportion score of 50% or greater. J Clin Oncol 37(7):537–546. https://doi.org/10.1200/JCO.18.00149
Reck M, Rodríguez-Abreu D, Robinson AG et al (2019) OA14.01 KEYNOTE-024 3-year survival update: pembrolizumab vs platinum-based chemotherapy for advanced non-small-cell lung cancer. J Thorac Oncol 14(10):S243
Aguilar EJ, Ricciuti B, Gainor JF et al (2019) Outcomes to first-line pembrolizumab in patients with non-small-cell lung cancer and very high PD-L1 expression. Ann Oncol 30(10):1653–1659. https://doi.org/10.1093/annonc/mdz288
Tamiya M, Tamiya A, Hosoya K et al (2019) Efficacy and safety of pembrolizumab as first-line therapy in advanced non-small cell lung cancer with at least 50% PD-L1 positivity: a multicenter retrospective cohort study (HOPE-001). Investig New Drugs 37(6):1266–1273. https://doi.org/10.1007/s10637-019-00843-y
Velcheti V, Chandwani S, Chen X et al (2019) Outcomes of first-line pembrolizumab monotherapy for PD-L1-positive (TPS ≥ 50%) metastatic NSCLC at US oncology practices. Immunotherapy 11(18):1541–1554. https://doi.org/10.2217/imt-2019-0177
Facchinetti F, Mazzaschi G, Barbieri F et al (2020) First-line pembrolizumab in advanced non-small cell lung cancer patients with poor performance status. Eur J Cancer 130:155–167. https://doi.org/10.1016/j.ejca.2020.02.023
Gandhi L, Rodríguez-Abreu D, Gadgeel S et al (2018) Pembrolizumab plus chemotherapy in metastatic non-small-cell lung cancer. N Engl J Med 378(22):2078–2092. https://doi.org/10.1056/NEJMoa1801005
Paz-Ares L, Luft A, Vicente D et al (2018) Pembrolizumab plus chemotherapy for squamous non-small-cell lung cancer. N Engl J Med 379(21):2040–2051. https://doi.org/10.1056/NEJMoa1810865
Eisenhauer EA, Therasse P, Bogaerts J et al (2009) New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 45:228–247
Gainor JF, Rizvi H, Jimenez Aguilar E et al (2020) Clinical activity of programmed cell death 1 (PD-1) blockade in never, light, and heavy smokers with non-small cell lung cancer and PD-L1 expresion ≥ 50%. Ann Oncol. https://doi.org/10.1016/j.annonc.2019.11.015(in press)
Gridelli C, Balducci L, Ciardiello F et al (2015) Treatment of elderly patients with non-small-cell lung cancer: results of an international expert panel meeting of the Italian Association of Thoracic Oncology. Clin Lung Cancer 16(5):325–333
Bersanelli M, Lattanzi E, D’Abbiero N et al (2020) Palliative radiotherapy in advanced cancer patients treated with immune-checkpoint inhibitors: the PRACTICE study. Biomed Rep 12(2):59–67. https://doi.org/10.3892/br.2019.1265
Koletsi D, Pandis N (2016) The Chi square test for trend. Am J Orthod Dentofac Orthop 150(6):1066–1067. https://doi.org/10.1016/j.ajodo.2016.10.001
Bonate PL (2017) Effect of correlation on covariate selection in linear and nonlinear mixed effect models. Pharm Stat 16(1):45–54. https://doi.org/10.1002/pst.1776
Bonate PL (1999) The effect of collinearity on parameter estimates in nonlinear mixed effect models. Pharm Res 16(5):709–717
Ribbing J, Jonsson EN (2004) Power, selection bias, and predictive performance of the population pharmacokinetic covariate model. J Pharmacokinet Pharmacodyn 31(2):109–134
Hosmer DW Jr, Lemeshow S (2013) Sturdivant RX applied logistic regression, 3rd edn. Wiley, Hoboken
Kaplan EL, Meier P (1958) Nonparametric estimation of incomplete observations. J Am Stat Assoc 53:457–481
Schemper M, Smith TL (1997) A note on quantifying follow-up in studies of failure time. Control Clin Trials 17(343–346):10
Cox DR (1972) Regression models and life tables (with discussion). J R Stat Soc (Ser B) 74:187–200
PD-L1 IHC 22C3 pharmDx interpretation manual—NSCLC. https://www.agilent.com/cs/library/usermanuals/public/29158_pd-l1-ihc-22C3-pharmdx-nsclc-interpretation-manual.pdf. Accessed 18 Feb 2020
Hanley JA, McNeil BJ (1982) The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology 143(1):29–36
Ihaka R, Gentleman R (1996) A language for data analysis and graphics. J Comput Graph Stat 5:299–314
Teixidó C, Vilariño N, Reyes R et al (2018) PD-L1 expression testing in non-small cell lung cancer. Ther Adv Med Oncol. https://doi.org/10.1177/1758835918763493
Kim S, Koh J, Kwon D et al (2017) Comparative analysis of PD-L1 expression between primary and metastatic pulmonary adenocarcinomas. Eur J Cancer 75:141–149. https://doi.org/10.1016/j.ejca.2017.01.004
Lee CC, Soon YY, Lum JHY et al (2020) Frequency of discordance in programmed death-ligand 1 (PD-L1) expression between primary tumors and paired distant metastases in advanced cancers: a systematic review and meta-analysis. Acta Oncol. https://doi.org/10.1080/0284186x.2020.1741678
Howell D (2002) Statistical methods for psychology. Duxbury, Pacific Grove, pp 324–325. ISBN 0-534-37770-X
Peto R, Peto J (1972) Asymptomatically efficient rank invariant test procedures. J R Stat Soc A 135:185–206
Mok TSK, Wu YL, Kudaba I et al (2019) Pembrolizumab versus chemotherapy for previously untreated, PD-L1-expressing, locally advanced or metastatic non-small-cell lung cancer (KEYNOTE-042): a randomised, open-label, controlled, phase 3 trial. Lancet 393(10183):1819–1830. https://doi.org/10.1016/S0140-6736(18)32409-7
Landi L, D’Incà F, Gelibter A et al (2019) Bone metastases and immunotherapy in patients with advanced non-small-cell lung cancer. J Immunother Cancer 7(1):316. https://doi.org/10.1186/s40425-019-0793-8
Botticelli A, Salati M, Di Pietro FR et al (2019) A nomogram to predict survival in non-small cell lung cancer patients treated with nivolumab. J Transl Med 17(1):99. https://doi.org/10.1186/s12967-019-1847-x
Zhou Y, Lin Z, Zhang X et al (2019) First-line treatment for patients with advanced non-small cell lung carcinoma and high PD-L1 expression: pembrolizumab or pembrolizumab plus chemotherapy. J Immunother Cancer 7(1):120. https://doi.org/10.1186/s40425-019-0600-6
Kim R, Keam B, Hahn S et al (2019) First-line pembrolizumab versus pembrolizumab plus chemotherapy versus chemotherapy alone in non-small-cell lung cancer: a systematic review and network meta-analysis. Clin Lung Cancer 20(5):331–338.e4. https://doi.org/10.1016/j.cllc.2019.05.009
Garon EB, Rizvi NA, Hui R et al (2015) Pembrolizumab for the treatment of non-small-cell lung cancer. N Engl J Med 372(21):2018–2028. https://doi.org/10.1056/NEJMoa1501824
Kim JH, Kim HS, Kim BJ et al (2017) Prognostic value of smoking status in non-small-cell lung cancer patients treated with immune checkpoint inhibitors: a meta-analysis. Oncotarget 8(54):93149–93155. https://doi.org/10.18632/oncotarget.18703
Theelen WSME, Peulen HMU, Lalezari F et al (2019) Effect of pembrolizumab after stereotactic body radiotherapy vs pembrolizumab alone on tumor response in patients with advanced non-small cell lung cancer: results of the PEMBRO-RT phase 2 randomized clinical trial. JAMA Oncol. https://doi.org/10.1001/jamaoncol.2019.1478
Ricciuti B, Dahlberg SE, Adeni A et al (2019) Immune checkpoint inhibitor outcomes for patients with non-small-cell lung cancer receiving baseline corticosteroids for palliative versus nonpalliative indications. J Clin Oncol 37(22):1927–1934. https://doi.org/10.1200/JCO.19.00189
Lee CK, Man J, Lord S et al (2017) Checkpoint inhibitors in metastatic EGFR-mutated non-small cell lung cancer-a meta-analysis. J Thorac Oncol 12(2):403–407. https://doi.org/10.1016/j.jtho.2016.10.007
Acknowledgements
A special thanks to the “Consorzio Interuniversitario Nazionale per la Bio‑Oncologia” for their support in this study.
Funding
No funding was received.
Author information
Authors and Affiliations
Contributions
All authors contributed to the publication according to the ICMJE guidelines for the authorship (study conception and design, acquisition of data, analysis and interpretation of data, drafting of manuscript, critical revision). All authors read and approved the submitted version of the manuscript (and any substantially modified version that involves the author’s contribution to the study). Each author have agreed both to be personally accountable for the author’s own contributions and to ensure that questions related to the accuracy or integrity of any part of the work, even ones in which the author was not personally involved, are appropriately investigated, resolved, and the resolution documented in the literature.
Corresponding author
Ethics declarations
Conflict of interest
Dr. Alessio Cortellini received speaker fees and grant consultancies by Astrazeneca, MSD, BMS, Roche, Novartis, Istituto Gentili, Astellas and Ipsen. Dr. Emilio Bria received speaker and travel fees from MSD, Astra-Zeneca, Pfizer, Helsinn, Eli-Lilly, BMS, Novartis and Roche. Dr. Emilio Bria received grant consultancies by Roche and Pfizer. Dr. Marcello Tiseo received speaker fees and grant consultancies by Astrazeneca, Pfizer, Eli-Lilly, BMS, Novartis, Roche, MSD, Boehringer Ingelheim, Otsuka, Takeda and Pierre Fabre. Dr. Alessandro Morabito received speaker fees by Astra, Roche, BMS, MSD, Boehringer, Pfizer, Takeda. Dr. Francesca Mazzoni received grant consultancies by MSD and Takeda. Dr. Raffaele Gisti received speaker fees and grant consultancies by Astrazeneca and Roche. Dr. Francesco Passiglia received grant consultancies by MSD and Astrazeneca. Dr. Paolo Bironzo received grant consultancies by Astrazeneca and Boehringer-Ingelheim. Dr. Alex Friedlaender received grant consultancies by Roche, Pfizer, Astellas and BMS. Dr. Alfredo Addeo received grant consultancies by Takeda, MSD, BMJ, Astrazeneca, Roche and Pfizer. Dr. Rita Chiari received speaker fees by BMS, MSD, Takeda, Pfizer, Roche and Astrazeneca. Dr. Carlo Genova received speaker fees/grant consultancies by Astrazeneca, BMS, Boehringer-Ingelheim, Roche and MSD.
Consent for publication
Not applicable.
Ethical approval
All patients provided written, informed consent to treatment with immunotherapy. The procedures followed were in accordance with the precepts of Good Clinical Practice and the declaration of Helsinki. The study was approved by the respective local ethical committees on human experimentation of each institution, after previous approval by the coordinating center (Comitato Etico per le provice di L’Aquila e Teramo, verbale N.15 del 28 Novembre 2019).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Table 1:
Patients characteristics. *Available for 731 patients (67.3%). # Available for 128 out of 181 (70.7%) palliative radiation treatments. ¥ Available for 35 out of 47 (74.5%) non-palliative radiation treatments. NA: not available (DOC 63 kb)
Table 2:
Correlation analyses between previous RT categories, baseline steroids and sites of metastases. # χ2 test for trend. (DOC 38 kb)
Supplementary file 3:
List of the oncological institution of the study (PDF 155 kb)
Rights and permissions
About this article
Cite this article
Cortellini, A., Tiseo, M., Banna, G.L. et al. Clinicopathologic correlates of first-line pembrolizumab effectiveness in patients with advanced NSCLC and a PD-L1 expression of ≥ 50%. Cancer Immunol Immunother 69, 2209–2221 (2020). https://doi.org/10.1007/s00262-020-02613-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-020-02613-9