Abstract
Purpose
We aimed to develop a preoperative prediction model for extraprostatic extension (EPE) in prostate cancer (PCa) patients following radical prostatectomy (RP) using MRI and clinical factors.
Methods
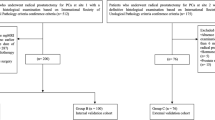
This retrospective study enrolled 266 consecutive patients who underwent RP for PCa in 2022. These patients were divided into a training set (n = 187) and a test set (n = 79) through random assignment. The evaluated variables included age, prostate-specific antigen (PSA) level, prostate volume, PSA density (PSAD), index tumor length on MRI, Prostate Imaging-Reporting and Data System (PI-RADS) category, and EPE-related MRI features as defined by PI-RADS v2.1. A predictive model was constructed through multivariable logistic regression and subsequently translated into a scoring system. The performance of this scoring system in terms of prediction and calibration was assessed using C statistics and the Hosmer‒Lemeshow test.
Results
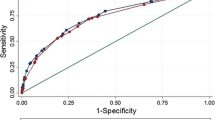
Among patients in the training and test cohorts, 74 (39.6%) and 25 (31.6%), respectively, exhibited EPE after RP. The formulated scoring system incorporated the following factors: PSAD, index tumor length, bulging prostatic contour, and tumor-capsule interface > 10 mm as identified on MRI. This scoring system demonstrated strong prediction performance for EPE in both the training (C statistic, 0.87 [95% confidence interval, 0.86–0.87]) and test cohorts (C statistic, 0.85 [0.83–0.89]). Furthermore, the scoring system exhibited good calibration in both cohorts (P = 0.988 and 0.402, respectively).
Conclusion
Our scoring system, built upon MRI features defined by the PI-RADS, offers valuable assistance in assessing the likelihood of EPE after RP.
Graphical Abstract




Similar content being viewed by others
Abbreviations
- CI:
-
Confidence interval
- DCE:
-
Dynamic contrast-enhanced imaging
- DWI:
-
Diffusion-weighted imaging
- EPE:
-
Extraprostatic extension
- IRE:
-
Irreversible electroporation
- ISUP:
-
International Society of Urological Pathology
- MRI:
-
Magnetic resonance imaging
- mpMRI:
-
Multiparametric MRI
- OR:
-
Odds ratio
- PI-RADS:
-
Prostate Imaging-Reporting and Data System
- PI-QUAL:
-
Prostate Image Quality
- PCa:
-
Prostate cancer
- PSA:
-
Prostate-specific antigen
- PSAD:
-
Prostate-specific antigen density
- RP:
-
Radical prostatectomy
- TCI:
-
Tumor-capsule interface
References
Sung H, Ferlay J, Siegel RL et al (2021) Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin 71:209-249. https://doi.org/https://doi.org/10.3322/caac.21660
Epstein JI, Zelefsky MJ, Sjoberg DD et al (2016) A Contemporary Prostate Cancer Grading System: A Validated Alternative to the Gleason Score. Eur Urol 69:428-435. https://doi.org/https://doi.org/10.1016/j.eururo.2015.06.046
Leapman MS, Cowan JE, Simko J et al (2017) Application of a Prognostic Gleason Grade Grouping System to Assess Distant Prostate Cancer Outcomes. Eur Urol 71:750-759. https://doi.org/https://doi.org/10.1016/j.eururo.2016.11.032
Sandhu S, Moore CM, Chiong E et al (2021) Prostate cancer. Lancet 398:1075-1090. https://doi.org/https://doi.org/10.1016/s0140-6736(21)00950-8
Parker C, Castro E, Fizazi K et al (2020) Prostate cancer: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol 31:1119-1134. https://doi.org/https://doi.org/10.1016/j.annonc.2020.06.011
Amin MB, Greene FL, Edge SB et al (2017) The Eighth Edition AJCC Cancer Staging Manual: Continuing to build a bridge from a population‐based to a more “personalized” approach to cancer staging. CA Cancer J Clin 67:93-99. https://doi.org/https://doi.org/10.3322/caac.21388
Würnschimmel C, Wenzel M, Wang N et al (2021) Radical prostatectomy for localized prostate cancer: 20-year oncological outcomes from a German high-volume center. Urol Oncol 39:830.e17-830.e26. https://doi.org/https://doi.org/10.1016/j.urolonc.2021.04.031
Stabile A, Giganti F, Rosenkrantz AB et al (2019) Multiparametric MRI for prostate cancer diagnosis: current status and future directions. Nat Rev Urol 17:41-61. https://doi.org/https://doi.org/10.1038/s41585-019-0212-4
American College of Radiology (2019) Prostate Imaging–Reporting and Data System Version 2.1. https://www.acr.org/-/media/ACR/Files/RADS/PI-RADS/PIRADS-V2-1.pdf. Accessed 15 October 2023
de Rooij M, Hamoen EHJ, Witjes JA et al (2016) Accuracy of Magnetic Resonance Imaging for Local Staging of Prostate Cancer: A Diagnostic Meta-analysis. Eur Urol 70:233-245. https://doi.org/https://doi.org/10.1016/j.eururo.2015.07.029
Zhang F, Liu C-L, Chen Q et al (2019) Accuracy of multiparametric magnetic resonance imaging for detecting extracapsular extension in prostate cancer: a systematic review and meta-analysis. Br J Radiol 92:20190480. https://doi.org/https://doi.org/10.1259/bjr.20190480
Li W, Dong A, Hong G et al (2021) Diagnostic performance of ESUR scoring system for extraprostatic prostate cancer extension: A meta-analysis. Eur J Radiol 143:109896. https://doi.org/https://doi.org/10.1016/j.ejrad.2021.109896
Choi MH, Kim DH, Lee YJ et al (2023) Imaging features of the PI-RADS for predicting extraprostatic extension of prostate cancer: systematic review and meta-analysis. Insights Imaging 14:77. https://doi.org/https://doi.org/10.1186/s13244-023-01422-9
Mehralivand S, Shih JH, Harmon S et al (2019) A Grading System for the Assessment of Risk of Extraprostatic Extension of Prostate Cancer at Multiparametric MRI. Radiology 290:709-719. https://doi.org/https://doi.org/10.1148/radiol.2018181278
Park KJ, Kim M-h, Kim JK (2020) Extraprostatic Tumor Extension: Comparison of Preoperative Multiparametric MRI Criteria and Histopathologic Correlation after Radical Prostatectomy. Radiology 296:87-95. https://doi.org/https://doi.org/10.1148/radiol.2020192133
Giganti F, Allen C, Emberton M et al (2020) Prostate Imaging Quality (PI-QUAL): A New Quality Control Scoring System for Multiparametric Magnetic Resonance Imaging of the Prostate from the PRECISION trial. Eur Urol Oncol 3:615-619. https://doi.org/https://doi.org/10.1016/j.euo.2020.06.007
Guerra A, Alves FC, Maes K et al (2022) Early biomarkers of extracapsular extension of prostate cancer using MRI-derived semantic features. Cancer Imaging 22:74. https://doi.org/https://doi.org/10.1186/s40644-022-00509-8
Gatti M, Faletti R, Gentile F et al (2022) mEPE-score: a comprehensive grading system for predicting pathologic extraprostatic extension of prostate cancer at multiparametric magnetic resonance imaging. Eur Radiol 32:4942-4953. https://doi.org/https://doi.org/10.1007/s00330-022-08595-9
D'Amico AV (1998) Biochemical Outcome After Radical Prostatectomy, External Beam Radiation Therapy, or Interstitial Radiation Therapy for Clinically Localized Prostate Cancer. JAMA 280:969-974. https://doi.org/https://doi.org/10.1001/jama.280.11.969
Barentsz JO, Richenberg J, Clements R et al (2012) ESUR prostate MR guidelines 2012. Eur Radiol 22:746-757. https://doi.org/https://doi.org/10.1007/s00330-011-2377-y
Gaunay GS, Patel V, Shah P et al (2017) Multi-parametric MRI of the prostate: Factors predicting extracapsular extension at the time of radical prostatectomy. Asian J Urol 4:31-36. https://doi.org/https://doi.org/10.1016/j.ajur.2016.07.002
Alessi S, Pricolo P, Summers P et al (2019) Low PI-RADS assessment category excludes extraprostatic extension (≥pT3a) of prostate cancer: a histology-validated study including 301 operated patients. Eur Radiol 29:5478-5487. https://doi.org/https://doi.org/10.1007/s00330-019-06092-0
Karavitakis M, Ahmed HU, Abel PD et al (2012) Margin Status After Laparoscopic Radical Prostatectomy and the Index Lesion: Implications for Preoperative Evaluation of Tumor Focality in Prostate Cancer. J Endourol 26:503-508. https://doi.org/https://doi.org/10.1089/end.2011.0345
Pooli A, Johnson DC, Shirk J et al (2021) Predicting Pathological Tumor Size in Prostate Cancer Based on Multiparametric Prostate Magnetic Resonance Imaging and Preoperative Findings. J Urol 205:444-451. https://doi.org/https://doi.org/10.1097/ju.0000000000001389
Benson MC, Seong Whang I, Pantuck A et al (1992) Prostate Specific Antigen Density: A Means of Distinguishing Benign Prostatic Hypertrophy and Prostate Cancer. J Urol 147:815-816. https://doi.org/https://doi.org/10.1016/s0022-5347(17)37393-7
Yusim I, Krenawi M, Mazor E et al (2020) The use of prostate specific antigen density to predict clinically significant prostate cancer. Sci Rep 10:20015. https://doi.org/https://doi.org/10.1038/s41598-020-76786-9
Lin S, Zhang Q, Li P et al (2014) Prediction of Extraprostatic Extension in Patients with Clinically Organ-Confined Prostate Cancer. Urol Int 92:282-288. https://doi.org/https://doi.org/10.1159/000353654
Xu L, Zhang G, Zhang X et al (2021) External Validation of the Extraprostatic Extension Grade on MRI and Its Incremental Value to Clinical Models for Assessing Extraprostatic Cancer. Front Oncol 11:655093. https://doi.org/https://doi.org/10.3389/fonc.2021.655093
Youn SY, Choi MH, Lee YJ et al (2023) Prostate gland volume estimation: anteroposterior diameters measured on axial versus sagittal ultrasonography and magnetic resonance images. Ultrasonography 42:154-164. https://doi.org/https://doi.org/10.14366/usg.22104
Kim T-H, Woo S, Han S et al (2020) The Diagnostic Performance of the Length of Tumor Capsular Contact on MRI for Detecting Prostate Cancer Extraprostatic Extension: A Systematic Review and Meta-Analysis. Korean J Radiol 21:684-694. https://doi.org/https://doi.org/10.3348/kjr.2019.0842
Funding
No funding was received for this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval and informed consent
This study was approved by institutional review board, and informed patient consent was waived due to the retrospective nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Moon, H.W., Kim, D.H., Kim, J. et al. A preoperative scoring system for predicting the extraprostatic extension of prostate cancer following radical prostatectomy using magnetic resonance imaging and clinical factors. Abdom Radiol (2024). https://doi.org/10.1007/s00261-024-04345-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00261-024-04345-1