Abstract
Objective
Portal hypertension leads to hepatic artery dilatation and a higher risk of bleeding. We tried to identify the bleeding risk after gastroesophageal varices (GOV) treatment using hepatic artery diameter of contrast-enhanced CT.
Methods
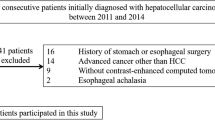
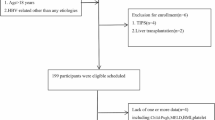
Retrospective retrieval of 258 patients with cirrhosis who underwent contrast-enhanced CT from January 2022 to May 2023 and endoscopy within one month thereafter at Hainan Affiliated Hospital of Hainan Medical University. Cirrhotic patients before GOV treatment were used as the test cohort (n = 199), and cirrhotic patients after GOV treatment were used as the validation cohort (n = 59). The grading and bleeding risk was classified according to the endoscopic findings. Arterial-phase images of contrast-enhanced CT were used for coronal reconstruction, and the midpoint diameter of the hepatic artery was measured on coronal images. The optimal cutoff value for identifying bleeding risk was analyzed and calculated in the test cohort, and its diagnostic performance was evaluated in the validation cohort.
Results
In the test cohort, hepatic artery diameters were significantly higher in high-risk GOV than in low-risk GOV [4.69 (4.31, 5.56) vs. 3.10 (2.59, 3.77), P < 0.001]. With a hepatic artery diameter cutoff value of 4.06 mm, the optimal area under the operating characteristic curve was 0.940 (95% confidence interval: 0.908–0.972), with a sensitivity of 0.887, a specificity of 0.892, a positive predictive value of 0.904, and a negative predictive value of 0.874 for identifying bleeding risk in the test cohort, while in the validation cohort, the sensitivity was 0.885, specificity was 0.939, positive predictive value was 0.920, and negative predictive value was 0.912.
Conclusion
Hepatic artery diameter has high diagnostic performance in identifying bleeding risk after GOV treatment.
Graphical abstract







Similar content being viewed by others
References
Franchis R de, Bosch J, Garcia-Tsao G, et al. Baveno VII – Renewing consensus in portal hypertension. Journal of Hepatology. 2022;76(4):959-974. https://doi.org/10.1016/j.jhep.2021.12.022
Chinese Society of Hepatology, Chinese Society of Gastroenterology, and Chinese Society of Digestive Endoscopology of Chinese Medical Association. [Guidelines on the management of esophagogastric variceal bleeding in cirrhotic portal hypertension]. Zhonghua Gan Zang Bing Za Zhi. 2022;30(10):1029–1043. https://doi.org/10.3760/cma.j.cn501113-20220824-00436
Carbonell N, Pauwels A, Serfaty L, Fourdan O, Lévy VG, Poupon R. Improved survival after variceal bleeding in patients with cirrhosis over the past two decades. Hepatology. 2004;40(3):652-659. https://doi.org/10.1002/hep.20339
Rogal SS, Hansen L, Patel A, et al. AASLD Practice Guidance: Palliative care and symptom-based management in decompensated cirrhosis. Hepatology. 2022;76(3):819-853. https://doi.org/10.1002/hep.32378
European Association for the Study of the Liver. Electronic address: easloffice@easloffice.eu, European Association for the Study of the Liver. EASL Clinical Practice Guidelines for the management of patients with decompensated cirrhosis. J Hepatol. 2018;69(2):406–460. https://doi.org/10.1016/j.jhep.2018.03.024
Assy N, Rosser BG, Grahame GR, Minuk GY. Risk of sedation for upper GI endoscopy exacerbating subclinical hepatic encephalopathy in patients with cirrhosis. Gastrointest Endosc. 1999;49(6):690-694. https://doi.org/10.1016/s0016-5107(99)70283-x
Vasudevan AE, Goh KL, Bulgiba AM. Impairment of psychomotor responses after conscious sedation in cirrhotic patients undergoing therapeutic upper GI endoscopy. Am J Gastroenterol. 2002;97(7):1717-1721. https://doi.org/10.1111/j.1572-0241.2002.05831.x
Manchec B, Pham E, Noor M, et al. Contrast-Enhanced CT May Identify High-Risk Esophageal Varices in Patients With Cirrhosis. American Journal of Roentgenology. 2020;215(3):617-623. https://doi.org/10.2214/AJR.19.22474
Kim SH, Kim YJ, Lee JM, et al. Esophageal varices in patients with cirrhosis: multidetector CT esophagography--comparison with endoscopy. Radiology. 2007;242(3):759-768. https://doi.org/10.1148/radiol.2423050784
Han X, An W, Cao Q, Liu C, Shang S, Zhao L. Noninvasive evaluation of esophageal varices in cirrhotic patients based on spleen hemodynamics: a dual-energy CT study. Eur Radiol. 2020;30(6):3210-3216. https://doi.org/10.1007/s00330-020-06680-5
Lennartz S, Parakh A, Cao J, Zopfs D, Große Hokamp N, Kambadakone A. Inter-scan and inter-scanner variation of quantitative dual-energy CT: evaluation with three different scanner types. Eur Radiol. 2021;31(7):4438-4451. https://doi.org/10.1007/s00330-020-07611-0
Peng Y, Li R, Tang G, Wang K, Sun M, Guan J. Correlation of Riolan’s arch diameter to treatment choice in patients with isolated superior mesenteric artery dissection. Abdom Radiol (NY). 2022;47(10):3628-3637. https://doi.org/10.1007/s00261-022-03622-1
Guan J, Peng Y, Ouyang L, et al. Evaluation of Therapeutic Effects on Collateral Circulation in Patients with Chronic Leriche Syndrome: a Case-Control Study of Intraluminal Stent Implantation and Surgical Bypass Grafting. Cardiovasc Intervent Radiol. 2021;44(4):550-557. https://doi.org/10.1007/s00270-020-02766-1
Toni R, Bolondi L, Gaiani S, et al. Accessory ultrasonographic findings in chronic liver disease: diameter of splenic and hepatic arteries, fasting gallbladder volume, and course of left portal vein. J Clin Ultrasound. 1985;13(9):611-618.
Aoki H, Hasumi A, Hashizume M, Kato H, Moriyasu F, Idezuki Y. Hemodynamic analysis of findings in patients with portal hypertension: multicenter analysis in Japan. Japan Portal Hypertension Study Group. Hepatogastroenterology. 1995;42(6):1030-1038.
Iwakiri Y. Pathophysiology of portal hypertension. Clin Liver Dis. 2014;18(2):281-291. https://doi.org/10.1016/j.cld.2013.12.001
Iwakiri Y. The molecules: mechanisms of arterial vasodilatation observed in the splanchnic and systemic circulation in portal hypertension. J Clin Gastroenterol. 2007;41 Suppl 3:S288-294. https://doi.org/10.1097/MCG.0b013e3181468b4c
Michels NA. Newer anatomy of the liver and its variant blood supply and collateral circulation. Am J Surg. 1966;112(3):337-347. https://doi.org/10.1016/0002-9610(66)90201-7
Hiatt JR, Gabbay J, Busuttil RW. Surgical anatomy of the hepatic arteries in 1000 cases. Ann Surg. 1994;220(1):50-52. https://doi.org/10.1097/00000658-199407000-00008
Tajiri T, Yoshida H, Obara K, et al. General rules for recording endoscopic findings of esophagogastric varices (2nd edition). Dig Endosc. 2010;22(1):1–9. https://doi.org/10.1111/j.1443-1661.2009.00929.x
Morishita N, Hiramatsu N, Oze T, et al. Liver stiffness measurement by acoustic radiation force impulse is useful in predicting the presence of esophageal varices or high-risk esophageal varices among patients with HCV-related cirrhosis. J Gastroenterol. 2014;49(7):1175-1182. https://doi.org/10.1007/s00535-013-0877-z
Wu L, Fang QQ, Huang XQ, et al. Risk factors associated with failure of endoscopic combined treatment to prevent varices rebleeding in patients with liver cirrhosis. Expert Rev Gastroenterol Hepatol. 2023;17(3):301-308. https://doi.org/10.1080/17474124.2023.2181787
D’Amico G, Pasta L, Morabito A, et al. Competing risks and prognostic stages of cirrhosis: a 25-year inception cohort study of 494 patients. Aliment Pharmacol Ther. 2014;39(10):1180-1193. https://doi.org/10.1111/apt.12721
Turco L, Reiberger T, Vitale G, La Mura V. Carvedilol as the new non-selective beta-blocker of choice in patients with cirrhosis and portal hypertension. Liver Int. 2023;43(6):1183-1194. https://doi.org/10.1111/liv.15559
Sauerbruch T, Mengel M, Dollinger M, et al. Prevention of Rebleeding From Esophageal Varices in Patients With Cirrhosis Receiving Small-Diameter Stents Versus Hemodynamically Controlled Medical Therapy. Gastroenterology. 2015;149(3):660-668.e1. https://doi.org/10.1053/j.gastro.2015.05.011
Attia D, Rodt T, Marquardt S, et al. Shear wave elastography prior to transjugular intrahepatic portosystemic shunt may predict the decrease in hepatic vein pressure gradient. Abdom Radiol (NY). 2019;44(3):1127-1134. https://doi.org/10.1007/s00261-018-1795-6
Mattos ÂZ, Schacher FC, John Neto G, Mattos AA. Screening for esophageal varices in cirrhotic patients - Non-invasive methods. Ann Hepatol. 2019;18(5):673-678. https://doi.org/10.1016/j.aohep.2019.06.003
Cankal F, Kaya M, Guner MA. Evaluation of Celiac Trunk, Hepatic Artery Variations, and Their Collateral Arteries by Multi-Slice Computed Tomography. Sisli Etfal Hastan Tip Bul. 2021;55(2):217-223. https://doi.org/10.14744/SEMB.2021.90698
Zeng DB, Dai CZ, Lu SC, He N, Wang W, Li HJ. Abnormal splenic artery diameter/hepatic artery diameter ratio in cirrhosis-induced portal hypertension. World J Gastroenterol. 2013;19(8):1292-1298. https://doi.org/10.3748/wjg.v19.i8.1292
Funding
This work was supported by Hainan Provincial Natural Science Foundation of China (Grant No. 821RC677); Joint Program on Health Science & Technology Innovation of Hainan Province (SQ2023WSJK0041); and the Hainan Province Clinical Medical Center.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict interest.
Ethical approval
The institutional ethics committee has approved this retrospective study and has waived the requirement of informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, G., Cai, Q., Qin, X. et al. Hepatic artery diameter predicts bleeding risk after gastroesophageal varices treatment: a contrast-enhanced CT study. Abdom Radiol (2024). https://doi.org/10.1007/s00261-024-04291-y
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00261-024-04291-y