Abstract
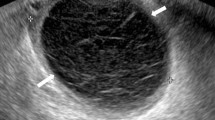
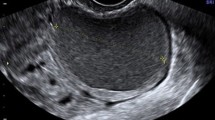
Adnexal masses during pregnancy are a relatively uncommon entity. Their clinical management is challenging given the overlapping features of certain entities on imaging and histopathology, which can mimic malignancy, and the potential side effects to the mother and fetus, whether expectant management versus surgery is pursued. Ultrasonography with Doppler evaluation is the modality of choice for evaluating adnexal masses during pregnancy. Magnetic resonance imaging is the second-line modality useful when US findings are inconclusive/indeterminate. Most adnexal masses in pregnant patients are benign in origin (e.g., functional cysts, mature cystic teratoma, decidualization of endometrioma), but a few are malignant in origin (e.g., dysgerminoma, granulosa cell tumor). Most cases of adnexal masses are asymptomatic, but complications such as ovarian torsion can occur. This review aims to familiarize the radiologist with the imaging of adnexal lesions during pregnancy so that the radiologist can identify ovarian cancer. Specifically, the review will detail the most common benign and malignant adnexal masses in pregnancy, mimickers, and their corresponding imaging findings on US and MRI.














Similar content being viewed by others
References
Thomassin-Naggara I, Fedida B, Sadowski E, Chevrier MC, Chabbert-Buffet N, Ballester M, et al. Complex US adnexal masses during pregnancy: Is pelvic MR imaging accurate for characterization? Eur J Radiol. 2017;93:200-8. https://doi.org/10.1016/j.ejrad.2017.05.024.
Whitecar MP, Turner S, Higby MK. Adnexal masses in pregnancy: a review of 130 cases undergoing surgical management. Am J Obstet Gynecol. 1999;181(1):19-24. https://doi.org/10.1016/s0002-9378(99)70429-1.
Hakoun AM, AbouAl-Shaar I, Zaza KJ, Abou-Al-Shaar H, MN AS. Adnexal masses in pregnancy: An updated review. Avicenna J Med. 2017;7(4):153–7. https://doi.org/10.4103/ajm.AJM_22_17.
Telischak NA, Yeh BM, Joe BN, Westphalen AC, Poder L, Coakley FV. MRI of adnexal masses in pregnancy. AJR Am J Roentgenol. 2008;191(2):364-70. https://doi.org/10.2214/ajr.07.3509.
Yacobozzi M, Nguyen D, Rakita D. Adnexal masses in pregnancy. Semin Ultrasound CT MR. 2012;33(1):55-64. https://doi.org/10.1053/j.sult.2011.10.004.
D'Ambrosio V, Brunelli R, Musacchio L, Del Negro V, Vena F, Boccuzzi G, et al. Adnexal masses in pregnancy: an updated review on diagnosis and treatment. Tumori. 2021;107(1):12-6. https://doi.org/10.1177/0300891620909144.
Forstner R, Thomassin-Naggara I, Cunha TM, Kinkel K, Masselli G, Kubik-Huch R, et al. ESUR recommendations for MR imaging of the sonographically indeterminate adnexal mass: an update. Eur Radiol. 2017;27(6):2248-57. https://doi.org/10.1007/s00330-016-4600-3.
Morice P, Uzan C, Gouy S, Verschraegen C, Haie-Meder C. Gynaecological cancers in pregnancy. Lancet. 2012;379(9815):558-69. https://doi.org/10.1016/s0140-6736(11)60829-5.
Korenaga TK, Tewari KS. Gynecologic cancer in pregnancy. Gynecol Oncol. 2020;157(3):799-809. https://doi.org/10.1016/j.ygyno.2020.03.015.
Lee SJ, Oh HR, Na S, Hwang HS, Lee SM. Ultrasonographic ovarian mass scoring system for predicting malignancy in pregnant women with ovarian mass. Obstet Gynecol Sci. 2022;65(1):1-13. https://doi.org/10.5468/ogs.21212.
Leiserowitz GS, Xing G, Cress R, Brahmbhatt B, Dalrymple JL, Smith LH. Adnexal masses in pregnancy: how often are they malignant? Gynecol Oncol. 2006;101(2):315-21. https://doi.org/10.1016/j.ygyno.2005.10.022.
Schmeler KM, Mayo-Smith WW, Peipert JF, Weitzen S, Manuel MD, Gordinier ME. Adnexal masses in pregnancy: surgery compared with observation. Obstet Gynecol. 2005;105(5 Pt 1):1098-103. https://doi.org/10.1097/01.AOG.0000157465.99639.e5.
Yen CF, Lin SL, Murk W, Wang CJ, Lee CL, Soong YK, et al. Risk analysis of torsion and malignancy for adnexal masses during pregnancy. Fertil Steril. 2009;91(5):1895-902. https://doi.org/10.1016/j.fertnstert.2008.02.014.
Aggarwal P, Kehoe S. Ovarian tumours in pregnancy: a literature review. Eur J Obstet Gynecol Reprod Biol. 2011;155(2):119-24. https://doi.org/10.1016/j.ejogrb.2010.11.023.
Committee Opinion No. 723: Guidelines for Diagnostic Imaging During Pregnancy and Lactation. Obstet Gynecol. 2017;130(4):e210-e6. https://doi.org/10.1097/aog.0000000000002355.
Ray JG, Vermeulen MJ, Bharatha A, Montanera WJ, Park AL. Association Between MRI Exposure During Pregnancy and Fetal and Childhood Outcomes. Jama. 2016;316(9):952-61. https://doi.org/10.1001/jama.2016.12126.
Horowitz JM, Hotalen IM, Miller ES, Barber EL, Shahabi S, Miller FH. How Can Pelvic MRI with Diffusion-Weighted Imaging Help My Pregnant Patient? Am J Perinatol. 2020;37(6):577-88. https://doi.org/10.1055/s-0039-1685492.
Vandecaveye V, Amant F, Lecouvet F, Van Calsteren K, Dresen RC. Imaging modalities in pregnant cancer patients. Int J Gynecol Cancer. 2021;31(3):423-31. https://doi.org/10.1136/ijgc-2020-001779.
Jung DC, Kim SH, Kim SH. MR imaging findings of ovarian cystadenofibroma and cystadenocarcinofibroma: clues for the differential diagnosis. Korean J Radiol. 2006;7(3):199-204. https://doi.org/10.3348/kjr.2006.7.3.199.
Petkovska I, Duke E, Martin DR, Irani Z, Geffre CP, Cragun JM, et al. MRI of ovarian torsion: Correlation of imaging features with the presence of perifollicular hemorrhage and ovarian viability. Eur J Radiol. 2016;85(11):2064-71. https://doi.org/10.1016/j.ejrad.2016.09.020.
Takeuchi M, Matsuzaki K, Uehara H, Nishitani H. Malignant transformation of pelvic endometriosis: MR imaging findings and pathologic correlation. Radiographics. 2006;26(2):407-17. https://doi.org/10.1148/rg.262055041.
Cusidó M, Fábregas R, Pere BS, Escayola C, Barri PN. Ovulation induction treatment and risk of borderline ovarian tumors. Gynecol Endocrinol. 2007;23(7):373-6. https://doi.org/10.1080/09513590701350341.
Mittal K, Koticha R, Dey AK, Anandpara K, Agrawal R, Sarvothaman MP, et al. Radiological illustration of spontaneous ovarian hyperstimulation syndrome. Pol J Radiol. 2015;80:217-27. https://doi.org/10.12659/pjr.893536.
Blake EA, Carter CM, Kashani BN, Kodama M, Mabuchi S, Yoshino K, et al. Feto-maternal outcomes of pregnancy complicated by ovarian sex-cord stromal tumor: a systematic review of literature. Eur J Obstet Gynecol Reprod Biol. 2014;175:1-7. https://doi.org/10.1016/j.ejogrb.2013.12.025.
Chen Y, Luo Y, Han C, Tian W, Yang W, Wang Y, et al. Ovarian dysgerminoma in pregnancy: A case report and literature review. Cancer Biol Ther. 2018;19(8):649-58. https://doi.org/10.1080/15384047.2018.1450118.
Litzka C, Leebmann H, Wiesinger H, Kirchner T, Seelbach-Göbel B, Häusler SFM. [Management of intra-abdominal dysgerminoma During pregnancy - A Case Report and Literature Review]. Z Geburtshilfe Neonatol. 2020;224(5):306-14. https://doi.org/10.1055/a-1112-0506.
Ngwenya S. Ovarian dysgerminoma presenting as a pregnancy: case report. Trop Doct. 2017;47(1):69-71. https://doi.org/10.1177/0049475516659415.
Alrjoub MM, Sindiani A, Alshriedeh O, Amarin Z. Pregnancy and Delivery After Ovarian Yolk Sac Tumor: A Case Report. Am J Case Rep. 2021;22:e932091. https://doi.org/10.12659/ajcr.932091.
Miyamoto M, Takano M, Goto T, Kato M, Sasaki N, Furuya K. Ovarian yolk sac tumor associated with pregnancy: a case report and review of the literature. Eur J Gynaecol Oncol. 2014;35(6):738-40.
Shaaban AM, Rezvani M, Elsayes KM, Baskin H, Jr., Mourad A, Foster BR, et al. Ovarian malignant germ cell tumors: cellular classification and clinical and imaging features. Radiographics. 2014;34(3):777-801. https://doi.org/10.1148/rg.343130067.
Fauvet R, Brzakowski M, Morice P, Resch B, Marret H, Graesslin O, et al. Borderline ovarian tumors diagnosed during pregnancy exhibit a high incidence of aggressive features: results of a French multicenter study. Ann Oncol. 2012;23(6):1481-7. https://doi.org/10.1093/annonc/mdr452.
Mooney J, Silva E, Tornos C, Gershenson D. Unusual features of serous neoplasms of low malignant potential during pregnancy. Gynecol Oncol. 1997;65(1):30-5. https://doi.org/10.1006/gyno.1996.4592.
Sahin H, Akdogan AI, Smith J, Zawaideh JP, Addley H. Serous borderline ovarian tumours: an extensive review on MR imaging features. Br J Radiol. 2021;94(1125):20210116. https://doi.org/10.1259/bjr.20210116.
Acknowledgements
The authors would like to thank Joanne Chin, MFA, ELS, for her editorial support.
Funding
This work was funded in part through the NIH/NCI Cancer Center Support Grant P30 CA008748.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
For this review, no ethical approval is required.
Informed consent
For this type of study formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Causa Andrieu, P.I., Wahab, S.A., Nougaret, S. et al. Ovarian cancer during pregnancy. Abdom Radiol 48, 1694–1708 (2023). https://doi.org/10.1007/s00261-022-03768-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03768-y