Abstract
Purpose
The need for incorporation of quantitative imaging biomarkers of pancreatic parenchymal and ductal structures has been highlighted in recent proposals for new scoring systems in chronic pancreatitis (CP). To quantify inter- and intra-observer variability in CT-based measurements of ductal- and gland diameters in CP patients.
Materials and Methods
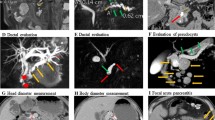
Prospectively acquired pancreatic CT examinations from 50 CP patients were reviewed by 12 radiologists and four pancreatologists from 10 institutions. Assessment entailed measuring maximum diameter in the axial plane of four structures: (1) pancreatic head (PDhead), (2) pancreatic body (PDbody), (3) main pancreatic duct in the pancreatic head (MPDhead), and (4) body (MPDbody). Agreement was assessed by the 95% limits of agreement with the mean (LOAM), representing how much a single measurement for a specific subject may plausibly deviate from the mean of all measurements on the specific subject. Bland–Altman limits of agreement (LoA) were generated for intra-observer pairs.
Results
The 16 observers completed 6400 caliper placements comprising a first and second measurement session. The widest inter-observer LOAM was seen with PDhead (± 9.1 mm), followed by PDbody (± 5.1 mm), MPDhead (± 3.2 mm), and MPDbody (± 2.6 mm), whereas the mean intra-observer LoA width was ± 7.3, ± 5.1, ± 3.7, and ± 2.4 mm, respectively.
Conclusion
Substantial intra- and inter-observer variability was observed in pancreatic two-point measurements. This was especially pronounced for parenchymal and duct diameters of the pancreatic head. These findings challenge the implementation of two-point measurements as the foundation for quantitative imaging scoring systems in CP.
Graphical abstract




Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- CP:
-
Chronic pancreatitis
- ICC:
-
Intraclass correlation coefficient
- LoA:
-
Limits of agreement
- DICOM:
-
Digital Imaging and Communications in Medicine
- PDhead:
-
Largest parenchymal diameter of the pancreatic head
- PDbody:
-
Largest parenchymal diameter of the pancreatic body
- MPDhead:
-
Largest main pancreatic duct diameter in the pancreatic head
- MPDbody:
-
Largest main pancreatic duct diameter in the pancreatic body
- MRI:
-
Magnetic resonance imaging
- SBPC:
-
Scandinavian Baltic Pancreatic Club
- LOAM:
-
Limits of agreement with the mean
References
Muniraj, T., Aslanian, H. R., Farrell, J. & Jamidar, P. A. Chronic pancreatitis, a comprehensive review and update. Part I: epidemiology, etiology, risk factors, genetics, pathophysiology, and clinical features. Dis. Mon. 60, 530–550 (2014).
Conwell, D. L. et al. American Pancreatic Association Practice Guidelines in Chronic Pancreatitis: evidence-based report on diagnostic guidelines. Pancreas 43, 1143–1162 (2014).
Frøkjær, J. B. et al. Guidelines for the Diagnostic Cross Sectional Imaging and Severity Scoring of Chronic Pancreatitis. Pancreatology 18, 764–773 (2018).
Tirkes, T. et al. Reporting Standards for Chronic Pancreatitis by Using CT, MRI, and MR Cholangiopancreatography: The Consortium for the Study of Chronic Pancreatitis, Diabetes, and Pancreatic Cancer. Radiology 290, 207–215 (2019).
Dasyam, A. K., Shah, Z. K., Tirkes, T., Dasyam, N. & Borhani, A. A. Cross-sectional imaging-based severity scoring of chronic pancreatitis: why it is necessary and how it can be done. Abdom Radiol (NY) 45, 1447–1457 (2020).
Sarner, M. & Cotton, P. B. Classification of pancreatitis. Gut 25, 756–759 (1984).
Whitcomb, D. C. et al. Chronic pancreatitis: An international draft consensus proposal for a new mechanistic definition. Pancreatology 16, 218–224 (2016).
Kumar, H., DeSouza, S. V. & Petrov, M. S. Automated pancreas segmentation from computed tomography and magnetic resonance images: A systematic review. Comput. Methods Programs Biomed. 178, 319–328 (2019).
Steinkohl, E. et al. Progression of parenchymal and ductal findings in patients with chronic pancreatitis: A 4-year follow-up MRI study. Eur. J. Radiol. 125, 108868 (2020).
Kipp, J. P. et al. Normal pancreatic volume in adults is influenced by visceral fat, vertebral body width and age. Abdominal Radiology vol. 44 958–966 (2019).
Lisitskaya, M. V. et al. Systematic approach for assessment of imaging features in chronic pancreatitis: a feasibility and validation study from the Scandinavian Baltic Pancreatic Club (SBPC) database. Abdom Radiol (NY) 45, 1468–1480 (2020).
Razek, A. A. K. A., Elfar, E. & Abubacker, S. Interobserver agreement of computed tomography reporting standards for chronic pancreatitis. Abdom Radiol (NY) 44, 2459–2465 (2019).
Olesen, S. S., Laukkarinen, J., Drewes, A. M. & Nojgaard, C. The Scandinavian Baltic Pancreatic Club (SBPC) Database: Design, Rationale and Characterisation of the Study Cohort. Pancreatology vol. 17 S58 (2017).
Schneider, A., Löhr, J. M. & Singer, M. V. The M-ANNHEIM classification of chronic pancreatitis: introduction of a unifying classification system based on a review of previous classifications of the disease. J. Gastroenterol. 42, 101–119 (2007).
Borgbjerg, J. Novel web-based tool for conducting observer performance studies in imaging research. (2016), accessed 25 August 2022, <https://epos.myesr.org/poster/esr/ecr2016/C-1635>.
Borgbjerg, J. MULRECON: A Web-based Imaging Viewer for Visualization of Volumetric Images. Curr. Probl. Diagn. Radiol. 48, 531–534 (2019).
Borgbjerg, J. Web-based imaging viewer for real-color volumetric reconstruction of human visible project and DICOM datasets. Clin. Anat. 34, 470–477 (2021).
Christensen, H. S., Borgbjerg, J., Børty, L. & Bøgsted, M. On Jones et al.’s method for extending Bland-Altman plots to limits of agreement with the mean for multiple observers. BMC Med. Res. Methodol. 20, 304 (2020).
McGraw, K. O. & Wong, S. P. Forming inferences about some intraclass correlation coefficients. Psychological Methods vol. 1 30–46 (1996).
Cohen, J. Statistical Power Analysis for the Behavioral Sciences. (Routledge, 2013).
deSouza, N. M. et al. Validated imaging biomarkers as decision-making tools in clinical trials and routine practice: current status and recommendations from the EIBALL* subcommittee of the European Society of Radiology (ESR). Insights Imaging 10, 87 (2019).
Farzin, B. et al. Agreement studies in radiology research. Diagn. Interv. Imaging 98, 227–233 (2017).
Trout, A. T. et al. Interobserver Agreement for CT and MRI Findings of Chronic Pancreatitis in Children: A Multicenter Ancillary Study Under the INSPPIRE Consortium. AJR Am. J. Roentgenol. 1–11 (2022).
Trout, A. T. et al. Normal pancreatic parenchymal thickness by CT in healthy children. Pediatr. Radiol. 48, 1600–1605 (2018).
Bankier, A. A., Levine, D., Halpern, E. F. & Kressel, H. Y. Consensus Interpretation in Imaging Research: Is There a Better Way? Radiology vol. 257 14–17 (2010).
McNitt-Gray, M. F. et al. Determining the Variability of Lesion Size Measurements from CT Patient Data Sets Acquired under ‘No Change’ Conditions. Translational Oncology vol. 8 55–64 (2015).
Bankier, A. A. et al. Recommendations for Measuring Pulmonary Nodules at CT: A Statement from the Fleischner Society. Radiology 285, 584–600 (2017).
Anaizi, A., Hart, P. A. & Conwell, D. L. Diagnosing Chronic Pancreatitis. Dig. Dis. Sci. 62, 1713–1720 (2017).
Funding
This work did not receive any grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors attest that they meet the current International Committee of Medical Journal Editors (ICMJE) criteria for Authorship and have made contributions to the paper as follows JB, ES, SSO, HSC, JBF: Conception and design of the study. JB, ES, SSO, FA, AB, EB, TE, ISH, NK, MVL, GN, SN, IO-Z, AEP, JKS, AMD, JBF: Acquisition of data. JB, ES, SSO, FA, AB, EB, HSC, TE, ISH, NK, MVL, GN, SN, IO-Z, AEP, JKS, AMD, JBF: Analysis and interpretation of data. JB, HSC, JBF: Drafting the article. JB, ES, SSO, FA, AB, EB, HSC, TE, ISH, NK, MVL, GN, SN, IO-Z, AEP, JKS, AMD, JBF: Revising the article. JB, ES, SSO, FA, AB, EB, HSC, TE, ISH, NK, MVL, GN, SN, IO-Z, AEP, JKS, AMD, JBF: Final approval.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest to disclose.
Research involving human and animal participants
The authors declare that the work described has been carried out in accordance with the Declaration of Helsinki of the World Medical Association revised in 2013 for experiments involving humans. Informed consent and patient details The authors declare that this report does not contain any personal information that could lead to the identification of the patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary video A (MP4 1294 KB)
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Borgbjerg, J., Steinkohl, E., Olesen, S.S. et al. Inter- and intra-observer variability of computed tomography-based parenchymal- and ductal diameters in chronic pancreatitis: a multi-observer international study. Abdom Radiol 48, 306–317 (2023). https://doi.org/10.1007/s00261-022-03667-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03667-2