Abstract
Purpose
In this preliminary study, our aim was to assess the utility of quantitative native-T1 (T1-pre), iron-corrected T1 (cT1) of the liver/spleen and T1 mapping of the liver obtained during hepatobiliary phase (T1-HBP) post-gadoxetate disodium, compared to spleen size/volume and APRI (aspartate aminotransferase-to-platelet ratio index) for noninvasive diagnosis of clinically significant portal hypertension [CSPH, defined as hepatic venous pressure gradient (HVPG) ≥ 10 mm Hg].
Methods
Forty-nine patients (M/F: 27/22, mean age 53y) with chronic liver disease, HVPG measurement and MRI were included. Breath-held T1 and cT1 measurements were obtained using an inversion recovery Look-Locker sequence and a T2* corrected modified Look-Locker sequence, respectively. Liver T1-pre (n = 49), spleen T1 (obtained pre-contrast, n = 47), liver and spleen cT1 (both obtained pre-contrast, n = 30), liver T1-HBP (obtained 20 min post gadoxetate disodium injection, n = 36) and liver T1 uptake (ΔT1, n = 36) were measured. Spleen size/volume and APRI were also obtained. Spearman correlation coefficients were used to assess the correlation between each of liver/spleen T1/cT1 parameters, spleen size/volume and APRI with HVPG. ROC analysis was performed to determine the performance of measured parameters for diagnosis of CSPH.
Results
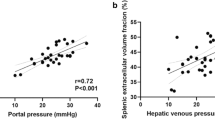
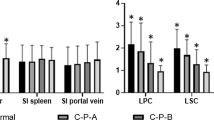
There were 12/49 (24%) patients with CSPH. Liver T1-pre (r = 0.287, p = 0.045), liver T1-HBP (r = 0.543, p = 0.001), liver ΔT1 (r = − 0.437, p = 0.008), spleen T1 (r = 0.311, p = 0.033) and APRI (r = 0.394, p = 0.005) were all significantly correlated with HVPG, while liver cT1, spleen cT1 and spleen size/volume were not. The highest AUCs for the diagnosis of CSPH were achieved with liver T1-HBP, liver ΔT1 and spleen T1: 0.881 (95%CI 0.76–1.0, p = 0.001), 0.852 (0.72–0.98, p = 0.002) and 0.781 (0.60–0.95, p = 0.004), respectively.
Conclusion
Our preliminary results demonstrate the potential of liver T1 mapping obtained during HBP post gadoxetate disodium for the diagnosis of CSPH. These results require further validation.
Graphical abstract





Similar content being viewed by others
Abbreviations
- APRI:
-
Aspartate aminotransferase-to-platelet ratio index
- AST:
-
Aspartate aminotransferase
- AUC:
-
Area under the curve
- CSPH:
-
Clinically significant portal hypertension (defined by HVPG ≥ 10 mm Hg)
- cT1:
-
Iron-corrected longitudinal relaxation time
- HBP:
-
Hepatobiliary phase
- HVPG:
-
Hepatic venous pressure gradient
- LL IR:
-
Look-Locker Inversion Recovery
- MRE:
-
Magnetic resonance elastography
- PH:
-
Portal hypertension (defined by HVPG > 5 mmHg)
- ROC:
-
Receiver operating characteristic
- SWE:
-
Shear wave elastography
- T1:
-
Longitudinal or spin–lattice relaxation time
- TE:
-
Transient elastography
- TI:
-
Inversion time
- TJ:
-
Transjugular
- VFA:
-
Variable flip angle
References
de Franchis, R., Expanding consensus in portal hypertension: Report of the Baveno VI Consensus Workshop: Stratifying risk and individualizing care for portal hypertension. J Hepatol, 2015. 63(3): p. 743-52. https://doi.org/https://doi.org/10.1016/j.jhep.2015.05.022
Abraldes, J. G., Araujo, I. K., Turón, F., & Berzigotti, A. Diagnosing and monitoring cirrhosis: Liver biopsy, hepatic venous pressure gradient and elastography. Gastroenterol Hepatol, 2012. 35(7): p. 488-95. https://doi.org/10.1016/j.gastrohep.2012.02.010
You, M. W., Kim, K. W., Pyo, J. et al. A Meta-analysis for the Diagnostic Performance of Transient Elastography for Clinically Significant Portal Hypertension. Ultrasound Med Biol, 2017. 43(1): p. 59-68. https://doi.org/https://doi.org/10.1016/j.ultrasmedbio.2016.07.025
Kennedy, P., Bane, O., Hectors, S. J. et al. Noninvasive imaging assessment of portal hypertension. Abdom Radiol (NY), 2020. 45(11): p. 3473-3495. https://doi.org/https://doi.org/10.1007/s00261-020-02729-7
Hectors, S. J., Bane, O., Stocker, D. et al. Splenic T 1ρ as a noninvasive biomarker for portal hypertension. J Magn Reson Imaging 2020. 52(3): p. 787-794. https://doi.org/10.1002/jmri.27087
Wagner, M., Hectors, S., Bane, O. et al., Noninvasive prediction of portal pressure with MR elastography and DCE-MRI of the liver and spleen: Preliminary results. J Magn Reson Imaging, 2018. 48(4): p. 1091-1103. https://doi.org/https://doi.org/10.1002/jmri.26026
Besa, C., Wagner, M., Lo, G. et al. Detection of liver fibrosis using qualitative and quantitative MR elastography compared to liver surface nodularity measurement, gadoxetate uptake, and serum markers. J Magn Reson Imaging, 2018. 47(6): p. 1552-1561. https://doi.org/https://doi.org/10.1002/jmri.25911
Singh, S., Venkatesh, S. K., Loomba, R. et al. Magnetic resonance elastography for staging liver fibrosis in non-alcoholic fatty liver disease: a diagnostic accuracy systematic review and individual participant data pooled analysis. Eur Radiol, 2016. 26(5): p. 1431-40. https://doi.org/https://doi.org/10.1007/s00330-015-3949-z
Luetkens, J. A., Klein, S., Träber, F. et al. Quantification of Liver Fibrosis at T1 and T2 Mapping with Extracellular Volume Fraction MRI: Preclinical Results. Radiology, 2018. 288(3): p. 748-754. https://doi.org/https://doi.org/10.1148/radiol.2018180051
Bane, O., Hectors, S. J., Wagner, M. et al. Accuracy, repeatability, and interplatform reproducibility of T(1) quantification methods used for DCE-MRI: Results from a multicenter phantom study. Magn Reson Med, 2018. 79(5): p. 2564-2575. https://doi.org/https://doi.org/10.1002/mrm.26903
Mesropyan, N., Isaak, A., Faron, A. et al. Magnetic resonance parametric mapping of the spleen for non-invasive assessment of portal hypertension. Eur Radiol, 2021. 31(1): p. 85-93. https://doi.org/https://doi.org/10.1007/s00330-020-07080-5
Palaniyappan, N., Cox, E., Bradley, C. et al. Non-invasive assessment of portal hypertension using quantitative magnetic resonance imaging. J Hepatol, 2016. 65(6): p. 1131-1139. https://doi.org/https://doi.org/10.1016/j.jhep.2016.07.021
Hoffman, D. H., Ayoola, A., Nickel, D., Han, F., Chandarana, H., Shanbhogue, K. P. T1 mapping, T2 mapping and MR elastography of the liver for detection and staging of liver fibrosis. Abdom Radiol (NY), 2020. 45(3): p. 692-700. https://doi.org/https://doi.org/10.1007/s00261-019-02382-9
Ding, Y., Rao, S. X., Zhu, T., Chen, C. Z., Li, R. C., Zeng, M. S. Liver fibrosis staging using T1 mapping on gadoxetate-enhanced MRI compared with DW imaging. Clin Radiol, 2015. 70(10): p. 1096-103. https://doi.org/https://doi.org/10.1016/j.crad.2015.04.014
Obmann, V. C., Berzigotti, A., Catucci, D. et al. T1 mapping of the liver and the spleen in patients with liver fibrosis-does normalization to the blood pool increase the predictive value? Eur Radiol, 2020. https://doi.org/https://doi.org/10.1007/s00330-020-07447-8
Pan, S., X.Q. Wang, Q.Y. Guo Quantitative assessment of hepatic fibrosis in chronic hepatitis B and C: T1 mapping on Gd-EOB-DTPA-enhanced liver magnetic resonance imaging. World J Gastroenterol, 2018. 24(18): p. 2024-2035. https://doi.org/https://doi.org/10.3748/wjg.v24.i18.2024
Yoon, J. H., Lee, J. M., Paek, M., Han, J. K., Choi, B. I. Quantitative assessment of hepatic function: modified look-locker inversion recovery (MOLLI) sequence for T1 mapping on Gd-EOB-DTPA-enhanced liver MR imaging. Eur Radiol, 2016. 26(6): p. 1775-82. https://doi.org/https://doi.org/10.1007/s00330-015-3994-7
Besa, C., Bane, O., Jajamovich, G., Marchione, J., Taouli, B. 3D T1 relaxometry pre and post gadoxetate injection for the assessment of liver cirrhosis and liver function. Magn Reson Imaging, 2015. 33(9): p. 1075-1082. https://doi.org/https://doi.org/10.1016/j.mri.2015.06.013
Cassinotto, C., Feldis, M., Vergniol, J. et al. MR relaxometry in chronic liver diseases: Comparison of T1 mapping, T2 mapping, and diffusion-weighted imaging for assessing cirrhosis diagnosis and severity. Eur J Radiol, 2015. 84(8): p. 1459-1465. https://doi.org/https://doi.org/10.1016/j.ejrad.2015.05.019
Haimerl, M., Verloh, N., Zeman, F. et al. Assessment of clinical signs of liver cirrhosis using T1 mapping on Gd-EOB-DTPA-enhanced 3T MRI. PLoS One, 2013. 8(12): p. e85658. https://doi.org/https://doi.org/10.1371/journal.pone.0085658
Katsube, T., Okada, M., Kumano, S. et al. Estimation of liver function using T1 mapping on Gd-EOB-DTPA-enhanced magnetic resonance imaging. Invest Radiol, 2011. 46(4): p. 277-83. https://doi.org/https://doi.org/10.1097/RLI.0b013e318200f67d
Hoffman, D. H., Ayoola, A., Nickel, D. et al. MR elastography, T1 and T2 relaxometry of liver: role in noninvasive assessment of liver function and portal hypertension. Abdom Radiol (NY), 2020. 45(9): p. 2680-2687. https://doi.org/https://doi.org/10.1007/s00261-020-02432-7
Haimerl, M., Verloh, N., Fellner, C. et al. MRI-based estimation of liver function: Gd-EOB-DTPA-enhanced T1 relaxometry of 3T vs. the MELD score. Sci Rep, 2014. 4: p. 5621. https://doi.org/https://doi.org/10.1038/srep05621
Kim, K. A., Park, M. S., Kim, I. S. et al. Quantitative evaluation of liver cirrhosis using T1 relaxation time with 3 tesla MRI before and after oxygen inhalation. J Magn Reson Imaging, 2012. 36(2): p. 405-10. https://doi.org/https://doi.org/10.1002/jmri.23620
Zhou, Z. P., Long, L. L., Qiu, W. J. et al. Comparison of 10- and 20-min hepatobiliary phase images on Gd-EOB-DTPA-enhanced MRI T1 mapping for liver function assessment in clinic. Abdom Radiol (NY), 2017. 42(9): p. 2272-2278. https://doi.org/https://doi.org/10.1007/s00261-017-1143-2
Nakagawa, M., Namimoto, T., Shimizu, K. et al. Measuring hepatic functional reserve using T1 mapping of Gd-EOB-DTPA enhanced 3T MR imaging: A preliminary study comparing with (99m)Tc GSA scintigraphy and signal intensity based parameters. Eur J Radiol, 2017. 92: p. 116-123. https://doi.org/https://doi.org/10.1016/j.ejrad.2017.05.011
Yoon, J. H., Lee, J. M., Kim, E., Okuaki, T., & Han, J. K. Quantitative Liver Function Analysis: Volumetric T1 Mapping with Fast Multisection B(1) Inhomogeneity Correction in Hepatocyte-specific Contrast-enhanced Liver MR Imaging. Radiology, 2017. 282(2): p. 408-417. https://doi.org/https://doi.org/10.1148/radiol.2016152800
Kim, J. E., Kim, H. O., Bae, K., Choi, D. S., & Nickel, D. T1 mapping for liver function evaluation in gadoxetate-enhanced MR imaging: comparison of look-locker inversion recovery and B(1) inhomogeneity-corrected variable flip angle method. Eur Radiol, 2019. 29(7): p. 3584-3594. https://doi.org/https://doi.org/10.1007/s00330-018-5947-4
Kamimura, K., Fukukura, Y., Yoneyama, T. et al. Quantitative evaluation of liver function with T1 relaxation time index on Gd-EOB-DTPA-enhanced MRI: comparison with signal intensity-based indices. J Magn Reson Imaging, 2014. 40(4): p. 884-9. https://doi.org/https://doi.org/10.1002/jmri.24443
Yoneyama, T., Fukukura, Y., Kamimura, K. et al. Efficacy of liver parenchymal enhancement and liver volume to standard liver volume ratio on Gd-EOB-DTPA-enhanced MRI for estimation of liver function. Eur Radiol, 2014. 24(4): p. 857-65. https://doi.org/https://doi.org/10.1007/s00330-013-3086-5
Yoon, J. H., Lee, J. M., Kang, H. J. et al. Quantitative Assessment of Liver Function by Using Gadoxetate-enhanced MRI: Hepatocyte Uptake Ratio. Radiology, 2019. 290(1): p. 125-133. https://doi.org/https://doi.org/10.1148/radiol.2018180753
Yamada, A., Hara, T., Li, F., Fujinaga, Y., Ueda, K., Kadoya, M., & Doi, K. (2011). Quantitative evaluation of liver function with use of gadoxetate disodium–enhanced MR imaging. Radiology, 260(3), 727-733. https://doi.org/https://doi.org/10.1148/radiol.11100586
Levick, C., Phillips-Hughes, J., Collier, J. et al. Non-invasive assessment of portal hypertension by multi-parametric magnetic resonance imaging of the spleen: A proof of concept study. PLoS One, 2019. 14(8): p. e0221066. https://doi.org/10.1371/journal.pone.0221066
Lin, Z. H., Xin, Y. N., Dong, Q. J. et al. Performance of the aspartate aminotransferase-to-platelet ratio index for the staging of hepatitis C-related fibrosis: an updated meta-analysis. Hepatology. 2011; 53:726-36. https://doi.org/https://doi.org/10.1002/hep.24105
Hectors, S. J., Bane, O., Kennedy, P. et al. Noninvasive diagnosis of portal hypertension using gadoxetate DCE-MRI of the liver and spleen.Eur Radiol (2021): 1-9. https://doi.org/https://doi.org/10.1007/s00330-020-07495-0
Piechnik, S. K., Ferreira VM., Dall'Armellina E. et al. Shortened Modified Look-Locker Inversion recovery (ShMOLLI) for clinical myocardial T1-mapping at 1.5 and 3 T within a 9 heartbeat breathhold." J Cardiovasc Magn Reson 12 (2010): 69. https://doi.org/https://doi.org/10.1186/1532-429X-12-69
Kennedy, P., Stocker, D., Carbonell, G. et al. MR elastography outperforms shear wave elastography for the diagnosis of clinically significant portal hypertension. Eur Radiol (2022). https://doi.org/10.1007/s00330-022-08935-9
Banerjee, R., Pavlides, M., Tunnicliffe, E. M. et al. Multiparametric magnetic resonance for the non-invasive diagnosis of liver disease. J Hepatol 60.1 (2014): 69-77. https://doi.org/https://doi.org/10.1016/j.jhep.2013.09.002
Labranche, R., Gilbert, G., Cerny, M. et al. (2018). Liver iron quantification with MR imaging: a primer for radiologists. Radiographics, 38(2), 392-412. https://doi.org/https://doi.org/10.1148/rg.2018170079
Yamada, A., Hara, T., Li, F. et al. Quantitative evaluation of liver function with use of gadoxetate disodium–enhanced MR imaging. Radiology 260.3 (2011): 727-733. https://doi.org/https://doi.org/10.1148/radiol.11100586
Dennis, A., Kelly, M. D., Fernandes, C. et al. Correlations between MRI biomarkers PDFF and cT1 with histopathological features of non-alcoholic steatohepatitis. Front Endocrinol 11 (2021): 1053. https://doi.org/https://doi.org/10.3389/fendo.2020.575843
Li, Z., Sun, J., Hu, X. et al. Assessment of liver fibrosis by variable flip angle T1 mapping at 3.0T. J Magn Reson Imaging, 2016. 43(3): p. 698-703. https://doi.org/https://doi.org/10.1002/jmri.25030
Liberman, G., Y. Louzoun, D. Ben Bashat, T1 mapping using variable flip angle SPGR data with flip angle correction. J Magn Reson Imaging, 2014. 40(1): p. 171-80. https://doi.org/https://doi.org/10.1002/jmri.24373
Acknowledgements
None.
Funding
This study has received funding by National Institute of Diabetes and Kidney Diseases (NIDDK, Grant 1R01DK113272), Perspectum, and Siemens Healthineers. None of these sponsors were involved in the collection, analysis, and interpretation of data; in the writing of the report; and in the decision to submit the article for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Bachir Taouli: consultancy and/or advisory roles for Bayer, Helio Health and research funding/support from Bayer, Takeda, Regeneron, Siemens Healthineers, Echosens, Stefanie Hectors: Employee of Regeneron, Matthew D. Kelly: Employee of Perspectum. The authors declare they have no non-financial interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was approved by the Institutional Review Board of Mount Sinai Hospital.
Consent to participate
Written informed consent was obtained from all patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Altinmakas, E., Bane, O., Hectors, S.J. et al. Performance of native and gadoxetate-enhanced liver and spleen T1 mapping for noninvasive diagnosis of clinically significant portal hypertension: preliminary results. Abdom Radiol 47, 3758–3769 (2022). https://doi.org/10.1007/s00261-022-03645-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03645-8