Abstract
Purpose
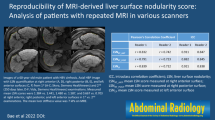
To compare the MRI-derived liver surface nodularity (LSN) scores acquired on both 1.5 T and 3 T.
Materials and methods
Forty chronic liver disease patients who underwent gadoxetic acid-enhanced MRI at both 1.5 and 3 T were included. Axial hepatobiliary phase images with the same voxel size were used to calculate the LSN score in both liver lobes with a quantitative software. Rank correlation, Wilcoxon test, and Bland–Altman limits of agreement were used for statistical analysis.
Results
There was a weak correlation between the right and left liver lobe on 1.5 T (rs = 0.331, p = 0.037) and 3 T (rs = 0.381, p = 0.015). The correlation between 1.5 T and 3 T on both liver lobes showed a very strong correlation (right, rs = 0.927, p < 0.001; left, rs = 0.845, p < 0.001). LSN scores differed significantly between both lobes on 1.5 T (median, 1.201 vs. 0.674, right vs. left) and 3 T (1.076 vs. 0.592) (all p < 0.001). LSN scores differed significantly between 1.5 T and 3 T on both lobes (all p < 0.001). The Bland–Altman plot comparing 1.5 T and 3 T on right and left liver lobes showed a systemic bias of 0.08 and 0.07, respectively.
Conclusions
LSN scores differed significantly on 1.5 T vs. 3 T and right vs. left liver lobe. Caution should be made when comparing LSN scores derived from different field strengths or the hepatic lobe. Interplatform, interlobar reproducibility should be resolved to use LSN scores, which is relatively easy to perform without additional hardware or images.




Similar content being viewed by others
Abbreviations
- LF::
-
Liver fibrosis
- CLD::
-
Chronic liver disease
- HBV::
-
Hepatitis B virus
- HCV::
-
Hepatitis C virus
- NAFLD::
-
Nonalcoholic fatty liver disease
- HCC::
-
Hepatocellular carcinoma
- LSN::
-
Liver surface nodularity
- HBP::
-
Hepatobiliary phase
- WALTS::
-
Wonkwang Abdomen and Liver Total Solution
- IQR::
-
Interquartile range
- CV::
-
Coefficient of variation
References
Bataller R, Brenner DA (2005) Liver fibrosis. J Clin Invest 115 (2):209-218. doi:https://doi.org/10.1172/JCI24282
Asrani SK, Devarbhavi H, Eaton J, Kamath PS (2019) Burden of liver diseases in the world. J Hepatol 70 (1):151-171. doi:https://doi.org/10.1016/j.jhep.2018.09.014
Stepanova M, De Avila L, Afendy M, Younossi I, Pham H, Cable R, Younossi ZM (2017) Direct and Indirect Economic Burden of Chronic Liver Disease in the United States. Clin Gastroenterol Hepatol 15 (5):759-766 e755. doi:https://doi.org/10.1016/j.cgh.2016.07.020
Bedossa P, Poynard T (1996) An algorithm for the grading of activity in chronic hepatitis C. The METAVIR Cooperative Study Group. Hepatology 24 (2):289-293. doi:https://doi.org/10.1002/hep.510240201
Rockey DC, Caldwell SH, Goodman ZD, Nelson RC, Smith AD, American Association for the Study of Liver D (2009) Liver biopsy. Hepatology 49 (3):1017-1044. doi:https://doi.org/10.1002/hep.22742
Bedossa P, Carrat F (2009) Liver biopsy: the best, not the gold standard. J Hepatol 50 (1):1-3. doi:https://doi.org/10.1016/j.jhep.2008.10.014
Venkatesh SK, Yin M, Takahashi N, Glockner JF, Talwalkar JA, Ehman RL (2015) Non-invasive detection of liver fibrosis: MR imaging features vs. MR elastography. Abdom Imaging 40 (4):766-775. doi:https://doi.org/10.1007/s00261-015-0347-6
Ito K, Mitchell DG, Siegelman ES (2002) Cirrhosis: MR imaging features. Magn Reson Imaging Clin N Am 10 (1):75-92, vi. doi:https://doi.org/10.1016/s1064-9689(03)00050-3
Lubner MG, Pickhardt PJ (2018) Multidetector Computed Tomography for Retrospective, Noninvasive Staging of Liver Fibrosis. Gastroenterol Clin North Am 47 (3):569-584. doi:https://doi.org/10.1016/j.gtc.2018.04.012
Smith AD, Branch CR, Zand K, Subramony C, Zhang H, Thaggard K, Hosch R, Bryan J, Vasanji A, Griswold M, Zhang X (2016) Liver Surface Nodularity Quantification from Routine CT Images as a Biomarker for Detection and Evaluation of Cirrhosis. Radiology 280 (3):771-781. doi:https://doi.org/10.1148/radiol.2016151542
Catania R, Furlan A, Smith AD, Behari J, Tublin ME, Borhani AA (2021) Diagnostic value of MRI-derived liver surface nodularity score for the non-invasive quantification of hepatic fibrosis in non-alcoholic fatty liver disease. Eur Radiol 31 (1):256-263. doi:https://doi.org/10.1007/s00330-020-07114-y
Lubner MG, Jones D, Said A, Kloke J, Lee S, Pickhardt PJ (2018) Accuracy of liver surface nodularity quantification on MDCT for staging hepatic fibrosis in patients with hepatitis C virus. Abdom Radiol (NY) 43 (11):2980-2986. doi:https://doi.org/10.1007/s00261-018-1572-6
Besa C, Wagner M, Lo G, Gordic S, Chatterji M, Kennedy P, Stueck A, Thung S, Babb J, Smith A, Taouli B (2018) Detection of liver fibrosis using qualitative and quantitative MR elastography compared to liver surface nodularity measurement, gadoxetic acid uptake, and serum markers. J Magn Reson Imaging 47 (6):1552-1561. doi:https://doi.org/10.1002/jmri.25911
Kim TH, Kim JE, Ryu JH, Jeong CW (2019) Development of liver surface nodularity quantification program and its clinical application in nonalcoholic fatty liver disease. Sci Rep 9 (1):9994. doi:https://doi.org/10.1038/s41598-019-46442-y
Kim SW, Kim YR, Choi KH, Cho EY, Song JS, Kim JE, Kim TH, Lee YH, Yoon KH (2020) Staging of Liver Fibrosis by Means of Semiautomatic Measurement of Liver Surface Nodularity in MRI. AJR Am J Roentgenol 215 (3):624-630. doi:https://doi.org/10.2214/AJR.19.22041
Kim YK, Kim CS, Han YM, Yu HC, Choi D (2011) Detection of small hepatocellular carcinoma: intraindividual comparison of gadoxetic acid-enhanced MRI at 3.0 and 1.5 T. Invest Radiol 46 (6):383-389. doi:https://doi.org/10.1097/RLI.0b013e318217b8fb
Akoglu H (2018) User's guide to correlation coefficients. Turk J Emerg Med 18 (3):91-93. doi:https://doi.org/10.1016/j.tjem.2018.08.001
Smith A, Varney E, Zand K, Lewis T, Sirous R, York J, Florez E, Abou Elkassem A, Howard-Claudio CM, Roda M, Parker E, Scortegagna E, Joyner D, Sandlin D, Newsome A, Brewster P, Lirette ST, Griswold M (2018) Precision analysis of a quantitative CT liver surface nodularity score. Abdom Radiol (NY) 43 (12):3307-3316. doi:https://doi.org/10.1007/s00261-018-1617-x
Smith AD, Zand KA, Florez E, Sirous R, Shlapak D, Souza F, Roda M, Bryan J, Vasanji A, Griswold M, Lirette ST (2017) Liver Surface Nodularity Score Allows Prediction of Cirrhosis Decompensation and Death. Radiology 283 (3):711-722. doi:https://doi.org/10.1148/radiol.2016160799
Sohrabpour AA, Mohamadnejad M, Malekzadeh R (2012) Review article: the reversibility of cirrhosis. Aliment Pharmacol Ther 36 (9):824-832. doi:https://doi.org/10.1111/apt.12044
Castera L (2012) Noninvasive methods to assess liver disease in patients with hepatitis B or C. Gastroenterology 142 (6):1293-1302.e1294. doi:https://doi.org/10.1053/j.gastro.2012.02.017
De Vos N, Sartoris R, Cauchy F, Rautou PE, Vilgrain V, Ronot M (2020) Performance of liver surface nodularity quantification for the diagnosis of portal hypertension in patients with cirrhosis: comparison between MRI with hepatobiliary phase sequences and CT. Abdom Radiol (NY) 45 (2):365-372. doi:https://doi.org/10.1007/s00261-019-02355-y
Dyvorne HA, Jajamovich GH, Bane O, Fiel MI, Chou H, Schiano TD, Dieterich D, Babb JS, Friedman SL, Taouli B (2016) Prospective comparison of magnetic resonance imaging to transient elastography and serum markers for liver fibrosis detection. Liver International 36 (5):659-666. doi:https://doi.org/10.1111/liv.13058
Elster AD (1997) How much contrast is enough?. Dependence of enhancement on field strength and MR pulse sequence. Eur Radiol 7 Suppl 5:276-280. doi:https://doi.org/10.1007/pl00006908
Kim T-H, Kim YR, Jeong C-W, Lee C, Noh S, Kim JE, Lee YH, Yoon K-H Regional variation of liver surface nodularity scores for evaluating hepatic fi brosis on asingle axial MR image. . In: Proc. Intl. Soc. Mag. Reson. Med., 2021. vol 29. p 2758
Motulsky H, Christopoulos A (2004) Fitting models to biological data using linear and nonlinear regression: a practical guide to curve fitting. Oxford University Press, Oxford
Acknowledgements
This study was supported by the grant of the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare (HI18C1216). The authors thank Wade Martin of Emareye Medical Editing Service for his assistance in editing the article.
Funding
None to be declared.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jang, W., Song, J.S., Kim, TH. et al. Intraindividual comparison of MRI-derived liver surface nodularity score at 1.5 T and 3 T. Abdom Radiol 47, 1053–1060 (2022). https://doi.org/10.1007/s00261-022-03415-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03415-6