Abstract
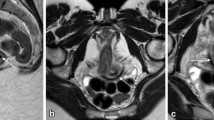
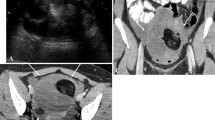
Pelvic tumors are common in females and have a broad differential diagnosis. The clinical management of pelvic tumors varies widely—from observation to surgical resection—and imaging plays a pivotal role in diagnosis and clinical decision-making in these cases. In particular, imaging can help determine the organ of origin and tissue content of these tumors, which are the most important steps to narrowing the differential diagnosis. Fat has a characteristic appearance and is often easily identified on ultrasonography (US), computed tomography (CT), and magnetic resonance imaging (MRI). The amount and distribution of intralesional fat varies in different types of tumors. Macroscopic intralesional fat is often easily recognized by its hyperechoic appearance on US and low attenuation on CT similar to subcutaneous fat. On MRI, macroscopic fat is hyperintense on T1-weighted (T1W) images, with characteristic signal loss on fat-saturated sequences and India-ink artifact on opposed-phase T1W images. Macroscopic fat is the hallmark of teratomas, which are the most common ovarian neoplasms. Uterine lipoleiomyomas, peritoneal loose bodies, intraperitoneal and extraperitoneal primary lipomatous tumors such as lipoma and liposarcomas, and extra-adrenal myelolipomas are other pelvic masses distinguished by the presence of macroscopic fat. However, the imaging diagnosis of pelvic masses containing minimal or microscopic fat, such as immature ovarian teratomas, steroid cell ovarian neoplasms, and extramedullary hematopoiesis, can present a diagnostic challenge owing to their nonspecific appearance on US or CT. Obtaining MRI with in-phase and opposed-phase dual-echo T1W sequences and depicting chemical shift artifacts can be helpful in distinguishing these lesions.


















Similar content being viewed by others
Data availability
The author(s) declare(s) that they had full access to all of the data in this study and the author(s) take(s) complete responsibility for the integrity of the data and the accuracy of the data analysis.
References:
Dodd, G.D., 3rd and R.F. Budzik, Jr., Lipomatous tumors of the pelvis in women: spectrum of imaging findings. AJR Am J Roentgenol, 1990. 155(2): p. 317–22.
2.Foti, P.V., et al., MR imaging of ovarian masses: classification and differential diagnosis. Insights Imaging, 2016. 7(1): p. 21-41.
3.Jeong, Y.Y., E.K. Outwater, and H.K. Kang, Imaging evaluation of ovarian masses. Radiographics, 2000. 20(5): p. 1445-70.
4.Jung, S.E., et al., CT and MR imaging of ovarian tumors with emphasis on differential diagnosis. Radiographics, 2002. 22(6): p. 1305-25.
5.Luczak, J. and M. Baglaj, Ovarian teratoma in children: a plea for collaborative clinical study. J Ovarian Res, 2018. 11(1): p. 75.
6.Outwater, E.K., E.S. Siegelman, and J.L. Hunt, Ovarian teratomas: tumor types and imaging characteristics. Radiographics, 2001. 21(2): p. 475-90.
7.Sahin, H., S. Abdullazade, and M. Sanci, Mature cystic teratoma of the ovary: a cutting edge overview on imaging features. Insights Imaging, 2017. 8(2): p. 227-241.
8.Jung, S.E., et al., Xanthogranulomatous oophoritis: MR imaging findings with pathologic correlation. AJR Am J Roentgenol, 2002. 178(3): p. 749-51.
9.Maruyama, M., et al., MR Imaging of Xanthogranulomatous Oophoritis. Magn Reson Med Sci, 2018. 17(3): p. 191-192.
10.Jiang, W., et al., Benign and malignant ovarian steroid cell tumors, not otherwise specified: case studies, comparison, and review of the literature. J Ovarian Res, 2013. 6: p. 53.
11.Saida, T., Y.O. Tanaka, and M. Minami, Steroid cell tumor of the ovary, not otherwise specified: CT and MR findings. AJR Am J Roentgenol, 2007. 188(4): p. W393-4.
12.Liu, A.X., et al., Steroid cell tumors, not otherwise specified (NOS), in an accessory ovary: a case report and literature review. Gynecol Oncol, 2005. 97(1): p. 260-2.
64.Kocaoglu, M. and D.P. Frush, Pediatric presacral masses. Radiographics, 2006. 26(3): p. 833-57.
13.Sakamoto, K., et al., MR diagnosis of steroid cell tumor of the ovary: value of chemical shift imaging. Magn Reson Med Sci, 2009. 8(4): p. 193-5.
14.Shaaban, A.M., et al., Ovarian malignant germ cell tumors: cellular classification and clinical and imaging features. Radiographics, 2014. 34(3): p. 777-801.
15.Faten, H., et al., Ovarian Steroid Cell Tumor (Not Otherwise Specified): A Case Report of Ovarian Hyperandrogenism. Case Rep Oncol Med, 2020. 2020: p. 6970823.
16.Haroon, S., et al., Ovarian steroid cell tumor, not otherwise specified: a clinicopathological and immunohistochemical experience of 12 cases. J Obstet Gynaecol Res, 2015. 41(3): p. 424-31.
17.Das, A., S. Panda, and A.S. Singh, Steroid cell tumor: A rare virilizing ovarian tumor. J Cancer Res Ther, 2015. 11(3): p. 660.
18.Wang, P.H., et al., Steroid cell tumors of the ovary: clinical, ultrasonic, and MRI diagnosis--a case report. Eur J Radiol, 1998. 26(3): p. 269-73.
Dodd, G.D., 3rd and R.F. Budzik, Jr., Lipomatous uterine tumors: diagnosis by ultrasound, CT, and MR. J Comput Assist Tomogr, 1990. 14(4): p. 629–32.
Hertzberg, B.S., et al., Lipomatous uterine masses: potential to mimic ovarian dermoids on endovaginal sonography. J Ultrasound Med, 1995. 14(9): p. 689–92; quiz 693–4.
21.Tsushima, Y., T. Kita, and K. Yamamoto, Uterine lipoleiomyoma: MRI, CT and ultrasonographic findings. Br J Radiol, 1997. 70(838): p. 1068-70.
22.Kitajima, K., et al., MRI findings of uterine lipoleiomyoma correlated with pathologic findings. AJR Am J Roentgenol, 2007. 189(2): p. W100-4.
23.Arikawa, S., et al., Significance of the "beak sign" in the differential diagnosis of uterine lipoleiomyoma from ovarian dermoid cyst. Kurume Med J, 2006. 53(1-2): p. 37-40.
24.Nougaret, S., et al., MRI of Tumors and Tumor Mimics in the Female Pelvis: Anatomic Pelvic Space-based Approach. Radiographics, 2019. 39(4): p. 1205-1229.
A Kamaya, M.P.F.T.S.D., Imaging manifestations of abdominal fat necrosis and its mimics. Radiographics, 2011. 31(7): p. 2021–2034.
26.Gayer, G., I. Petrovitch, and R.B. Jeffrey, Foreign objects encountered in the abdominal cavity at CT. Radiographics, 2011. 31(2): p. 409-28.
27.Ghosh, P., et al., Peritoneal mice implicated in intestinal obstruction: report of a case and review of the literature. J Clin Gastroenterol, 2006. 40(5): p. 427-30.
28.Huang, C.H., et al., Numerous peritoneal loose bodies with ileus. Histopathology, 2011. 58(2): p. 318-9.
29.Huang, Q., et al., Two giant peritoneal loose bodies were simultaneously found in one patient: A case report and review of the literature. Int J Surg Case Rep, 2017. 36: p. 74-77.
30.Zhang, H., et al., Giant peritoneal loose body in the pelvic cavity confirmed by laparoscopic exploration: a case report and review of the literature. World J Surg Oncol, 2015. 13: p. 118.
37.Paunipagar, B.K., et al., Ultrasound features of deep-seated lipomas. Insights Imaging, 2010. 1(3): p. 149-153.
38.Gupta, P., et al., Spectrum of Fat-containing Soft-Tissue Masses at MR Imaging: The Common, the Uncommon, the Characteristic, and the Sometimes Confusing. Radiographics, 2016. 36(3): p. 753-66.
39.Drylewicz, M.R., et al., Fatty masses of the abdomen and pelvis and their complications. Abdom Radiol (NY), 2019. 44(4): p. 1535-1553.
40.Kransdorf, M.J., et al., Imaging of fatty tumors: distinction of lipoma and well-differentiated liposarcoma. Radiology, 2002. 224(1): p. 99-104.
32.Drevelegas, A., M. Pilavaki, and D. Chourmouzi, Lipomatous tumors of soft tissue: MR appearance with histological correlation. Eur J Radiol, 2004. 50(3): p. 257-67.
41.Papathanassiou, Z.G., et al., Imaging of hibernomas: A retrospective study on twelve cases. Clin Sarcoma Res, 2011. 1(1): p. 3.
42.Pandya, A. and A.P. Wasnik, Presacral hibernoma: Radiologic-pathologic correlation. Indian J Radiol Imaging, 2011. 21(4): p. 270-3.
Tsapralis, N., et al., Unusual "Dumbbell"-Shaped Hibernoma. Plast Reconstr Surg Glob Open, 2019. 7(4): p. e2142.
44.Cohade, C., K.A. Mourtzikos, and R.L. Wahl, "USA-Fat": prevalence is related to ambient outdoor temperature-evaluation with 18F-FDG PET/CT. J Nucl Med, 2003. 44(8): p. 1267-70.
46.Kim, J.D. and H.W. Lee, Hibernoma: Intense Uptake on F18-FDG PET/CT. Nucl Med Mol Imaging, 2012. 46(3): p. 218-22.
51.Fisher, M.F., et al., Abdominal lipoblastomatosis: radiographic, echographic, and computed tomographic findings. Radiology, 1981. 138(3): p. 593-6.
52.Moholkar, S., N.J. Sebire, and D.J. Roebuck, Radiological-pathological correlation in lipoblastoma and lipoblastomatosis. Pediatr Radiol, 2006. 36(8): p. 851-6.
34.Levy, A.D., M.A. Manning, and M.M. Miettinen, Soft-Tissue Sarcomas of the Abdomen and Pelvis: Radiologic-Pathologic Features, Part 2-Uncommon Sarcomas. Radiographics, 2017. 37(3): p. 797-812.
47.Sung, M.S., et al., Myxoid liposarcoma: appearance at MR imaging with histologic correlation. Radiographics, 2000. 20(4): p. 1007-19.
Wang, L., et al., Pleomorphic liposarcoma: An analysis of 6 case reports and literature review. Medicine (Baltimore), 2018. 97(8): p. e9986.
36.Shaaban, A.M., et al., Fat-containing Retroperitoneal Lesions: Imaging Characteristics, Localization, and Differential Diagnosis. Radiographics, 2016. 36(3): p. 710-34.
49.Hong, S.H., et al., Dedifferentiated liposarcoma of retroperitoneum: spectrum of imaging findings in 15 patients. Clin Imaging, 2010. 34(3): p. 203-10.
Tateishi, U., et al., Primary dedifferentiated liposarcoma of the retroperitoneum. Prognostic significance of computed tomography and magnetic resonance imaging features. J Comput Assist Tomogr, 2003. 27(5): p. 799–804.
53.Itani, M., A.P. Wasnik, and J.F. Platt, Radiologic-pathologic correlation in extra-adrenal myelolipoma. Abdom Imaging, 2014. 39(2): p. 394-7.
54.Tokuyama, N., et al., Incidental Presacral Myelolipoma Resembling the Liposarcoma: A Case Report and Literature Review. Case Rep Urol, 2016. 2016: p. 6510930.
55.Patel, N., et al., Imaging of presacral masses--a multidisciplinary approach. Br J Radiol, 2016. 89(1061): p. 20150698.
56.Wadood, D.Q., et al., A rare case of co-existing adrenal and pelvic myelolipomas. Radiol Case Rep, 2018. 13(5): p. 999-1002.
57.Littrell, L.A., et al., Extra-adrenal myelolipoma and extramedullary hematopoiesis: Imaging features of two similar benign fat-containing presacral masses that may mimic liposarcoma. Eur J Radiol, 2017. 93: p. 185-194.
58.Fowler, M.R., et al., Extra-adrenal myelolipomas compared with extramedullary hematopoietic tumors: a case of presacral myelolipoma. Am J Surg Pathol, 1982. 6(4): p. 363-74.
45.Smith, C.S., et al., False-positive findings on 18F-FDG PET/CT: differentiation of hibernoma and malignant fatty tumor on the basis of fluctuating standardized uptake values. AJR Am J Roentgenol, 2008. 190(4): p. 1091-6.
59.Ginzel, A.W., et al., Mass-like extramedullary hematopoiesis: imaging features. Skeletal Radiol, 2012. 41(8): p. 911-6.
60.Roberts, A.S., et al., Extramedullary haematopoiesis: radiological imaging features. Clin Radiol, 2016. 71(9): p. 807-14.
61.Avni, F.E., et al., MR imaging of fetal sacrococcygeal teratoma: diagnosis and assessment. AJR Am J Roentgenol, 2002. 178(1): p. 179-83.
62.Danzer, E., et al., Diagnosis and characterization of fetal sacrococcygeal teratoma with prenatal MRI. AJR Am J Roentgenol, 2006. 187(4): p. W350-6.
63.Yoon, H.M., et al., Sacrococcygeal teratomas in newborns: a comprehensive review for the radiologists. Acta Radiol, 2018. 59(2): p. 236-246.
65.Yoo, E., et al., A case of mesenteric cystic lymphangioma: fat saturation and chemical shift MR imaging. Journal of Magnetic Resonance Imaging: An Official Journal of the International Society for Magnetic Resonance in Medicine, 2006. 23(1): p. 77-80.
31.Akcalar, S., et al., Imaging findings of lipomatosis: a comprehensive review. Jpn J Radiol, 2013. 31(1): p. 1-8.
33.Kim, T., et al., CT and MR imaging of abdominal liposarcoma. AJR Am J Roentgenol, 1996. 166(4): p. 829-33.
35.Pickhardt, P.J. and S. Bhalla, Primary neoplasms of peritoneal and sub-peritoneal origin: CT findings. Radiographics, 2005. 25(4): p. 983-95.
Funding
No financial support/funding.
Author information
Authors and Affiliations
Contributions
All authors contributed to this paper with conception and design of the study, literature review and analysis, drafting and critical revision and editing, and final approval of the final version.
Corresponding author
Ethics declarations
Conflict of interest
No potential conflicts of interest.
Ethical approval
Compliance with ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fattahi, N., Moeini, A., Morani, A.C. et al. Fat-containing pelvic lesions in females. Abdom Radiol 47, 362–377 (2022). https://doi.org/10.1007/s00261-021-03299-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-021-03299-y