Abstract
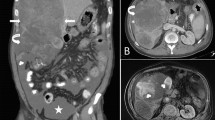
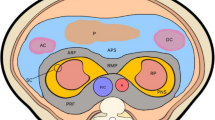
Hemorrhage is a potential complication of benign and malignant tumors and tumor-like conditions in the abdomen. Patients often have non-specific presentations, although they may present critically ill and hemodynamically unstable. Imaging plays an important role not only in the diagnosis of hemorrhage but also in the detection and characterization of an underlying mass. Ultrasound, computed tomography, and magnetic resonance imaging are utilized in evaluating these patients, with each having particular strengths and limitations. Spontaneous tumor hemorrhage is most commonly seen in hepatic and renal lesions, although it can arise from nearly every abdominal organ. In this article, we will review principles of tumor hemorrhage, illustrate common and uncommon imaging features, and highlight different options for management.










Similar content being viewed by others
References
Lai EC, Lau WY. Spontaneous rupture of hepatocellular carcinoma: a systematic review. Arch Surg 2006;141(2):191–198. https://doi.org/10.1001/archsurg.141.2.191
Chang SY, Ma CP, Lee SK. Spontaneous retroperitoneal hemorrhage from kidney causes. Eur Urol 1988;15(3–4):281–284. https://doi.org/10.1159/000473452
Yoshida H, Mamada Y, Taniai N, Uchida E. Spontaneous ruptured hepatocellular carcinoma. Hepatol Res 2016;46(1):13–21. https://doi.org/10.1111/hepr.12498
Thomas AJ, Menias CO, Pickhardt PJ, Shaaban AM, Gaballah AH, Yedururi S, Elsayes KM. Bleeding Liver Masses: Imaging Features With Pathologic Correlation and Impact on Management. AJR Am J Roentgenol 2019:1–9. https://doi.org/10.2214/AJR.19.21240
Revel-Mouroz P, Mokrane FZ, Collot S, Chabbert V, Rousseau H, Meyrignac O, Otal P. Hemostastic embolization in oncology. Diagn Interv Imaging 2015;96(7–8):807–821. https://doi.org/10.1016/j.diii.2015.06.008
Whitworth PW, 3rd, Dyer RB. The "Page kidney". Abdom Radiol (NY) 2017;42(9):2387–2388. https://doi.org/10.1007/s00261-017-1139-y
Smyth A, Collins CS, Thorsteinsdottir B, Madsen BE, Oliveira GH, Kane G, Garovic VD. Page kidney: etiology, renal function outcomes and risk for future hypertension. J Clin Hypertens (Greenwich) 2012;14(4):216–221. https://doi.org/10.1111/j.1751-7176.2012.00601.x
Lubner M, Menias C, Rucker C, Bhalla S, Peterson CM, Wang L, Gratz B. Blood in the belly: CT findings of hemoperitoneum. Radiographics 2007;27(1):109–125. https://doi.org/10.1148/rg.271065042
Tirkes T, Sandrasegaran K, Patel AA, Hollar MA, Tejada JG, Tann M, Akisik FM, Lappas JC. Peritoneal and retroperitoneal anatomy and its relevance for cross-sectional imaging. Radiographics 2012;32(2):437–451. https://doi.org/10.1148/rg.322115032
Savatmongkorngul S, Wongwaisayawan S, Kaewlai R. Focused assessment with sonography for trauma: current perspectives. Open Access Emerg Med 2017;9:57–62. https://doi.org/10.2147/OAEM.S120145
Perera P, Mailhot T, Riley D, Mandavia D. The RUSH exam: Rapid Ultrasound in SHock in the evaluation of the critically lll. Emerg Med Clin North Am 2010;28(1):29–56, vii. https://doi.org/10.1016/j.emc.2009.09.010
Shiozawa K, Watanabe M, Ikehara T, Matsukiyo Y, Ishii K, Igarashi Y, Sumino Y. Usefulness of contrast-enhanced ultrasonography in the diagnosis of ruptured hepatocellular carcinoma. Clin J Gastroenterol 2013;6(4):334–337. https://doi.org/10.1007/s12328-013-0398-6
Sun H, Hou XY, Xue HD, Li XG, Jin ZY, Qian JM, Yu JC, Zhu HD. Dual-source dual-energy CT angiography with virtual non-enhanced images and iodine map for active gastrointestinal bleeding: image quality, radiation dose and diagnostic performance. Eur J Radiol 2015;84(5):884–891. https://doi.org/10.1016/j.ejrad.2015.01.013
Kalisz K, Halliburton S, Abbara S, Leipsic JA, Albrecht MH, Schoepf UJ, Rajiah P. Update on Cardiovascular Applications of Multienergy CT. Radiographics 2017;37(7):1955–1974. https://doi.org/10.1148/rg.2017170100
Lall C, Bura V, Lee TK, Bhosale P, Faria SC, Choi JI, Wang ZJ. Diffusion-weighted imaging in hemorrhagic abdominal and pelvic lesions: restricted diffusion can mimic malignancy. Abdom Radiol (NY) 2018;43(7):1772–1784. https://doi.org/10.1007/s00261-017-1366-2
Expert Panels on Vascular I, Gastrointestinal I, Singh-Bhinder N, Kim DH, Holly BP, Johnson PT, Hanley M, Carucci LR, Cash BD, Chandra A, Gage KL, Lambert DL, Levy AD, Oliva IB, Peterson CM, Strax R, Rybicki FJ, Dill KE. ACR Appropriateness Criteria((R)) Nonvariceal Upper Gastrointestinal Bleeding. J Am Coll Radiol 2017;14(5S):S177–S188. https://doi.org/10.1016/j.jacr.2017.02.038
Allen TW, Tulchinsky M. Nuclear medicine tests for acute gastrointestinal conditions. Semin Nucl Med 2013;43(2):88–101. https://doi.org/10.1053/j.semnuclmed.2012.11.001
Wilson MW, Fidelman N, Lull RJ, Marder SR, Laberge JM, Kerlan RK, Jr., Gordon RL. Evaluation of active bleeding into hematomas by technetium-99m red blood cell scintigraphy before angiography. Clin Nucl Med 2002;27(11):763–766. https://doi.org/10.1097/00003072-200211000-00001
Tang A, Hallouch O, Chernyak V, Kamaya A, Sirlin CB. Epidemiology of hepatocellular carcinoma: target population for surveillance and diagnosis. Abdom Radiol (NY) 2018;43(1):13–25. https://doi.org/10.1007/s00261-017-1209-1
Singh Bhinder N, Zangan SM. Hepatocellular carcinoma rupture following transarterial chemoembolization. Semin Intervent Radiol 2015;32(1):49–53. https://doi.org/10.1055/s-0034-1396964
Cerny M, Chernyak V, Olivie D, Billiard JS, Murphy-Lavallee J, Kielar AZ, Elsayes KM, Bourque L, Hooker JC, Sirlin CB, Tang A. LI-RADS Version 2018 Ancillary Features at MRI. Radiographics 2018;38(7):1973–2001. https://doi.org/10.1148/rg.2018180052
Kow AW, Kwon CH, Song S, Shin M, Kim JM, Joh JW. Risk factors of peritoneal recurrence and outcome of resected peritoneal recurrence after liver resection in hepatocellular carcinoma: review of 1222 cases of hepatectomy in a tertiary institution. Ann Surg Oncol 2012;19(7):2246–2255. https://doi.org/10.1245/s10434-012-2260-3
Barthelmes L, Tait IS. Liver cell adenoma and liver cell adenomatosis. HPB (Oxford) 2005;7(3):186–196. https://doi.org/10.1080/13651820510028954
Dokmak S, Paradis V, Vilgrain V, Sauvanet A, Farges O, Valla D, Bedossa P, Belghiti J. A single-center surgical experience of 122 patients with single and multiple hepatocellular adenomas. Gastroenterology 2009;137(5):1698–1705. https://doi.org/10.1053/j.gastro.2009.07.061
Khanna M, Ramanathan S, Fasih N, Schieda N, Virmani V, McInnes MD. Current updates on the molecular genetics and magnetic resonance imaging of focal nodular hyperplasia and hepatocellular adenoma. Insights Imaging 2015;6(3):347–362. https://doi.org/10.1007/s13244-015-0399-8
Ribeiro MA, Jr., Papaiordanou F, Goncalves JM, Chaib E. Spontaneous rupture of hepatic hemangiomas: A review of the literature. World J Hepatol 2010;2(12):428–433. https://doi.org/10.4254/wjh.v2.i12.428
Prasanna PM, Fredericks SE, Winn SS, Christman RA. Best cases from the AFIP: giant cavernous hemangioma. Radiographics 2010;30(4):1139–1144. https://doi.org/10.1148/rg.304095198
Lantinga MA, Gevers TJ, Drenth JP. Evaluation of hepatic cystic lesions. World J Gastroenterol 2013;19(23):3543–3554. https://doi.org/10.3748/wjg.v19.i23.3543
Molina E, Hernandez A. Clinical manifestations of primary hepatic angiosarcoma. Dig Dis Sci 2003;48(4):677–682. https://doi.org/10.1023/a:1022868221670
Pickhardt PJ, Kitchin D, Lubner MG, Ganeshan DM, Bhalla S, Covey AM. Primary hepatic angiosarcoma: multi-institutional comprehensive cancer centre review of multiphasic CT and MR imaging in 35 patients. Eur Radiol 2015;25(2):315–322. https://doi.org/10.1007/s00330-014-3442-0
Lee SW, Song CY, Gi YH, Kang SB, Kim YS, Nam SW, Lee DS, Kim JO. Hepatic angiosarcoma manifested as recurrent hemoperitoneum. World J Gastroenterol 2008;14(18):2935–2938. https://doi.org/10.3748/wjg.14.2935
Disibio G, French SW. Metastatic patterns of cancers: results from a large autopsy study. Arch Pathol Lab Med 2008;132(6):931–939. https://doi.org/10.1043/1543-2165(2008)132[931:MPOCRF]2.0.CO;2
Casillas VJ, Amendola MA, Gascue A, Pinnar N, Levi JU, Perez JM. Imaging of nontraumatic hemorrhagic hepatic lesions. Radiographics 2000;20(2):367–378. https://doi.org/10.1148/radiographics.20.2.g00mc10367
Zhang JQ, Fielding JR, Zou KH. Etiology of spontaneous perirenal hemorrhage: a meta-analysis. J Urol 2002;167(4):1593–1596. https://doi.org/10.1097/00005392-200204000-00006
Diaz JR, Agriantonis DJ, Aguila J, Calleros JE, Ayyappan AP. Spontaneous perirenal hemorrhage: what radiologists need to know. Emerg Radiol 2011;18(4):329–334. https://doi.org/10.1007/s10140-011-0944-9
Kim KH, Yun BH, Jung SI, Hwang IS, Hwang EC, Kang TW, Kwon DD, Park K, Kim JW. Usefulness of the ice-cream cone pattern in computed tomography for prediction of angiomyolipoma in patients with a small renal mass. Korean J Urol 2013;54(8):504–509. https://doi.org/10.4111/kju.2013.54.8.504
Pokharel SS, Macura KJ, Kamel IR, Zaheer A. Current MR imaging lipid detection techniques for diagnosis of lesions in the abdomen and pelvis. Radiographics 2013;33(3):681–702. https://doi.org/10.1148/rg.333125068
Li YL, Lee KH, Yu ML, Lau V. The sunburst sign in renal angiomyolipoma. Abdom Radiol (NY) 2018;43(5):1279–1280. https://doi.org/10.1007/s00261-017-1295-0
Papanicolaou N, Pfister RC, Yoder IC. Spontaneous and traumatic rupture of renal cysts: diagnosis and outcome. Radiology 1986;160(1):99–103. https://doi.org/10.1148/radiology.160.1.3715054
Hiraki Y, Okamoto D, Nishie A, Asayama Y, Ishigami K, Ushijima Y, Takayama Y, Fujita N, Eto M, Kinoshita F, Honda H. Papillary renal cell carcinoma with massive hematoma mimicking hemangioma. Radiol Case Rep 2019;14(8):1003–1006. https://doi.org/10.1016/j.radcr.2019.05.025
Marti JL, Millet J, Sosa JA, Roman SA, Carling T, Udelsman R. Spontaneous adrenal hemorrhage with associated masses: etiology and management in 6 cases and a review of 133 reported cases. World J Surg 2012;36(1):75–82. https://doi.org/10.1007/s00268-011-1338-6
Nixon AM, Botou A, Aggeli C, Falidas E, Choreftaki T, Zografos GN. Haemorrhage in pre-existing adrenal masses. A case series. Int J Surg Case Rep 2020;69:76–78. https://doi.org/10.1016/j.ijscr.2020.03.031
Renzulli P, Hostettler A, Schoepfer AM, Gloor B, Candinas D. Systematic review of atraumatic splenic rupture. Br J Surg 2009;96(10):1114–1121. https://doi.org/10.1002/bjs.6737
Saboo SS, Krajewski KM, O'Regan KN, Giardino A, Brown JR, Ramaiya N, Jagannathan JP. Spleen in haematological malignancies: spectrum of imaging findings. Br J Radiol 2012;85(1009):81–92. https://doi.org/10.1259/bjr/31542964
Myoteri D, Despoina M, Dellaportas D, Dionysios D, Ayiomamitis G, Georgios A, Strigklis K, Konstantinos S, Kouroumpas E, Efstratios K, Zizi-Sermpetzoglou A, Adamantia ZS. Primary angiosarcoma of the spleen: an oncological enigma. Case Rep Oncol Med 2014;2014:193036. https://doi.org/10.1155/2014/193036
Balthazar EJ, Fisher LA. Hemorrhagic complications of pancreatitis: radiologic evaluation with emphasis on CT imaging. Pancreatology 2001;1(4):306–313. https://doi.org/10.1159/000055829
Mohammadi A, Porghasem J, Esmaeili A, Ghasemi-Rad M. Spontaneous rupture of a pancreatic acinar cell carcinoma presenting as an acute abdomen. Int J Surg Case Rep 2012;3(7):293–295. https://doi.org/10.1016/j.ijscr.2012.03.025
Sagami R, Nishikiori H, Ikuyama S, Murakami K. Rupture of small cystic pancreatic neuroendocrine tumor with many microtumors. World J Gastroenterol 2017;23(37):6911–6919. https://doi.org/10.3748/wjg.v23.i37.6911
Schatz RA, Rockey DC. Gastrointestinal Bleeding Due to Gastrointestinal Tract Malignancy: Natural History, Management, and Outcomes. Dig Dis Sci 2017;62(2):491–501. https://doi.org/10.1007/s10620-016-4368-y
Costi R, Le Bian A, Creuze N, Prevot S, Cauchy F, Violi V, Smadja C. Hemoperitoneum caused by a ruptured GIST located in the posterior gastric wall managed by endoscopic diagnosis and laparoscopic treatment: case report and literature review. Surg Laparosc Endosc Percutan Tech 2011;21(6):e316–318. https://doi.org/10.1097/SLE.0b013e318231998b
Eleje GU, Eke AC, Igberase GO, Igwegbe AO, Eleje LI. Palliative interventions for controlling vaginal bleeding in advanced cervical cancer. Cochrane Database Syst Rev 2019;3:CD011000. https://doi.org/10.1002/14651858.CD011000.pub3
Pentecost MJ, Daniels JR, Teitelbaum GP, Stanley P. Hepatic chemoembolization: safety with portal vein thrombosis. J Vasc Interv Radiol 1993;4(3):347–351. https://doi.org/10.1016/s1051-0443(93)71873-4
Zou J, Li C, Chen Y, Chen R, Xue T, Xie X, Zhang L, Ren Z. Retrospective analysis of transcatheter arterial chemoembolization treatment for spontaneously ruptured hepatocellular carcinoma. Oncol Lett 2019;18(6):6423-6430. https://doi.org/10.3892/ol.2019.11037
Thomeer MG, Broker M, Verheij J, Doukas M, Terkivatan T, Bijdevaate D, De Man RA, Moelker A, JN IJ. Hepatocellular adenoma: when and how to treat? Update of current evidence. Therap Adv Gastroenterol 2016;9(6):898–912. https://doi.org/10.1177/1756283X16663882
Kuusk T, Biancari F, Lane B, Tobert C, Campbell S, Rimon U, D'Andrea V, Mehik A, Vaarala MH. Treatment of renal angiomyolipoma: pooled analysis of individual patient data. BMC Urol 2015;15:123. https://doi.org/10.1186/s12894-015-0118-2
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kalisz, K., Enzerra, M. & Mansoori, B. Overview of spontaneous intraabdominal tumor hemorrhage: etiologies, imaging findings, and management. Abdom Radiol 46, 427–440 (2021). https://doi.org/10.1007/s00261-020-02663-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-020-02663-8