Abstract
Purpose
To compare the performance of advanced radiomics analysis to morphological assessment by expert radiologists to predict a good or complete response to chemoradiotherapy in rectal cancer using baseline staging MRI.
Materials and methods
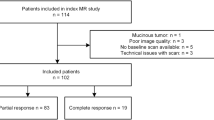
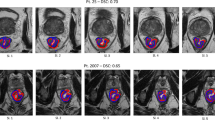
We retrospectively assessed the primary staging MRIs [prior to chemoradiotherapy (CRT)] of 133 rectal cancer patients from 2 centers. First, two expert radiologists subjectively estimated the likelihood of achieving a “complete response” (ypT0) and “good response” (TRG 1–2), using a 5-point score (based on TN-stage, MRF/EMVI-status, size/signal/shape). Next, tumor volumes were segmented on high b value DWI (semi-automated, corrected by 2 non-expert and 2-expert readers, resulting in 5 segmentations), copied to the remaining sequences after which a total of 2505 radiomic features were extracted from T2W, low and high b value DWI and ADC. Stability of features for noise due to inter-reader and inter-scanner and protocol variations was assessed using intraclass correlation (ICC) and the Kruskal–Wallis test. Using data from center 1 (n = 86; training set), top 9 features were selected using minimum Redundancy Maximum Relevance and combined in a logistic regression model. Finally, diagnostic performance of the fitted models was assessed on data from center 2 (n = 47; validation set) and compared to the performance of the radiologists.
Results
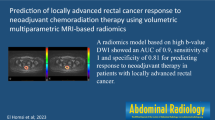
The Radiomic models resulted in AUCs of 0.69–0.79 (with similar results for the segmentations performed by expert/non-expert readers) to predict response, results similar to the morphologic prediction by the expert radiologists (AUC 0.67–0.83). Radiomics using semi-automatically generated segmentations (without manual input) did not result in significant predictive performance.
Conclusions
Radiomics could predict response to therapy with comparable diagnostic performance as expert radiologists, regardless of whether image segmentation was performed by non-expert or expert readers, indicating that expert input is not required in order for the radiomics workflow to produce significant predictive performance.



Similar content being viewed by others
References
Maas M, Beets-Tan RG, Lambregts DM, Lammering G, Nelemans PJ, Engelen SM, et al. (2011) Wait-and-see policy for clinical complete responders after chemoradiation for rectal cancer. J Clin Oncol 29:4633–40. https://doi.org/10.1200/jco.2011.37.7176.
Martens MH, Maas M, Heijnen LA, Lambregts DMJ, Leijtens JWA, Stassen LPS, et al. (2016) Long-term Outcome of an Organ Preservation Program After Neoadjuvant Treatment for Rectal Cancer. J Natl Cancer Inst 108:djw171. https://doi.org/10.1093/jnci/djw171.
van der Valk MJM, Hilling DE, Bastiaannet E, Meershoek-Klein Kranenbarg E, Beets GL, Figueiredo NL, et al. (2018) Long-term outcomes of clinical complete responders after neoadjuvant treatment for rectal cancer in the International Watch & Wait Database (IWWD): an international multicentre registry study. Lancet 391:2537–45. https://doi.org/10.1016/s0140-6736(18)31078-x.
Verseveld M, De Graaf EJR, Verhoef C, van Meerten E, Punt CJA, de Hingh IHJT, et al. (2015) Chemoradiation therapy for rectal cancer in the distal rectum followed by organ-sparing transanal endoscopic microsurgery (CARTS study). Br J Surg 102:853–60. https://doi.org/10.1002/bjs.9809.
Bujko K, Richter P, Smith FM, Polkowski W, Szczepkowski M, Rutkowski A, et al. (2013) Preoperative radiotherapy and local excision of rectal cancer with immediate radical re-operation for poor responders: a prospective multicentre study. Radiother Oncol 106:198–205. https://doi.org/10.1016/j.radonc.2012.12.005.
Rombouts AJM, Al-Najami I, Abbott NL, Appelt A, Baatrup G, Bach S, et al. (2017) Can we Save the rectum by watchful waiting or T rans A nal microsurgery following (chemo) R adiotherapy versus T otal mesorectal excision for early RE ctal C ancer (STAR-TREC study)?: protocol for a multicentre, randomised feasibility study. BMJ Open 7:e019474. https://doi.org/10.1136/bmjopen-2017-019474.
Maas M, Nelemans PJ, Valentini V, Das P, Rodel C, Kuo LJ, et al. (2010) Long-term outcome in patients with a pathological complete response after chemoradiation for rectal cancer: a pooled analysis of individual patient data. Lancet Oncol 11:835–44.
Curvo-Semedo L, Lambregts DMJ, Maas M, Thywissen T, Mehsen RT, Lammering G, et al. (2011) Rectal Cancer: Assessment of Complete Response to Preoperative Combined Radiation Therapy with Chemotherapy—Conventional MR Volumetry versus Diffusion-weighted MR Imaging. Radiology 260:734–43. https://doi.org/10.1148/radiol.11102467.
Lambregts DM, Rao SX, Sassen S, Martens MH, Heijnen LA, Buijsen J, et al. (2015) MRI and Diffusion-weighted MRI Volumetry for Identification of Complete Tumor Responders After Preoperative Chemoradiotherapy in Patients With Rectal Cancer: A Bi-institutional Validation Study. Ann Surg 262:1034–9. https://doi.org/10.1097/sla.0000000000000909.
Mahadevan LS, Zhong J, Venkatesulu B, Kaur H, Bhide S, Minsky B, et al. (2018) Imaging predictors of treatment outcomes in rectal cancer: An overview. Crit Rev Oncol Hematol 129:153–62. https://doi.org/10.1016/j.critrevonc.2018.06.009.
Hötker AM, Tarlinton L, Mazaheri Y, Woo KM, Gönen M, Saltz LB, et al. (2016) Multiparametric MRI in the assessment of response of rectal cancer to neoadjuvant chemoradiotherapy: A comparison of morphological, volumetric and functional MRI parameters. Eur Radiol:1–10. https://doi.org/10.1007/s00330-016-4283-9.
Martens MH, Subhani S, Heijnen LA, Lambregts DM, Buijsen J, Maas M, et al. (2015) Can perfusion MRI predict response to preoperative treatment in rectal cancer? Radiother Oncol 114:218–23. https://doi.org/10.1016/j.radonc.2014.11.044.
Chen Y-G, Chen M-Q, Guo Y-Y, Li S-C, Wu J-X, Xu B-H. (2016) Apparent Diffusion Coefficient Predicts Pathology Complete Response of Rectal Cancer Treated with Neoadjuvant Chemoradiotherapy. PLoS One 11:e0153944. https://doi.org/10.1371/journal.pone.0153944.
Hosny A, Parmar C, Quackenbush J, Schwartz LH, W L Aerts HJ. (2018). Artificial intelligence in radiology. https://doi.org/10.1038/s41568-018-0016-5.
Kumar V, Gu Y, Basu S, Berglund A, Eschrich SA, Schabath MB, et al. (2012) Radiomics: the process and the challenges. Magn Reson Imaging 30:1234–48. https://doi.org/10.1016/j.mri.2012.06.010.
Gillies RJ, Kinahan PE, Hricak H. (2015) Radiomics: Images Are More than Pictures, They Are Data. Radiology 278:151169. https://doi.org/10.1148/radiol.2015151169.
Aerts HJ, Velazquez ER, Leijenaar RT, Parmar C, Grossmann P, Carvalho S, et al. (2014) Decoding tumour phenotype by noninvasive imaging using a quantitative radiomics approach. Nat Commun 5:4006. https://doi.org/10.1038/ncomms5006.
Liu Z, Zhang X-Y, Shi Y-J, Wang L, Zhu H-T, Tang Z-C, et al. (2017) Radiomics Analysis for Evaluation of Pathological Complete Response to Neoadjuvant Chemoradiotherapy in Locally Advanced Rectal Cancer. Clin Cancer Res:clincanres.1038.2017. https://doi.org/10.1158/1078-0432.ccr-17-1038.
Cui Y, Yang X, Shi Z, Yang Z, Du X, Zhao Z, et al. (2019) Radiomics analysis of multiparametric MRI for prediction of pathological complete response to neoadjuvant chemoradiotherapy in locally advanced rectal cancer. Eur Radiol 29:1211–20. https://doi.org/10.1007/s00330-018-5683-9.
Cusumano D, Dinapoli N, Luca Boldrini ·, Chiloiro G, Gatta · Roberto, Masciocchi C, et al. (2018) Fractal-based radiomic approach to predict complete pathological response after chemo-radiotherapy in rectal cancer. Radiol Med 123:286–95. https://doi.org/10.1007/s11547-017-0838-3.
Mandard AM, Dalibard F, Mandard JC, Marnay J, Henry-Amar M, Petiot JF, et al. (1994) Pathologic assessment of tumor regression after preoperative chemoradiotherapy of esophageal carcinoma. Clinicopathologic correlations. Cancer 73:2680–6.
van Heeswijk MM, Lambregts DMJ, van Griethuysen JJM, Oei S, Rao S-X, de Graaff CAM, et al. (2016) Automated and Semiautomated Segmentation of Rectal Tumor Volumes on Diffusion-Weighted MRI: Can It Replace Manual Volumetry? Int J Radiat Oncol 94:824–31. https://doi.org/10.1016/j.ijrobp.2015.12.017.
Klein S, Staring M, Murphy K, Viergever MA, Pluim JPW. (2010) Elastix: A toolbox for intensity-based medical image registration. IEEE Trans Med Imaging 29:196–205. https://doi.org/10.1109/tmi.2009.2035616.
Shamonin DP, Bron EE, Lelieveldt BPF, Smits M, Klein S, Staring M, et al. (2014) Fast parallel image registration on CPU and GPU for diagnostic classification of Alzheimer’s disease for the Alzheimer’s Disease Neuroimaging Initiative. https://doi.org/10.3389/fninf.2013.00050.
van Griethuysen JJM, Fedorov A, Parmar C, Hosny A, Aucoin N, Narayan V, et al. (2017) Computational Radiomics System to Decode the Radiographic Phenotype. Cancer Res 77:e104–7. https://doi.org/10.1158/0008-5472.can-17-0339.
Collewet G, Strzelecki M, Mariette F. (2004) Influence of MRI acquisition protocols and image intensity normalization methods on texture classification. Magn Reson Imaging 22:81–91. https://doi.org/10.1016/j.mri.2003.09.001.
Pedregosa FABIANPEDREGOSA F, Michel V, Grisel OLIVIERGRISEL O, Blondel M, Prettenhofer P, Weiss R, et al. (2011). Scikit-learn: Machine Learning in Python. vol. 12.
Hanchuan Peng, Fuhui Long, Ding C. (2005) Feature selection based on mutual information criteria of max-dependency, max-relevance, and min-redundancy. IEEE Trans Pattern Anal Mach Intell 27:1226–38. https://doi.org/10.1109/tpami.2005.159.
Ross BC. (2014) Mutual Information between Discrete and Continuous Data Sets. PLoS One 9:e87357. https://doi.org/10.1371/journal.pone.0087357.
DeLong ER, DeLong DM, Clarke-Pearson DL. (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44:837–45.
Horvat N, Veeraraghavan H, Khan M, Blazic I, Zheng J, Capanu M, et al. (2018) MR Imaging of Rectal Cancer: Radiomics Analysis to Assess Treatment Response after Neoadjuvant Therapy. Radiology 287:172300. https://doi.org/10.1148/radiol.2018172300.
Nie K, Shi L, Chen Q, Hu X, Jabbour S, Yue N, et al. (2016) Rectal Cancer: Assessment of Neoadjuvant Chemo-Radiation Outcome Based on Radiomics of Multi-Parametric MRI. Clin Cancer Res. https://doi.org/10.1158/1078-0432.ccr-15-2997.
Huang Y -q., Liang C -s. C -h., He L, Tian J, Liang C -s. C -h., Chen X, et al. (2016) Development and Validation of a Radiomics Nomogram for Preoperative Prediction of Lymph Node Metastasis in Colorectal Cancer SUPPLEMENT. J Clin Oncol:JCO659128. https://doi.org/10.1200/jco.2015.65.9128.
Coroller TP, Grossmann P, Hou Y, Rios Velazquez E, Leijenaar RT, Hermann G, et al. (2015) CT-based radiomic signature predicts distant metastasis in lung adenocarcinoma. Radiother Oncol 114:345–50. https://doi.org/10.1016/j.radonc.2015.02.015.
Maas M, Lambregts DM, Nelemans PJ, Heijnen LA, Martens MH, Leijtens JW, et al. (2015) Assessment of Clinical Complete Response After Chemoradiation for Rectal Cancer with Digital Rectal Examination, Endoscopy, and MRI: Selection for Organ-Saving Treatment. Ann Surg Oncol 22:3873–80. https://doi.org/10.1245/s10434-015-4687-9.
Funding
This work was supported by the Dutch Cancer Society (KWF) (Grant No. 2016-2/10611).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Aerts declares stock options in Sphera and Genospace, all other authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
van Griethuysen, J.J.M., Lambregts, D.M.J., Trebeschi, S. et al. Radiomics performs comparable to morphologic assessment by expert radiologists for prediction of response to neoadjuvant chemoradiotherapy on baseline staging MRI in rectal cancer. Abdom Radiol 45, 632–643 (2020). https://doi.org/10.1007/s00261-019-02321-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-019-02321-8