Abstract
Purpose
To review the pertinent anatomy and the imaging features of common and uncommon benign and malignant neoplasms and masses of the ischiorectal fossa.
Results
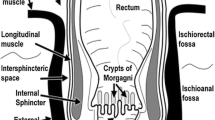
The ischiorectal or ischioanal fossa is the largest space in the anorectal region. The benign neoplasms that develop in the ischiorectal originate from the different components that forms the fossa including vascular tumors such as aggressive angiomyxoma or hemangioma; neural tumors as plexiform neurofibroma or schwannoma; fat tumors as lipoma; skin/skin appendages tumors as hidradenoma papilliferum; smooth or skeletal muscle tumors as solitary fibrous tumor. The malignant neoplasms that develop in the ischiorectal fossa also originate from different components that forms the fossa including vascular tumors such as angiosarcoma, neural tumors as malignant granular cell tumor and malignant peripheral nerve sheath tumor; fat tumors as liposarcoma; smooth or skeletal muscle tumors as leiomyosarcoma, rhabdomyosarcoma, malignant PEComa, or undifferentiated pleomorphic sarcoma. Additionally, the ischiorectal fossa can also harbor secondary hematogenous metastases and be affected by direct invasion from neoplasms of adjacent pelvic organs and structures. Furthermore, other miscellaneous masses can occur in the ischiorectal fossa including congenital and developmental lesions, and inflammatory and infectious processes.
Conclusion
Knowledge of the anatomy, and the spectrum of imaging findings of common and uncommon benign and malignant neoplasms of the ischiorectal fossa is crucial for the radiologists during interpretation of images allowing them to make contributions to the diagnosis and better patient management.


























Similar content being viewed by others
References
Moore KL, Dalley AF, Agur AMR (2014) Clinically oriented anatomy. 7th edn. Williams & Wilkins, Baltimore
Llauger J, Palmer J, Perez C, Monill JM, Ribe J, Moreno A (1998) The normal and pathologic ischiorectal fossa at CT and MR imaging. Radiographics 18 (1):61–82. https://doi.org/10.1148/radiographics.18.1.9460109
Hoeffel C, Crema MD, Azizi L, Lewin M, Monnier-Cholley L, Arrive L, Tubiana JM (2007) Magnetic resonance imaging of the ischiorectal fossa: spectrum of disease. J Comput Assist Tomogr 31 (2):251–257. https://doi.org/10.1097/01.rct.0000236419.90019.40
Hammer RP, Shrewsbury MM (1977) A reconsideration of the ischiorectal fossa. Diseases of the Colon & Rectum 20 (8):681–689. https://doi.org/10.1007/bf02586690
Abu JI, Bamford WM, Malin G, Brown L, Davies Q, Ireland D (2005) Aggressive angiomyxoma of the perineum. International Journal of Gynecological Cancer 15 (6):1097–1100. https://doi.org/10.1111/j.1525-1438.2005.00182.x
Satheshkumar T, Saklani AP, Banerjee D, Jones DRB (2003) Angiomyofibrosarcoma: A rare ischiorectal fossa swelling. Hospital Medicine 64 (4):244-245
Jeyadevan NN, Sohaib SAA, Thomas JM, Jeyarajah A, Shepherd JH, Fisher C (2003) Imaging Features of Aggressive Angiomyxoma. Clinical Radiology 58 (2):157–162. https://doi.org/10.1053/crad.2002.1127
Kransdorf MJ, Jelinek JS, Moser RP, Jr., Utz JA, Brower AC, Hudson TM, Berrey BH (1989) Soft-tissue masses: diagnosis using MR imaging. AJR American journal of roentgenology 153 (3):541–547. https://doi.org/10.2214/ajr.153.3.541
Surabhi VR, Garg N, Frumovitz M, Bhosale P, Prasad SR, Meis JM (2014) Aggressive angiomyxomas: a comprehensive imaging review with clinical and histopathologic correlation. AJR American journal of roentgenology 202 (6):1171–1178. https://doi.org/10.2214/AJR.13.11668
Hosseinzadeh K, Heller MT, Houshmand G (2012) Imaging of the female perineum in adults. Radiographics 32 (4):E129–E168. https://doi.org/10.1148/rg.324115134
Arneja JS, Gosain AK (2008) Vascular malformations. Plastic and Reconstructive Surgery 121 (4):195E–206E. https://doi.org/10.1097/01.prs.0000304607.29622.3c
Arbelo-Cruz N, Lisanti C, Walker K, Schwope R, Bui-Mansfield LT, Reiter M (2016) Anatomy and Pathology of the Ischiorectal Fossa. Contemporary Diagnostic Radiology 39 (17):1–7. https://doi.org/10.1097/01.CDR.0000490026.20869.7b
Ros PR, Eshaghi N (1991) Plexiform neurofibroma of the pelvis: CT and MRI findings. Magnetic Resonance Imaging 9 (3):463–465. https://doi.org/10.1016/0730-725X(91)90436-P
Jett K, Friedman JM (2010) Clinical and genetic aspects of neurofibromatosis 1. Genetics in Medicine 12 (1):1–11. https://doi.org/10.1097/GIM.0b013e3181bf15e3
Halefoglu AM (2012) Neurofibromatosis type 1 presenting with plexiform neurofibromas in two patients: MRI features. Case Reports in Medicine 2012:1–3. https://doi.org/10.1155/2012/498518
Mazzola CR, Power N, Bilsky MH, Robert R, Guillonneau B (2014) Pudendal schwannoma: A case report and literature review. Can Urol Assoc J 8 (3-4):E199–203. https://doi.org/10.5489/cuaj.1734
Majbar A, Hrora A, Jahid A, Ahallat M, Raiss M (2016) Perineal schwannoma. BMC research notes 9 (1):304. https://doi.org/10.1186/s13104-016-2108-1
Pantè S, Terranova M-L, Leonello G, Fedele F, Ascenti G, Famulari C (2009) Perineal schwannoma. Canadian Journal of Surgery 52 (1):E8–E9
Chen S, Gaynor B, Levi AD (2016) Transischiorectal fossa approach for resection of pudendal nerve schwannoma: case report. J Neurosurg Spine 25 (5):636–639. https://doi.org/10.3171/2016.4.SPINE151449
Munk PL, Lee MJ, Janzen DL, Connell DG, Logan PM, Poon PY, Bainbridge TC (1997) Lipoma and liposarcoma: Evaluation using CT and MR imaging. American Journal of Roentgenology 169 (2):589–594
SScurry J, Van Der Putte SCJ, Pyman J, Chetty N, Szabo R (2009) Mammary-like gland adenoma of the vulva: Review of 46 cases. Pathology 41 (4):372–378. https://doi.org/10.1080/00313020902884493
Filho EFA, de Carvalho AL, de Oliveira Costa PF, de Carvalho AC (2016) Resection of ischiorectal fossa tumors – surgical technique. Journal of Coloproctology 36 (3):179–183. https://doi.org/10.1016/j.jcol.2016.04.006
Chen X, Wu JT (2017) Imaging findings of big hidradenoma papilliferum in ischiorectal fossa: a case report. INTERNATIONAL JOURNAL OF CLINICAL AND EXPERIMENTAL MEDICINE 10 (8):12693–12697
Handa Y, Yamanaka N, Inagaki H, Tomita Y (2003) Large Ulcerated Perianal Hidradenoma Papilliferum in a Young Female. Dermatologic Surgery 29 (7):790–792. https://doi.org/10.1046/j.1524-4725.2003.29201.x
Yap T, Hamzah L, Oshowo A, Taylor I (2003) Myxoid solitary fibrous tumour of the ischiorectal fossa. European Journal of Surgical Oncology 29 (1):98–100. https://doi.org/10.1053/ejso.2002.1400
Levy AD, Manning MA, Miettinen MM (2017) Soft-Tissue Sarcomas of the Abdomen and Pelvis: Radiologic-Pathologic Features, Part 2-Uncommon Sarcomas. Radiographics 37 (3):797–812. https://doi.org/10.1148/rg.2017160201
Chun HJ, Byun JY, Jung SE, Kim KH, Shinn KS (1998) Benign solitary fibrous tumour of the pre-sacral space: MRI findings. British Journal of Radiology 71 (846):677–679. https://doi.org/10.1259/bjr.71.846.9849394
Vossough A, Torigian DA, Zhang PJ, Siegelman ES, Banner MP (2005) Extrathoracic solitary fibrous tumor of the pelvic peritoneum with central malignant degeneration on CT and MRI. Journal of Magnetic Resonance Imaging 22 (5):684–686. https://doi.org/10.1002/jmri.20433
Zhang W-d, Chen J-y, Cao Y, Liu Q-y, Luo R-g (2011) Computed tomography and magnetic resonance imaging findings of solitary fibrous tumors in the pelvis: Correlation with histopathological findings. European Journal of Radiology 78 (1):65–70. https://doi.org/10.1016/j.ejrad.2009.09.001
Shin SS, Jeong YY, Kang HK (2008) Myxoid solitary fibrous tumor of the retroperitoneum: MRI findings with the pathologic correlation. Korean J Radiol 9 (3):279–282. https://doi.org/10.3348/kjr.2008.9.3.279
Menassa-Moussa L, Kanso H, Checrallah A, Abboud J, Ghossain M (2005) CT and MR findings of a retrorectal cystic hamartoma confused with an adnexal mass on ultrasound. European Radiology 15 (2):263–266. https://doi.org/10.1007/s00330-004-2330-4
Yang DM, Park CH, Jin W, Chang SK, Kim JE, Choi SJ, Jung DH (2005) Tailgut Cyst: MRI Evaluation. AJR American journal of roentgenology 184 (5):1519-1523
Sritharan K, Ghani Y, Thompson H (2014) An unusual encounter of an epidermoid cyst. BMJ case reports 2014 (may13 1):bcr2014204186. https://doi.org/10.1136/bcr-2014-204186
Kesici U, Sakman G, Mataraci E (2013) Retrorectal/Presacral epidermoid cyst: report of a case. The Eurasian journal of medicine 45 (3):207–210. https://doi.org/10.5152/eajm.2013.40
Fujimoto H, Murakami K, Kashimada A, Terauchi M, Ozawa K, Nosaka K, Arimizu N (1993) Large epidermal cyst involving the ischiorectal fossa: MR demonstration. Clinical Imaging 17 (2):146-148. https://doi.org/10.1016/0899-7071(93)90056-S
Kransdorf MJ, Jelinek JS, Moser RP, Jr., Utz JA, Brower AC, Hudson TM, Berrey BH (1989) Soft-tissue masses: diagnosis using MR imaging. AJR Am J Roentgenol 153 (3):541–547. https://doi.org/10.2214/ajr.153.3.541
Kim HK, Kim SM, Lee SH, Racadio JM, Shin MJ (2011) Subcutaneous epidermal inclusion cysts: Ultrasound (US) and MR imaging findings. Skeletal Radiology 40 (11):1415–1419. https://doi.org/10.1007/s00256-010-1072-4
Deshmukh SP, Gonsalves CF, Guglielmo FF, Mitchell DG (2012) Role of MR imaging of uterine leiomyomas before and after embolization. Radiographics 32 (6):E251–E281
Casillas J, Joseph RC, Guerra Jr JJ (1990) CT appearance of uterine leiomyomas. Radiographics 10 (6):999–1007
Kim HG, Song YJ, Na YJ, Choi OH (2013) A case of torsion of a subserosal leiomyoma. J Menopausal Med 19 (3):147–150. https://doi.org/10.6118/jmm.2013.19.3.147
Odobasic A, Pasic A, Iljazovic-Latifagic E, Arnautalic L, Odobasic A, Idrizovic E, Dervisefendic M, Dedić L (2010) Perineal endometriosis: a case report and review of the literature. Techniques in Coloproctology 14 (S1):25–27. https://doi.org/10.1007/s10151-010-0642-8
Chene G, Darcha C, Dechelotte P, Mage G, Canis M (2007) Malignant degeneration of perineal endometriosis in episiotomy scar, case report and review of the literature. International Journal of Gynecological Cancer 17 (3):709–714. https://doi.org/10.1111/j.1525-1438.2007.00822.x
Wiley DJ, Douglas J, Beutner K, Cox T, Fife K, Moscicki A-B, Fukumoto L (2002) External Genital Warts: Diagnosis, Treatment, and Prevention. Clinical Infectious Diseases 35 (2):S210–S224. https://doi.org/10.1086/342109
Billingham RP, Isler JT, Kimmins MH, Nelson JM, Schweitzer J, Murphy MM (2004) The diagnosis and management of common anorectal disorders. Current Problems in Surgery 41 (7):586–645. https://doi.org/10.1016/j.cpsurg.2004.04.002
Trombetta LJ, Place RJ (2001) Giant condyloma acuminatum of the anorectum: Trends in epidemiology and management: Report of a case and review of the literature. Diseases of the Colon & Rectum 44 (12):1878–1886. https://doi.org/10.1007/BF02234473
Nelson Montaña C, Labra A, Schiappacasse G (2014) Giant condyloma acuminatum (Buschke-Lowenstein tumor). Series of seven cases and review of the literature. Revista Chilena de Radiología 20 (2):57-63
Singh VA, Gunasagaran J, Pailoor J (2015) Granular cell tumour: malignant or benign? SINGAPORE MEDICAL JOURNAL 56 (9):513–517. https://doi.org/10.11622/smedj.2015136
Nasser H, Ahmed Y, Szpunar SM, Kowalski PJ (2011) Malignant granular cell tumor: a look into the diagnostic criteria. Pathol Res Pract 207 (3):164–168. https://doi.org/10.1016/j.prp.2010.12.007
Fanburg-Smith JC, Meis-Kindblom JM, Fante R, Kindblom LG (1999) Malignant granular cell tumor of soft tissue - Diagnostic criteria and clinicopathologic correlation, (vol 22, pg 779, 1998). AMERICAN JOURNAL OF SURGICAL PATHOLOGY 23 (1):136
Osanai T, Ishikawa A, Ogino T, Yamakawa M (2004) Contrast-enhanced magnetic resonance imaging of malignant granular cell tumor with pathological correlation: a case report. Journal of Orthopaedic Science 9 (5):529–532. https://doi.org/10.1007/s00776-004-0814-3
Bhosale P, Wang J, Varma D, Jensen C, Patnana M, Wei W, Chauhan A, Feig B, Patel S, Somaiah N, Sagebiel T (2016) Can abdominal computed tomography imaging help accurately identify a dedifferentiated component in a well-differentiated liposarcoma? Journal of Computer Assisted Tomography 40 (6):872–879. https://doi.org/10.1097/RCT.0000000000000462
Gupta P, Potti TA, Wuertzer SD, Lenchik L, Pacholke DA (2016) Spectrum of fat-containing soft-tissue masses at MR imaging: The common, the uncommon, the characteristic, and the sometimes confusing. Radiographics 36 (3):753–766. https://doi.org/10.1148/rg.2016150133
Wang TK, Chung MT (1998) Anorectal leiomyosarcomas. Journal of gastroenterology 33 (3):402–407
Mehta N, Konarski A, Rooney P, Chandrasekar C (2015) Leiomyosarcoma of the ischiorectal fossa: report of a novel sphincter and sciatic nerve sparing simultaneous trans-abdominal and trans-gluteal resection and review of the literature. J Surg Case Rep 2015 (3):rjv016–rjv016. https://doi.org/10.1093/jscr/rjv016
Reisner D, Amadi C, Beckman I, Patel S, Surampudi R (2014) Pelvic alveolar rhabdomyosarcoma in a young adult. Radiol Case Rep 9 (4):798. https://doi.org/10.2484/rcr.v9i4.798
Agrons GA, Wagner BJ, Lonergan GJ, Dickey GE, Kaufman MS (1997) From the archives of the AFIP. Genitourinary rhabdomyosarcoma in children: radiologic-pathologic correlation. Radiographics 17 (4):919–937. https://doi.org/10.1148/radiographics.17.4.9225391
Stever MR, Hernandez E, Sakas EL (1988) Malignant fibrous histiocytoma of the pelvis. Gynecologic Oncology 30 (2):285–290. https://doi.org/10.1016/0090-8258(88)90034-0
Mohan RP, Verma S, Siddhu VK, Agarwal N (2013) Malignant fibrous histiocytoma. BMJ Case Rep 2013. https://doi.org/10.1136/bcr-2013-008875
Fletcher CD, Bridge JA, Hogendoorn PC, Mertens F (2013) WHO classification of tumours of soft tissue and bone. IARC Press, Lyon
Hornick JL, Fletcher CDM (2006) PEComa: what do we know so far? Histopathology 48 (1):75–82. https://doi.org/10.1111/j.1365-2559.2005.02316.x
Folpe AL, Mentzel T, Lehr HA, Fisher C, Balzer BL, Weiss SW (2005) Perivascular epithelioid cell neoplasms of soft tissue and gynecologic origin: a clinicopathologic study of 26 cases and review of the literature. Am J Surg Pathol 29 (12):1558–1575
Tirumani SH, Shinagare AB, Hargreaves J, Jagannathan JP, Hornick JL, Wagner AJ, Ramaiya NH (2014) Imaging Features of Primary and Metastatic Malignant Perivascular Epithelioid Cell Tumors. AMERICAN JOURNAL OF ROENTGENOLOGY 202 (2):252–258. https://doi.org/10.2214/AJR.13.10909
Durot C, Dohan A, Boudiaf M, Servois V, Soyer P, Hoeffel C (2017) Cancer of the Anal Canal: Diagnosis, Staging and Follow-Up with MRI. Korean J Radiol 18 (6):946–956. https://doi.org/10.3348/kjr.2017.18.6.946
Granata V, Fusco R, Reginelli A, Roberto L, Granata F, Rega D, Rotondo A, Grassi R, Izzo F, Petrillo A (2016) Radiological assessment of anal cancer: an overview and update. INFECTIOUS AGENTS AND CANCER 11 (1):1–9. https://doi.org/10.1186/s13027-016-0100-y
Roy AC, Wattchow D, Astill D, Singh S, Pendlebury S, Gormly K, Segelov E (2017) Uncommon Anal Neoplasms. SURGICAL ONCOLOGY CLINICS OF NORTH AMERICA 26 (1):143. https://doi.org/10.1016/j.soc.2016.07.009
Scherrer A, Reboul F, Martin D, Dupuy JC, Menu Y (1990) CT of malignant anal canal tumors. Radiographics 10 (3):433–453. https://doi.org/10.1148/radiographics.10.3.2188307
Mahmud A, Poon R, Jonker D (2017) PET imaging in anal canal cancer: a systematic review and meta-analysis. BRITISH JOURNAL OF RADIOLOGY 90 (1080). https://doi.org/10.1259/bjr.20170370
Casali PG, Stacchiotti S, Sangalli C, Olmi P, Gronchi A (2007) Chordoma. Current Opinion in Oncology 19 (4):367–370. https://doi.org/10.1097/CCO.0b013e3281214448
Acknowledgement
We thank Kelly Kage, medical illustrator at MD Anderson Cancer Center for the illustration provided in this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no disclosure or conflict of interests.
Ethical approval
No IRB approval was required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
CME activity
This article has been selected as the CME activity for the current month. Please visit https://ce.mayo.edu/node/82514 and follow the instructions to complete this CME activity.
Rights and permissions
About this article
Cite this article
Faria, S.C., Elsherif, S.B., Sagebiel, T. et al. Ischiorectal fossa: benign and malignant neoplasms of this “ignored” radiological anatomical space. Abdom Radiol 44, 1644–1674 (2019). https://doi.org/10.1007/s00261-019-01930-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-019-01930-7