Abstract
Objective
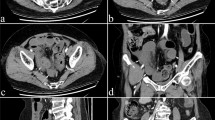
To determine if the attenuation of contrast material in the excluded stomach compared with the gastric pouch is helpful in diagnosing gastrogastric (GG) fistula.
Materials and methods
In a retrospective study, 13 CT scans in 12 patients (age 43.2 ± 9.2, 10 females) who had undergone Roux-en-Y gastric bypass and who had oral contrast in both the gastric pouch and excluded stomach were qualitatively and quantitatively evaluated for GG fistula by two radiologists, using upper GI series (UGI) as the gold standard. Quantitative analysis was performed by computing the relative attenuation (RA) ratio (HU in excluded stomach/HU in gastric pouch). Statistical analysis was performed to determine if the RA ratio values correlated with the UGI findings of GG fistula.
Results
46.2% (6/13) of UGI studies demonstrated a GG fistula. Statistical analysis demonstrated a significant difference in RA ratio (P < 0.05) between the fistula group (1.12 ± 0.29) and the reflux group (0.56 ± 0.19). A receiver operating characteristic analysis identified an RA ratio of 0.8 that maximized sensitivity (100%), at the expense of specificity (78.6%), for diagnosing GG fistula. In contrast, the initial qualitative evaluation for GG fistula yielded a lower sensitivity (45.8%) and a higher specificity (89.2%). After taking RA ratios into account, radiologists’ final conclusions achieved higher sensitivity (58.3%) and specificity (100%).
Conclusion
The relative attenuation ratio of oral contrast in the excluded stomach versus the gastric pouch can be a reliable tool in differentiating GG fistula from oral contrast reflux up the biliopancreatic limb on CT.



Similar content being viewed by others
References
Capella JF, Capella RF (1999) Gastro-gastric fistulas and marginal ulcers in gastric bypass procedures for weight reduction. Obes Surg 9(1):22–27
D’Hondt M, Vansteenkiste F, Van Rooy F, Devriendt D (2006) Gastrogastric fistula after gastric bypass–is surgery always needed? Obes Surg 16(11):1548–1551
Merkle EM, Hallowell PT, Crouse C, Nakamoto DA, Stellato TA (2005) Roux-en-Y gastric bypass for clinically severe obesity: normal appearance and spectrum of complications at imaging 1. Radiology. 234(3):674–683
Sandrasegaran K, Rajesh A, Lall C, et al. (2005) Gastrointestinal complications of bariatric Roux-en-Y gastric bypass surgery. Eur Radiol 15(2):254–262
Varghese JC, Roy-Choudhury SH (2009) Radiological imaging of the GI tract after bariatric surgery. Gastrointest Endosc 70(6):1176–1181
Scheirey CD, Scholz FJ, Shah PC, et al. (2006) Radiology of the laparoscopic Roux-en-Y gastric bypass procedure: conceptualization and precise interpretation of results 1. Radiographics. 26(5):1355–1371
Blachar A, Federle MP, Pealer KM, Ikramuddin S, Schauer PR (2002) Gastrointestinal complications of laparoscopic Roux-en-Y gastric bypass surgery: clinical and imaging findings 1. Radiology. 223(3):625–632
Dresel A, Kuhn JA, McCarty TM (2004) Laparoscopic Roux-en-Y gastric bypass in morbidly obese and super morbidly obese patients. Am J Surg 187(2):230–232
Gould JC, Garren MJ, Starling JR (2004) Lessons learned from the first 100 cases in a new minimally invasive bariatric surgery program. Obes Surg 14(5):618–625
Fleiss JL (1981) Statistical methods for rates and proportions. New York: Wiley, p 218
Stanczyk M, Deveney CW, Traxler SA, McConnell DB, Jobe BA (2006) O’rourke RW. Gastro-gastric fistula in the era of divided Roux-en-Y gastric bypass: strategies for prevention, diagnosis, and management. Obes Surg 16(3):359–364
Carrodeguas L, Szomstein S, Soto F, et al. (2005) Management of gastrogastric fistulas after divided Roux-en-Y gastric bypass surgery for morbid obesity: analysis of 1292 consecutive patients and review of literature. Surg Obes Relat Dis 1(5):467–474
Gustavsson S, Sundbom M (2003) Excellent weight result after Roux-en-Y gastric bypass in spite of gastro-gastric fistula. Obes Surg 13(3):457–459
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Guangzu Gao, M.D., Nariman Nezami, M.D., Mahan Mathur, M.D., Patricia Balcacer, M.D., Gary Israel, M.D., and Michael Spektor, M.D. declares that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Gao, G., Nezami, N., Mathur, M. et al. Diagnosis of gastrogastric fistula on computed tomography: a quantitative approach. Abdom Radiol 43, 1329–1333 (2018). https://doi.org/10.1007/s00261-017-1304-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-017-1304-3