Abstract
Purpose
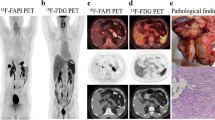
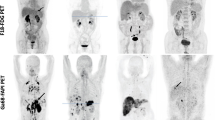
Gallium-68-labeled fibroblast activation protein inhibitor (68Ga-FAPI) is an emerging promising tumor tracer. This study aims to evaluate the diagnostic efficiency of 68Ga-FAPI PET in gastrointestinal cancer, and to determine its potential impact on clinical management.
Methods
Patients with malignancies were prospectively enrolled in a clinical trial to evaluate the diagnostic value of 68Ga-FAPI PET. One hundred twenty patients with gastrointestinal malignancies (121 68Ga-FAPI PET scans) between June 2020 and May 2021 were retrospectively analyzed. Initial staging of untreated patients and restaging of treated patients were evaluated. The treatment scheme promoted by imaging was determined according to NCCN guidelines. Final diagnosis and treatment reference standards were determined by a dedicated multidisciplinary team. The diagnostic performance and treatment guidance of 68Ga-FAPI PET were compared with those of conventional imaging (CI) and 18F-FDG PET.
Results
The diagnostic accuracy of 68Ga-FAPI PET was much higher than that of CI and 18F-FDG PET (95.0% vs. 65.1% and 69.0%, respectively, both p < 0.001). 68Ga-FAPI PET revised diagnosis in 30.3% and 26.2% of patients compared with CI and 18F-FDG PET. The accordance rate of 68Ga-FAPI PET-guided treatment in comparison with the reference standard was significantly higher than that of CI and 18F-FDG PET (96.7% vs. 75.2% and 76.2%, respectively, both p < 0.001). 68Ga-FAPI PET changed treatment in 22.9% and 23.8% of patients compared with CI and 18F-FDG PET.
Conclusions
68Ga-FAPI PET showed remarkable diagnostic performance in gastrointestinal cancer, resulting in more accurate staging and guidance for timely treatment revision, thereby having a critical impact on clinical management.
Trial registration
NCT04554719. Registered September 8, 2020—retrospectively registered, http://clinicaltrails.gov/show/NCT04554719





Similar content being viewed by others
References
Arnold M, Abnet CC, Neale RE, Vignat J, Giovannucci EL, McGlynn KA, et al. Global burden of 5 major types of gastrointestinal cancer. Gastroenterology. 2020;159:335-49.e15. https://doi.org/10.1053/j.gastro.2020.02.068.
Fitzmaurice C, Abate D, Abbasi N, Abbastabar H, Abd-Allah F, Abdel-Rahman O, et al. Global, regional, and national cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life-years for 29 cancer groups, 1990 to 2017: a systematic analysis for the global burden of disease study. JAMA Oncol. 2019;5:1749–68. https://doi.org/10.1001/jamaoncol.2019.2996.
NCCN Clinical Practice Guidelines in Oncology. Colon Cancer Version 4.2020. https://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf. Published June 15, 2020. Accessed November 13, 2020.
NCCN Clinical Practice Guidelines in Oncology. Gastric Cancer Version 3.2020. https://www.nccn.org/professionals/physician_gls/pdf/gastric.pdf. Published August 14, 2020. Accessed November 13, 2020.
Clair K, Tanjasiri S, Bristow R. Does adherence to National Comprehensive Cancer Network (NCCN) practice guidelines improve survival? [abstract]. In: Proceedings of the Twelfth AACR Conference on the Science of Cancer Health Disparities in Racial/Ethnic Minorities and the Medically Underserved; 2019 Sep 20–23; San Francisco, CA. Philadelphia (PA): AACR; Cancer Epidemiol Biomarkers Prev 2020;29(6 Suppl_2):Abstract nr D069.
Boland GM, Chang GJ, Haynes AB, Chiang YJ, Chagpar R, Xing Y, et al. Association between adherence to National Comprehensive Cancer Network treatment guidelines and improved survival in patients with colon cancer. Cancer. 2013;119:1593–601. https://doi.org/10.1002/cncr.27935.
Chagpar R, Xing Y, Chiang YJ, Feig BW, Chang GJ, You YN, et al. Adherence to stage-specific treatment guidelines for patients with colon cancer. J Clin Oncol. 2012;30:972–9. https://doi.org/10.1200/jco.2011.39.6937.
Lee SS, Oh TS, Kim HJ, Chung JW, Park SH, Kim AY, et al. Obscure gastrointestinal bleeding: diagnostic performance of multidetector CT enterography. Radiology. 2011;259:739–48. https://doi.org/10.1148/radiol.11101936.
Karaosmanoglu AD, Onur MR, Arellano RS. Imaging in gastrointestinal cancers. In: Yalcin S., Philip P. (eds) Textbook of Gastrointestinal Oncology. Springer, Cham. 2019: https://doi.org/10.1007/978-3-030-18890-0_25.
Kwee RM, Kwee TC. Modern imaging techniques for preoperative detection of distant metastases in gastric cancer. World J Gastroenterol. 2015;21:10502–9. https://doi.org/10.3748/wjg.v21.i37.10502.
Blake MA, Singh A, Setty BN, Slattery J, Kalra M, Maher MM, et al. Pearls and pitfalls in interpretation of abdominal and pelvic PET-CT. Radiographics. 2006;26:1335–53. https://doi.org/10.1148/rg.265055208.
Hofman MS, Hicks RJ. How we read oncologic FDG PET/CT. Cancer Imaging. 2016;16:35. https://doi.org/10.1186/s40644-016-0091-3.
Alakus H, Batur M, Schmidt M, Drebber U, Baldus SE, Vallböhmer D, et al. Variable 18F-fluorodeoxyglucose uptake in gastric cancer is associated with different levels of GLUT-1 expression. Nucl Med Commun. 2010;31:532–8. https://doi.org/10.1097/MNM.0b013e32833823ac.
Flavell RR, Naeger DM, Aparici CM, Hawkins RA, Pampaloni MH, Behr SC. Malignancies with low fluorodeoxyglucose uptake at PET/CT: pitfalls and prognostic importance: resident and fellow education feature. Radiographics. 2016;36:293–4. https://doi.org/10.1148/rg.2016150073.
Soussan M, Des Guetz G, Barrau V, Aflalo-Hazan V, Pop G, Mehanna Z, et al. Comparison of FDG-PET/CT and MR with diffusion-weighted imaging for assessing peritoneal carcinomatosis from gastrointestinal malignancy. Eur Radiol. 2012;22:1479–87. https://doi.org/10.1007/s00330-012-2397-2.
Wang Z, Chen JQ. Imaging in assessing hepatic and peritoneal metastases of gastric cancer: a systematic review. BMC Gastroenterol. 2011;11:19. https://doi.org/10.1186/1471-230x-11-19.
Watabe T, Liu Y, Kaneda-Nakashima K, Shirakami Y, Lindner T, Ooe K, et al. Theranostics targeting fibroblast activation protein in the tumor stroma: (64)Cu- and (225)Ac-labeled FAPI-04 in pancreatic cancer xenograft mouse models. J Nucl Med. 2020;61:563–9. https://doi.org/10.2967/jnumed.119.233122.
Loktev A, Lindner T, Mier W, Debus J, Altmann A, Jäger D, et al. A tumor-imaging method targeting cancer-associated fibroblasts. J Nucl Med. 2018;59:1423–9. https://doi.org/10.2967/jnumed.118.210435.
Chen H, Pang Y, Wu J, Zhao L, Hao B, Wu J, et al. Comparison of [(68)Ga]Ga-DOTA-FAPI-04 and [(18)F] FDG PET/CT for the diagnosis of primary and metastatic lesions in patients with various types of cancer. Eur J Nucl Med Mol Imaging. 2020;47:1820–32. https://doi.org/10.1007/s00259-020-04769-z.
Kratochwil C, Flechsig P, Lindner T, Abderrahim L, Altmann A, Mier W, et al. (68)Ga-FAPI PET/CT: tracer uptake in 28 different kinds of cancer. J Nucl Med. 2019;60:801–5. https://doi.org/10.2967/jnumed.119.227967.
Giesel FL, Kratochwil C, Lindner T, Marschalek MM, Loktev A, Lehnert W, et al. (68)Ga-FAPI PET/CT: Biodistribution and preliminary dosimetry estimate of 2 DOTA-containing FAP-targeting agents in patients with various cancers. J Nucl Med. 2019;60:386–92. https://doi.org/10.2967/jnumed.118.215913.
Meyer C, Dahlbom M, Lindner T, Vauclin S, Mona C, Slavik R, et al. Radiation dosimetry and biodistribution of (68)Ga-FAPI-46 PET imaging in cancer patients. J Nucl Med. 2020;61:1171–7. https://doi.org/10.2967/jnumed.119.236786.
Pang Y, Zhao L, Luo Z, Hao B, Wu H, Lin Q, et al. Comparison of (68)Ga-FAPI and (18)F-FDG uptake in gastric, duodenal, and colorectal cancers. Radiology. 2021;298:393–402. https://doi.org/10.1148/radiol.2020203275.
Guo W, Chen H. (68)Ga FAPI PET/CT imaging in peritoneal carcinomatosis. Radiology. 2020;297:521. https://doi.org/10.1148/radiol.2020202469.
Guglielmo PGL. Radiolabeled fibroblast activation protein inhibitor (FAPI) PET in oncology: has the time come for 18F-fluorodeoxyglucose to think to a well-deserved retirement? Clinical and Translational Imaging. 2021;9:1–2.
Qin C, Shao F, Gai Y, Liu Q, Ruan W, Liu F, et al. (68)Ga-DOTA-FAPI-04 PET/MR in the evaluation of gastric carcinomas: comparison with (18)F-FDG PET/CT. J Nucl Med. 2021. https://doi.org/10.2967/jnumed.120.258467.
Zhao L, Pang Y, Luo Z, Fu K, Yang T, Zhao L, et al. Role of [(68)Ga]Ga-DOTA-FAPI-04 PET/CT in the evaluation of peritoneal carcinomatosis and comparison with [(18)F]-FDG PET/CT. Eur J Nucl Med Mol Imaging. 2021;48:1944–55. https://doi.org/10.1007/s00259-020-05146-6.
Federle M, Jeffrey RB, Woodward P, Borhani A. Diagnostic imaging—abdomen, 2nd ed, Lippincott Williams Wilkins, Philadelphia, PA (2010), ISBN 978–1–931884–71–6.
Amin MBES, Greene F. AJCC Cancer Staging Manual. 8th ed. New York: Springer; 2017.
Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45:228–47. https://doi.org/10.1016/j.ejca.2008.10.026.
Schwartz LH, Litière S, de Vries E, Ford R, Gwyther S, Mandrekar S, et al. RECIST 1.1-Update and clarification: from the RECIST committee. Eur J Cancer. 2016;62:132–7. https://doi.org/10.1016/j.ejca.2016.03.081.
Wahl RL, Jacene H, Kasamon Y, Lodge MA. From RECIST to PERCIST: evolving considerations for PET response criteria in solid tumors. J Nucl Med. 2009;50(Suppl 1):122s-s150. https://doi.org/10.2967/jnumed.108.057307.
Bentley-Hibbert S, Schwartz L. Use of imaging for GI cancers. J Clin Oncol. 2015;33:1729–36. https://doi.org/10.1200/jco.2014.60.2847.
Koerber SA, Staudinger F, Kratochwil C, Adeberg S, Haefner MF, Ungerechts G, et al. The role of (68)Ga-FAPI PET/CT for patients with malignancies of the lower gastrointestinal tract: first clinical experience. J Nucl Med. 2020;61:1331–6. https://doi.org/10.2967/jnumed.119.237016.
Kobayashi H, Enomoto A, Woods SL, Burt AD, Takahashi M, Worthley DL. Cancer-associated fibroblasts in gastrointestinal cancer. Nat Rev Gastroenterol Hepatol. 2019;16:282–95. https://doi.org/10.1038/s41575-019-0115-0.
Yun M. Imaging of gastric cancer metabolism using 18F-FDG PET/CT. J Gastrointest Cancer. 2014;14:1.
Petersen RK, Hess S, Alavi A, Høilund-Carlsen PF. Clinical impact of FDG-PET/CT on colorectal cancer staging and treatment strategy. Am J Nucl Med Mol Imaging. 2014;4:471–82.
Röhrich M, Naumann P, Giesel FL, Choyke PL, Staudinger F, Wefers A, et al. Impact of (68)Ga-FAPI PET/CT imaging on the therapeutic management of primary and recurrent pancreatic ductal adenocarcinomas. J Nucl Med. 2021;62:779–86. https://doi.org/10.2967/jnumed.120.253062.
Kuten J, Levine C, Shamni O, Pelles S, Wolf I, Lahat G, et al. Head-to-head comparison of [(68)Ga]Ga-FAPI-04 and [(18)F]-FDG PET/CT in evaluating the extent of disease in gastric adenocarcinoma. Eur J Nucl Med Mol Imaging. 2021. https://doi.org/10.1007/s00259-021-05494-x.
Funding
This study was supported in part by the National Natural Science Foundation of China (Grant Nos. 82030052 and 82171985).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethics approval
This article does not contain any experiments with animals. All procedures involving human participants were carried out in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study was approved by the Clinical Research Ethics Committee of Union Hospital, Tongji Medical College, Huazhong University of Science and Technology (No. 20200290).
Consent to participate
Informed consent was obtained from all individual participants included in this study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Oncology—Digestive tract.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Qin, C., Song, Y., Gai, Y. et al. Gallium-68-labeled fibroblast activation protein inhibitor PET in gastrointestinal cancer: insights into diagnosis and management. Eur J Nucl Med Mol Imaging 49, 4228–4240 (2022). https://doi.org/10.1007/s00259-022-05847-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-022-05847-0