Abstract
Background
Isoform 2 of claudin 18 (CLDN18.2) is overexpressed in gastric cancer and may be a promising imaging target. In this study, we constructed three anti-CLDN18.2 antibodies and compared them in preclinical experiments.
Methods
Screening from anti-CLDN18.2 nanobody library, we constructed three antibodies, anti-CLDN18.2 VHH (recombinant single-chain antibody fused with poly-histidine-tag), anti-CLDN18.2 VHH-ABD (recombinant single-chain antibody fused fused with albumin binding domain), and anti-CLDN18.2 VHH-Fc (recombinant single-chain antibody fused with IgG1-Fc) and radiolabeled with 89Zr. Affinity assay, in vitro stability, immunoactivity, blood pharmacokinetics, in vivo and ex vivo biodistribution study, specificity study, and immunohistochemical analysis were performed to assess these radiotracers.
Results
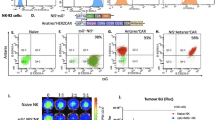
The EC50 were 12.21 nM, 2.48 nM, and 0.14 nM for anti-CLDN18.2 VHH, anti-CLDN18.2 VHH-ABD, and anti-CLDN18.2 VHH-Fc, respectively. 89Zr-anti-CLDN18.2 VHH demonstrated the lowest tumor uptake in PET imaging. Both 89Zr-anti-CLDN18.2 VHH-ABD and 89Zr-anti-CLDN18.2 VHH-Fc demonstrated high tumor accumulation, with highest ID%/g of 25.78 ± 5.60 at 24 h post-injection with 89Zr-anti-CLDN18.2 VHH-ABD and 49.43 ± 9.86 at 72 h post-injection with 89Zr-anti-CLDN18.2 VHH-Fc. The specificity of 89Zr-anti-CLDN18.2 VHH-Fc targeting CLDN18.2 was further confirmed by blocking study. The ex vivo biodistribution results were consistent with in vivo biodistribution data. For 89Zr-anti-CLDN18.2 VHH-ABD, tumor uptake was 21.46 ± 1.78 ID%/g at 12 h and 13.73 ± 2.22 ID%/g at 108 h. For 89Zr-anti-CLDN18.2 VHH-Fc, the tumor accumulation was 25.28 ± 3.83 ID%/g at 12 h and 40.13 ± 9.50 ID%/g at 108 h. Immunohistochemistry of the xenograft tissue revealed high and homogenous CLDN18.2 expression in CO-SNU620 tumor.
Conclusion
Both anti-CLDN18.2 VHH-ABD and anti-CLDN18.2 VHH-Fc can be efficiently and stably radiolabeled with 89Zr for noninvasive imaging and quantification of CLDN18.2 expression in gastric cancer, of which 89Zr-anti-CLDN18.2 VHH-ABD seems to be the optimal choice balancing tumor uptake and liver background. They can provide essential information to select patients who are likely to benefit from CLDN18.2-targeted treatment.




Similar content being viewed by others
Data availability
Not applicable
Code availability
Not applicable
References
Bouché O, Raoul JL, Bonnetain F, Giovannini M, Etienne PL, Lledo G, et al. Randomized multicenter phase II trial of a biweekly regimen of fluorouracil and leucovorin (LV5FU2), LV5FU2 plus cisplatin, or LV5FU2 plus irinotecan in patients with previously untreated metastatic gastric cancer: a Federation Francophone de Cancerologie Digestive Group Study–FFCD 9803. J Clin Oncol. 2004;22:4319–28. https://doi.org/10.1200/jco.2004.01.140.
Pozzo C, Barone C, Szanto J, Padi E, Peschel C, Bükki J, et al. Irinotecan in combination with 5-fluorouracil and folinic acid or with cisplatin in patients with advanced gastric or esophageal-gastric junction adenocarcinoma: results of a randomized phase II study. Ann Oncol. 2004;15:1773–81. https://doi.org/10.1093/annonc/mdh473.
Swisshelm K, Macek R, Kubbies M. Role of claudins in tumorigenesis. Adv Drug Deliv Rev. 2005;57:919–28. https://doi.org/10.1016/j.addr.2005.01.006.
Sahin U, Koslowski M, Dhaene K, Usener D, Brandenburg G, Seitz G, et al. Claudin-18 splice variant 2 is a pan-cancer target suitable for therapeutic antibody development. Clin Cancer Res. 2008;14:7624–34. https://doi.org/10.1158/1078-0432.Ccr-08-1547.
Singh P, Toom S, Huang Y. Anti-claudin 18.2 antibody as new targeted therapy for advanced gastric cancer. J Hematol Oncol. 2017;10:105. https://doi.org/10.1186/s13045-017-0473-4.
Türeci O, Sahin U, Schulze-Bergkamen H, Zvirbule Z, Lordick F, Koeberle D, et al. A multicentre, phase IIa study of zolbetuximab as a single agent in patients with recurrent or refractory advanced adenocarcinoma of the stomach or lower oesophagus: the MONO study. Ann Oncol. 2019;30:1487–95. https://doi.org/10.1093/annonc/mdz199.
Sahin U, Türeci Ö, Manikhas G, Lordick F, Rusyn A, Vynnychenko I, et al. FAST: a randomised phase II study of zolbetuximab (IMAB362) plus EOX versus EOX alone for first-line treatment of advanced CLDN18.2-positive gastric and gastro-oesophageal adenocarcinoma. Ann Oncol. 2021;32:609–19. https://doi.org/10.1016/j.annonc.2021.02.005.
Garin-Chesa P, Old LJ, Rettig WJ. Cell surface glycoprotein of reactive stromal fibroblasts as a potential antibody target in human epithelial cancers. Proc Natl Acad Sci U S A. 1990;87:7235–9. https://doi.org/10.1073/pnas.87.18.7235.
Fan L, Chong X, Zhao M, Jia F, Wang Z, Zhou Y, et al. Ultrasensitive gastric cancer circulating tumor cellular CLDN18.2 RNA detection based on a molecular beacon. Anal Chem. 2021;93:665–70. https://doi.org/10.1021/acs.analchem.0c04055.
Bao C, Gao Q, Li LL, Han L, Zhang B, Ding Y, et al. The Application of Nanobody in CAR-T Therapy. Biomolecules. 2021;11:238. https://doi.org/10.3390/biom11020238.
Flux GD, Guy MJ, Beddows R, Pryor M, Flower MA. Estimation and implications of random errors in whole-body dosimetry for targeted radionuclide therapy. Phys Med Biol. 2002;47:3211–23. https://doi.org/10.1088/0031-9155/47/17/311.
Vincke C, Loris R, Saerens D, Martinez-Rodriguez S, Muyldermans S, Conrath K. General strategy to humanize a camelid single-domain antibody and identification of a universal humanized nanobody scaffold. J Biol Chem. 2009;284:3273–84. https://doi.org/10.1074/jbc.M806889200.
Wei L, Shi J, Afari G, Bhattacharyya S. Preparation of clinical-grade (89) Zr-panitumumab as a positron emission tomography biomarker for evaluating epidermal growth factor receptor-targeted therapy. J Label Compd Radiopharm. 2014;57:25–35. https://doi.org/10.1002/jlcr.3134.
Bang YJ, Van Cutsem E, Feyereislova A, Chung HC, Shen L, Sawaki A, et al. Trastuzumab in combination with chemotherapy versus chemotherapy alone for treatment of HER2-positive advanced gastric or gastro-oesophageal junction cancer (ToGA): a phase 3, open-label, randomised controlled trial. Lancet. 2010;376:687–97. https://doi.org/10.1016/s0140-6736(10)61121-x.
Shitara K, Bang YJ, Iwasa S, Sugimoto N, Ryu MH, Sakai D, et al. Trastuzumab deruxtecan in previously treated HER2-positive gastric cancer. N Engl J Med. 2020;382:2419–30. https://doi.org/10.1056/NEJMoa2004413.
Milenic DE, Garmestani K, Brady ED, Albert PS, Ma D, Abdulla A, et al. Targeting of HER2 antigen for the treatment of disseminated peritoneal disease. Clin Cancer Res. 2004;10:7834–41. https://doi.org/10.1158/1078-0432.Ccr-04-1226.
Ray GL, Baidoo KE, Keller LM, Albert PS, Brechbiel MW, Milenic DE. Pre-clinical assessment of Lu-labeled trastuzumab targeting HER2 for treatment and management of cancer patients with disseminated intraperitoneal disease. Pharmaceuticals (Basel). 2011;5:1–15. https://doi.org/10.3390/ph5010001.
O’Donoghue JA, Lewis JS, Pandit-Taskar N, Fleming SE, Schöder H, Larson SM, et al. Pharmacokinetics, biodistribution, and radiation dosimetry for (89)Zr-trastuzumab in patients with esophagogastric cancer. J Nucl Med. 2018;59:161–6. https://doi.org/10.2967/jnumed.117.194555.
Grabsch H, Sivakumar S, Gray S, Gabbert HE, Müller W. HER2 expression in gastric cancer: rare, heterogeneous and of no prognostic value - conclusions from 924 cases of two independent series. Cell Oncol. 2010;32:57–65. https://doi.org/10.3233/clo-2009-0497.
Rohde C, Yamaguchi R, Mukhina S, Sahin U, Itoh K, Türeci Ö. Comparison of Claudin 18.2 expression in primary tumors and lymph node metastases in Japanese patients with gastric adenocarcinoma. Jpn J Clin Oncol. 2019;49:870–6. https://doi.org/10.1093/jjco/hyz068.
Moran D, Maurus D, Rohde C, Arozullah A. Prevalence of CLDN18. 2, HER2 and PD-L1 in gastric cancer samples. Ann Oncol. 2018;29:viii32.
Dijkers EC, Kosterink JG, Rademaker AP, Perk LR, van Dongen GA, Bart J, et al. Development and characterization of clinical-grade 89Zr-trastuzumab for HER2/neu immunoPET imaging. J Nucl Med. 2009;50:974–81. https://doi.org/10.2967/jnumed.108.060392.
Papp KA, Weinberg MA, Morris A, Reich K. IL17A/F nanobody sonelokimab in patients with plaque psoriasis: a multicentre, randomised, placebo-controlled, phase 2b study. Lancet. 2021;397:1564–75. https://doi.org/10.1016/s0140-6736(21)00440-2.
Warnders FJ, Terwisscha van Scheltinga AGT, Knuehl C, van Roy M, de Vries EFJ, Kosterink JGW, et al. Human epidermal growth factor receptor 3-specific tumor uptake and biodistribution of (89)Zr-MSB0010853 visualized by real-time and noninvasive PET imaging. J Nucl Med. 2017;58:1210–5. https://doi.org/10.2967/jnumed.116.181586.
Tijink B, Laeremans T, Budde M, Stigter-van Walsum M, Dreier T, de Haard H, et al. Improved tumor targeting of anti-epidermal growth factor receptor nanobodies through albumin binding: taking advantage of modular Nanobody technology. Mol Cancer Ther. 2008;7:2288–97. https://doi.org/10.1158/1535-7163.Mct-07-2384.
White JM, Keinänen OM, Cook BE, Zeglis BM, Gibson HM, Viola NT. Removal of Fc glycans from [(89)Zr]Zr-DFO-Anti-CD8 prevents peripheral depletion of CD8(+) T cells. Mol Pharm. 2020;17:2099–108. https://doi.org/10.1021/acs.molpharmaceut.0c00270.
Vivier D, Fung K, Rodriguez C, Adumeau P, Ulaner GA, Lewis JS, et al. The Influence of glycans-specific bioconjugation on the FcγRI binding and in vivo performance of (89)Zr-DFO-pertuzumab. Theranostics. 2020;10:1746–57. https://doi.org/10.7150/thno.39089.
Sun Z, Zheng H, Yu J, Huang W, Li T, Chen H, et al. Liver metastases in newly diagnosed gastric cancer: a population-based study from SEER. J Cancer. 2019;10:2991–3005. https://doi.org/10.7150/jca.30821.
Chomet M, Schreurs M, Vos R, Verlaan M, Kooijman EJ, Poot AJ, et al. Performance of nanoScan PET/CT and PET/MR for quantitative imaging of (18)F and (89)Zr as compared with ex vivo biodistribution in tumor-bearing mice. EJNMMI Res. 2021;11:57. https://doi.org/10.1186/s13550-021-00799-2.
Aerts HJ, Dubois L, Perk L, Vermaelen P, van Dongen GA, Wouters BG, et al. Disparity between in vivo EGFR expression and 89Zr-labeled cetuximab uptake assessed with PET. J Nucl Med. 2009;50:123–31. https://doi.org/10.2967/jnumed.108.054312.
Verel I, Visser G, Boellaard R, Boerman O, van Eerd J, Snow G, et al. Quantitative 89Zr immuno-PET for in vivo scouting of 90Y-labeled monoclonal antibodies in xenograft-bearing nude mice. J Nucl Med: official publication, Society of Nuclear Medicine. 2003;44:1663–70.
Oude Munnink TH, Arjaans ME, Timmer-Bosscha H, Schröder CP, Hesselink JW, Vedelaar SR, et al. PET with the 89Zr-labeled transforming growth factor-β antibody fresolimumab in tumor models. J Nucl Med. 2011;52:2001–8. https://doi.org/10.2967/jnumed.111.092809.
Funding
This work was supported in part by the National Key Research and Development Program of China (No. 2016YFC0901500, 2020YFC2002702),CAMS initiative for Rare Diseases Research Program (No. 2016ZX310174-4), and the National Natural Science Foundation of China (No. 82071967). Antibody drugs were produced and donated by Norry Biotech.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethics approval
All animal studies were performed in accordance with the guidelines of Animal Welfare Office of Peking Union Medical College, all procedures were reviewed and approved by the Institutional Animal Care and Use Committee, and all the animals were maintained under isoflurane anesthesia during the model-building, injection, accumulation, and scanning periods to avoid animal suffering at each stage of the experiment.
Conflict of interest
Wenwen Duan and Peipei Zhou: Employees of Zhejiang Doer Biologics Corporation. All authors declare that no conflicts of interest relevant to this article exist and that the research was conducted in the absence of any commercial or financial relationships that could be constructed as a potential conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Oncology—Digestive tract
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hu, G., Zhu, W., Liu, Y. et al. Development and comparison of three 89Zr-labeled anti-CLDN18.2 antibodies to noninvasively evaluate CLDN18.2 expression in gastric cancer: a preclinical study. Eur J Nucl Med Mol Imaging 49, 2634–2644 (2022). https://doi.org/10.1007/s00259-022-05739-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-022-05739-3