Abstract
Purpose
The objective of this study was to estimate the incidence of secondary cancers and the factors associated with their development among patients who underwent radioiodine therapy (RIT) with differentiated thyroid cancer.
Methods
We retrospectively collected medical records for patients who underwent first RIT between January 1, 2000, and December 31, 2005, from seven tertiary hospitals in South Korea after total thyroidectomy for differentiated thyroid cancer. Cancer incidence and calculated standardized rate ratio were compared with Korean cancer incidence data. The association between the development of secondary cancers and various parameters was analyzed by Cox-proportional hazard regression.
Results
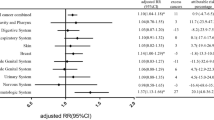
A total of 3106 patients were included in this study. Mean age at the time of diagnosis of thyroid cancer was 45.7 ± 13.3 years old, and 2669 (85.9%) patients were female. The follow-up period was 11.9 ± 4.6 (range, 1.2–19.6) years. A total of 183 secondary cancers, which included 162 solid and 21 hematologic cancers, occurred in 173 patients (5.6%). There was no significant difference between solid cancer incidence in our study population who underwent RIT and the overall Korean population, but the incidence of hematologic cancers and total cancer in our study was significantly higher compared with that of the Korean population. A multivariate analysis identified independent prognostic factors for the development of secondary cancer including age at 1st RIT, male, and total cumulative dose over 200 mCi.
Conclusion
We need to assess the risk benefit for patients who receive over 200 mCi of a total cumulative dose.


Similar content being viewed by others
Data availability
Not applicable
Code availability
Not applicable
References
Jung KW, Won YJ, Kong HJ, Lee ES. Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2016. Cancer Res Treat. 2019;51:417–30. https://doi.org/10.4143/crt.2019.138.
Kilfoy BA, Zheng T, Holford TR, Han X, Ward MH, Sjodin A, et al. International patterns and trends in thyroid cancer incidence, 1973–2002. Cancer Causes Control. 2009;20:525–31. https://doi.org/10.1007/s10552-008-9260-4.
Hong CM, Ahn BC. Factors associated with dose determination of radioactive iodine therapy for differentiated thyroid cancer. Nucl Med Mol Imaging. 2018;52:247–53. https://doi.org/10.1007/s13139-018-0522-0.
Hsu WL, Preston DL, Soda M, Sugiyama H, Funamoto S, Kodama K, et al. The incidence of leukemia, lymphoma and multiple myeloma among atomic bomb survivors: 1950–2001. Radiat Res. 2013;179:361–82. https://doi.org/10.1667/RR2892.1.
Preston DL, Ron E, Tokuoka S, Funamoto S, Nishi N, Soda M, et al. Solid cancer incidence in atomic bomb survivors: 1958–1998. Radiat Res. 2007;168:1–64. https://doi.org/10.1667/RR0763.1.
Kitahara CM, Berrington de Gonzalez A, Bouville A, Brill AB, Doody MM, Melo DR, et al. Association of radioactive iodine treatment with cancer mortality in patients with hyperthyroidism. JAMA Intern Med. 2019. https://doi.org/10.1001/jamainternmed.2019.0981.
Sawka AM, Thabane L, Parlea L, Ibrahim-Zada I, Tsang RW, Brierley JD, et al. Second primary malignancy risk after radioactive iodine treatment for thyroid cancer: a systematic review and meta-analysis. Thyroid. 2009;19:451–7. https://doi.org/10.1089/thy.2008.0392.
Yu CY, Saeed O, Goldberg AS, Farooq S, Fazelzad R, Goldstein DP, et al. A Systematic review and meta-analysis of subsequent malignant neoplasm risk after radioactive iodine treatment of thyroid cancer. Thyroid. 2018;28:1662–73. https://doi.org/10.1089/thy.2018.0244.
Molenaar RJ, Sidana S, Radivoyevitch T, Advani AS, Gerds AT, Carraway HE, et al. Risk of hematologic malignancies after radioiodine treatment of well-differentiated thyroid cancer. J Clin Oncol. 2018;36:1831–9. https://doi.org/10.1200/JCO.2017.75.0232.
Seo GH, Cho YY, Chung JH, Kim SW. Increased risk of leukemia after radioactive iodine therapy in patients with thyroid cancer: a nationwide, population-based study in Korea. Thyroid. 2015;25:927–34. https://doi.org/10.1089/thy.2014.0557.
Tulchinsky M, Binse I, Campenni A, Dizdarevic S, Giovanella L, Jong I, et al. Radioactive iodine therapy for differentiated thyroid cancer: lessons from confronting controversial literature on risks for secondary malignancy. J Nucl Med. 2018;59:723–5. https://doi.org/10.2967/jnumed.118.211359.
Haugen BR, Alexander EK, Bible KC, Doherty GM, Mandel SJ, Nikiforov YE, et al. 2015 American Thyroid Association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: the American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid. 2016;26:1–133. https://doi.org/10.1089/thy.2015.0020.
Tuttle RM, Leboeuf R, Robbins RJ, Qualey R, Pentlow K, Larson SM, et al. Empiric radioactive iodine dosing regimens frequently exceed maximum tolerated activity levels in elderly patients with thyroid cancer. J Nucl Med. 2006;47:1587–91.
Radivoyevitch T, Sachs RK, Gale RP, Molenaar RJ, Brenner DJ, Hill BT, et al. Defining AML and MDS second cancer risk dynamics after diagnoses of first cancers treated or not with radiation. Leukemia. 2016;30:285–94. https://doi.org/10.1038/leu.2015.258.
Menzel C, Grunwald F, Schomburg A, Palmedo H, Bender H, Spath G, et al. “High-dose” radioiodine therapy in advanced differentiated thyroid carcinoma. J Nucl Med. 1996;37:1496–503.
Beierwaltes WH. The treatment of thyroid carcinoma with radioactive iodine. Semin Nucl Med. 1978;8:79–94. https://doi.org/10.1016/s0001-2998(78)80009-9.
Maxon HR, Thomas SR, Hertzberg VS, Kereiakes JG, Chen IW, Sperling MI, et al. Relation between effective radiation dose and outcome of radioiodine therapy for thyroid cancer. N Engl J Med. 1983;309:937–41. https://doi.org/10.1056/NEJM198310203091601.
Segi M, Kyokai NT, Igakubu ThD. Cancer mortality for selected sites in 24 countries. 1950.
Boyle P, Parkin DM. Cancer registration: principles and methods. Statistical methods for registries. IARC Sci Publ. 1991;126-58.
Seo GH, Ae Kong K, Kim BS, Seo YK, Moon BS, Yoon HJ, et al. Radioactive iodine treatment for children and young adults with thyroid cancer in South Korea: a population-based study. J Clin Endocrinol Metab. 2021. https://doi.org/10.1210/clinem/dgab192.
Molenaar RJ, Pleyer C, Radivoyevitch T, Sidana S, Godley A, Advani AS, et al. Risk of developing chronic myeloid neoplasms in well-differentiated thyroid cancer patients treated with radioactive iodine. Leukemia. 2018;32:952–9. https://doi.org/10.1038/leu.2017.323.
Silva-Vieira M, Carrilho Vaz S, Esteves S, Ferreira TC, Limbert E, Salgado L, et al. Second primary cancer in patients with differentiated thyroid cancer: does radioiodine play a role? Thyroid. 2017;27:1068–76. https://doi.org/10.1089/thy.2016.0655.
Ko KY, Kao CH, Lin CL, Huang WS, Yen RF. (131)I treatment for thyroid cancer and the risk of developing salivary and lacrimal gland dysfunction and a second primary malignancy: a nationwide population-based cohort study. Eur J Nucl Med Mol Imaging. 2015;42:1172–8. https://doi.org/10.1007/s00259-015-3055-0.
American Thyroid Association Guidelines Taskforce on Thyroid Nodules and Differentiated Thyroid Cancer, Cooper DS, Doherty GM, Haugen BR, Kloos RT, et al. Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid. 2009;19:1167–214. https://doi.org/10.1089/thy.2009.0110.
Singer PA, Cooper DS, Daniels GH, Ladenson PW, Greenspan FS, Levy EG, et al. Treatment guidelines for patients with thyroid nodules and well-differentiated thyroid cancer. American Thyroid Association. Arch Intern Med. 1996;156:2165–72.
Durante C, Haddy N, Baudin E, Leboulleux S, Hartl D, Travagli JP, et al. Long-term outcome of 444 patients with distant metastases from papillary and follicular thyroid carcinoma: benefits and limits of radioiodine therapy. J Clin Endocrinol Metab. 2006;91:2892–9. https://doi.org/10.1210/jc.2005-2838.
Ahn HS, Kim HJ, Kim KH, Lee YS, Han SJ, Kim Y, et al. Thyroid cancer screening in South Korea increases detection of papillary cancers with no impact on other subtypes or thyroid cancer mortality. Thyroid. 2016;26:1535–40. https://doi.org/10.1089/thy.2016.0075.
National Health Insurance Service. Statistical information report of health screening statistics. 2021.
Chan HP, Liu WS, Liou WS, Hu C, Chiu YL, Peng NJ. Comparison of FDG-PET/CT for cancer detection in populations with different risks of underlying malignancy. In Vivo. 2020;34:469–78. https://doi.org/10.21873/invivo.11797.
Tong J, Zou Y, Jiang J, Shi W, Tao R, Ye J, et al. Cancer screening of asymptomatic individuals using 18F-FDG PET/CT in China: a retrospective study. Discov Med. 2016;22:181–8.
Funding
This work was supported by the Korean Thyroid Association Clinical Research Award 2019.
Author information
Authors and Affiliations
Contributions
C.M.H. and J.L. performed the study design, and J.L contributed for funding resources. C.M.H., J-Y.S., S.Y.J., and S-W.L. performed the data analysis. J-Y.S. contributed statistical assistance and review. C.M.H. and J.L. wrote the initial draft, and B.I.K., H-C.S., J-K.Y., K.S.W., S-M.K., and I.H.C. contributed for data collection and review of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
The Institutional Review board approved this study.
Consent to participate
Informed consent was waived by the Institutional Review Board.
Consent for publication
Patients signed an informed consent which was waived by Institutional Review Board.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Oncology - Head and Neck
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Hong, C.M., Shin, JY., Kim, B.I. et al. Incidence rate and factors associated with the development of secondary cancers after radioiodine therapy in differentiated thyroid cancer: a multicenter retrospective study. Eur J Nucl Med Mol Imaging 49, 1661–1670 (2022). https://doi.org/10.1007/s00259-021-05608-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-021-05608-5