Abstract
Purpose
Hyperparathyroidism (HPT) is a common endocrine disorder caused by hyperfunctioning parathyroid glands (HP). The correct detection and localization of HP is challenging but crucial, as it may guide surgical treatment, particularly in patients with primary HPT. There is a growing body of data regarding the role of radiolabelled choline positron emission tomography (PET) in this setting. Therefore, we performed a systematic review and meta-analysis of the diagnostic performance of this method in detecting HP in patients with HPT.
Methods
This systematic review and meta-analysis was carried out according to PRISMA guidelines. A comprehensive computer literature search of PubMed/MEDLINE, EMBASE and Cochrane Library databases for studies published through May 2018 was performed using the following search algorithm: (a) “choline” or “fluorocholine” or “F-choline” or “C-choline” or “FCH” or “CH” or “FECH” or “FMCH” and (b) “PET” or “positron emission tomography” and (c) “parathyroid” or “hyperparathyroidism”. The diagnostic performance of radiolabelled choline PET was expressed as sensitivity and positive predictive value (PPV) on a per-patient and per-lesion basis and as detection rate (DR) on a per-patient basis, with pooled proportion and 95% confidence interval (95% CI) obtained using a random-effects model.
Results
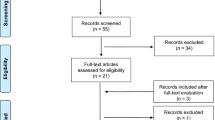
Eighteen studies were included in the systematic review. Fourteen articles (517 patients) were selected for the meta-analysis. The meta-analysis provided the following results on a per-patient analysis analysis: sensitivity 95% (95% CI: 92–97%), PPV 97% (95% CI: 95–98%) and DR 91% (95% CI: 87–94%). On a per-lesion analysis, pooled sensitivity and PPV were 92% (95% CI: 88–96) and 92% (95% CI: 89–95%), respectively. No significant heterogeneity was found among the selected studies.
Conclusions
Radiolabelled choline PET demonstrated excellent diagnostic performance in detecting HP in patients with HPT. Large multicentre studies and cost-effectiveness analyses are needed to better define the role of this imaging method in this setting.




Similar content being viewed by others
References
Bilezikian JP, Bandeira L, Khan A, Cusano NE. Hyperparathyroidism. Lancet. 2018;391(10116):168–78.
Walker MD, Silverberg SJ. Primary hyperparathyroidism. Nat Rev Endocrinol. 2018;14(2):115–25.
Portillo MR, Rodríguez-Ortiz ME. Secondary hyperparthyroidism: pathogenesis, diagnosis, preventive and therapeutic strategies. Rev Endocr Metab Disord. 2017;18(1):79–95.
Cocchiara G, Fazzotta S, Palumbo VD, Damiano G, Cajozzo M, Maione C, et al. The medical and surgical treatment in secondary and tertiary hyperparathyroidism. Review. Clin Ter. 2017;168(2):e158–67.
Udelsman R, Åkerström G, Biagini C, Duh QY, Miccoli P, Niederle B, et al. The surgical management of asymptomatic primary hyperparathyroidism: proceedings of the fourth international workshop. J Clin Endocrinol Metab. 2014;99:3595–606.
Stephen AE, Mannstadt M, Hodin RA. Indications for surgical management of hyperparathyroidism: a review. JAMA Surg. 2017;152(9):878–82.
Treglia G, Trimboli P, Huellner M, Giovanella L. Imaging in primary hyperparathyroidism: focus on the evidence-based diagnostic performance of different methods. Minerva Endocrinol. 2018;43(2):133–43.
Liddy S, Worsley D, Torreggiani W, Feeney J. Preoperative imaging in primary hyperparathyroidism: literature review and recommendations. Can Assoc Radiol J. 2017;68(1):47–55.
Kuzminski SJ, Sosa JA, Hoang JK. Update in parathyroid imaging. Magn Reson Imaging Clin N Am. 2018;26(1):151–66.
Kluijfhout WP, Pasternak JD, Drake FT, Beninato T, Gosnell JE, Shen WT, et al. Use of PET tracers for parathyroid localization: a systematic review and meta-analysis. Langenbeck’s Arch Surg. 2016;401(7):925–35.
Caldarella C, Treglia G, Isgrò MA, Giordano A. Diagnostic performance of positron emission tomography using 11C-methionine in patients with suspected parathyroid adenoma: a meta-analysis. Endocrine. 2013;43(1):78–83.
Imperiale A, Taïeb D, Hindié E. (18)F-Fluorocholine PET/CT as a second line nuclear imaging technique before surgery for primary hyperparathyroidism. Eur J Nucl Med Mol Imaging. 2018;45(4):654–7.
Prior JO. New scintigraphic methods for parathyroid imaging. Ann Endocrinol. 2015;76(2):145–7.
Treglia G, Giovannini E, Di Franco D, Calcagni ML, Rufini V, Picchio M, et al. The role of positron emission tomography using carbon-11 and fluorine-18 choline in tumors other than prostate cancer: a systematic review. Ann Nucl Med. 2012;26(6):451–61.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol. 2009;62:e1–34.
Sadeghi R, Treglia G. Systematic reviews and meta-analyses of diagnostic studies: a practical guideline. Clin Transl Imaging. 2017;5:83–7.
Whiting PF, Rutjes AW, Westwood ME, Mallett S, Deeks JJ, Reitsma JB, et al. Bossuyt PM; QUADAS-2 group. QUADAS-2: a revised tool for the quality assessment of diagnostic accuracy studies. Ann Intern Med. 2011;155(8):529–36.
Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21(11):1539–58.
Harbord RM, Egger M, Sterne JA. A modified test for small-study effects in meta-analyses of controlled trials with binary endpoints. Stat Med. 2006;25(20):3443–57.
Morland D, Richard C, Godard F, Deguelte S, Delemer B. Temporal uptake patterns of 18F-Fluorocholine among hyperfunctioning parathyroid glands. Clin Nucl Med. 2018;43(7):504–5.
Alharbi AA, Alshehri FM, Albatly AA, Sah BR, Schmid C, Huber GF, et al. [(18)F]Fluorocholine uptake of parathyroid adenoma is correlated with parathyroid hormone level. Mol Imaging Biol. 2018; https://doi.org/10.1007/s11307-018-1179-x.
Grimaldi S, Young J, Kamenicky P, Hartl D, Terroir M, Leboulleux S, et al. Challenging pre-surgical localization of hyperfunctioning parathyroid glands in primary hyperparathyroidism: the added value of (18)F-Fluorocholine PET/CT. Eur J Nucl Med Mol Imaging. 2018; https://doi.org/10.1007/s00259-018-4018-z.
Beheshti M, Hehenwarter L, Paymani Z, Rendl G, Imamovic L, Rettenbacher R, et al. (18)F-Fluorocholine PET/CT in the assessment of primary hyperparathyroidism compared with (99m)Tc-MIBI or (99m)Tc-tetrofosmin SPECT/CT: a prospective dual-centre study in 100 patients. Eur J Nucl Med Mol Imaging. 2018; https://doi.org/10.1007/s00259-018-3980-9.
Fischli S, Suter-Widmer I, Nguyen BT, Müller W, Metzger J, Strobel K, et al. The significance of 18F-Fluorocholine-PET/CT as localizing imaging technique in patients with primary hyperparathyroidism and negative conventional imaging. Front Endocrinol. 2018;8:380. https://doi.org/10.3389/fendo.2017.00380.
Huber GF, Hüllner M, Schmid C, Brunner A, Sah B, Vetter D, et al. Benefit of (18)F-fluorocholine PET imaging in parathyroid surgery. Eur Radiol. 2018;28(6):2700–7.
Parvinian A, Martin-Macintosh EL, Goenka AH, Durski JM, Mullan BP, Kemp BJ, et al. (11)C-choline PET/CT for detection and localization of parathyroid adenomas. AJR Am J Roentgenol. 2018;210(2):418–22.
Quak E, Blanchard D, Houdu B, Le Roux Y, Ciappuccini R, Lireux B, et al. F18-choline PET/CT guided surgery in primary hyperparathyroidism when ultrasound and MIBI SPECT/CT are negative or inconclusive: the APACH1 study. Eur J Nucl Med Mol Imaging. 2018;45(4):658–66.
Rep S, Hocevar M, Vaupotic J, Zdesar U, Zaletel K, Lezaic L. (18)F-choline PET/CT for parathyroid scintigraphy: significantly lower radiation exposure of patients in comparison to conventional nuclear medicine imaging approaches. J Radiol Prot. 2018;38(1):343–56.
Hocevar M, Lezaic L, Rep S, Zaletel K, Kocjan T, Sever MJ, et al. Focused parathyroidectomy without intraoperative parathormone testing is safe after pre-operative localization with (18)F-Fluorocholine PET/CT. Eur J Surg Oncol. 2017;43(1):133–7.
Kluijfhout WP, Pasternak JD, Gosnell JE, Shen WT, Duh QY, Vriens MR, et al. (18)F Fluorocholine PET/MR imaging in patients with primary hyperparathyroidism and inconclusive conventional imaging: a prospective pilot study. Radiology. 2017;284(2):460–7.
Taywade SK, Damle NA, Behera A, Devasenathipathy K, Bal C, Tripathi M, et al. Comparison of 18F-Fluorocholine positron emission tomography/computed tomography and four-dimensional computed tomography in the preoperative localization of parathyroid adenomas-initial results. Indian J Endocrinol Metab. 2017;21(3):399–403.
Thanseer N, Bhadada SK, Sood A, Mittal BR, Behera A, Gorla AKR, et al. Comparative effectiveness of ultrasonography, 99mTc-Sestamibi, and 18F-Fluorocholine PET/CT in detecting parathyroid adenomas in patients with primary hyperparathyroidism. Clin Nucl Med. 2017;42(12):e491–7.
Kluijfhout WP, Vorselaars WM, van den Berk SA, Vriens MR, Borel Rinkes IH, Valk GD, et al. Fluorine-18 fluorocholine PET-CT localizes hyperparathyroidism in patients with inconclusive conventional imaging: a multicenter study from the Netherlands. Nucl Med Commun. 2016;37(12):1246–52.
Kluijfhout WP, Vorselaars WM, Vriens MR, Borel Rinkes IH, Valk GD, de Keizer B. Enabling minimal invasive parathyroidectomy for patients with primary hyperparathyroidism using Tc-99m-sestamibi SPECT-CT, ultrasound and first results of (18)F-fluorocholine PET-CT. Eur J Radiol. 2015;84(9):1745–51.
Michaud L, Balogova S, Burgess A, Ohnona J, Huchet V, Kerrou K, et al. A pilot comparison of 18F-fluorocholine PET/CT, ultrasonography and 123I/99mTc-sestaMIBI dual-phase dual-isotope scintigraphy in the preoperative localization of Hyperfunctioning parathyroid glands in primary or secondary hyperparathyroidism: influence of thyroid anomalies. Medicine (Baltimore). 2015;94(41):e1701.
Rep S, Lezaic L, Kocjan T, Pfeifer M, Sever MJ, Simoncic U, et al. Optimal scan time for evaluation of parathyroid adenoma with [(18)F]-fluorocholine PET/CT. Radiol Oncol. 2015;49(4):327–33.
Lezaic L, Rep S, Sever MJ, Kocjan T, Hocevar M, Fettich J. 18F-Fluorocholine PET/CT for localization of hyperfunctioning parathyroid tissue in primary hyperparathyroidism: a pilot study. Eur J Nucl Med Mol Imaging. 2014;41(11):2083–9.
Michaud L, Burgess A, Huchet V, Lefèvre M, Tassart M, Ohnona J, et al. Is 18F-fluorocholine-positron emission tomography/computerized tomography a new imaging tool for detecting hyperfunctioning parathyroid glands in primary or secondary hyperparathyroidism? J Clin Endocrinol Metab. 2014;99(12):4531–6.
Orevi M, Freedman N, Mishani E, Bocher M, Jacobson O, Krausz Y. Localization of parathyroid adenoma by 11C-choline PET/CT: preliminary results. Clin Nucl Med. 2014;39(12):1033–8.
Treglia G, Sadeghi R, Schalin-Jäntti C, Caldarella C, Ceriani L, Giovanella L, et al. Detection rate of (99m) Tc-MIBI single photon emission computed tomography (SPECT)/CT in preoperative planning for patients with primary hyperparathyroidism: a meta-analysis. Head Neck. 2016;38(Suppl 1):E2159–72.
Kluijfhout WP, Pasternak JD, Beninato T, Drake FT, Gosnell JE, Shen WT, et al. Diagnostic performance of computed tomography for parathyroid adenoma localization; a systematic review and meta-analysis. Eur J Radiol. 2017;88:117–28.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no financial or non-financial competing interests.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Treglia, G., Piccardo, A., Imperiale, A. et al. Diagnostic performance of choline PET for detection of hyperfunctioning parathyroid glands in hyperparathyroidism: a systematic review and meta-analysis. Eur J Nucl Med Mol Imaging 46, 751–765 (2019). https://doi.org/10.1007/s00259-018-4123-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-018-4123-z