Abstract
Purpose
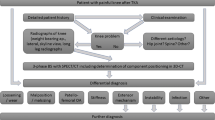
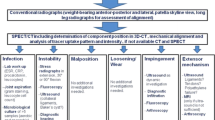
Bone single photon emission computed tomography (SPECT)/CT is considered as beneficial in unhappy patients with pain, stiffness or swelling after total knee arthroplasty (TKA). The purpose of this study was to identify typical patterns of bone tracer uptake (BTU), distribution and intensity values in patients after TKA. The above findings were correlated with the type and fixation of TKA, the time from TKA and intraoperative findings at revision surgery.
Methods
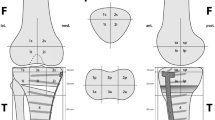
A total of 100 knees of 84 consecutive patients (mean age ± SD 70 ± 11 years) after TKA with persistent knee pain were prospectively included. All patients underwent clinical examination, standardized radiographs and 99mTc-hydroxymethane diphosphonate (HDP) SPECT/CT as part of a routine diagnostic algorithm. The diagnosis before and after SPECT/CT and final treatment were recorded. TKA component position was determined on 3-D reconstructed images. Intensity and anatomical distribution of BTU was determined. Maximum intensity values were recorded as well as ratios in relation to the proximal midshaft of the femur. Univariate analyses (chi-square test, Pearson’s correlation and t test for independent samples) were performed (p < 0.05).
Results
SPECT/CT changed the clinical diagnosis and final treatment in 85/100 (85 %) knees. Intraoperative findings confirmed the preoperative SPECT/CT diagnosis in 32/33 knees (97 %). TKA loosening as well as progression of patellofemoral osteoarthritis (OA) was correctly diagnosed in 100 % of knees. Typical patterns of BTU for specific pathologies were identified. Loose femoral TKA components significantly correlated with increased BTU at the lateral femoral regions (p < 0.05). Loose tibial TKA components significantly correlated with increased BTU at all tibial regions (p < 0.05) and around the tibial peg (p > 0.01).
Conclusion
The diagnostic benefits of SPECT/CT in patients after TKA have been proven. Typical pathology-related BTU patterns were identified, which will improve reporting quality. Due to the benefits in establishing the correct diagnosis, SPECT/CT should be part of the routine diagnostic algorithm for patients with pain after TKA.






Similar content being viewed by others
References
Mannion AF, Kämpfen S, Munzinger U, Kramers-de Quervain I. The role of patient expectations in predicting outcome after total knee arthroplasty. Arthritis Res Ther 2009;11(5):R139. doi:10.1186/ar2811.
Hirschmann MT, Konala P, Iranpour F, Kerner A, Rasch H, Friederich NF. Clinical value of SPECT/CT for evaluation of patients with painful knees after total knee arthroplasty–a new dimension of diagnostics? BMC Musculoskelet Disord 2011;12:36. doi:10.1186/1471-2474-12-36.
Rasch H, Falkowski AL, Forrer F, Henckel J, Hirschmann MT. 4D-SPECT/CT in orthopaedics: a new method of combined quantitative volumetric 3D analysis of SPECT/CT tracer uptake and component position measurements in patients after total knee arthroplasty. Skeletal Radiol 2013;42(9):1215–23. doi:10.1007/s00256-013-1643-2.
Hirschmann MT, Testa E, Amsler F, Friederich NF. The unhappy total knee arthroplasty (TKA) patient: higher WOMAC and lower KSS in depressed patients prior and after TKA. Knee Surg Sports Traumatol Arthrosc 2013;21(10):2405–11. doi:10.1007/s00167-013-2409-z.
Hirschmann MT, Henckel J, Rasch H. SPECT/CT in patients with painful knee arthroplasty-what is the evidence? Skeletal Radiol 2013;42(9):1201–7. doi:10.1007/s00256-013-1657-9.
Hirschmann MT, Wagner CR, Rasch H, Henckel J. Standardized volumetric 3D-analysis of SPECT/CT imaging in orthopaedics: overcoming the limitations of qualitative 2D analysis. BMC Med Imaging 2012;12:5. doi:10.1186/1471-2342-12-5.
Schön SN, Afifi FK, Rasch H, Amsler F, Friederich NF, Arnold MP, et al. Assessment of in vivo loading history of the patellofemoral joint: a study combining patellar position, tilt, alignment and bone SPECT/CT. Knee Surg Sports Traumatol Arthrosc 2014;22(12):3039–46. doi:10.1007/s00167-013-2698-2.
Mucha A, Dordevic M, Testa EA, Rasch H, Hirschmann MT. Assessment of the loading history of patients after high tibial osteotomy using SPECT/CT—a new diagnostic tool and algorithm. J Orthop Surg Res 2013;8(1):46. doi:10.1186/1749-799X-8-46.
Hirschmann MT, Schön S, Afifi FK, Amsler F, Rasch H, Friederich NF, et al. Assessment of loading history of compartments in the knee using bone SPECT/CT: a study combining alignment and 99mTc-HDP tracer uptake/distribution patterns. J Orthop Res 2013;31(2):268–74. doi:10.1002/jor.22206.
Henderson IJ, Tuy B, Connell D, Oakes B, Hettwer WH. Prospective clinical study of autologous chondrocyte implantation and correlation with MRI at three and 12 months. J Bone Joint Surg Br 2003;85(7):1060–6.
Ryd L, Gustafson T, Lindstrand A. 99mTc-diphosphonate scintigraphy in successful knee arthroplasty and its relation to micromotion. Clin Orthop Relat Res 1993;287:61–7.
Klett R, Steiner D, Laurich S, Bauer R, Kordelle J. Evaluation of aseptic loosening of knee prostheses by quantitative bone scintigraphy. Nuklearmedizin 2008;47(4):163–6.
Sacchetti GM, Ghisellini F, Brambilla M, De Consoli A, Fornara P, Rizzo E, et al. Quantitative scintigraphic evaluation of total knee arthroplasties: a feasibility study. Clin Orthop Relat Res 1996;325:181–9.
Saari T, Uvehammer J, Carlsson LV, Regnér L, Kärrholm J. Posterior stabilized component increased femoral bone loss after total knee replacement. 5-year follow-up of 47 knees using dual energy X-ray absorptiometry. Knee 2006;13(6):435–9. doi:10.1016/j.knee.2006.08.002.
Soininvaara T, Nikola T, Vanninen E, Miettinen H, Kröger H. Bone mineral density and single photon emission computed tomography changes after total knee arthroplasty: a 2-year follow-up study. Clin Physiol Funct Imaging 2008;28(2):101–6. doi:10.1111/j.1475-097X.2007.00782.x.
Windisch C, Windisch B, Kolb W, Kolb K, Grützner P, Roth A. Osteodensitometry measurements of periprosthetic bone using dual energy X-ray absorptiometry following total knee arthroplasty. Arch Orthop Trauma Surg 2012;132(11):1595–601. doi:10.1007/s00402-012-1601-9.
Minoda Y, Ikebuchi M, Kobayashi A, Iwaki H, Inori F, Nakamura H. A cemented mobile-bearing total knee replacement prevents periprosthetic loss of bone mineral density around the femoral component: a matched cohort study. J Bone Joint Surg Br 2010;92(6):794–8. doi:10.1302/0301-620X.92B6.23159.
Toegel S, Hoffmann O, Wadsak W, Ettlinger D, Mien LK, Wiesner K, et al. Uptake of bone-seekers is solely associated with mineralisation! A study with 99mTc-MDP, 153Sm-EDTMP and 18F-fluoride on osteoblasts. Eur J Nucl Med Mol Imaging 2006;33(4):491–4. doi:10.1007/s00259-005-0026-x.
Li MG, Nilsson KG. No relationship between postoperative changes in bone density at the proximal tibia and the migration of the tibial component 2 years after total knee arthroplasty. J Arthroplasty 2001;16(7):893–900. doi:10.1054/arth.2001.24376.
Hirschmann MT, Davda K, Iranpour F, Rasch H, Friederich NF. Combined single photon emission computerised tomography and conventional computerised tomography (SPECT/CT) in patellofemoral disorders: a clinical review. Int Orthop 2011;35(5):675–80. doi:10.1007/s00264-010-1049-x.
Hirschmann MT, Konala P, Iranpour F, Kerner A, Rasch H, Friederich NF. Clinical value of SPECT/CT for assessment of patients with painful knees after total knee arthroplasty—a new dimension of diagnostics? BMC Musculoskelet Disord 2011;12:36.
Ahmad R, Kumar GS, Katam K, Dunlop D, Pozo JL. Significance of a “hot patella” in total knee replacement without primary patellar resurfacing. Knee 2009;16(5):337–40. doi:10.1016/j.knee.2009.02.001.
Hirschmann MT, Konala P, Amsler F, Iranpour F, Friederich NF, Cobb JP. The position and orientation of total knee replacement components: a comparison of conventional radiographs, transverse 2D-CT slices and 3D-CT reconstruction. J Bone Joint Surg Br 2011;93(5):629–33. doi:10.1302/0301-620X.93B5.25893.
Hirschmann MT, Iranpour F, Konala P, Kerner A, Rasch H, Cobb JP, et al. A novel standardized algorithm for evaluating patients with painful total knee arthroplasty using combined single photon emission tomography and conventional computerized tomography. Knee Surg Sports Traumatol Arthrosc 2010;18(7):939–44. doi:10.1007/s00167-010-1070-z.
Srivastava A, Lee GY, Steklov N, Colwell Jr CW, Ezzet KA, D’Lima DD. Effect of tibial component varus on wear in total knee arthroplasty. Knee 2012;19(5):560–3. doi:10.1016/j.knee.2011.11.003.
Matsuda S, Whiteside LA, White SE. The effect of varus tilt on contact stresses in total knee arthroplasty: a biomechanical study. Orthopedics 1999;22(3):303–7.
Green GV, Berend KR, Berend ME, Glisson RR, Vail TP. The effects of varus tibial alignment on proximal tibial surface strain in total knee arthroplasty: the posteromedial hot spot. J Arthroplasty 2002;17(8):1033–9. doi:10.1054/arth.2002.35796.
Werner FW, Ayers DC, Maletsky LP, Rullkoetter PJ. The effect of valgus/varus malalignment on load distribution in total knee replacements. J Biomech 2005;38(2):349–55. doi:10.1016/j.jbiomech.2004.02.024.
Perillo-Marcone A, Taylor M. Effect of varus/valgus malalignment on bone strains in the proximal tibia after TKR: an explicit finite element study. J Biomech Eng 2007;129(1):1–11. doi:10.1115/1.2401177.
Hofmann S, Romero J, Roth-Schiffl E, Albrecht T. Rotational malalignment of the components may cause chronic pain or early failure in total knee arthroplasty. Orthopade 2003;32(6):469–76. doi:10.1007/s00132-003-0503-5.
Fehring TK. Rotational malalignment of the femoral component in total knee arthroplasty. Clin Orthop Relat Res 2000;380:72–9.
Kuriyama S, Ishikawa M, Furu M, Ito H, Matsuda S. Malrotated tibial component increases medial collateral ligament tension in total knee arthroplasty. J Orthop Res 2014;32(12):1658–66. doi:10.1002/jor.22711.
Kessler O, Lacatusu E, Sommers MB, Mayr E, Bottlang M. Malrotation in total knee arthroplasty: effect on tibial cortex strain captured by laser-based strain acquisition. Clin Biomech (Bristol, Avon) 2006;21(6):603–9. doi:10.1016/j.clinbiomech.2006.01.011.
Petersen MM, Olsen C, Lauritzen JB, Lund B. Changes in bone mineral density of the distal femur following uncemented total knee arthroplasty. J Arthroplasty 1995;10(1):7–11.
Petersen MM, Nielsen PT, Lebech A, Toksvig-Larsen S, Lund B. Preoperative bone mineral density of the proximal tibia and migration of the tibial component after uncemented total knee arthroplasty. J Arthroplasty 1999;14(1):77–81.
van Loon CJ, Oyen WJ, de Waal Malefijt MC, Verdonschot N. Distal femoral bone mineral density after total knee arthroplasty: a comparison with general bone mineral density. Arch Orthop Trauma Surg 2001;121(5):282–5.
Li MG, Nilsson KG. Changes in bone mineral density at the proximal tibia after total knee arthroplasty: a 2-year follow-up of 28 knees using dual energy X-ray absorptiometry. J Orthop Res 2000;18(1):40–7. doi:10.1002/jor.1100180107.
Lonner JH, Klotz M, Levitz C, Lotke PA. Changes in bone density after cemented total knee arthroplasty: influence of stem design. J Arthroplasty 2001;16(1):107–11. doi:10.1054/arth.2001.16486.
Hernandez-Vaquero D, Garcia-Sandoval MA, Fernandez-Carreira JM, Gava R. Influence of the tibial stem design on bone density after cemented total knee arthroplasty: a prospective seven-year follow-up study. Int Orthop 2008;32(1):47–51. doi:10.1007/s00264-006-0280-y.
Boyd Jr AD, Ewald FC, Thomas WH, Poss R, Sledge CB. Long-term complications after total knee arthroplasty with or without resurfacing of the patella. J Bone Joint Surg Am 1993;75(5):674–81.
Fitzpatrick CK, Baldwin MA, Ali AA, Laz PJ, Rullkoetter PJ. Comparison of patellar bone strain in the natural and implanted knee during simulated deep flexion. J Orthop Res 2011;29(2):232–9. doi:10.1002/jor.21211.
Compliance with ethical standards
Funding
This study was funded by a research grant from Deutsche Arthrose-Hilfe e.V., Frankfurt, Germany.
Conflicts of interest
None.
Research involving human participants and/or animals
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hirschmann, M.T., Amsler, F. & Rasch, H. Clinical value of SPECT/CT in the painful total knee arthroplasty (TKA): a prospective study in a consecutive series of 100 TKA. Eur J Nucl Med Mol Imaging 42, 1869–1882 (2015). https://doi.org/10.1007/s00259-015-3095-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-015-3095-5