Abstract
Objective
This study was carried out to investigate the effects of abdominal subcutaneous adiposity and visceral adiposity on osteoporotic compression fractures.
Material and methods
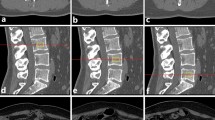
The study group consisted of a total of 152 individuals aged 50–80 years; 76 were included in the vertebral fracture group and 76 in the healthy control group, whose bone mineral density was calculated. In order to determine the distribution of abdominal fat in both groups, four different measurements, i.e., sagittal abdominal diameter (SAD), abdominal diameter (AD), ventral subcutaneous thickness (VST), and dorsal subcutaneous thickness (DST), were made using lumbar magnetic resonance imaging (MRI). The visceral fat ratio (VFR) was also calculated based on these measurements.
Results
There was a significant difference between the patient and control groups in VST and DST values, both when gender distribution was and was not taken into account (p < 0.006 for all cases). There was no significant difference between the patient and control groups in SAD and AS values, both when only female patients were considered, and gender distribution was not taken into account (p > 0.25 for all cases). On the other hand, in the analysis, when only male patients were considered, the SAD and AD values of the patient group were found to be significantly lower than those of the control group (p = 0.046 and p = 0.048, respectively).
Conclusion
In conclusion, the study findings indicated that high SAD values in the male gender and high VST and DST values in both genders were associated with low lumbar vertebral fracture risk.


Similar content being viewed by others
References
Watts NB, Bilezikian JP, Camacho PM, Greenspan SL, Harris ST, Hodgson SF, et al. American Association of Clinical Endocrinologists Medical Guidelines for Clinical Practice for the Diagnosis and Treatment of Postmenopausal Osteoporosis: executive summary of recommendations. Endocr Pract. 2010;16:1016–9.
Radak TL. Caloric restriction and calcium’s effect on bone metabolism and body composition in overweight and obese premenopausal women. Nutr Rev. 2004;62:468–81.
Guney E, Kisakol G, Ozgen G, Yilmaz C, Yilmaz R, Kabalak T. Effect of weight loss on bone metabolism: comparison of vertical banded gastroplasty and medical intervention. Obes Surg. 2003;13:383–8.
Laslett LL, Just nee Foley SJ, Quinn SJ, Winzenberg TM, Jones G. Excess body fat is associated with higher risk of vertebral deformities in older women but not in men: a cross-sectional study. Osteoporosis International. 2012;23:67–74.
Kim K-C, Shin D-H, Lee S-Y, Im J-A, Lee D-C. Relation between obesity and bone mineral density and vertebral fractures in Korean postmenopausal women. Yonsei Med J. 2010;51:857.
Premaor MO, Pilbrow L, Tonkin C, Parker RA, Compston J. Obesity and fractures in postmenopausal women. J Bone Miner Res. 2010;25:292–7.
Fang H, Berg E, Cheng X, Shen W. How to best assess abdominal obesity. Curr Opin Clin Nutr Metab Care. 2018;21:360–5.
Kullberg J, von Below C, Lönn L, Lind L, Ahlström H, Johansson L. Practical approach for estimation of subcutaneous and visceral adipose tissue. Clin Physiol Funct Imaging. 2007;27:148–53.
Zamboni M, Turcato E, Armellini F, Kahn H, Zivelonghi A, Santana H, et al. Sagittal abdominal diameter as a practical predictor of visceral fat. Int J Obes. 1998;22:655–60.
Hayashi T, Boyko EJ, McNeely MJ, Leonetti DL, Kahn SE, Fujimoto WY. Visceral adiposity, not abdominal subcutaneous fat area, is associated with an increase in future insulin resistance in Japanese Americans. Diabetes. 2008;57:1269–75.
Fox CS, Massaro JM, Hoffmann U, Pou KM, Maurovich-Horvat P, Liu C-Y, et al. Abdominal visceral and subcutaneous adipose tissue compartments. Circulation. 2007;116:39–48.
Prevention and management of osteoporosis. World Health Organ Tech Rep Ser. 2003;921.
Genant HK, Wu CY, van Kuijk C, Nevitt MC. Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res. 2009;8:1137–48.
Gilsanz V, Chalfant J, Mo AO, Lee DC, Dorey FJ, Mittelman SD. Reciprocal relations of subcutaneous and visceral fat to bone structure and strength. J Clin Endocrinol Metab. 2009;94(9):3387–93.
Nguyen ND, Pongchaiyakul C, Center JR, Eisman JA, Nguyen TV. Abdominal fat and hip fracture risk in the elderly: the Dubbo Osteoporosis Epidemiology Study. BMC Musculoskelet Disord. 2005;23(6):11. https://doi.org/10.1186/1471-2474-6-11.PMID:15727686;PMCID:PMC554111.
Yang S, Nguyen ND, Center JR, Eisman JA, Nguyen T v. Association between abdominal obesity and fracture risk: a prospective study. J Clin Endocrinol Metab. 2013;98:2478–83.
Rudman HA, Birrell F, Pearce MS, Tuck SP, Francis RM, Treadgold L, et al. Obesity, bone density relative to body weight and prevalent vertebral fracture at age 62 years: the Newcastle thousand families study. Osteoporos Int. 2019;30:829–36.
Gilsanz V, Chalfant J, Mo AO, Lee DC, Dorey FJ, Mittelman SD. Reciprocal relations of subcutaneous and visceral fat to bone structure and strength. J Clin Endocrinol Metab. 2009;94:3387–93.
Saad MAN, Jorge AJL, de Ávila DX, Martins W de A, dos Santos MMS, Tedeschi LT, et al. Sagittal abdominal diameter as a marker of visceral obesity in older primary care patients. J Geriatr Cardiol [Internet]. 2020;17:279–83. Available from: http://www.ncbi.nlm.nih.gov/pubmed/32547611
Yim JY, Kim D, Lim SH, Park MJ, Choi SH, Lee CH, et al. Sagittal abdominal diameter is a strong anthropometric measure of visceral adipose tissue in the Asian general population. Diabetes Care. 2010;33:2665–70.
Öhrvall M, Berglund L, Vessby B. Sagittal abdominal diameter compared with other anthropometric measurements in relation to cardiovascular risk. Int J Obes. 2000;24:497–501.
de Souza NC, de Oliveira EP. Sagittal abdominal diameter shows better correlation with cardiovascular risk factors than waist circumference and BMI. J Diabetes Metab Disord. 2013;12:41.
Empana JP, Ducimetiere P, Charles MA, Jouven X. Sagittal abdominal diameter and risk of sudden death in asymptomatic middle-aged men. Circulation. 2004;110:2781–5.
LuizaLoro M, Sayre J, Roe TF, Goran MI, Kaufman FR, Gilsanz V. Early identification of children predisposed to low peak bone mass and osteoporosis later in life 1. J Clin Endocrinol Metab. 2000;85:3908–18.
Nguyen ND, Pongchaiyakul C, Center JR, Eisman JA, Nguyen T v. Abdominal fat and hip fracture risk in the elderly: The Dubbo Osteoporosis Epidemiology Study. BMC Musculoskelet Disord. 2005;6:11.
Premaor MO, Compston JE, FinaAvilés F, Pagès-Castellà A, Nogués X, Díez-Pérez A, Prieto-Alhambra D. The association between fracture site and obesity in men: a population-based cohort study. J Bone Miner Res. 2013;28(8):1771–7. https://doi.org/10.1002/jbmr.1878
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. The study protocol was approved by the local ethics committee.
Informed consent
Approval from the Institutional Review Board was obtained, and in keeping with the policies for a retrospective review, informed consent was not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gürbüz, A.F., Keven, A., Elasan, S. et al. Evaluation of the relationship between abdominal fat distribution and osteoporotic vertebral compression fracture with MRI. Skeletal Radiol 52, 1203–1210 (2023). https://doi.org/10.1007/s00256-022-04247-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-022-04247-7