Abstract
Objective
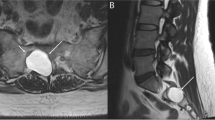
To present cases of juxtaneural ganglia arising from the hip with a discussion of the magnetic resonance imaging (MRI) findings, presenting symptoms, and possible treatment option.
Materials and methods
Two radiologists performed a consensus review of MRI scans obtained between January 2013 and March 2021 to identify patients with juxtaneural ganglia around the hip. A total of 11 patients with 11 juxtaneural ganglia were identified. Medical records and MRI findings were retrospectively reviewed.
Results
Eight patients had lesions involving the sciatic nerve, and three patients had lesions involving the obturator nerve. Sciatic ganglia arose from a paralabral cyst in the posteroinferior quadrant and continued through a narrow channel running along the posterior acetabulum, showing increased diameter in the sciatic foramen and intrapelvic portion. Obturator ganglia showed a J- or reverse J-shape on the coronal imaging plane and extended from a paralabral cyst in the anteroinferior quadrant via the obturator canal. Nine patients (9/11, 81.8%) had symptoms resembling those of lumbosacral radiculopathy. Four patients underwent arthroscopic surgery, and one patient underwent ultrasound-guided aspiration, all of whom showed partial improvement. Spontaneous decrease in the extent of the ganglion was observed in three patients (3/11, 27.3%).
Conclusion
This article describes rare cases of juxtaneural ganglia arising from the hip joint and involving the sciatic and obturator nerves. The lesions share similar MRI findings, and each type of cyst (sciatic or obturator ganglia) involves a specific labral quadrant.







Similar content being viewed by others
References
Desy NM, Wang H, Elshiekh MA, et al. Intraneural ganglion cysts: a systematic review and reinterpretation of the world’s literature. J Neurosurg. 2016;125(3):615–30.
Spinner RJ, Hebert-Blouin MN, Trousdale RT, et al. Intraneural ganglia in the hip and pelvic region. Clinical article J Neurosurg. 2009;111(2):317–25.
Desy NM, Lipinski LJ, Tanaka S, Amrami KK, Rock MG, Spinner RJ. Recurrent intraneural ganglion cysts: pathoanatomic patterns and treatment implications. Clin Anat. 2015;28(8):1058–69.
Spinner RJ, Vincent JF, Wolanskyj AP, Scheithauer BW. Intraneural ganglion cyst: a 200-year-old mystery solved. Clin Anat. 2008;21(7):611–8.
Spinner RJ, Atkinson JL, Tiel RL. Peroneal intraneural ganglia: the importance of the articular branch. A unifying theory J Neurosurg. 2003;99(2):330–43.
Spinner RJ, Amrami KK, Wolanskyj AP, et al. Dynamic phases of peroneal and tibial intraneural ganglia formation: a new dimension added to the unifying articular theory. J Neurosurg. 2007;107(2):296–307.
Spinner RJ, Luthra G, Desy NM, Anderson ML, Amrami KK. The clock face guide to peroneal intraneural ganglia: critical “times” and sites for accurate diagnosis. Skeletal Radiol. 2008;37(12):1091–9.
Spinner RJ, Desy NM, Amrami KK, Vosoughi AR, Klaue K. Expanding on the term “balloon” sign. Acta Neurochir (Wien). 2016;158(10):1891–3.
Nagpal AS, Brennick C, Occhialini AP, et al. Innervation of the posterior hip capsule: a cadaveric study. Pain Med. 2021;22(5):1072–9.
Jitpun E, Howe BMM, Amrami KK, Trousdale RT, Spinner RJ. Obturator intraneural ganglion cysts: joint connected and underdiagnosed. World Neurosurg. 2019;126:e259–69.
Beaman FD, Kransdorf MJ, Menke DM. Schwannoma: radiologic-pathologic correlation. Radiographics. 2004;24(5):1477–81.
Palmer W, Bancroft L, Bonar F, et al. Glossary of terms for musculoskeletal radiology. Skeletal Radiol. 2020;49(Suppl 1):1–33.
Torriani M, Souto SC, Thomas BJ, Ouellette H, Bredella MA. Ischiofemoral impingement syndrome: an entity with hip pain and abnormalities of the quadratus femoris muscle. AJR Am J Roentgenol. 2009;193(1):186–90.
Tosun O, Algin O, Yalcin N, Cay N, Ocakoglu G, Karaoglanoglu M. Ischiofemoral impingement: evaluation with new MRI parameters and assessment of their reliability. Skeletal Radiol. 2012;41(5):575–87.
Mascarenhas VV, Castro MO, Rego PA, et al. The Lisbon Agreement on Femoroacetabular Impingement Imaging-part 1: overview. Eur Radiol. 2020;30(10):5281–97.
Spinner RJ, Scheithauer BW, Desy NM, Rock MG, Holdt FC, Amrami KK. Coexisting secondary intraneural and vascular adventitial ganglion cysts of joint origin: a causal rather than a coincidental relationship supporting an articular theory. Skeletal Radiol. 2006;35(10):734–44.
Birnbaum K, Prescher A, Hessler S, Heller KD. The sensory innervation of the hip joint—an anatomical study. Surg Radiol Anat. 1997;19(6):371–5.
Kampa RJ, Prasthofer A, Lawrence-Watt DJ, Pattison RM. The internervous safe zone for incision of the capsule of the hip. A cadaver study. J Bone Joint Surg Br. 2007;89(7):971–6.
Peri G. The, “critical zones” of entrapment of the nerves of the lower limb. Surg Radiol Anat. 1991;13(2):139–43.
Yukata K, Arai K, Yoshizumi Y, Tamano K, Imada K, Nakaima N. Obturator neuropathy caused by an acetabular labral cyst: MRI findings. AJR Am J Roentgenol. 2005;184(3 Suppl):S112–4.
Vidoni A, Sankara STV, Ramana V, Botchu R. Ganglion cyst arising from the transverse acetabular ligament (TAL): a rare cause of entrapment of the anterior branch of the obturator nerve. Case report and review of the literature. Skeletal Radiol. 2019;48(1):163–5.
Lovaglio AC, Mansilla B, Cejas C, Spinner RJ, Socolovsky M. Femoral intraneural ganglion cyst: the first confirmed case report. Br J Neurosurg. 2020:1–3.
James SL, Ali K, Malara F, Young D, O’Donnell J, Connell DA. MRI findings of femoroacetabular impingement. AJR Am J Roentgenol. 2006;187(6):1412–9.
Magerkurth O, Jacobson JA, Girish G, Brigido MK, Bedi A, Fessell D. Paralabral cysts in the hip joint: findings at MR arthrography. Skeletal Radiol. 2012;41(10):1279–85.
Chhabra A, Lee PP, Bizzell C, Soldatos T. 3 Tesla MR neurography—technique, interpretation, and pitfalls. Skeletal Radiol. 2011;40(10):1249–60.
Chhabra A, Madhuranthakam AJ, Andreisek G. Magnetic resonance neurography: current perspectives and literature review. Eur Radiol. 2018;28(2):698–707.
Knoll A, Pal’a A, Pedro MT, et al. Clinical outcome after decompression of intraneural peroneal ganglion cyst and its morphologic correlation to postoperative nerve ultrasound. J Neurosurg. 2019:1–7.
Park SH, Do HK, Jo GY. Compressive peroneal neuropathy by an intraneural ganglion cyst combined with L5 radiculopathy: a case report. Medicine (Baltimore). 2019;98(44):e17865.
Liang T, Panu A, Crowther S, Low G, Lambert R. Ultrasound-guided aspiration and injection of an intraneural ganglion cyst of the common peroneal nerve. HSS J. 2013;9(3):270–4.
Li P, Lou D, Lu H. The cubital tunnel syndrome caused by intraneural ganglion cyst of the ulnar nerve at the elbow: a case report. BMC Neurol. 2018;18(1):217.
Kim SH, Seok H, Lee SY, Park SW. Acetabular paralabral cyst as a rare cause of obturator neuropathy: a case report. Ann Rehabil Med. 2014;38(3):427–32.
Elangovan S, Odegard GM, Morrow DA, Wang H, Hebert-Blouin MN, Spinner RJ. Intraneural ganglia: a clinical problem deserving a mechanistic explanation and model. Neurosurg Focus. 2009;26(2):E11.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Approval from the institutional review board was obtained and in keeping with the policies for a retrospective review; informed consent was not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shin, N., Kim, H.S., Lee, J.H. et al. Juxtaneural ganglia arising from the hip joint: focus on magnetic resonance imaging findings and clinical manifestations. Skeletal Radiol 51, 1439–1452 (2022). https://doi.org/10.1007/s00256-022-03989-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-022-03989-8