Abstract
Aim
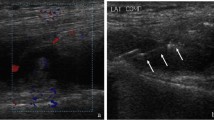
Synovial sampling can be used in the diagnosis of peri-prosthetic joint infection (PJI). The purpose of this study was to establish the role of simultaneous image-guided synovial aspiration and biopsy (SAB) during an initial 2-year experience at our institution.
Methods
Retrospective review of consecutive SABs performed during 2014–2016 at a tertiary referral musculoskeletal centre. Radiological SAB microbiology culture results were compared with intra-operative surgical samples or multidisciplinary team (MDT) meeting outcome at 1-year follow-up if surgery was not undertaken. Sensitivity, specificity and accuracy of synovial aspiration (SA), synovial biopsy (SB) and simultaneous SAB were calculated.
Results
103 patients (46 male, 57 female) totalling 111 procedures were analysed with mean age 65 years (range 31–83). Image-guided synovial procedures were performed on 52 (46.9%) hip and 59 (53.1%) knee joint prostheses. The mean combined sensitivity, specificity and accuracy for the entire cohort was 72.6%, 96.9% and 90%, respectively. When only SB was obtained, diagnostic accuracy (92.5%) was similar to SA alone (94.1%). In total, there were 21 (18.9%) true-positive, 80 (72.1%) true-negative, 2 (1.8%) false-positive and 8 (7.2%) false-negative cases (PPV 91.3% and NPV 90.9%). No post-procedural complications were recorded at 1-year follow-up.
Conclusion
Percutaneous image-guided SAB is a valuable technique in assessing suspected PJI, with most samples indicative of infective status and causative organisms when validated against intra-operative results and specialist MDT evaluation. Image-guided SB is a safe and useful additional procedure following failed SA with equivalent levels of diagnostic accuracy.


Similar content being viewed by others
References
Izakovicova P, Borens O, Trampuz A. Periprosthetic joint infection: current concepts and outlook. EFORT Open Rev. 2019;4(7):482–94.
Rangan A, Falworth M, Watts AC, et al. Investigation and management of periprosthetic joint infection in the shoulder and elbow: evidence and consensus based guidelines of the British Elbow and Shoulder Society [published correction appears in shoulder elbow. 2018 Oct;10(4):NP1]. Should Elb. 2018;10(1 Suppl):S5–S19.
Gbejuade HO, Lovering AM, Webb JC. The role of microbial biofilms in prosthetic joint infections. Acta Orthop. 2015;86(2):147–58.
Renz N, Mudrovcic S, Perka C, Trampuz A. Orthopedic implant-associated infections caused by Cutibacterium spp. – a remaining diagnostic challenge. PLoS One. 2018;13(8):e0202639.
Saleh A, George J, Faour M, et al. Serum biomarkers in periprosthetic joint infections. Bone Joint Res. 2018;7(1):85–93.
Yee DK, Chiu KY, Yan CH, et al. Review article: joint aspiration for diagnosis of periprosthetic infection. J Orthop Surg (Hong Kong). 2013 Aug;21(2):236–40.
Cross MC, Kransdorf MJ, Chivers FS, et al. Utility of percutaneous joint aspiration and synovial biopsy in identifying culture-positive infected hip arthroplasty. Skelet Radiol. 2014;43(2):165–8.
Ali F, Wilkinson JM, Cooper JR, et al. Accuracy of joint aspiration for the preoperative diagnosis of infection in total hip arthroplasty. J Arthroplast. 2006;21:221–6.
Fink B, Gebhard A, Fuerst M, Berger I, et al. High diagnostic value of synovial biopsy in periprosthetic joint infection of the hip. Clin Orthop Relat Res. 2013;471(3):956–64.
Fink B, Makowiak C, Fuerst M, Berger I, Schäfer P, Frommelt L. The value of synovial biopsy, joint aspiration and C-reactive protein in the diagnosis of late peri-prosthetic infection of total knee replacements. J Bone Joint Surg (Br). 2008;90(7):874–8.
Signore A, Sconfienza LM, Borens O, et al. Consensus document for the diagnosis of prosthetic joint infections: a joint paper by the EANM, EBJIS, and ESR (with ESCMID endorsement) [published correction appears in Eur J Nucl med Mol imaging. 2019 Feb 9]. Eur J Nucl Med Mol Imaging. 2019;46(4):971–88.
Fowler TJ, Sayers A, Whitehouse MR. Two-stage revision surgery for periprosthetic joint infection following total hip arthroplasty. Ann Transl Med. 2019;7(Suppl 8):S261.
Taha M, Abdelbary H, Ross FP, et al. New innovations in the treatment of PJI and biofilms-clinical and preclinical topics. Curr Rev Musculoskelet Med. 2018;11(3):380–8.
Alvand A, Carrington R, Miles J. Surgical strategies for management of infection following knee arthroplasty and arthroscopic procedures. Orthop Trauma. 2019;33. https://doi.org/10.1016/j.mporth.2019.03.003.
Parvizi J, Gehrke T, Chen AF. Proceedings of the international consensus on periprosthetic joint infection. Bone Joint J. 2013;95-B(11):1450–2.
Tande AJ, Patel R. Prosthetic joint infection. Clin Microbiol Rev. 2014;27(2):302–45.
Fey PD, Olson ME. Current concepts in biofilm formation of Staphylococcus epidermidis. Future Microbiol. 2010;5(6):917–33.
Lourtet-Hascoët J, Bicart-See A, Félicé MP, et al. Staphylococcus lugdunensis, a serious pathogen in periprosthetic joint infections: comparison to Staphylococcus aureus and Staphylococcus epidermidis. Int J Infect Dis. 2016;51:56–61.
Shah NB, Osmon DR, Fadel H, et al. Laboratory and clinical characteristics of Staphylococcus lugdunensis prosthetic joint infections. J Clin Microbiol. 2010;48:1600–3.
Ottink KD, Strahm C, Muller-Kobold A, et al. Factors to consider when assessing the diagnostic accuracy of synovial leukocyte count in periprosthetic joint infection. J Bone Jt Infect. 2019;4(4):167–73.
Cazanave C, Greenwood-Quaintance KE, Hanssen AD, et al. Corynebacterium prosthetic joint infection. J Clin Microbiol. 2012;50(5):1518–23.
Reisener M, Perka C. Do culture-negative periprosthetic joint infections have a worse outcome than culture-positive periprosthetic joint infections? A Systematic Review and Meta-Analysis Biomed Res Int. 2018;2018:6278012.
Parker S, Key T, Hughes H, et al. The myth of surgical sterility: bacterial contamination of knee arthroplasty drapes. 2018;98-B,(SUPP_23,).
Xu C, Tan TL, Li WT, et al. Reporting outcomes of treatment for periprosthetic joint infection of the knee and hip together with a minimum 1-year follow-up is reliable. J Arthroplast. 2020;35(7):1906–1911.e5.
Ntalos D, Berger-Groch J, Rohde H, et al. Implementation of a multidisciplinary infections conference affects the treatment plan in prosthetic joint infections of the hip: a retrospective study. Arch Orthop Trauma Surg. 2019;139(4):467–73.
Acknowledgements
The authors would like to thank all members of the Joint Replacement Unit Infection MDT at the Royal National Orthopaedic Hospital, Stanmore, comprising nursing and administrative colleagues, orthopaedic surgeons, microbiologists and radiologists. The authors would also like to extend thanks to Dr Peter Munk and Dr Hugue Ouellette (Vancouver General Hospital, University of British Columbia) for identifying the potential benefits of percutaneous synovial biopsy at the time of synovial aspiration using co-axial interventional radiology techniques.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rajakulasingam, R., Cleaver, L., Khoo, M. et al. Introducing image-guided synovial aspiration and biopsy in assessing peri-prosthetic joint infection: an early single-centre experience. Skeletal Radiol 50, 2031–2040 (2021). https://doi.org/10.1007/s00256-021-03774-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-021-03774-z