Abstract
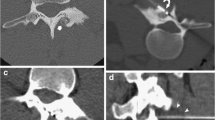
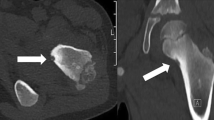
A 37-year-old man presented with a 2-year history of left hip pain. Pretherapeutic imaging demonstrated a 4 cm osteoblastoma located in the intertrochanteric region of the proximal femur, surrounded by extensive bone marrow edema. After multidisciplinary meeting, percutaneous cryoablation was decided and performed under computed tomography guidance using three cryoprobes to match the exact size and shape of the tumor, resulting in complete resolution of symptoms. Magnetic resonance imaging follow-up demonstrated resolution of the bone marrow edema pattern and ingrowth of fat at the periphery of the ablation zone consistent with long-term healing of the tumor.




Similar content being viewed by others
References
Yalcinkaya U, Doganavsargil B, Sezak M, Kececi B, Argin M, Basdemir G, et al. Clinical and morphological characteristics of osteoid osteoma and osteoblastoma: a retrospective single-center analysis of 204 patients. Ann Diagn Pathol. 2014;18:319–25.
Zhang Y, Rosenberg AE. Bone-forming tumors. Surgical Pathology Clinics. 2017;10:513–35.
Berry M, Mankin H, Gebhardt M, Rosenberg A, Hornicek F. Osteoblastoma: a 30-year study of 99 cases. J Surg Oncol. 2008;98:179–83.
Rosenthal D, Callstrom MR. Critical review and state of the art in interventional oncology: benign and metastatic disease involving bone. Radiology. 2012;262:765–80.
Callstrom MR, Kurup AN. Percutaneous ablation for bone and soft tissue metastases-why cryoablation? Skelet Radiol. 2009;38:835–9.
Thacker PG, Callstrom MR, Curry TB, et al. Palliation of painful metastatic disease involving bone with imaging-guided treatment: Comparison of patients’ immediate response to radiofrequency ablation and cryoablation. Am J Roentgenol. 2011;197:510–5.
Fletcher CDM, Bidge JA, Hogendoom P, et al. World Health Organisation classification of tumours, pathology and genetics. In: Tumours of soft tissue and bone, vol. 5. 4th ed: ARC; 2013. p. 277–80.
Weber MA, Sprengel SD, Omlor GW, et al. Clinical long-term outcome, technical success, and cost analysis of radiofrequency ablation for the treatment of osteoblastomas and spinal osteoid osteomas in comparison to open surgical resection. Skelet Radiol. 2015;44:981–93.
Coupal TM, Mallinson PI, Munk PL, Liu D, Clarkson P, Ouellette H. CT-guided percutaneous cryoablation for osteoid osteoma: initial experience in adults. Am J Roentgenol. 2014;202:1136–9.
Santiago E, Pauly V, Brun G, Guenoun D, Champsaur P, Le Corroller T. Percutaneous cryoablation for the treatment of osteoid osteoma in the adult population. Eur Radiol. 2018;28:2336–44.
Kumasaka S, Miyazaki M, Tsushima Y. CT- guided percutaneous cryoablation of an aggressive osteoblastoma: a case report. J Vasc Interv Radiol. 2015;26:1746–8.
Cazzato RL, Auloge P, Dalili D, De Marini P, Di Marco A, Garnon J, et al. Percutaneous image-guided cryoablation of osteoblastoma. AJR Am J Roentgenol. 2019;213:1157–62.
Auloge P, Cazzato RL, Rousseau C, Caudrelier J, Koch G, Rao P, et al. Complications of percutaneous bone tumor cryoablation: a 10-year experience. Radiology. 2019;291:521–8.
Jennings JW. Is percutaneous bone cryoablation safe? Radiology. 2019;291:529–30.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Poullain, F., Mattei, J., Rochwerger, A. et al. Percutaneous cryoablation of osteoblastoma in the proximal femur. Skeletal Radiol 49, 1467–1471 (2020). https://doi.org/10.1007/s00256-020-03413-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-020-03413-z