Abstract
Objective
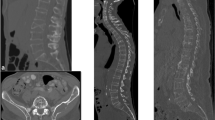
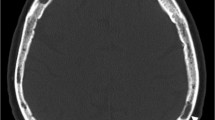
To observe the distribution and potential distribution patterns of osteolytic and sclerotic vertebral involvement in a representative collective of multiple myeloma patients.
Materials and methods
A total of 66 consecutive patients with a diagnosis of multiple myeloma at initial diagnosis or during follow-up were examined by multidetector reduced-dose computed tomography to evaluate the distribution of bone lesions along the spine with focus on size, location, and lesion character. Confirmation of diagnosis was performed by comparison to follow-up computed tomography or magnetic resonance tomography. If >50 % of all detected malignant lesions occurred in one spinal segment, the distribution pattern was called cervical, thoracic, lumbar, or sacral, otherwise a “mixed” pattern was classified.
Results
Of a total number of 933 osseous spine lesions, 632 (67.7 %) were classified as malignant (98.9 % of them osteolytic) and 293 (31.5 %) as benign. The distribution pattern analysis yielded two patients (3.8 %) with a cervical, 26 (50 %) with a thoracic, 4 (7.7 %) with a lumbar, one (1.9 %) with a sacral pattern, and 19 cases (36.6 %) showed a mixed distribution pattern. Segment-wise, the mean lesion size was 6.52 ± 2.76 mm (cervical), 8.97 ± 5.43 mm (thoracic), 11.97 ± 7.11 mm (lumbar), and 17.5 ± 16.465 (sacral), whilst, related to the vertebra size, the lesion/vertebra size ratio is decreasing through the whole spine beginning from the top.
Conclusions
Multiple myeloma bone lesions occur preferably and are larger in the thoracic and lumbar spine. Moreover, a specific distribution pattern is present in about 60 %.



Similar content being viewed by others
References
Kyle RA, Gertz MA, Witzig TE, Lust JA, Lacy MQ, Dispenzieri A, et al. Review of 1027 patients with newly diagnosed multiple myeloma. Mayo Clin Proc. 2003;78:21–33.
Durie BG, Salmon SE. A clinical staging system for multiple myeloma. Correlation of measured myeloma cell mass with presenting clinical features, response to treatment, and survival. Cancer. 1975;36(3):842–54.
International Myeloma Working G. Criteria for the classification of monoclonal gammopathies, multiple myeloma and related disorders: a report of the International Myeloma Working Group. Br J Haematol. 2003;121(5):749–57.
Terpos E, Dimopoulos MA. Myeloma bone disease: pathophysiology and management. Ann Oncol Off J Eur Soc Med Oncol ESMO. 2005;16(8):1223–31.
Lacy MQ, Gertz MA, Hanson CA, Inwards DJ, Kyle RA. Multiple myeloma associated with diffuse osteosclerotic bone lesions: a clinical entity distinct from osteosclerotic myeloma (POEMS syndrome). Am J Hematol. 1997;56(4):288–93.
Prasad R, Yadav RR, Singh A, Mathur SP, Mangal Y, Singh M. Case report. Non-secretory multiple myeloma presenting with diffuse sclerosis of affected bones interspersed with osteolytic lesions. Br J Radiol. 2009;82(974):e29–31.
Baur A, Stabler A, Bartl R, Lamerz R, Reiser M. Infiltration patterns of plasmacytomas in magnetic resonance tomography. RoFo Fortschritte auf dem Gebiete der Rontgenstrahlen und der Nuklearmedizin. 1996;164(6):457–63.
Song MK, Chung JS, Lee JJ, Min CK, Ahn JS, Lee SM, et al. Magnetic resonance imaging pattern of bone marrow involvement as a new predictive parameter of disease progression in newly diagnosed patients with multiple myeloma eligible for autologous stem cell transplantation. Br J Haematol. 2014;165(6):777–85.
Moulopoulos LA, Dimopoulos MA, Kastritis E, Christoulas D, Gkotzamanidou M, Roussou M, et al. Diffuse pattern of bone marrow involvement on magnetic resonance imaging is associated with high risk cytogenetics and poor outcome in newly diagnosed, symptomatic patients with multiple myeloma: a single center experience on 228 patients. Am J Hematol. 2012;87(9):861–4.
Croucher PI, Apperley JF. Bone disease in multiple myeloma. Br J Haematol. 1998;103(4):902–10.
Prasad D, Schiff D. Malignant spinal-cord compression. Lancet Oncol. 2005;6(1):15–24.
Lecouvet FE, Malghem J, Michaux L, Michaux JL, Lehmann F, Maldague BE, et al. Vertebral compression fractures in multiple myeloma. Part II. Assessment of fracture risk with MR imaging of spinal bone marrow. Radiology. 1997;204(1):201–5.
Ramos L, de Las Heras JA, Sanchez S, Gonzalez-Porras JR, Gonzalez R, Mateos MV, et al. Medium-term results of percutaneous vertebroplasty in multiple myeloma. Eur J Haematol. 2006;77(1):7–13.
McDonald RJ, Trout AT, Gray LA, Dispenzieri A, Thielen KR, Kallmes DF. Vertebroplasty in multiple myeloma: outcomes in a large patient series. AJNR Am J Neuroradiol. 2008;29(4):642–8.
Anselmetti GC, Manca A, Montemurro F, Hirsch J, Chiara G, Grignani G, et al. Percutaneous vertebroplasty in multiple myeloma: prospective long-term follow-up in 106 consecutive patients. Cardiovasc Intervent Radiol. 2012;35(1):139–45.
Cai W, Yan W, Huang Q, Huang W, Yin H, Xiao J. Surgery for plasma cell neoplasia patients with spinal instability or neurological impairment caused by spinal lesions as the first clinical manifestation. Eur Spine J Off Publ Eur Spine Soc Eur Spinal Deformity Soc Eur Sect Cervical Spine Res Soc. 2014.
Tamburrelli FC, Proietti L, Scaramuzzo L, De Stefano V, Logroscino CA. Bisphosphonate therapy in multiple myeloma in preventing vertebral collapses: preliminary report. Eur Spine J Off Publ Eur Spine Soc Eur Spinal Deformity Soc Eur Sect Cervical Spine Res Soc. 2012;21 Suppl 1:S141–5.
Lecouvet FE, Vande Berg BC, Maldague BE, Michaux L, Laterre E, Michaux JL, et al. Vertebral compression fractures in multiple myeloma. Part I. Distribution and appearance at MR imaging. Radiology. 1997;204(1):195–9.
Princewill K, Kyere S, Awan O, Mulligan M. Multiple myeloma lesion detection with whole body CT versus radiographic skeletal survey. Cancer Investig. 2013;31(3):206–11.
Tancioni F, Lorenzetti M, Navarria P, Nozza A, Castagna L, Gaetani P, et al. Vertebroplasty for pain relief and spinal stabilization in multiple myeloma. Neurol Sci Off J Ital Neurol Soc Ital Soc Clin Neurophysiol. 2010;31(2):151–7.
Hayman JA, Callahan JW, Herschtal A, Everitt S, Binns DS, Hicks RJ, et al. Distribution of proliferating bone marrow in adult cancer patients determined using FLT-PET imaging. Int J Radiat Oncol Biol Phys. 2011;79(3):847–52.
Hur J, Yoon CS, Ryu YH, Yun MJ, Suh JS. Efficacy of multidetector row computed tomography of the spine in patients with multiple myeloma: comparison with magnetic resonance imaging and fluorodeoxyglucose-positron emission tomography. J Comput Assist Tomogr. 2007;31(3):342–7.
Bannas P, Kroger N, Adam G, Derlin T. Modern imaging techniques in patients with multiple myeloma. RoFo Fortschritte auf dem Gebiete der Rontgenstrahlen und der Nuklearmedizin. 2013;185(1):26–33.
Acknowledgments
This study was supported by the Ludwig Hiermaier Foundation for Applied Cancer Research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Bier, G., Kloth, C., Schabel, C. et al. Vertebral lesion distribution in multiple myeloma—assessed by reduced-dose whole-body MDCT. Skeletal Radiol 45, 127–133 (2016). https://doi.org/10.1007/s00256-015-2268-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-015-2268-4