Abstract
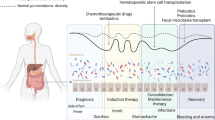
Prophylactic or therapeutic antibiotic use along with chemotherapy treatment potentially has a long-standing adverse effect on the resident gut microbiota. We have established a case-control cohort of 32 pediatric and adolescent acute lymphoblastic leukemia (ALL) patients and 25 healthy siblings (sibling controls) to assess the effect of chemotherapy as well as antibiotic prophylaxis on the gut microbiota. We observe that the microbiota diversity and richness of the ALL group is significantly lower than that of the control group at diagnosis and during chemotherapy. The microbiota diversity is even lower in antibiotics-exposed ALL patients. Although the gut microbial diversity tends to stabilize after 1-year post-chemotherapy, their abundances were altered because of chemotherapy and prophylactic antibiotic treatments. Specifically, the abundances of mucolytic gram-positive anaerobic bacteria, including Ruminococcus gnavus and Ruminococcus torques, tended to increase during the chemotherapy regimen and continued to be elevated 1 year beyond the initiation of chemotherapy. This dysbiosis may contribute to the development of gastrointestinal complications in ALL children following chemotherapy. These findings set the stage to further understand the role of the gut microbiome dynamics in ALL patients and their potential role in alleviating some of the adverse side effects of chemotherapy and antibiotics use in immunocompromised children.




Similar content being viewed by others
Data Availability
The 16S rRNA gene sequencing data utilized in the study is available via the NIH BioProject Accession PRJNA421352. The metadata is available in the supplementary files as well as available from the NIH Biosamples.
References
Smith MA RL, Gurney JG, et al. (1999) Leukemia. In: Ries LA, Smith MA, Gurney JG, et al., eds Cancer incidence and survival among children and adolescents: United States SEER Program 1975-1995. Bethesda, Md: National Cancer Institute, SEER Program NIH PubNo 99-4649, pp 17-34.
Ward E, DeSantis C, Robbins A, Kohler B, Jemal A (2014) Childhood and adolescent cancer statistics, 2014. CA Cancer J Clin 64:83–103. https://doi.org/10.3322/caac.21219
Oeffinger KC, Mertens AC, Sklar CA, Kawashima T, Hudson MM, Meadows AT, Friedman DL, Marina N, Hobbie W, Kadan-Lottick NS, Schwartz CL, Leisenring W, Robison LL, Childhood Cancer Survivor S (2006) Chronic health conditions in adult survivors of childhood cancer. N Engl J Med 355:1572–1582. https://doi.org/10.1056/NEJMsa060185
van Vliet MJ, Harmsen HJ, de Bont ES, Tissing WJ (2010) The role of intestinal microbiota in the development and severity of chemotherapy-induced mucositis. PLoS Pathog 6:e1000879. https://doi.org/10.1371/journal.ppat.1000879
Hudson MM, Ness KK, Gurney JG, Mulrooney DA, Chemaitilly W, Krull KR, Green DM, Armstrong GT, Nottage KA, Jones KE, Sklar CA, Srivastava DK, Robison LL (2013) Clinical ascertainment of health outcomes among adults treated for childhood cancer. JAMA 309:2371–2381. https://doi.org/10.1001/jama.2013.6296
Gibson TM, Ehrhardt MJ, Ness KK (2016) Obesity and metabolic syndrome among adult survivors of childhood leukemia. Curr Treat Options in Oncol 17:17. https://doi.org/10.1007/s11864-016-0393-5
Rajagopala SV, Vashee S, Oldfield LM, Suzuki Y, Venter JC, Telenti A, Nelson KE (2017) The human microbiome and cancer. Cancer Prev Res (Phila) 10:226–234. https://doi.org/10.1158/1940-6207.CAPR-16-0249
Karlsson F, Tremaroli V, Nielsen J, Backhed F (2013) Assessing the human gut microbiota in metabolic diseases. Diabetes 62:3341–3349. https://doi.org/10.2337/db13-0844
Le Chatelier E, Nielsen T, Qin J, Prifti E, Hildebrand F, Falony G, Almeida M, Arumugam M, Batto JM, Kennedy S, Leonard P, Li J, Burgdorf K, Grarup N, Jorgensen T, Brandslund I, Nielsen HB, Juncker AS, Bertalan M, Levenez F, Pons N, Rasmussen S, Sunagawa S, Tap J, Tims S, Zoetendal EG, Brunak S, Clement K, Dore J, Kleerebezem M, Kristiansen K, Renault P, Sicheritz-Ponten T, de Vos WM, Zucker JD, Raes J, Hansen T, Meta HITc, Bork P, Wang J, Ehrlich SD, Pedersen O (2013) Richness of human gut microbiome correlates with metabolic markers. Nature 500:541–546. https://doi.org/10.1038/nature12506
Pedersen HK, Gudmundsdottir V, Nielsen HB, Hyotylainen T, Nielsen T, Jensen BA, Forslund K, Hildebrand F, Prifti E, Falony G, Le Chatelier E, Levenez F, Dore J, Mattila I, Plichta DR, Poho P, Hellgren LI, Arumugam M, Sunagawa S, Vieira-Silva S, Jorgensen T, Holm JB, Trost K, Meta HITC, Kristiansen K, Brix S, Raes J, Wang J, Hansen T, Bork P, Brunak S, Oresic M, Ehrlich SD, Pedersen O (2016) Human gut microbes impact host serum metabolome and insulin sensitivity. Nature 535:376–381. https://doi.org/10.1038/nature18646
Turnbaugh PJ, Hamady M, Yatsunenko T, Cantarel BL, Duncan A, Ley RE, Sogin ML, Jones WJ, Roe BA, Affourtit JP, Egholm M, Henrissat B, Heath AC, Knight R, Gordon JI (2009) A core gut microbiome in obese and lean twins. Nature 457:480–484. https://doi.org/10.1038/nature07540
Fulde M, Hornef MW (2014) Maturation of the enteric mucosal innate immune system during the postnatal period. Immunol Rev 260:21–34. https://doi.org/10.1111/imr.12190
Sivan A, Corrales L, Hubert N, Williams JB, Aquino-Michaels K, Earley ZM, Benyamin FW, Lei YM, Jabri B, Alegre ML, Chang EB, Gajewski TF (2015) Commensal Bifidobacterium promotes antitumor immunity and facilitates anti-PD-L1 efficacy. Science 350:1084–1089. https://doi.org/10.1126/science.aac4255
Vetizou M, Pitt JM, Daillere R, Lepage P, Waldschmitt N, Flament C, Rusakiewicz S, Routy B, Roberti MP, Duong CP, Poirier-Colame V, Roux A, Becharef S, Formenti S, Golden E, Cording S, Eberl G, Schlitzer A, Ginhoux F, Mani S, Yamazaki T, Jacquelot N, Enot DP, Berard M, Nigou J, Opolon P, Eggermont A, Woerther PL, Chachaty E, Chaput N, Robert C, Mateus C, Kroemer G, Raoult D, Boneca IG, Carbonnel F, Chamaillard M, Zitvogel L (2015) Anticancer immunotherapy by CTLA-4 blockade relies on the gut microbiota. Science 350:1079–1084. https://doi.org/10.1126/science.aad1329
Rajagopala SV, Yooseph S, Harkins DM, Moncera KJ, Zabokrtsky KB, Torralba MG, Tovchigrechko A, Highlander SK, Pieper R, Sender L, Nelson KE (2016) Gastrointestinal microbial populations can distinguish pediatric and adolescent acute lymphoblastic leukemia (ALL) at the time of disease diagnosis. BMC Genomics 17:635. https://doi.org/10.1186/s12864-016-2965-y
Hakim H, Dallas R, Wolf J, Tang L, Schultz-Cherry S, Darling V, Johnson C, Karlsson EA, Chang TC, Jeha S, Pui CH, Sun Y, Pounds S, Hayden RT, Tuomanen E, Rosch JW (2018) Gut microbiome composition predicts infection risk during chemotherapy in children with acute lymphoblastic leukemia. Clin Infect Dis. https://doi.org/10.1093/cid/ciy153
Edgar RC (2013) UPARSE: highly accurate OTU sequences from microbial amplicon reads. Nat Methods 10:996–998. https://doi.org/10.1038/nmeth.2604
Miquel S, Martin R, Rossi O, Bermudez-Humaran LG, Chatel JM, Sokol H, Thomas M, Wells JM, Langella P (2013) Faecalibacterium prausnitzii and human intestinal health. Curr Opin Microbiol 16:255–261. https://doi.org/10.1016/j.mib.2013.06.003
Frank DN, St Amand AL, Feldman RA, Boedeker EC, Harpaz N, Pace NR (2007) Molecular-phylogenetic characterization of microbial community imbalances in human inflammatory bowel diseases. Proc Natl Acad Sci U S A 104:13780–13785. https://doi.org/10.1073/pnas.0706625104
Machiels K, Joossens M, Sabino J, De Preter V, Arijs I, Eeckhaut V, Ballet V, Claes K, Van Immerseel F, Verbeke K, Ferrante M, Verhaegen J, Rutgeerts P, Vermeire S (2014) A decrease of the butyrate-producing species Roseburia hominis and Faecalibacterium prausnitzii defines dysbiosis in patients with ulcerative colitis. Gut 63:1275–1283. https://doi.org/10.1136/gutjnl-2013-304833
Sokol H, Pigneur B, Watterlot L, Lakhdari O, Bermudez-Humaran LG, Gratadoux JJ, Blugeon S, Bridonneau C, Furet JP, Corthier G, Grangette C, Vasquez N, Pochart P, Trugnan G, Thomas G, Blottiere HM, Dore J, Marteau P, Seksik P, Langella P (2008) Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients. Proc Natl Acad Sci U S A 105:16731–16736. https://doi.org/10.1073/pnas.0804812105
Chua LL, Rajasuriar R, Azanan MS, Abdullah NK, Tang MS, Lee SC, Woo YL, Lim YA, Ariffin H, Loke P (2017) Reduced microbial diversity in adult survivors of childhood acute lymphoblastic leukemia and microbial associations with increased immune activation. Microbiome 5:35. https://doi.org/10.1186/s40168-017-0250-1
Pinheiro J, Bates D, DebRoy S, Sarkar D, Team RC (2018) nlme: linear and nonlinear mixed effects models. R package version 31-137
Rekha R, Rizvi MA, Jaishree P (2006) Designing and validation of genus-specific primers for human gut flora study
Galloway-Pena JR, Smith DP, Sahasrabhojane P, Ajami NJ, Wadsworth WD, Daver NG, Chemaly RF, Marsh L, Ghantoji SS, Pemmaraju N, Garcia-Manero G, Rezvani K, Alousi AM, Wargo JA, Shpall EJ, Futreal PA, Guindani M, Petrosino JF, Kontoyiannis DP, Shelburne SA (2016) The role of the gastrointestinal microbiome in infectious complications during induction chemotherapy for acute myeloid leukemia. Cancer 122:2186–2196. https://doi.org/10.1002/cncr.30039
Montassier E, Gastinne T, Vangay P, Al-Ghalith GA, Bruley des Varannes S, Massart S, Moreau P, Potel G, de La Cochetiere MF, Batard E, Knights D (2015) Chemotherapy-driven dysbiosis in the intestinal microbiome. Aliment Pharmacol Ther 42:515–528. https://doi.org/10.1111/apt.13302
Hansen SG, Skov MN, Justesen US (2013) Two cases of Ruminococcus gnavus bacteremia associated with diverticulitis. J Clin Microbiol 51:1334–1336. https://doi.org/10.1128/JCM.03382-12
Graziani F, Pujol A, Nicoletti C, Dou S, Maresca M, Giardina T, Fons M, Perrier J (2016) Ruminococcus gnavus E1 modulates mucin expression and intestinal glycosylation. J Appl Microbiol 120:1403–1417. https://doi.org/10.1111/jam.13095
Lee JY, Arai H, Nakamura Y, Fukiya S, Wada M, Yokota A (2013) Contribution of the 7beta-hydroxysteroid dehydrogenase from Ruminococcus gnavus N53 to ursodeoxycholic acid formation in the human colon. J Lipid Res 54:3062–3069. https://doi.org/10.1194/jlr.M039834
Mohammed Saif M, Farid SF, Khaleel SA, Sabry NA, El-Sayed MH (2012) Hepatoprotective efficacy of ursodeoxycholic acid in pediatrics acute lymphoblastic leukemia. Pediatr Hematol Oncol 29:627–632. https://doi.org/10.3109/08880018.2012.713083
Dabard J, Bridonneau C, Phillipe C, Anglade P, Molle D, Nardi M, Ladire M, Girardin H, Marcille F, Gomez A, Fons M (2001) Ruminococcin A, a new lantibiotic produced by a Ruminococcus gnavus strain isolated from human feces. Appl Environ Microbiol 67:4111–4118
Yooseph S, Kirkness EF, Tran TM, Harkins DM, Jones MB, Torralba MG, O’Connell E, Nutman TB, Doumbo S, Doumbo OK, Traore B, Crompton PD, Nelson KE (2015) Stool microbiota composition is associated with the prospective risk of Plasmodium falciparum infection. BMC Genomics 16:631. https://doi.org/10.1186/s12864-015-1819-3
Caporaso JG, Lauber CL, Walters WA, Berg-Lyons D, Lozupone CA, Turnbaugh PJ, Fierer N, Knight R (2011) Global patterns of 16S rRNA diversity at a depth of millions of sequences per sample. Proc Natl Acad Sci U S A 108:4516–4522. https://doi.org/10.1073/pnas.1000080107
Turner S, Pryer KM, Miao VP, Palmer JD (1999) Investigating deep phylogenetic relationships among cyanobacteria and plastids by small subunit rRNA sequence analysis. J Eukaryot Microbiol 46:327–338
Kozich JJ, Westcott SL, Baxter NT, Highlander SK, Schloss PD (2013) Development of a dual-index sequencing strategy and curation pipeline for analyzing amplicon sequence data on the MiSeq Illumina sequencing platform. Appl Environ Microbiol 79:5112–5120. https://doi.org/10.1128/AEM.01043-13
Cox MP, Peterson DA, Biggs PJ (2010) SolexaQA: At-a-glance quality assessment of Illumina second-generation sequencing data. BMC Bioinforma 11:485. https://doi.org/10.1186/1471-2105-11-485
Schloss PD, Westcott SL, Ryabin T, Hall JR, Hartmann M, Hollister EB, Lesniewski RA, Oakley BB, Parks DH, Robinson CJ, Sahl JW, Stres B, Thallinger GG, Van Horn DJ, Weber CF (2009) Introducing mothur: open-source, platform-independent, community-supported software for describing and comparing microbial communities. Appl Environ Microbiol 75:7537–7541. https://doi.org/10.1128/AEM.01541-09
Quast C, Pruesse E, Yilmaz P, Gerken J, Schweer T, Yarza P, Peplies J, Glockner FO (2013) The SILVA ribosomal RNA gene database project: improved data processing and web-based tools. Nucleic Acids Res 41:D590–D596. https://doi.org/10.1093/nar/gks1219
McMurdie PJ, Holmes S (2013) phyloseq: an R package for reproducible interactive analysis and graphics of microbiome census data. PLoS One 8:e61217. https://doi.org/10.1371/journal.pone.0061217
Dehbi HM, Jones S, Sohaib SM, Finegold JA, Siggers JH, Stegemann B, Whinnett ZI, Francis DP (2015) A novel curve fitting method for AV optimisation of biventricular pacemakers. Physiol Meas 36:1889–1900. https://doi.org/10.1088/0967-3334/36/9/1889
Love MI, Huber W, Anders S (2014) Moderated estimation of fold change and dispersion for RNA-seq data with DESeq2. Genome Biol 15:550. https://doi.org/10.1186/s13059-014-0550-8
Untergasser A, Cutcutache I, Koressaar T, Ye J, Faircloth BC, Remm M, Rozen SG (2012) Primer3--new capabilities and interfaces. Nucleic Acids Res 40:e115. https://doi.org/10.1093/nar/gks596
Funding
This project was funded by Hyundai Motor America and Hyundai Hope on Wheels and J. Craig Venter Institute (JCVI).
Author information
Authors and Affiliations
Contributions
Managed study participant’s consent and sample collection: LS, KBZ. Performed experiments: SVR, YY, MT, KJM, BF, MT. Performed computational analysis: SVR, HS. Analyzed the data and provided input to the manuscript: SRV, HS, YY, KBZ, MT, BF, RP, LS, KEN. Wrote the paper: SVR, HS, KEN. Conceived, designed, and supervised: SVR, KEN, LS. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Human subject protocols along with consent forms were established. Written informed consent was obtained from a parent and/or legal guardian for all the study participants, and all methods were performed in accordance with the relevant guidelines and regulations.
Competing Interests
The authors declare that they have no competing interests.
Consent for Publication
Informed consent (and assent, where appropriate) and authorization to use, create, and disclose health information for research was obtained from and documented for each research participant enrolled to study at the Hyundai Cancer Institute at CHOC Children’s.
Ethics Approval and Consent to Participate
This study was reviewed and approved by the In-House Institutional Review Board at CHOC Children’s (protocol number 120555).
Electronic supplementary material
ESM 1
(DOCX 530 kb)
Rights and permissions
About this article
Cite this article
Rajagopala, S.V., Singh, H., Yu, Y. et al. Persistent Gut Microbial Dysbiosis in Children with Acute Lymphoblastic Leukemia (ALL) During Chemotherapy. Microb Ecol 79, 1034–1043 (2020). https://doi.org/10.1007/s00248-019-01448-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00248-019-01448-x