Abstract
Background
The magnetic resonance imaging (MRI) characteristics of evolving duodenal hematomas in children are unknown.
Objective
To describe the MRI changes exhibited by evolving duodenal hematomas and the likely mechanisms behind these changes.
Materials and methods
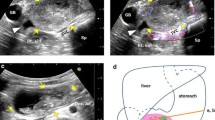
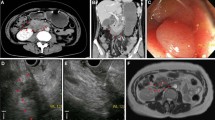
We retrospectively reviewed the MR features of intramural duodenal hematomas (6 lesions, 10 examinations) studied on a 1.5-T MR unit. All patients had clinical histories of blunt abdominal trauma or endoscopic procedures and we were able to determine the time interval between the onset and MR imaging. We evaluated and analyzed the appearance and signal intensity patterns of hematomas of varying ages and we compared the results with those in previously reported intracranial hematomas.
Results
The imaging appearances on five examinations were consistent with presence of deoxyhemoglobin. Two of these lesions were hypointense on T2-weighted images and iso- to hyperintense on T1-weighted images. Three had heterogeneous appearances on both T1- and T2-weighted images, and the bulk of the hematoma progressively increased in size and signal intensity on T2-weighted images. On the remaining five examinations, one lesion was hyperintense on T1-weighted images and iso- to hyperintense on T2-weighted images, consistent with intracellular methemoglobin, and four lesions were hyperintense on both T1- and T2-weighted images, consistent with the presence of extracellular methemoglobin. Duodenal hematoma stages were slower than those of intracranial hematomas; the acute stage spanned 2–7 days, and early and late subacute stages occurred 10–17 days after the injury.
Conclusion
Duodenal hematomas evolve like intracranial hematomas, but slower. Signal heterogeneity is common in the acute stage.





Similar content being viewed by others
References
Peterson ML, Abbas PI, Fallon SC et al (2015) Management of traumatic duodenal hematomas in children. J Surg Res 199:126–129
Hameed S, McHugh K, Shah N et al (2014) Duodenal haematoma following endoscopy as a marker of coagulopathy. Pediatr Radiol 44:392–397
Iuchtman M, Steiner T, Faierman T et al (2006) Post-traumatic intramural duodenal hematoma in children. Isr Med Assoc J 8:95–97
Chalela JA, Gomes J (2004) Magnetic resonance imaging in the evaluation of intracranial hemorrhage. Expert Rev Neurother 4:267–273
Bradley WG Jr (1993) MR appearance of hemorrhage in the brain. Radiology 189:15–26
Alemany Ripoll M, Stenborg A, Sonninen P et al (2004) Detection and appearance of intraparenchymal haematomas of the brain at 1.5 T with spin-echo, FLAIR and GE sequences: poor relationship to the age of the haematoma. Neuroradiology 46:435–443
Neumayer B, Hassler E, Petrovic A et al (2014) Age determination of soft tissue hematomas. NMR Biomed 27:1397–1402
Rubin JI, Gomori JM, Grossman RI et al (1987) High-field MR imaging of extracranial hematomas. AJR Am J Roentgenol 148:813–817
Yamashita Y, Hatanaka Y, Torashima M et al (1995) Magnetic resonance characteristics of intrapelvic haematomas. Br J Radiol 68:979–985
Hassler EM, Ogris K, Petrovic A et al (2015) Contrast of artificial subcutaneous hematomas in MRI over time. Int J Legal Med 129:317–324
Whang JS, Kolber M, Powell DK et al (2015) Diffusion-weighted signal patterns of intracranial haemorrhage. Clin Radiol 70:909–916
Hayman LA, Taber KH, Ford JJ et al (1991) Mechanisms of MR signal alteration by acute intracerebral blood: old concepts and new theories. AJNR Am J Neuroradiol 12:899–907
Bosman GJ, Werre JM, Willekens FL et al (2008) Erythrocyte ageing in vivo and in vitro: structural aspects and implications for transfusion. Transfus Med 18:335–347
Taber KH, Ford JJ, Jensen RS et al (1992) Change in red blood cell relaxation with hydration: application to MR imaging of hemorrhage. J Magn Reson Imaging 2:203–208
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Zhou, H., Ma, X., Sheng, M. et al. Evolution of intramural duodenal hematomas on magnetic resonance imaging. Pediatr Radiol 48, 1593–1599 (2018). https://doi.org/10.1007/s00247-018-4178-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-018-4178-9