Abstract
Background
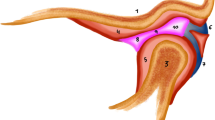
Juvenile idiopathic arthritis (JIA) has an incidence that ranges from 1 to 22 per 100,000 children worldwide, with involvement of the temporomandibular joint (TMJ) in 17–87% of patients. Intraarticular corticosteroid injections are beneficial in the local treatment of JIA and of other types of arthritis.
Objective
To describe and assess the accuracy of an US-guided technique for visualization of needle placement within the TMJ in children.
Materials and methods
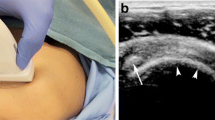
Between January 2000 and November 2007, 180 TMJ injections were performed during 116 encounters in 83 children with arthritis (71 girls, 12 boys; mean age 12.0 years). Access was obtained under sterile conditions using US guidance (linear 15-MHz or curvilinear 8-MHz transducers) in a coronal plane, and confirmed with CT. To minimize radiation, a limited focused CT protocol was developed.
Results
A bilateral injection was performed in 65 encounters (57%). Twenty-three children had repeat TMJ injections. All injections were performed using US guidance. CT confirmation was used in 127/180 TMJs (70%). In those confirmed with CT, the needle tip was intra-articular in 91% of cases. Triamcinolone hexacetonide was used in 92% of injections and triamcinolone acetonide in 8%. One major complication was encountered (skin atrophy at the injection site).
Conclusion
In our experience, TMJ injections using sonographic guidance is a safe, effective and accurate procedure.






Similar content being viewed by others
References
Weiss J, Ilowite N (2005) Juvenile idiopathic arthritis. Pediatr Clin N Am 52:413–442
Manners PJ, Bowers C (2002) Worldwide prevalence of juvenile arthritis: why does it vary so much? J Rheumatol 29:1520–1530
Haskes P, Laxer R (2005) Medical treatment of juvenile idiopathic arthritis. JAMA 294:1671–1684
Borchers A, Selmi C, Cheema G et al (2006) Juvenile idiopathic arthritis. Autoimmun Rev 5:279–298
Pedersen TK, Jensen JJ, Melsen B et al (2001) Resorption of the temporomandibular condylar bone according to subtypes of juvenile chronic arthritis. J Rheumatol 28:2109–2115
Arabshahi B, Dewitt EM, Cahill AM et al (2005) Utility of corticoesteroid injection for temporomandibular arthritis in children with juvenile idiopathic arthritis. Arthritis Rheum 52:3563–3569
Cleary AG, Murphy HD, Davidson JE (2003) Intraarticular corticosteroid injections in juvenile idiopathic arthritis. Arch Dis Child 88:192–196
Cahill AM, Baskin KM, Kaye RD et al (2007) CT-Guided percutaneous steroid injection for management of inflammatory arthropathy of the temporomandibular joint in children. AJR 188:182–186
Raza K, Lee CY, Pilling D et al (2003) Ultrasound guidance allows accurate needle placement and aspiration from small joints in patients with early inflammatory arthritis. Rheumatology 42:976–979
Grassi W, Lamanna G, Farina A et al (1999) Synovitis of small joints: sonography guided diagnostic and therapeutic approach. Ann Rheum Dis 58:595–597
Landes C, Walendzik H, Klein C (2000) Sonography of the temporomandibular joint from 60 examinations and comparison with MRI and axiography. J Craniomaxillofacial Surg 28:352–361
Patonay L, Nagy K, Engelke W (2002) Real-time endoarticular ultrasound imaging of the TMJ—a new diagnostic possibility? A cadaver study. Int J Oral Maxillofac Surg 31:553–557
SIR Quality Improvement Documents (2003) Quality improvement guidelines for the reporting and archiving of interventional radiology procedures. J Vasc Interv Radiol 14:S293–S295
Arabshahi B, Cron R (2006) Temporomandibular joint arthritis in juvenile idiopathic arthritis: the forgotten joint. Curr Opin Rheumatol 18:490–495
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Parra, D.A., Chan, M., Krishnamurthy, G. et al. Use and accuracy of US guidance for image-guided injections of the temporomandibular joints in children with arthritis. Pediatr Radiol 40, 1498–1504 (2010). https://doi.org/10.1007/s00247-010-1581-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-010-1581-2