Abstract
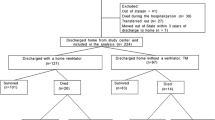
Neonates who require surgery for congenital heart disease (CHD) frequently have difficulty with oral feeds post-operatively and may require a feeding tube at hospital discharge. The purpose of this study was to determine the effect of oral or nasal intubation route on feeding method at hospital discharge. This was a non-blinded randomized control trial of 62 neonates who underwent surgery for CHD between 2018 and 2021. Infants in the nasal (25 patients) and oral (37 patients) groups were similar in terms of pre-operative risk factors for feeding difficulties including completed weeks of gestational age at birth (39 vs 38 weeks), birthweight (3530 vs 3100 g), pre-operative PO intake (92% vs 81%), and rate of pre-operative intubation (22% vs 28%). Surgical risk factors were also similar including Society of Thoracic Surgeons-European Association for Cardio-Thoracic Surgery category (3.9 vs 4.1), shunt placement (32% vs 41%), cardiopulmonary bypass time (181 vs 177 min), and cross-clamp time (111 vs 105 min). 96% of nasally intubated patients took full oral feeds by discharge as compared with 78% of orally intubated infants (p = 0.05). Nasally intubated infants reach full oral feeds an average of 3 days earlier than their orally intubated peers. In this cohort of patients, nasally intubated infants reach oral feeds more quickly and are less likely to require supplemental tube feeding in comparison to orally intubated peers. Intubation route is a potential modifiable risk factor for oral aversion and appears safe in neonates. The study was approved by the University of Virginia Institutional Review Board for Health Sciences Research and was retrospectively registered on clinicaltrials.gov (NCT05378685) on May 18, 2022.

Similar content being viewed by others
References
Piggott KD, Babb J, Yong S et al (2018) Risk factors for gastrostomy tube placement in single ventricle patients following the norwood procedure. Semin Thorac Cardiovasc Surg 30(4):443–447. https://doi.org/10.1053/j.semtcvs.2018.02.012
Goldstein SA, Watkins KJ, Lowery RE et al (2022) Oral aversion in infants with congenital heart disease: a single-center retrospective cohort study. Pediatr Crit Care Med 23(3):e171–e179. https://doi.org/10.1097/PCC.0000000000002879
Kogon BE, Ramaswamy V, Todd K et al (2007) Feeding difficulty in newborns following congenital heart surgery. Congenit Heart Dis 2(5):332–337. https://doi.org/10.1111/j.1747-0803.2007.00121.x
Christian CE, Thompson NE, Wakeham MK (2020) Use and outcomes of nasotracheal intubation among patients requiring mechanical ventilation across U.S. PICUs. Pediatr Crit Care Med 21(7):620–624. https://doi.org/10.1097/PCC.0000000000002267
Greene NH, Jooste EH, Thibault DP et al (2019) A study of practice behavior for endotracheal intubation site for children with congenital heart disease undergoing surgery: impact of endotracheal intubation site on perioperative outcomes—an analysis of the Society of Thoracic Surgeons Congenital Cardiac Anesthesia Society database. Anesth Analg 129(4):1061–1068. https://doi.org/10.1213/ANE.0000000000003594
Pinelli J, Symington A (2000) Non-nutritive sucking for promoting physiologic stability and nutrition in preterm infants. Cochrane Database Syst Rev 2:1071. doi:https://doi.org/10.1002/14651858.CD001071
Schulz KF, Altman DG, Moher D, CONSORT Group (2010) CONSORT 2010 statement: updated guidelines for reporting parallel group randomised trials. BMJ 340:c332. https://doi.org/10.1136/bmj.c332 (Published 2010 Mar 23)
The Society of Thoracic Surgeons—European Association for Cardio-Thoracic Surgery Congenital Heart Surgery Mortality Categories (STAT Mortality Categories). June 24, 2020. https://www.sts.org/sites/default/files/CHSD%20Appendix%20C%20-%20STAT%20Categories.pdf
Haughey BS, Dean P, Spaeder MC, Smith CJ, Conaway M, White SC (2022) Gastrostomy tube placement in congenital cardiac surgery: a multi-institutional database study. Cardiol Young 3:1–6. https://doi.org/10.1017/S1047951122003079
Marietta J, Glotzbach KL, Jones CE et al (2022) Assessing the impact of nasotracheal intubation on postoperative neonates with congenital heart disease: a quality improvement project at a single heart center. Pediatr Crit Care Med 23(7):e338–e346 (published online ahead of print, 2022 Apr 19).
Skinner ML, Halstead LA, Rubinstein CS, Atz AM, Andrews D, Bradley SM (2005) Laryngopharyngeal dysfunction after the Norwood procedure. J Thorac Cardiovasc Surg 130(5):1293–1301. https://doi.org/10.1016/j.jtcvs.2005.07.013
Hehir DA, Easley RB, Byrnes J (2016) Noncardiac challenges in the cardiac ICU: feeding, growth and gastrointestinal complications, anticoagulation, and analgesia. World J Pediatr Congenit Heart Surg 7(2):199–209. https://doi.org/10.1177/2150135115615847
Elgersma KM, Trebilcock AL, Whipple MO, Tanner LR, Pilditch SJ, Shah KM, McKechnie AC (2023) Risk factors for tube feeding at discharge in infants undergoing neonatal surgery for congenital heart disease: a systematic review. Pediatr Cardiol 44(4):769–794. https://doi.org/10.1007/s00246-022-03049-x. (Epub 2022 Nov 21 PMID: 36404346)
Spence K, Barr P (2000) Nasal versus oral intubation for mechanical ventilation of newborn infants. Cochrane Database Syst Rev 1999(2):CD000948. https://doi.org/10.1002/14651858.CD000948
Xue FS, Liao X, Liu KP et al (2007) The circulatory responses to tracheal intubation in children: a comparison of the oral and nasal routes. Anaesthesia 62(3):220–226. https://doi.org/10.1111/j.1365-2044.2007.04939.x
Kumar V, Angurana SK, Baranwal AK, Nallasamy K (2021) Nasotracheal vs. orotracheal intubation and post-extubation airway obstruction in critically ill children: an open-label randomized controlled trial. Front Pediatr 9:713516. Published 2021 Sep 16. doi:https://doi.org/10.3389/fped.2021.713516
Chen J, Chen J, Yang J, Chen Y, Liang Y, Lin Y (2020) Investigating the efficacy of hydrocolloid dressing for preventing nasotracheal tube-related pressure injury in the PICU. Pediatr Crit Care Med 21(9):e752–e758. https://doi.org/10.1097/PCC.0000000000002494
Censoplano NM, Barrett CS, Ing RJ, Reichert K, Rannie M, Kaufman J (2020) Achieving sustainability in reducing unplanned extubations in a pediatric cardiac ICU. Pediatr Crit Care Med 21(4):350–356. https://doi.org/10.1097/PCC.0000000000002193
Author information
Authors and Affiliations
Contributions
MY and DF: designed and led the study including subject recruitment and randomization, data collection, analysis, and drafting of the manuscript. MS: performed statistical analysis and contributed to drafting and editing of the manuscript, particularly the introduction and discussion. RC and LF: helped with study design and were essential to subject recruitment. BC, SH, PM, JR, RS, SV, AW: performed all intubations and contributed to safety observations and discussion. All authors reviewed and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yildirim, M.I., Spaeder, M.C., Castro, B.A. et al. The Impact of Nasal Intubation on Feeding Outcomes in Neonates Requiring Cardiac Surgery: A Randomized Control Trial. Pediatr Cardiol 45, 426–432 (2024). https://doi.org/10.1007/s00246-023-03322-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-023-03322-7