Abstract
Mid-systolic notching (MSN) of the pulmonary valve Doppler signal represents a reflected systolic pressure wave from the pulmonary vasculature and is often seen in pulmonary hypertension (PH). We hypothesize that MSN is associated with a higher pulmonary vascular resistance (PVR) and mean pulmonary artery pressure (mPAP), and a diagnosis of PH in pediatric patients. This was a retrospective study of patients ≤ 18 years who had an echocardiogram obtained ≤ 30 days before catheterization for suspected PH. MSN was defined as an indentation in the initial two thirds of the systolic Doppler signal. PH was defined as mPAP > 20 mmHg and PVR ≥ 3.0 Wu m2. Subgroups (MSN vs. normal) were compared. Receiver operator characteristic determined a continuous variable’s discriminatory ability for a diagnosis of PH. Reproducibility of MSN was assessed. In total, 90 patients (73 with congenital heart disease) were included, of which 36 had MSN and 54 were normal. MSN patients were more likely to have PH, and had significantly higher mPAP, PVR, and lower pulmonary stroke volume. The presence of MSN had good discriminatory ability for PH diagnosis. The presence of MSN had high specificity (96%) for PH, whereas sensitivity was lower (54%). Reproducibility was 100% for MSN. MSN is a simple, highly reproducible echocardiographic metric associated with higher mPAP and PVR. When present, there is a high likelihood a diagnosis of PH confirmed by catheterization. Incorporation of MSN into imaging protocols may be useful. MSN appears worthy of further investigation in pediatric patients with suspected PH.


Similar content being viewed by others
References
Ivy DD, Abman SH, Barst RJ et al (2013) Pediatric pulmonary hypertension. J Am Coll Cardiol 24:117–126
Rosensweig EB, Abman SH, Adatia I et al (2019) Paediatric pulmonary arterial hypertension: updates on definition, classification, diagnostics, and management. Eur Respir J 53:1801916
Lammers AE, Apitz C, Michel-Behnke I, Koestenberger M (2021) A guide to echocardiographic assessment in children and adolescents with pulmonary hypertension. Cardiovasc Diagn Ther 11(4):1160–1177
Mourani PM, Sontag MK, Younoszai A, Ivy DD, Abman SH (2008) Clinical utility of echocardiograph for the diagnosis and management of pulmonary vascular disease in young children with chronic lung disease. Pediatrics 121:317–325
Levy PT, Patel MD, Groh G et al (2016) Pulmonary artery acceleration time provides a reliable estimate of invasive pulmonary hemodynamics in children. J Am Soc Echocardiogr 29(11):1056–1065
Koestenberger M, Apitz C, Abdul-Khaliq H, Hansmann G (2016) Transthoracic echocardiography for the evaluation of children and adolescents with suspected or confirmed pulmonary hypertension. Heart 102:ii14–ii22
Jone P, Schäfer M, Li L, Craft M, Ivy DD, Kutty S (2017) Right atrial deformation in predicting outcomes in pediatric pulmonary hypertension. Circ Cardiovasc Imaging 10(12):e006250
Jone PN, Schäfer M, Pan Z, Ivy DD (2019) Right ventricular-arterial coupling ratio derived from 3-dimensional echocardiography predicts outcomes in pediatric pulmonary hypertension. Circ Cardiovasc Imaging 12:e008176
Weyman AE, Dillon JC, Feigenbaum H, Chang S (1974) Echocardiographic pattern of pulmonary valve motion with pulmonary hypertension. Circulation 50:905–910
Parker MW, Gottbrecht MF, Aurigemma GP (2021) Midsystolic notch and pulmonary hypertension: pathophysiologic mechanism and technical considerations. J Am Soc Echocardiogr 34:693–695
Skinner GJ (2017) Echocardiographic assessment of pulmonary arterial hypertension for pediatricians and neonatologists. Front Pediatr 5:168
Hinderliter AL, Willis PW, Long WA et al (2003) Frequency and severity of tricuspid regurgitation determined by Doppler echocardiography in primary pulmonary hypertension. Am J Cardiol 91:1033–1037
Espejo JC, de Soto JS, Camacho G, Laureano RC, Montero JG, Senorans AD (1995) Evaluation of pulmonary hypertension by Doppler echocardiography in children. Rev Esp Cardiol 48:122–127
Kitabatake A, Inoue M, Asao M et al (1983) Noninvasive evaluation of pulmonary hypertension by a pulsed Doppler technique. Circulation 2:302–309
Takahama H, McCully RB, Frantz RP, Kane GC (2017) Unraveling the RV ejection Doppler envelope. JACC Cardiovasc Imaging 10:1268–1277
Chiba Y, Iwano H, Murayama M et al (2021) Presence and relevance of midsystolic notching on right ventricular outflow tract flow velocity envelopes in pulmonary hypertension due to heart failure. J Am Soc Echocardiogr 34:690–692
Nijres BM, Bokowski J, Mubayed L et al (2020) Utility of pulmonary artery acceleration time to estimate systolic pulmonary artery pressure in neonates and young infants. Pediatr Cardiol 41(2):265–271
Abman SH, Hansmann G, Archer SL et al (2015) Pediatric pulmonary hypertension: guidelines form the American Heart Association and American Thoracic Society. Circulation 132:2037–2099
Baumgartner H, De Backer J, Babu-Narayan SV et al (2021) 2020 ESC guidelines for the management of adult congenital heart disease. Eur Heart J 42:563–645
Humbert M, Kovacs G, Hoeper MM et al (2022) 2022 ESC/ERS guidelines for the diagnosis and treatment of pulmonary hypertension. Eur Heart J 32:3618–3731
Author information
Authors and Affiliations
Contributions
All of the co-authors made substantial contributions to this work. RWL, CT, FO, and AD were involved in the conception and design of the study. RWL and CT were involved in the data collection and analysis. All co-authors contributed to the interpretation of data. RWL was responsible for drafting and organizing the manuscript. All co-authors contributed to the revision of the manuscript, approved the submitted form, and are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file2 (DOCX 48 kb)
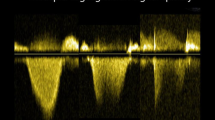
Supplemental Figure 1. Pulmonary valve pulse wave Doppler tracings for the same patient at two different time points. Figure on the left demonstrates a normal systolic Doppler signal, while the rightward figure demonstrates new notching of the Doppler signal.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Loar, R.W., Tsao, C., Ogunyankin, F. et al. Mid-Systolic Notching of the Pulmonary Valve Doppler Signal is Highly Associated with Pulmonary Hypertension. Pediatr Cardiol 44, 1667–1673 (2023). https://doi.org/10.1007/s00246-023-03285-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-023-03285-9