Abstract
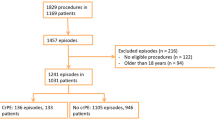
Pericardial effusion (PE) after cardiac surgery can be life threatening without timely detection, and the optimal screening method is unknown. We sought to evaluate the role of a surveillance echocardiogram on postoperative day 10 (± 2), determine the incidence of postoperative PE, and identify risk factors. We conducted a retrospective cohort study including all pediatric patients who underwent open heart surgery at a single institution over a 7-month period. To identify risk factors for PE, medical records of patients with PE detected within 6 weeks after surgery (cases) were compared with patients without PE (controls). Of 203 patients, 52 (26%) had PE within 6 weeks; 42 (81%) were trivial-small and 10 (19%) were moderate-large. Twenty-nine (56%) were first detected within 7 days post-operatively, including all cases developing cardiac tamponade (n = 3). An echocardiogram was done 10 (± 2) days post-operatively in 41/52 cases, of which 12/41 (29%) did not have a PE at this time, 24/41 (59%) had a trivial-small PE, and 5/41(12%) had a moderate-large PE; 2 of the latter had no prior detected PE. Closure of an atrial septal defect had the highest incidence of PE (42%). PE cases were associated with postoperative nasopharyngeal detection of a respiratory virus (OR 3.8, p = 0.03). In conclusion, the majority of PE cases were detected within 7 days post-operatively, including all cases subsequently developing cardiac tamponade. Day 10 echocardiography infrequently detected a moderate or large effusion that had previously gone undiagnosed. A positive perioperative nasopharyngeal aspirate for a respiratory virus was associated with postoperative PE.



Similar content being viewed by others
Data Availability
Data is available upon request.
References
Weitzmam LBTW, Kronzon I, Cohen ML, Glassman E, Spencer FC (1984) The incidence and natural history of pericardial effusion after cardiac surgery. Echocardiogr Study Circ 69:506–511
Clapp SK, Garson A Jr, Gutgesell HP, Cooley DA, McNamara DG (1980) Postoperative pericardial effusion and its relation to postpericardiotomy syndrome. Pediatrics 66(4):585–588
Stevenson LW, Child JS, Laks H, Kern L (1984) Incidence and significance of early pericardial effusions after cardiac surgery. Am J Cardiol 54(7):848–851
Beland MJ, Paquet M, Gibbons JE, Tchervenkov CI, Dobell AR (1990) Pericardial effusion after cardiac surgery in children and effects of aspirin for prevention. Am J Cardiol 65(18):1238–1241
Pastorek JS, Allen HD, Davis JT (1994) Current outcomes of surgical closure of secundum atrial septal defect. Am J Cardiol 74(1):75–77
Pepi M, Muratori M, Barbier P et al (1994) Pericardial effusion after cardiac surgery: incidence, site, size, and haemodynamic consequences. Heart 72(4):327–331
Prabhu AS, Ross RD, Heinert MR, Walters HL, Hakimi M (1996) Decreased incidence of postoperative pericardial effusions after cardiac surgery for congenital heart disease. Am J Cardiol 77(9):774–6
Yip AS, Chau EM, Chow WH, Kwok OH, Cheung KL (1997) Pericardial effusion in adults undergoing surgical repair of atrial septal defect. Am J Cardiol 79(12):1706–1708
Atik E, Ikari NM, Martins TC, Barbero-Marcial M (2002) Fontan operation and the cavopulmonary technique: immediate and late results according to the presence of atrial fenestration. Arq Bras Cardiol 78(2):162–166
Baskett RJF, Tancock E, Ross DB (2003) The gold standard for atrial septal defect closure: current surgical results, with an emphasis on morbidity. Pediatr Cardiol 24(5):444–447
Cheung EWY, Ho SA, Tang KKY, Chau AKT, Chiu CSW, Cheung YF (2003) Pericardial effusion after open heart surgery for congenital heart disease. Heart 89(7):780–783
Gill PJ, Forbes K, Coe JY (2009) The effect of short-term prophylactic acetylsalicylic acid on the incidence of postpericardiotomy syndrome after surgical closure of atrial septal defects. Pediatr Cardiol 30(8):1061–1067. https://doi.org/10.1007/s00246-009-9495-1
Adrichem R, Le Cessie S, Hazekamp MG et al (2019) Risk of clinically relevant pericardial effusion after pediatric cardiac surgery. Pediatr Cardiol 40(3):585–594. https://doi.org/10.1007/s00246-018-2031-4
Tsang TS, Barnes ME, Hayes SN et al (1999) 1979 Clinical and echocardiographic characteristics of significant pericardial effusions following cardiothoracic surgery and outcomes of echo-guided pericardiocentesis for management: mayo clinic experience. Chest 116(2):322–31
Khan NK, Jarvela KM, Loisa EL, Sutinen JA, Laurikka JO, Khan JA (2017) Incidence, presentation and risk factors of late postoperative pericardial effusions requiring invasive treatment after cardiac surgery. Interact Cardiovasc Thorac Surg 24(6):835–840. https://doi.org/10.1093/icvts/ivx011
Ashikhmina EA, Schaff HV, Sinak LJ et al (2010) Pericardial effusion after cardiac surgery: risk factors, patient profiles, and contemporary management. Ann Thorac Surg 89(1):112–118. https://doi.org/10.1016/j.athoracsur.2009.09.026
Shoiab I, Danford DA, Li L, Abdullah I, Hammel JM, Kutty S (2015) Predischarge transthoracic echocardiography after surgery for congenital heart disease: a routine with a reason? J Am Soc Echocardiogr 28(9):1030–1035. https://doi.org/10.1016/j.echo.2015.04.009
Cantinotti M, Spadoni I, Assanta N et al (2014) Controversies in the prophylaxis and treatment of postsurgical pericardial syndromes: a critical review with a special emphasis on paediatric age. J Cardiovasc Med 15(12):847–854. https://doi.org/10.2459/JCM.0b013e328362c5b5
Kuvin JT, Harati NA, Pandian NG, Bojar RM, Khabbaz KR (2002) Postoperative cardiac tamponade in the modern surgical era. Ann Thorac Surg 74(4):1148–1153
Bocsi J, Hambsch J, Osmancik P, Schneider P, Valet G, Tarnok A (2002) Preoperative prediction of pediatric patients with effusions and edema following cardiopulmonary bypass surgery by serological and routine laboratory data. Crit Care 6(3):226–233
Hauptman PJ, Couper GS, Aranki SF, Kartashov A, Mudge GH Jr, Loh E (1994) Pericardial effusions after cardiac transplantation. J Am Coll Cardiol 23(7):1625–1629
Malouf JF, Alam S, Gharzeddine W, Stefadouros MA (1993) The role of anticoagulation in the development of pericardial effusion and late tamponade after cardiac surgery. Eur Heart J 14(11):1451–7
Angelini GD, Penny WJ, el-Ghamary F, et al (1987) The incidence and significance of early pericardial effusion after open heart surgery. Eur J Cardio-Thorac Surg 1(3):165–168
Elias MD, Glatz AC, O’Connor MJ et al (2017) Prevalence and risk factors for pericardial effusions requiring readmission after pediatric cardiac surgery. Pediatr Cardiol 38(3):484–494. https://doi.org/10.1007/s00246-016-1540-2
Kirkpatrick E, Hurwitz R, Brown J (2008) A single center’s experience with the Ross procedure in pediatrics. Pediatr Cardiol 29(5):894–900. https://doi.org/10.1007/s00246-008-9224-1
Bortolotti U, Livi U, Frugoni C et al (1981) Delayed cardiac tamponade following open heart surgery. Analysis of 12 patients. Thorac Cardiovasc Surg 29(4):233–236
Dziadulewicz L, Shannon-Stone M (1995) Postpericardiotomy syndrome: a complication of cardiac surgery. AACN Clin Issues 6(3):464–470
Engle MA, Klein AA, Hepner S, Ehlers KH (1976) The postpericardiotomy and similar syndromes. Cardiovasc Clin 7(3):211–217
Bocsi J, Richter M, Hambsch J et al (2006) Transient Th1/Th2 disbalance indicates postoperative effusions and edema after cardiopulmonary bypass in children. Cytom Part A 69(3):165–168
Tarnok A, Bocsi J, Pipek M et al (2001) Preoperative prediction of postoperative edema and effusion in pediatric cardiac surgery by altered antigen expression patterns on granulocytes and monocytes. Cytometry 46(4):247–253
Funding
Dr. Galante was funded by a Women and Children’s Health Research Institute Trainee Grant, and by an American Academy of Pediatrics Resident Research Grant.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare that they have no conflict of interest.
Ethical Approval
Health Research Ethics Board, University of Alberta (Pro00022477_REN5).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Galante, G.J., Schantz, D.I., Myers, K.A. et al. Echocardiographic Screening for Postoperative Pericardial Effusion in Children. Pediatr Cardiol 42, 1531–1538 (2021). https://doi.org/10.1007/s00246-021-02637-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-021-02637-7