Abstract
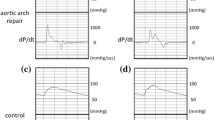
One of the most important problems in patients with aortic coarctation after aortic arch repair is future cardiovascular disease. We have previously reported that the enhancement of aortic pressure wave reflection in patients could be one of the causes of future cardiovascular diseases, because it results in an increase of the left ventricular workload and is disadvantageous for coronary circulation. Seventeen patients who had undergone aortic arch repair without pressure gradient in their aortic arch were enrolled. An ascending aortic pressure waveform was recorded by a pressure-sensor-mounted catheter, and a subendocardial viability ratio, which measures cardiac blood supply–workload balance, was calculated. The values were compared with those in age-matched controls. The patients’ mean age was 6.8 ± 2.8 years. The mean ascending aortic systolic pressure was higher (100.4 ± 12.9 vs. 90.2 ± 8.9 mmHg, p = 0.0011) and the pulse pressure was wider (38.1 ± 7.1 vs. 32.5 ± 5.4 mmHg, p = 0.0072) in patients than in control subjects. There was no difference in the mean subendocardial viability ratio (1.01 ± 0.25 vs. 1.01 ± 0.24, ns), while the mean tension time index (27.4 ± 5.6 vs. 23.0 ± 3.3, p = 0.0001) and diastolic pressure time index (28.4 ± 11.1 vs. 23.6 ± 8.0, p = 0.0082) were higher in patients than in controls. The cardiac blood supply–workload balance was preserved in patients after aortic arch repair, despite an increase in their cardiac workload.

Similar content being viewed by others
References
Presbitero P, Demarie D, Villani M, Perinetto EA, Riva G, Orzan F, Bobbio M, Morea M, Brusca A (1987) Long term results (15-30 years) of surgical repair of aortic coarctation. Br Heart J 57:462–467
Stewart AB, Ahmed R, Travill CM, Newman CG (1993) Coarctation of the aorta life and health 20-44 years after surgical repair. Br Heart J 69:65–70
Jenkins NP, Ward C (1999) Coarctation of the aorta: natural history and outcome after surgical treatment. QJM 92:365–371
Cohen M, Fuster V, Steele PM, Driscoll D, McGoon DC (1989) Coarctation of the aorta. Long-term follow-up and prediction of outcome after surgical correction. Circulation 80:840–845
Daniels SR (2001) Repair of coarctation of the aorta and hypertension: does age matter. Lancet 358:89
Lee MGY, Allen SL, Kawasaki R, Kotevski A, Koleff J, Kowalski R, Cheung MM, Konstantinov IE, Brizard CP, d’Udekem Y (2015) High prevalence of hypertension and end-organ damage late after coarctation repair in normal arches. Ann Thorac Surg 100:647–653
Celermajer DS, Greaves K (2002) Survivors of coarctation repair: fixed but not cured. Heart 88:113–114
Toro-Salazar OH, Steinberger J, Thomas W, Rocchini AP, Carpenter B, Moller JH (2002) Long-term follow-up of patients after coarctation of the aorta repair. Am J Cardiol 89:541–547
O’Sullivan JJ, Derrick G, Darnell R (2002) Prevalence of hypertension in children after early repair of coarctation of the aorta: a cohort study using casual and 24 hour blood pressure measurement. Heart 88:163–166
Murakami T, Takeda A (2005) Enhanced aortic pressure wave reflection in patients after repair of aortic coarctation. Ann Thorac Surg 80:995–999
Murakami T, Takeda A, Takei K, Ueno M, Yakuwa S, Yamazawa H, Furukawa T (2010) Aortic pressure wave reflection in children. Hypertens Res 33:225–228
Murakami T, Takeda A, Takei K, Tateno S, Kawasoe Y, Niwa K (2015) The cardiac blood supply-workload balance in children. Heart Vessels 30:626–631
Buckberg GD, Fixler DE, Archie JP, Hoffman JI (1972) Experimental subendocardial ischemia in dogs with normal coronary arteries. Circ Res 30:67–81
Buckberg GD, Olinger GN, Mulder DG, Maloney JV (1975) Depressed postoperative cardiac performance. Prevention by adequate myocardial protection during cardiopulmonary bypass. J Thorac Cardiovasc Surg 70:974–994
Hoffman JIE, Buckberg GD (2014) The myocardial oxygen supply: demand index revisited. J AM Heart Assoc 3:e000285
Murakami T, Takei K, Ueno M, Takeda A, Satoshi Y, Nakazawa M (2008) Aortic reservoir function after arterial switch operation in elementary school-aged children. Circ J 72:1291–1295
Di Micco L, Salvi P, Bellasi A, Sirico ML, Di Iorio B (2013) Subendocardial viability ratio predicts cardiovascular mortality in chronic kidney disease patients. Blood Purif 36:26–28
Vizinho RS, Santos C, Lucas C, Adragao T, Barata JD (2014) Effect of the arteriovenous access for hemodialysis on subendocardial viability ratio, pulse pressure and hospitalizations. J Nephrol 27:563–570
Theilade S, Hansen TW, Rossing P (2014) Central hemodynamics are associated with cardiovascular disease and albuminuria in type 1 diabetes. Am J Hypertens 27:1152–1159
Saiki H, Kuwata S, Kurishima C, Masutani S, Senzaki H (2016) Vulnerability of coronary circulation after Norwood operation. Ann Thorac Surg 101:1544–1551
Laugesen E, Hoyem P, Fleischer J, Kumarathas I, Knudsen ST, Hansen KW, Christiansen JS, Hansen TK, Poulsen PL (2016) Reduced subendocardial viability ratio is associated with unfavorable cardiovascular risk profile in women with short duration of type 2 diabetes. Am J Hypertens 29:1165–1172
Lombardi KC, Northrup V, McNamara RL, Sugeng L, Weismann CG (2013) Aortic stiffness and left ventricular diastolic function in children following early repair of aortic coarctation. Am J Cardiol 112:1828–1833
Kuhn A, Baumgartner D, Baumgartner C, Horer J, Schreiber C, Hess J, Vogt M (2009) Impaired elastic properties of the ascending aorta persist within the first 3 years after neonatal coarctation repair. Pediatr Cardiol 30:46–51
Ou P, Celermajer DS, Jolivet O, Buyens F, Herment A, Sidi D, Bonnet D, Mousseaux E (2008) Increased central aortic stiffness and left ventricular mass in normotensive young subjects after successful coarctation repair. Am Heart J 155:187–193
Vitarelli A, Conde Y, Cimino E, D’Orazio S, Stellato S, Battaglia D, Padella V, Caranci F, Continanza G, Dettori O, Capotosto L (2008) Assessment of ascending aorta distensibility after successful coarctation repair by strain Doppler echocardiography. J Am Soc Echocardiogr 21:729–736
Voges I, Kees J, Jerosch-Herold M, Gottschalk H, Trentmann J, Hart C, Gabbert DD, Pardun E, Pham M, Andrade AC, Wegner P, Kristo I, Jansen O, Kramer HH, Rickers C (2016) Aortic stiffening and its impact on left atrial volumes and function in patients after successful coarctation repair: a multiparametric cardiovascular magnetic resonance study. J Cardiovasc Magn Reson 18:56
Rinnstrom D, Dellborg M, Thilen U, Sorensson P, Nielsen N-E, Christersson C, Johansson B (2016) Left ventricular hypertrophy in adults with previous repair of coarctation of the aorta; association with systolic blood pressure in the high normal range. Int J Cardiol 218:59–64
Murakami T, Takeda A, Yamazawa H, Tateno S, Kawasoe Y, Niwa K (2013) Aortic pressure wave reflection in patients after successful aortic arch repair in early infancy. Hypertens Res 36:603–607
Yamazawa H, Murakami T, Takeda A, Takei K, Furukawa T, Nakajima H (2015) Serum concentration of procollagen type III amino-terminal peptide is increased in patients with successfully repaired coarctation of the aorta with left ventricular hypertrophy. Pediatr Cardiol 36:555–560
Czernin J, Müller P, Chan S, Brunken RC, Porenta G, Krivokapich J, Chen K, Chan A, Phelps ME, Schelbert HR (1993) Influence of age and hemodynamics on myocardial blood flow and flow reserve. Circulation 88:62–69
Hauser M, Bengel FM, Kühn A, Sauer U, Zylla S, Braun SL, Nekolla SG, Oberhoffer R, Lange R, Schwaiger M, Hess J (2001) Myocardial blood flow and flow reserve after coronary reimplantation in patients after arterial switch and Ross operation. Circulation 103:1875–1880
Acknowledgement
We thank Ashraf Malhas, PhD, from Edanz Group for editing a draft of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Rights and permissions
About this article
Cite this article
Murakami, T., Takeda, A. Preserved Cardiac Blood Supply–Workload Balance in Pediatric Patients After Aortic Arch Repair. Pediatr Cardiol 39, 294–298 (2018). https://doi.org/10.1007/s00246-017-1754-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-017-1754-y