Abstract
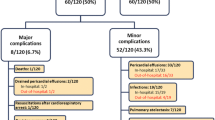
Interventional cardiac catheterization in children and adolescents is traditionally performed with the patient under general anesthesia and endotracheal intubation. However, percutaneous closure of atrial septum defect (ASD) without general anaesthesia is currently being attempted in a growing number of children. The study objective was to evaluate the success and complication rate of percutaneous ASD closure in spontaneously breathing children under deep sedation. Retrospective single centre cohort study of consecutive children undergoing percutaneous ASD closure at a tertiary care pediatric cardiology centre. Transesophageal echocardiography (TEE) and percutaneous ASD closure were performed with the patient under deep sedation with intravenous bolus of midazolam and ketamine for induction and propofol continuous infusion for maintenance of sedation in spontaneously breathing children. One hundred and ninety-seven patients (median age 6.1 years [minimum 0.5; maximum 18.8]) underwent TEE and ASD balloon sizing. Percutaneous ASD closure was attempted in 174 patients (88 %), and device implantation was performed successfully in 92 %. To achieve sufficient deep sedation, patients received a median ketamine dose of 2.7 mg/kg (0.3; 7) followed by a median propofol continuous infusion rate of 5 mg/kg/h (1.1; 10.7). There were no major cardiorespiratory complications associated with deep sedation, and only two patients (1 %) required endotracheal intubation due to bronchial obstruction immediately after induction of sedation. Seventeen patients (8 %) had minor respiratory complications and required frequent oral suctioning or temporary bag-mask ventilation. TEE and percutaneous ASD closure can be performed safely and successfully under deep sedation in spontaneously breathing children of all ages.


Similar content being viewed by others
References
Akin A, Esmaoglu A, Guler G, Demircioglu R, Narin N, Boyaci A (2005) Propofol and propofol-ketamine in pediatric patients undergoing cardiac catheterization. Pediatr Cardiol 26(5):553–557
American Academy of Pediatrics (2002) Guidelines for monitoring and management of pediatric patients during and after sedation for diagnostic and therapeutic procedures: addendum. Pediatrics 110(4):836–838
American Academy of Pediatrics Committee on Drugs (1992) Guidelines for monitoring and management of pediatric patients during and after sedation for diagnostic and therapeutic procedures. Pediatrics 89(6 Pt 1):1110–1115
American Society of Anesthesiologists, Task Force on Sedation and Analgesia by Non-Anesthesiologists (2002) Practice guidelines for sedation and analgesia by non-anesthesiologists. Anesthesiology 96(4):1004–1017
Amundsen LB, Artru AA, Dager SR, Shaw DW, Friedman S, Sparks B et al (2005) Propofol sedation for longitudinal pediatric neuroimaging research. J Neurosurg Anesthesiol 17(4):180–192
Anderson JL, Junkins E, Pribble C, Guenther E (2007) Capnography and depth of sedation during propofol sedation in children. Ann Emerg Med 49(1):9–13
Barbi E, Gerarduzzi T, Marchetti F, Neri E, Verucci E, Bruno I et al (2003) Deep sedation with propofol by nonanesthesiologists: a prospective pediatric experience. Arch Pediatr Adolesc Med 157(11):1097–1103
Barbi E, Petaros P, Badina L, Pahor T, Giuseppin I, Biasotto E et al (2006) Deep sedation with propofol for upper gastrointestinal endoscopy in children, administered by specially trained pediatricians: a prospective case series with emphasis on side effects. Endoscopy 38(4):368–375
Bassett KE, Anderson JL, Pribble CG, Guenther E (2003) Propofol for procedural sedation in children in the emergency department. Ann Emerg Med 42(6):773–782
Berkenbosch JW, Graff GR, Stark JM, Ner Z, Tobias JD (2004) Use of a remifentanil-propofol mixture for pediatric flexible fiberoptic bronchoscopy sedation. Paediatr Anaesth 14(11):941–946
Buehrer S, Immoos S, Frei M, Timmermann B, Weiss M (2007) Evaluation of propofol for repeated prolonged deep sedation in children undergoing proton radiation therapy. Br J Anaesth 99(4):556–560
Butera G, Lucente M, Rosti L, Chessa M, Micheletti A, Giamberti A et al (2007) A comparison between the early and mid-term results of surgical as opposed to percutaneous closure of defects in the oval fossa in children aged less than 6 years. Cardiol Young 17(1):35–41
Butera G, Romagnoli E, Carminati M, Chessa M, Piazza L, Negura D et al (2008) Treatment of isolated secundum atrial septal defects: impact of age and defect morphology in 1,013 consecutive patients. Am Heart J 156(4):706–712
Cardenas L, Panzer J, Boshoff D, Malekzadeh-Milani S, Ovaert C (2007) Transcatheter closure of secundum atrial defect in small children. Catheter Cardiovasc Interv 69(3):447–452
Chiaretti A, Ruggiero A, Barone G, Antonelli A, Lazzareschi I, Genovese O et al (2010) Propofol/alfentanil and propofol/ketamine procedural sedation in children with acute lymphoblastic leukaemia: safety, efficacy and their correlation with pain neuromediator expression. Eur J Cancer Care (Engl) 19(2):212–220
Chiaretti A, Ruggiero A, Barbi E, Pierri F, Maurizi P, Fantacci C et al (2011) Comparison of propofol versus propofol-ketamine combination in pediatric oncologic procedures performed by non-anesthesiologists. Pediatr Blood Cancer 57(7):1163–1167
Cravero JP, Beach ML, Blike GT, Gallagher SM, Hertzog JH (2009) The incidence and nature of adverse events during pediatric sedation/anesthesia with propofol for procedures outside the operating room: a report from the Pediatric Sedation Research Consortium. Anesth Analg 108(3):795–804
Diab KA, Cao QL, Bacha EA, Hijazi ZM (2007) Device closure of atrial septal defects with the Amplatzer septal occluder: safety and outcome in infants. J Thorac Cardiovasc Surg 134(4):960–966
Du ZD, Hijazi ZM, Kleinman CS, Silverman NH, Larntz K (2002) Comparison between transcatheter and surgical closure of secundum atrial septal defect in children and adults: results of a multicenter nonrandomized trial. J Am Coll Cardiol 39(11):1836–1844
Eich C, Verhagen-Henning S, Roessler M, Cremer F, Cremer S, Strack M et al (2011) Low-dose S-ketamine added to propofol anesthesia for magnetic resonance imaging in children is safe and ensures faster recovery: a prospective evaluation. Paediatr Anaesth 21(2):176–178
Elitsur Y, Blankenship P, Lawrence Z (2000) Propofol sedation for endoscopic procedures in children. Endoscopy 32(10):788–791
Everett AD, Jennings J, Sibinga E, Owada C, Lim DS, Cheatham J et al (2009) Community use of the Amplatzer atrial septal defect occluder: results of the multicenter MAGIC atrial septal defect study. Pediatr Cardiol 30(3):240–247
Formigari R, Di Donato RM, Mazzera E, Carotti A, Rinelli G, Parisi F et al (2001) Minimally invasive or interventional repair of atrial septal defects in children: experience in 171 cases and comparison with conventional strategies. J Am Coll Cardiol 37(6):1707–1712
Godambe SA, Elliot V, Matheny D, Pershad J (2003) Comparison of propofol/fentanyl versus ketamine/midazolam for brief orthopedic procedural sedation in a pediatric emergency department. Pediatrics 112(1 Pt 1):116–123
Gozal D, Rein AJ, Nir A, Gozal Y (2001) Propofol does not modify the hemodynamic status of children with intracardiac shunts undergoing cardiac catheterization. Pediatr Cardiol 22(6):488–490
Guenther E, Pribble CG, Junkins EP Jr, Kadish HA, Bassett KE, Nelson DS (2003) Propofol sedation by emergency physicians for elective pediatric outpatient procedures. Ann Emerg Med 42(6):783–791
Hasan RA, Reddy R (2009) Sedation with propofol for flexible bronchoscopy in children. Pediatr Pulmonol 44(4):373–378
Hasan RA, Shayevitz JR, Patel V (2003) Deep sedation with propofol for children undergoing ambulatory magnetic resonance imaging of the brain: experience from a pediatric intensive care unit. Pediatr Crit Care Med 4(4):454–458
Havel CJ Jr, Strait RT, Hennes H (1999) A clinical trial of propofol vs midazolam for procedural sedation in a pediatric emergency department. Acad Emerg Med 6(10):989–997
Hijazi ZM, Cao Q, Patel HT, Rhodes J, Hanlon KM (2000) Transesophageal echocardiographic results of catheter closure of atrial septal defect in children and adults using the Amplatzer device. Am J Cardiol 85(11):1387–1390
Hollman GA, Schultz MM, Eickhoff JC, Christenson DK (2008) Propofol-fentanyl versus propofol alone for lumbar puncture sedation in children with acute hematologic malignancies: propofol dosing and adverse events. Pediatr Crit Care Med 9(6):616–622
Hosey MT, Makin A, Jones RM, Gilchrist F, Carruthers M (2004) Propofol intravenous conscious sedation for anxious children in a specialist paediatric dentistry unit. Int J Paediatr Dent 14(1):2–8
Hughes ML, Maskell G, Goh TH, Wilkinson JL (2002) Prospective comparison of costs and short term health outcomes of surgical versus device closure of atrial septal defect in children. Heart 88(1):67–70
Kammache I, Mancini J, Ovaert C, Habib G, Fraisse A (2011) Feasibility of transcatheter closure in unselected patients with secundum atrial septal defect, using Amplatzer devices and a modified sizing balloon technique. Catheter Cardiovasc Interv 78(5):665–674
Kretschmar O, Sglimbea A, Daehnert I, Riede FT, Weiss M, Knirsch W (2010) Interventional closure of atrial septal defects with the Solysafe Septal Occluder: preliminary results in children. Int J Cardiol 143(3):373–377
Lightdale JR, Valim C, Newburg AR, Mahoney LB, Zgleszewski S, Fox VL (2008) Efficiency of propofol versus midazolam and fentanyl sedation at a pediatric teaching hospital: a prospective study. Gastrointest Endosc 67(7):1067–1075
Machata AM, Willschke H, Kabon B, Kettner SC, Marhofer P (2008) Propofol-based sedation regimen for infants and children undergoing ambulatory magnetic resonance imaging. Br J Anaesth 101(2):239–243
Mallory MD, Baxter AL, Kost SI (2009) Propofol vs pentobarbital for sedation of children undergoing magnetic resonance imaging: results from the Pediatric Sedation Research Consortium. Paediatr Anaesth 19(6):601–611
Mallory MD, Baxter AL, Yanosky DJ, Cravero JP (2011) Emergency physician-administered propofol sedation: a report on 25,433 sedations from the pediatric sedation research consortium. Ann Emerg Med 57(5):462–468 e461
Malviya S, Voepel-Lewis T, Tait AR (1997) Adverse events and risk factors associated with the sedation of children by nonanesthesiologists. Anesth Analg 85(6):1207–1213
Mart CR, Parrish M, Rosen KL, Dettorre MD, Ceneviva GD, Lucking SE et al (2006) Safety and efficacy of sedation with propofol for transoesophageal echocardiography in children in an outpatient setting. Cardiol Young 16(2):152–156
Pees C, Haas NA, Ewert P, Berger F, Lange PE (2003) Comparison of analgesic/sedative effect of racemic ketamine and S(+)-ketamine during cardiac catheterization in newborns and children. Pediatr Cardiol 24(5):424–429
Reinhold P, Graichen B (1999) Propofol for sedation in pediatric magnetic resonance imaging investigations. Klin Padiatr 211(1):40–43
Rossi RI, Cardoso Cde O, Machado PR, Francois LG, Horowitz ES, Sarmento-Leite R (2008) Transcatheter closure of atrial septal defect with Amplatzer device in children aged less than 10 years old: immediate and late follow-up. Catheter Cardiovasc Interv 71(2):231–236
Seigler RS, Avant MG, Gwyn DR, Lynch AL, Golding EM, Blackhurst DW et al (2001) A comparison of propofol and ketamine/midazolam for intravenous sedation of children. Pediatr Crit Care Med 2(1):20–23
Shah A, Mosdossy G, McLeod S, Lehnhardt K, Peddle M, Rieder M (2011) A blinded, randomized controlled trial to evaluate ketamine/propofol versus ketamine alone for procedural sedation in children. Ann Emerg Med 57(5):425–433422
Singh A, Girotra S, Mehta Y, Radhakrishnan S, Shrivastava S (2000) Total intravenous anesthesia with ketamine for pediatric interventional cardiac procedures. J Cardiothorac Vasc Anesth 14(1):36–39
Singh R, Batra YK, Bharti N, Panda NB (2010) Comparison of propofol versus propofol-ketamine combination for sedation during spinal anesthesia in children: randomized clinical trial of efficacy and safety. Paediatr Anaesth 20(5):439–444
Smith BG, Wilson N, Richens T, Knight WB (2008) Midterm follow-up of percutaneous closure of secundum atrial septal defect with Helex Septal Occluder. J Interv Cardiol 21(4):363–368
Srinivasan M, Turmelle M, Depalma LM, Mao J, Carlson DW (2012) Procedural sedation for diagnostic imaging in children by pediatric hospitalists using propofol: analysis of the nature, frequency, and predictors of adverse events and interventions. J Pediatr 160(5):801–806 e801
Tosun Z, Aksu R, Guler G, Esmaoglu A, Akin A, Aslan D et al (2007) Propofol-ketamine vs propofol-fentanyl for sedation during pediatric upper gastrointestinal endoscopy. Paediatr Anaesth 17(10):983–988
Tosun Z, Esmaoglu A, Coruh A (2008) Propofol-ketamine vs propofol-fentanyl combinations for deep sedation and analgesia in pediatric patients undergoing burn dressing changes. Paediatr Anaesth 18(1):43–47
Ulgey A, Aksu R, Bicer C, Akin A, Altuntas R, Esmaoglu A et al (2012) Is the addition of dexmedetomidine to a ketamine-propofol combination in pediatric cardiac catheterization sedation useful? Pediatr Cardiol 33(5):770–774
Vardi A, Salem Y, Padeh S, Paret G, Barzilay Z (2002) Is propofol safe for procedural sedation in children? A prospective evaluation of propofol versus ketamine in pediatric critical care. Crit Care Med 30(6):1231–1236
Vogel M, Berger F, Dahnert I, Ewert P, Lange PE (2000) Treatment of atrial septal defects in symptomatic children aged less than 2 years of age using the Amplatzer septal occluder. Cardiol Young 10(5):534–537
Weiss M, Frei M, Buehrer S, Feurer R, Goitein G, Timmermann B (2007) Deep propofol sedation for vacuum-assisted bite-block immobilization in children undergoing proton radiation therapy of cranial tumors. Paediatr Anaesth 17(9):867–873
Wheeler DS, Vaux KK, Ponaman ML, Poss BW (2003) The safe and effective use of propofol sedation in children undergoing diagnostic and therapeutic procedures: experience in a pediatric ICU and a review of the literature. Pediatr Emerg Care 19(6):385–392
Williams GD, Jones TK, Hanson KA, Morray JP (1999) The hemodynamic effects of propofol in children with congenital heart disease. Anesth Analg 89(6):1411–1416
Wilson NJ, Smith J, Prommete B, O’Donnell C, Gentles TL, Ruygrok PN (2008) Transcatheter closure of secundum atrial septal defects with the Amplatzer septal occluder in adults and children-follow-up closure rates, degree of mitral regurgitation and evolution of arrhythmias. Heart Lung Circ 17(4):318–324
Zanaboni S, Krauss B, Buscaglia R, Montagnini C, Gratarola A, Gualino J et al (2007) Changes in respiratory and hemodynamic parameters during low-dose propofol sedation in combination with regional anesthesia for herniorrhaphy and genitourinary surgery in children. Paediatr Anaesth 17(10):934–941
Conflict of interest
Nikolaus A. Haas works as proctor for interventional ASD closure for AGA Medical, Occlutech GmbH, and NMT Medical, Inc.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hanslik, A., Moysich, A., Laser, K.T. et al. Percutaneous Closure of Atrial Septal Defects in Spontaneously Breathing Children Under Deep Sedation: A Feasible and Safe Concept. Pediatr Cardiol 35, 215–222 (2014). https://doi.org/10.1007/s00246-013-0762-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-013-0762-9