Abstract
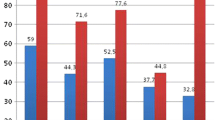
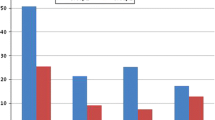
The aim of this study was to analyze the presence of lithogenic metabolic factors in the blood and urine of patients with osteopenia versus osteoporosis. This is a cross-sectional study including 67 patients who were divided into two groups according to the presence of either osteopenia or osteoporosis as measured by bone densitometry: group 1—40 patients with osteopenia (22 men and 18 women) and group 2—27 patients with osteoporosis (13 men and 14 women). Metabolic studies were performed on the blood and urine; statistical analysis was performed comparing means and conducting linear correlation and multivariate analyses with SPSS. Statistical significance was considered to be p ≤ 0.05. The mean age of patients in group 1 was 52.9 ± 12.8 years versus 50.3 ± 11.4 in group 2; the difference was not statistically significant. In group 2, higher levels of osteocalcin, β-crosslaps, urinary calcium, fasting urine calcium/creatinine, 24 h urine calcium/creatinine and 24 h oxaluria were observed compared to group 1. In the multivariate analysis, only the β-crosslaps and urinary calcium were independently associated with osteoporosis. It would be advisable to determine the urinary calcium levels in patients with osteoporosis since altered levels may necessitate modifying the diagnostic and therapeutic approach to osteoporosis.


Similar content being viewed by others
References
Olszynski WP, Shawn Davison K, Adachi JD, Brown JP, Cummings SR, Hanley DA, Harris SP, Hodsman AB, Kendler D, McClung MR, Miller PD, Yuen CK (2004) Osteoporosis in men: epidemiology, diagnosis, prevention, and treatment. Clin Ther 26:15–28
Gielen E, Vanderschueren D, Callewaert F, Boonen S (2011) Osteoporosis in men. Best Pract Res Clin Endocrinol Metab. 25:321–335
Painter SE, Kleerekoper M, Camacho PM (2006) Secondary osteoporosis: a review of the recent evidence. Endocr Pract. 12:436–445
Hudec SM, Camacho PM (2013) Secondary causes of osteoporosis. Endocr Pract 19:120–128
Polymeris A, Michalakis K, Sarantopoulou V (2013) Secondary osteoporosis—an endocrinological approach focusing on underlying mechanisms. Endocr Regul. 47:137–148
Arrabal Martín M, Fernández Rodríguez A, Arrabal Polo MA, Ruíz García MJ, Zuluaga Gómez A (2006) Study of the physical-chemical factors in patients with renal lithiasis. Arch Esp Urol 59:583–594
Audran M, Legrand E (2000) Hypercalciuria. Joint Bone Spine. 67:509–515
Arrabal-Polo MA, del Carmen Cano-García M, Canales BK, Arrabal-Martín M (2014) Calcium nephrolithiasis and bone demineralization: pathophysiology, diagnosis, and medical management. Curr Opin Urol 24:633–638
Zerwekh JE (2010) Bone disease and hypercalciuria in children. Pediatr Nephrol 25:395–401
Skalova S, Palicka V, Kutilek S (2005) Bone mineral density and urinary N-acetyl-beta-D-glucosaminidase activity in paediatric patients with idiopathic hypercalciuria. Nephrology (Carlton) 10:99–102
Penido MG, Lima EM, Marino VS, Tupinambá AL, França A, Souto MF (2003) Bone alterations in children with idiopathic hypercalciuria at the time of diagnosis. Pediatr Nephrol 18:133–139
Ryan LE, Ing SW (2012) Idiopathic hypercalciuria and bone health. Curr Osteoporos Rep. 10:286–295
Bilić-Curcić I, Milas-Ahić J, Smolić M, Smolić R, Mihaljević I, Tucak-Zorić S (2009) Urolithiasis and osteoporosis: clinical relevance and therapeutic implications. Coll Antropol. 33(Suppl 2):189–192
Ryan CS, Petkov VI, Adler RA (2011) Osteoporosis in men: the value of laboratory testing. Osteoporos Int 22:1845–1853
Cerdà D, Peris P, Monegal A, Albaladejo C, Martínez de Osaba MJ, Surís X, Guañabens N (2011) Increase of PTH in post-menopausal osteoporosis. Rev Clin Esp 211:338–343
Peris P, Ruiz-Esquide V, Monegal A, Alvarez L, Martínez de Osaba MJ, Martínez-Ferrer A, Reyes R, Guañabens N (2008) Idiopathic osteoporosis in premenopausal women. Clinical characteristics and bone remodelling abnormalities. Clin Exp Rheumatol 26:986–991
Odabasi E, Turan M, Tekbas F, Kutlu M (2009) Evaluation of secondary causes that may lead to bone loss in women with osteoporosis: a retrospective study. Arch Gynecol Obstet 279:863–867
Carvalho M, Kulak CA, Borba VZ (2012) Prevalence of hypercalciuria in postmenopausal women with osteoporosis. Arq Bras Endocrinol Metabol. 56:1–5
Odvina CV, Poindexter JR, Peterson RD, Zerwekh JE, Pak CY (2008) Intestinal hyperabsorption of calcium and low bone turnover in hypercalciuric postmenopausal osteoporosis. Urol Res 36:233–239
Acknowledgments
This article is a part of doctoral thesis by Maria Sierra Girón-Prieto in the Doctorado of Medicina Clinica and Salud Publica. Granada University. This investigation has been funded by Fundacion Progreso y Salud. Consejeria de Salud. Junta de Andalucia. Pi 0766/2013.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical statement
It is a low ethically responsible study in which the patients gave their informed consent after reading the Patient Information Sheet. The study was approved by the Hospital Ethics Committee.
Conflict of interest
The authors have no conflicts of interest to report.
Rights and permissions
About this article
Cite this article
Girón-Prieto, M.S., del Carmen Cano-García, M., Poyatos-Andújar, A. et al. The value of hypercalciuria in patients with osteopenia versus osteoporosis. Urolithiasis 45, 279–283 (2017). https://doi.org/10.1007/s00240-016-0909-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00240-016-0909-2