Abstract
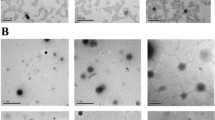
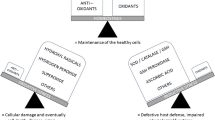
Although there is an ongoing controversy about the primary site of calcium oxalate stone (CaOx) formation, there is some evidence for extratubular crystallization. However, the mechanisms leading to such interstitial calcifications are not clear. Anatomical studies have demonstrated a close association between the renal vasculature and renal tubules. It has been hypothesized that disorders of the vasculature may contribute to renal stone formation. The exceptional papillary environment with low oxygen and high carbon dioxide is of interest in this context and its impact on CaOx toxicity to renal cells has to be evaluated. LLC-PK1, Madin-Darby canine kidney (MDCK), human umbilical vein endothelial (HUVEC) and fibroblast cell lines were exposed to hypoxia (3% O2) alone, hypercapnia combined with hypoxia (3% O2, 18% CO2) or standard culture conditions (20% O2) for 72 h. Cell survival rates were determined microscopically after 4 h of incubation with CaOx at final concentrations of 1, 2 and 4 mM. DAPI staining and western blot were used to evaluate the induction of apoptosis. We confirmed that CaOx leads to concentration-dependent effects on the viability of the cell lines. HUVECs were most vulnerable to CaOx among the four cell lines. Incubation under hypoxia alone had no impact on CaOx toxicity to any of the cell lines in terms of survival. However, under combined hypoxic and hypercapnic conditions, all cell lines displayed a significant reduction of cell survival compared to room air incubation. Again, this effect was most pronounced for HUVECs. The induction of apoptosis could not be demonstrated in any experimental setting. Combined hypoxia and hypercapnia clearly aggravate CaOx toxicity to renal cell lines. As we could not demonstrate the induction of apoptosis, this effect may be a result of toxic necrosis. Especially the CaOx effect on interstitial cell lines might be of interest in the chronic ischemic papillary environment. An increased toxicity may lead to recurrent stone formation, and vice versa, diseases of the vasculature, like arteriosclerosis, may further promote stone formation by induction of local ischemia. This issue has to be clarified by further studies.





Similar content being viewed by others
References
Strohmaier WL (2000) Course of calcium oxalate disease without treatment. What can we expect? Eur Urol 37:339–344
Verkoelen CF, Schepers MS (2000) Changing concepts in the aetiology of renal stones. Curr Opin Urol 10:539–544
Coe FL, Evan A, Worcester E (2005) Kidney stone disease. J Clin Invest 115:2598–2608
Lieske JC, Deganello S (1999) Nucleation, adhesion, and internalization of calcium-containing urinary crystals by renal cells. J Am Soc Nephrol 10(Suppl 14):S422–S429
Pak CY (1991) Etiology and treatment of urolithiasis. Am J Kidney Dis 18:624–637
Cifuentes Delatte L, Minon-Cifuentes J, Medina JA (1987) New studies on papillary calculi. J Urol 137:1024–1029
Finlayson B (1978) Physicochemical aspects of urolithiasis. Kidney Int 13:344–360
Baumann JM (1998) Stone prevention: why so little progress? Urol Res 26:77–81
Verkoelen CF, Van der Boom BG, Houtsmuller AB, Schroder FH, Romijn JC (1998) Increased calcium oxalate crystal binding to injured renal tubular epithelial cells in culture. Am J Physiol 274:F958–F965
Khan SR, Byer KJ, Thamiselvan S, Hackett RL, McCormack WT, Benson NA, Vaughn HL, Erdos GW (1999) Crystal-cell interaction and apoptosis in oxalate-associated injury of renal epithelial cells. J Am Soc Nephrol 10(Suppl):S457–S463
Evan AP, Lingeman JE, Coe FL, Parks JH, Bledsoe SB, Shao Y, Sommer AJ, Paterson RF, Kuo RL, Grynpas M (2003) Randall’s plaque of patients with nephrolithiasis begins in basement membranes of thin loops of Henle. J Clin Invest 111:607–616
Randall A (1937) The origin and growth of renal calculi. Ann Surg 105:1009–1027
Knoll T, Steidler A, Trojan L, Sagi S, Schaaf A, Yard B, Michel MS, Alken P (2004) The influence of oxalate on renal epithelial and interstitial cells. Urol Res 32:304–309
Stoller ML, Meng MV, Abrahams HM, Kane JP (2004) The primary stone event: a new hypothesis involving a vascular etiology. J Urol 171:1920–1924
Zhang W, Edwards A (2002) Oxygen transport across vasa recta in the renal medulla. Am J Physiol Heart Circ Physiol 283:H1042–H1055
Randall A (1940) Papillary pathology as a precursor of primary renal calculus. J Urol 44:580–589
Kok DJ (1996) Crystallization and stone formation inside the nephron. Scanning Microsc 10:471–484
Nakatani T, Ishii K, Sugimoto T, Kamikawa S, Yamamoto K, Yoneda Y, Kanazawa T, Kishimoto T (2003) Concentration gradient of oxalate from cortex to papilla in rat kidney. Int J Urol 10:86–89
Sampaio FJB, Aragao AHM (1990) Anatomical relationship between the intrarenal arteries and the kidney collecting system. J Urol 143:679–681
Sampaio FJB, Aragao AHM (1990) Anatomical relationship between the renal venous arrangement and the kidney collecting system. J Urol 144:1089–1093
Kim HH, Kwak J, Jeong BC, Kim SW (2002) Effect of oxalate on the growth of renal tubular epithelial cells. J Endourol 16:261–264
Thamilselvan S, Byer KJ, Hackett RL, Khan SR (2000) Free radical scavengers, catalase and superoxide dismutase provide protection from oxalate-associated injury to LLC-PK1 and MDCk cells. J Urol 164:224–229
Hackett RL, Shevock PN, Khan SR (1995) Alteration in MDCK and LLC-PK1 cells exposed to oxalate and calcium oxalate monohydrate crystals. Scanning Microsc 9:587–596
Hsieh N, Shih CH, Chen HY, Wu MC, Chen WC, Li CW (2003) Effects of Tamm-Horsfall protein on the protection of MDCK cells form oxalate induced free radical injury. Urol Res 31:10–16
Werness PG, Brown CM, Smith LH, Finlayson B (1985) EQUIL2: a BASIC computer program for the calculation of urinary saturation. J Urol 134:1242–1244
Miller C, Kennington L, Cooney R, Kohjimoto Y, Cao LC, Honeyman T, Pullman J, Jonassen J, Scheid C (2000) Oxalate toxicity in renal epithelial cells: characteristics of apoptosis and necrosis. Toxicol Appl Pharmacol 162:132–141
Saikumar P, Venkatachalam MA (2003) Role of apoptosis in hypoxic/ischemic damage in the kidney. Semin Nephrol 23:511–521
Schumer M, Colombel MC, Sawczuk IS, Gobe G, Connor J, O’Toole KM, Olsson CA, Wise GJ, Buttyan R (1992) Morphologic, biochemical, and molecular evidence of apoptosis during the reperfusion phase after brief periods of renal ischemia. Am J Pathol 140:831–838
Iwata M, Myerson D, Torok-Storb B, Zager RA (1994) An evaluation of renal tubular DNA laddering in response to oxygen deprivation and oxidant injury. J Am Soc Nephrol 5:1307–1313
Allen J, Winterford C, Axelsen RA, Gobe GC (1992) Effects of hypoxia on morphological and biochemical characteristics of renal epithelial cell and tubule cultures. Ren Fail 14:453–460
Hagar H, Ueda N, Shah SV (1996) Endonuclease induced DNA damage and cell death in chemical hypoxic injury to LLC-PK cells. Kidney Int 49:355–361
Wiegele G, Brandis M, Zimmerhackl LB (1998) Apoptosis and necrosis during ischemia in renal tubular cells (LLC-PK1 and MDCK). Nephrol Dial Transplant 13:1158–1167
Jiang H, Guo R, Powell-Coffman A (2001) The Caenorhabditis elegans hif-1 gene encodes a bHLH-PAS protein that is required for adaptation to hypoxia. Proc Natl Acad Sci USA 98:7916–7921
Lopez-Ramos JC, Martinez-Romero R, Molina F, Canuelo A, Martinez-Lara E, Siles E, Peinado MA (2005) Evidence of a decrease in nitric oxide-storage molecules following acute hypoxia and/or hypobaria, by means of chemiluminescence analysis. Nitric Oxide 13:62–67
Chandra A, Angle N (2005) Vascular endothelial growth factor stimulates a novel calcium-signaling pathway in vascular smooth muscle cells. Surgery 138:780–787
Eng E, Holgren C, Hubchak S, Naaz P, Schnaper HW (2005) Hypoxia regulates PDGF-B interactions between glomerular capillary endothelial and mesangial cells. Kidney Int 68:695–703
Pettersen EO, Larsen LH, Ramsing NB, Ebbesen P (2005) Pericellular oxygen depletion during ordinary tissue culturing, measured with oxygen microsensors. Cell Prolif 38:257–267
Acknowledgements
The authors wish to thank Dr. C. Weiss, Institute for Medical Biometrics, Mannheim University Hospital, Germany, for her valuable assistance in the data calculation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cao, Y., Sagi, S., Häcker, A. et al. Impact of hypoxia and hypercapnia on calcium oxalate toxicity in renal epithelial and interstitial cells. Urol Res 34, 271–276 (2006). https://doi.org/10.1007/s00240-006-0055-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00240-006-0055-3