Abstract
Background
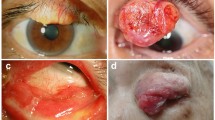
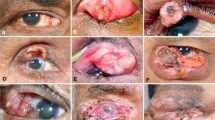
Eyelid sebaceous carcinoma is an uncommon aggressive cancer its capacity to cause serious harm and death underscores the significance of prompt identification and treatment. This study aims to evaluate the demographic, clinical, and pathological factors that impact the prognosis and survival of individuals with eyelid sebaceous carcinoma.
Methods
The data for this study was abstracted from the Surveillance, Epidemiology, and End Results (SEER) database from 2000–2018. The demographic and clinical data included several parameters, such as age, race, tumor grade, tumor size, surgical treatment, radiotherapy, chemotherapy, overall survival, and survival with specific treatments. The proportional hazard regression model was employed in this study to calculate hazard ratios and ascertain independent factors affecting survival outcomes. Data points with unidentified or missing values were excluded from the multivariate analysis to ensure robustness.
Results
A total 0f 903 of sebaceous carcinomas were extracted from the database. The mean age was 71.7 years and the majority (83.2%) were over 60 years old with a slight predominance of women (56.7%). Race was known for (96.6%) of cases, with White being the most dominant (86.6%) followed by Asian or Pacific Islander (10.2%). When tumor grade was known, poorly differentiated accounted for the majority (53.1%). Most cases with known tumor size were > 10 mm (44.9%). Where metastasis status was known, no metastasis was found in (99.2%). Most patients (80.2%) were treated with surgery alone. Being White and male had a better 5-year survival of 93.9% with a 95% confidence interval (C.I 95%) (C.I 95%, 61.3–99.0) and 95.3% (C.I 95%, 91.3–97.4) respectively. Multivariable analysis identified tumor size > 10 mm and age > 60 as independent risk factors for mortality (p < 0.010).
Conclusions
Our study found that old age and large tumor size are negative prognostic factors. Future research should target novel molecular targets and effective combination therapies to improve patient outcomes.
Level of evidence: Level III, Therapeutic; Diagnostic; Risk/Prognostic



Similar content being viewed by others
Data availability
Data is available on appropriate request from corresponding author.
References
Tripathi R, Chen Z, Li L, Bordeaux JS (2016) Incidence and survival of sebaceous carcinoma in the United States. J Am Acad Dermatol 75(6):1210–1215. https://doi.org/10.1016/j.jaad.2016.07.0462
Shields JA, Saktanasate J, Lally SE, Carrasco JR, Shields CL (2015) Sebaceous carcinoma of the ocular region: the 2014 professor winifred mao lecture. Asia Pac J Ophthalmol (Phila) 4(4):221–227. https://doi.org/10.1097/APO.00000000000001053
Shields JA, Demirci H, Marr BP, Eagle RC Jr, Shields CL (2005) Sebaceous carcinoma of the ocular region: a review. Surv Ophthalmol 50(2):103–122
Muqit MM, Foot B, Walters SJ, Mudhar HS, Roberts F, Rennie IG (2013) Observational prospective cohort study of patients with newly-diagnosed ocular sebaceous carcinoma. Br J Ophthalmol 97(1):47–51. https://doi.org/10.1136/bjophthalmol-2012-302443
Sargen MR, Mai ZM, Engels EA, Goldstein AM, Tucker MA, Pfeiffer RM et al (2020) Ambient ultraviolet radiation and sebaceous carcinoma incidence in the United States, 2000–2016. JNCI Cancer Spectr 4(2):pkaa020. https://doi.org/10.1093/jncics/pkaa020
Hussain RM, Matthews JL, Dubovy SR, Thompson JM, Wang G (2014) UV-independent p53 mutations in sebaceous carcinoma of the eyelid. Ophthalmic Plast Reconstr Surg 30(5):392–395. https://doi.org/10.1097/IOP.0000000000000121
Rajan KdA, Burris C, Iliff N, Grant M, Eshleman JR, Eberhart CG (2014) DNA mismatch repair defects and microsatellite instability status in periocular sebaceous carcinoma. Am J Ophthalmol 157(3):640–7.e72. https://doi.org/10.1016/j.ajo.2013.12.002
North JP, Golovato J, Vaske CJ, Sanborn JZ, Nguyen A, Wu W et al (2018) Cell of origin and mutation pattern define three clinically distinct classes of sebaceous carcinoma. Nat Commun 9(1):1894. https://doi.org/10.1038/s41467-018-04008-y.PMID:29760388;PMCID:PMC5951856
Dores GM, Curtis RE, Toro JR, Devesa SS, Fraumeni JF Jr (2008) Incidence of cutaneous sebaceous carcinoma and risk of associated neoplasms: insight into Muir-Torre syndrome. Cancer 113(12):3372–3381. https://doi.org/10.1002/cncr.23963
Owen JL, Kibbi N, Worley B, Kelm RC, Wang JV, Barker CA et al (2019) Sebaceous carcinoma: evidence-based clinical practice guidelines. Lancet Oncol 20(12):e699–e714. https://doi.org/10.1016/S1470-2045(19)30673-4
Flux K (2017) Sebaceous neoplasms. Surg Pathol Clin 10(2):367–382. https://doi.org/10.1016/j.path.2017.01.009
Grossniklaus HE, Eberhart CG, Kivela TT (2018) WHO classification of tumours of the eye, 4th edn. World Health Organization Classification of Tumours. International Agency for Research on Cancer, Lyon
Knackstedt T, Samie FH (2017) Sebaceous carcinoma: a review of the scientific literature. Curr Treat Options Oncol 18(8):47. https://doi.org/10.1007/s11864-017-0490-0
Cicinelli MV, Kaliki S (2019) Ocular sebaceous gland carcinoma: an update of the literature. Int Ophthalmol 39(5):1187–1197. https://doi.org/10.1007/s10792-018-0925-z
Phan K, Loya A (2019) Mohs micrographic surgery versus wide local excision for sebaceous adenocarcinoma of the eyelid : Analysis of a national database. J Plast Reconstr Aesthet Surg 72(6):1007–1011
Husain A, Blumenschein G, Esmaeli B (2008) Treatment and outcomes for metastatic sebaceous cell carcinoma of the eyelid. Int J Dermatol 47(3):276–279
Goto H, Tsubota K, Nemoto R, Ueda S, Umazume K, Usui Y et al (2020) Clinical features and prognosis of sebaceous carcinoma arising in the eyelid or conjunctiva. Jpn J Ophthalmol 64(5):549–554. https://doi.org/10.1007/s10384-020-00756-x
Zürcher M, Hintschich CR, Garner A, Bunce C, Collin JR (1998) Sebaceous carcinoma of the eyelid: a clinicopathological study. Br J Ophthalmol 82(9):1049–1055. https://doi.org/10.1136/bjo.82.9.1049
Shields JA, Demirci H, Marr BP, Eagle RC Jr, Shields CL (2004) Sebaceous carcinoma of the eyelids: personal experience with 60 cases. Ophthalmology 111(12):2151–2157. https://doi.org/10.1016/j.ophtha.2004.07.031
Callahan EF, Appert DL, Roenigk RK, Bartley GB (2004) Sebaceous carcinoma of the eyelid: a review of 14 cases. Dermatol Surg 30(8):1164–1168. https://doi.org/10.1111/j.1524-4725.2004.30348.x
Hou JL, Killian JM, Baum CL, Otley CC, Roenigk RK, Arpey CJ et al (2014) Characteristics of sebaceous carcinoma and early outcomes of treatment using Mohs micrographic surgery versus wide local excision: an update of the Mayo Clinic experience over the past 2 decades. Dermatol Surg 40(3):241–246. https://doi.org/10.1111/dsu.12433
Spencer JM, Nossa R, Tse DT, Sequeira M (2001) Sebaceous carcinoma of the eyelid treated with Mohs micrographic surgery. J Am Acad Dermatol 44(6):1004–1009. https://doi.org/10.1067/mjd.2001.113692
Takagawa Y, Tamaki W, Suzuki S, Inaba K, Murakami N, Takahashi K et al (2019) Radiotherapy for localized sebaceous carcinoma of the eyelid: a retrospective analysis of 83 patients. J Radiat Res 60(5):622–629. https://doi.org/10.1093/jrr/rrz046
Hata M, Koike I, Omura M, Maegawa J, Ogino I, Inoue T (2012) Noninvasive and curative radiation therapy for sebaceous carcinoma of the eyelid. Int J Radiat Oncol Biol Phys 82(2):605–611. https://doi.org/10.1016/j.ijrobp.2010.12.006
Yin VT, Merritt HA, Sniegowski M, Esmaeli B (2015) Eyelid and ocular surface carcinoma: diagnosis and management. Clin Dermatol 33(2):159–69. https://doi.org/10.1016/j.clindermatol.2014.10.008
Sa HS, Rubin ML, Xu S, Ning J, Tetzlaff M, Sagiv O et al (2019) Prognostic factors for local recurrence, metastasis and survival for sebaceous carcinoma of the eyelid: observations in 100 patients. Br J Ophthalmol 103(7):980–984. https://doi.org/10.1136/bjophthalmol-2018-312635
Ponti G, de Leon MP (2005) Muir-Torre syndrome. Lancet Oncol 6(12):980–987
Cohen PR, Kohn R, Kurzrock R (1991) Association of sebaceous gland tumors and internal malignancy: the Muir-Torre syndrome. Am J Med 90(5):606–613
Gaskin BJ, Fernando BS, Sullivan CA, Whitehead K, Sullivan TJ (2011) The significance of DNA mismatch repair genes in the diagnosis and management of periocular sebaceous cell carcinoma and Muir-Torre syndrome. Br J Ophthalmol 95(12):1686–1690. https://doi.org/10.1136/bjophthalmol-2011-300612
Kwon MJ, Nam ES, Cho SJ, Park HR, Min SK, Seo J et al (2017) Mutation analysis of CTNNB1 gene and the ras pathway genes KRAS, NRAS, BRAF, and PIK3CA in eyelid sebaceous carcinomas. Pathol Res Pract 213(6):654–658. https://doi.org/10.1016/j.prp.2017.02.015
Kodama T, Hayasaka S, Setogawa T (1995) Immunohistochemical localization of epidermal growth factor receptor and epithelial antigen in tumors of the human conjunctiva, eyelid, lacrimal gland, and orbit. Graefes Arch Clin Exp Ophthalmol 233:672–676
Yin VT, Merritt H, Esmaeli B (2014) Targeting EGFR and sonic hedgehog pathways for locally advanced eyelid and periocular carcinomas. World J Clin Cases 2(9):432–438
Domingo-Musibay E, Murugan P, Giubellino A, Sharma S, Steinberger D, Yuan J, Hunt MA, Lou E, Miller JS (2018) Near complete response to Pembrolizumab in microsatellite-stable metastatic sebaceous carcinoma. J Immunother Cancer 6(1):58. https://doi.org/10.1186/s40425-018-0357-3
Jayaraj P, Sen S (2019) Evaluation of PD-L1 and PD-1 expression in aggressive eyelid sebaceous gland carcinoma and its clinical significance. Indian J Ophthalmol 67(12):1983–1987
Funding
No funding has received for this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
The data of this manuscript is from SEER database which deidentified data from NCI and thus does not require IRB approval.
Conflict of interest
All the authors of this manuscript substantially contributed to this manuscript per ICMJE guidelines. Abdul Qahar Khan Yasinzai, Mya Goodbee, Jennifer Ahweyevu, Abdul Samad Khan Tareen, Hafeez Ullah, Muhammad Ayub Tareen, Abdul Waheed, Adil Karim, Dauod Arif, Marjan Khan, Luis Brandi, Asad Ullah declare no conflict of interest.
Patient consent
The data for this manuscript is obtained from SEER database which free available data from National Cancer Institute (NCI), USA. Thus patient consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Abdul Qahar Khan Yasinzai and Mya Goodbee equally contributed to this work and sharing for first coauthorship.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yasinzai, A.Q.K., Goodbee, M., Ahweyevu, J. et al. Sebaceous carcinoma of the eyelid: demographical analysis and role of surgery in the management. Eur J Plast Surg 46, 1011–1018 (2023). https://doi.org/10.1007/s00238-023-02137-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-023-02137-2