Abstract
Background
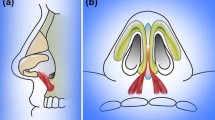
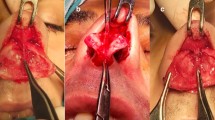
Rhinoplasty remains among the most challenging procedures to master, focusing on improving nasal appearance and/or function. Open tip rhinoplasty is performed in various methods, including sub- and supra-perichondrial rhinoplasty. This study aimed to compare the effects of sub- and supra-perichondrial rhinoplasty on nasalis muscle function using electromyography (EMG) and nerve conduction velocity (NCV).
Methods
Fifty women undergoing cosmetic rhinoplasty were enrolled in this prospective cohort and divided into sub-perichondrial and supra-perichondrial surgery groups. Pre- and two months post-operatively, nasal muscle function was evaluated by EMG and NCV in the two groups.
Results
This study was performed on 43 women aged 29 ± 4.1 years. Both surgeries significantly reduced almost all EMG and NCV parameters (P < 0.05). Still, there was no significant difference in the change of the EMG and NCV amplitude between the two groups (P > 0.05).
Conclusion
Sub- and supra-perichondrial open tip rhinoplasty temporarily reduce the nasal muscles’ function and change EMG and NCV parameters.
Level of evidence Level III, Risk/Prognostic.



Similar content being viewed by others
Data Availability
Data is available from the corresponding author upon reasonable request.
References
Kimura J (2013) Electrodiagnosis in diseases of nerve and muscle: principles and practice. Oxford University Press, Oxford
Neshat S, Daneii P, Neshat N et al (2021) Does cosmetic rhinoplasty affect sleep quality and/or contribute to the development of obstructive sleep apnea? CRANIO®. https://doi.org/10.1080/08869634.2021.1977900
Adamson PA (1987) Open rhinoplasty. Otolaryngol Clin North Am 20:837–852
Patron V, Hitier M, Gamby R et al (2019) How to perform subperichondrial and subperiosteal rhinoplasty. Eur Ann Otorhinolaryngol Head Neck Dis 136:325–329
Raggio BS, Asaria J (2019) Open rhinoplasty. StatPearls, Treasure Island
Cafferty A, Becker DG (2016) Open and closed rhinoplasty. Clin Plast Surg 43:17–27
Stewart MG, Smith TL, Weaver EM et al (2004) Outcomes after nasal septoplasty: results from the Nasal Obstruction Septoplasty Effectiveness (NOSE) study. Otolaryngol-Head Neck Surg 130:283–290
Gerbault O, Daniel RK, Kosins AM (2016) The role of piezoelectric instrumentation in rhinoplasty surgery. Aesthet Surg J 36:21–34
Cerkes N (2013) Concurrent elevation of the upper lateral cartilage perichondrium and nasal bone periosteum for management of dorsum: the perichondro-periosteal flap. Aesthet Surg J 33:899–914
Çakır B, Küçüker İ, Aksakal İA, Sağır HÖ (2017) Auto-rim flap technique for lateral crura caudal excess treatment. Aesthet Surg J 37:24–32. https://doi.org/10.1093/asj/sjw145
Çakır B, Öreroğlu AR, Doğan T, Akan M (2012) A complete subperichondrial dissection technique for rhinoplasty with management of the nasal ligaments. Aesthet Surg J 32:564–574
Neves JC, Zholtikov V, Cakir B et al (2021) Rhinoplasty dissection planes (subcutaneous, sub-SMAS, supra-perichondral, and sub-perichondral) and soft tissues management. Facial Plast Surg 37:2–11
Hassan Y, Leveille CF, Gallo L et al (2020) Reporting outcomes and outcome measures in open rhinoplasty: a systematic review. Aesthet Surg J 40:135–146
De Luca C (2006) Electromyography. Encyclopedia of medical devices and instrumentation. John Wiley Publisher, Hoboken
Stålberg E (1980) Macro EMG, a new recording technique. J Neurol Neurosurg Psychiatry 43:475–482
Garcia MAC, Vieira TMM (2011) Surface electromyography: why, when and how to use it. Rev Andal Med Deport 4:17–28
Zojaji R, Sobhani E, Meshkat M, Javanbakht M (2018) Quality of life after cosmetic rhinoplasty in Iran: a systematic review. J Fundam Mental Health 20:320–324
Sari AA, Babashahy S, Olyaeimanesh A, Rashidian A (2012) Estimating the frequency and rate of first 50 common types of invasive procedures in iran healthcare system. Iran J Public Health 41:60–64
Lam SM, Williams Iii EF (2002) Anatomic considerations in aesthetic rhinoplasty. Facial Plast Surg 18:209–214
Ozturan O, Ozcan C, Miman MC (2001) Intrinsic nasal muscles and their electromyographic evaluation after external septorhinoplasty. Otolaryngol Head Neck Surg 125:332–338
Zemek A, Garg R, Wong BJF (2010) Model for estimating the threshold mechanical stability of structural cartilage grafts used in rhinoplasty. Laryngoscope 120:1089–1093
Kırgezen T, Yigit O, Taskin U et al (2011) Electromyographic and electroneurographic changes in internal nasal muscles after endonasal and external rhinoplasty. Aesthet Surg J 31:297–301
Fattahi T (2008) Internal nasal valve: significance in nasal air flow. J Oral Maxillofac Surg 66:1921–1926
Vaiman M, Eviatar E, Segal S (2003) Intranasal electromyography in evaluation of the nasal valve. Rhinology 41:134–141
Batioglu-Karaaltin A, Karaaltin MV, Uzun N et al (2015) Effects of open technique rhinoplasty on mimicry: electroneurographic evaluation. J Craniofac Surg 26:1348–1351
Resuli AS, Ataus S (2020) Investigating the role of nasal muscles in nasal obstruction after open technique rhinoplasty: a case-control study by electromyographic evaluation. J Surg Med 4:207–211
Funding
None.
Author information
Authors and Affiliations
Contributions
All authors contributed considerably to this study. A.M. and N.Y. contributed to the study concept and design. K.M. contributed to material preparation, data collection, and data analysis. H.T. collected data and wrote the first draft of the manuscript. A.M. and N.Y. revised the manuscript. All authors read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki and approved by the Ethics Committee of Iran University of Medical Sciences (IR.IUMS.FMD.REC.1399.60).
Consent to participate
All patients provided written informed consent prior to their participation in the study.
Competing interests
Alireza Mohebi, Naseh Yousefi, Katayoon Moradi, and Hadis Tabatabaei declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mohebi, A., Yousefi, N., Moradi, K. et al. Nasal muscle function using electromyography (EMG) and nerve conduction velocity (NCV) in sub- and supra-perichondrial rhinoplasty. Eur J Plast Surg 46, 993–998 (2023). https://doi.org/10.1007/s00238-023-02114-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-023-02114-9