Abstract
Background
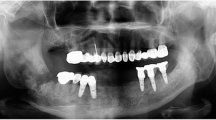
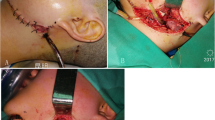
Excision for the ameloblastoma of the mandible and secondary cancer infiltration of the mandible are the most common causes of composite/compound lower jaw defects in our institute. The large post-excisional defects of the mandible challenge the prowess of the reconstructive surgeon. This study was conducted to evaluate the aesthetic and functional outcomes of microvascular reconstruction of large post-excisional defects of the mandible by using the chimeric double-barrel free fibula flap.
Methods
From March 2015 to March 2020, twenty-six patients, consisting of sixteen males and ten females, had undergone primary chimeric double-barrel free fibula flap reconstruction of post-excisional compound/composite defects of the mandible. There were sixteen patients with ameloblastoma and ten patients with infiltrating squamous cell carcinoma of the alveolus of the mandible-stage IVA. The average age of patients with ameloblastoma was 36.4 years, and those with squamous cell carcinoma (SCCA) were 51.3 years. All of them had undergone secondary dental rehabilitation at an average post-op period of 6 months. All patients with SCCA had adjuvant radiotherapy. All of them were followed for an average period of 16.5 months.
Results
Two patients (5%) had vascular insufficiency (one arterial and one venous thrombosis) but were successfully salvaged by early exploration and intervention. One patient (3.8%) had an infection of the reconstructed site, which was treated by infected mini plate removal and directive antibiotic therapy. One patient (3.8%) developed late hardware failure and fracture at the reconstructed site, which was treated conservatively and healed well. All of them had good to excellent functional and aesthetic outcome scores in the Institutional Computed Final Functional and Aesthetic Outcome Scoring system.
Conclusions
The chimeric double-barrel free fibula reconstruction not only provides a good contour in line with the lower border of the residuum lower jaw but also provides the well-vascularized bony stock for Osseo-integrated implants facilitating good functional and aesthetic outcomes. This may be added to the armamentarium of the plastic surgeon for large mandibuloplasties.
Level of evidence: Level IV, Therapeutic.










Similar content being viewed by others
References
Wang YY, Zhang HQ, Fan S, Zhang DM, Huang ZQ, Chen WL, Ye JT, Li JS (2016) Mandibular reconstruction with the vascularized fibula flap: comparison of virtual planning surgery and conventional surgery. Int J Oral Maxillofac Surg 45(11):1400–1405
He Y, Zhang ZY, Zhu HG, Wu YQ, Fu HH (2011) Double-barrel fibula vascularized free flap with dental rehabilitation for mandibular reconstruction. J Oral Maxillofac Surg 69(10):2663–2669
Fernandes R (2006) Fibula free flap in mandibular reconstruction. Atlas Oral Maxillofac Surg Clin North Am 14(2):143e150. https://doi.org/10.1016/j.cxom.2006.05.003
Takushima A, Harii K, Asato H, Nakatsuka T, Kimata Y (2001) Mandibular reconstruction using microvascular free flaps: a statistical analysis of 178 cases. Plast Reconstr Surg 108(6):1555e1563
Foster RD, Anthony JP, Sharma A, Pogrel MA (1999) Vascularized bone flaps versus no vascularized bone grafts for mandibular reconstruction: an outcome analysis of primary bony union and endosseous implant success. Head Neck 21(1):66e71
Pogrel MA, Podlesh S, Anthony JP, Alexander J (1997) A comparison of vascularized and no vascularized bone grafts for reconstruction of mandibular continuity defects. J Oral Maxillofac Surg 55(11):1200e1206
Gilbert A (1979) Vascularised transfer of the fibula shaft. Int J Microsurg 1:100–102
Jewer DD, Boyd JB, Manktelow RT, Zuker RM, Rosen IB, Gullane PJ et al (1989) Orofacial and mandibular reconstruction with the iliac crest free flap: a review of 60 cases and a new method of classification. Plast Reconstr Surg 84(3):391e403 (discussion 404e395)
Taylor GI, Miller GD, Ham FJ (1975) The free vascularized bone graft: a clinical extension of microvascular techniques. Plast Reconstr Surg 55:533
Hidalgo DA (1989) Fibula free flap: a new method of mandibular reconstruction. Plast Reconstr Surg 84:71–79
Chen ZW, Yan W (1983) The study and clinical application of the osteocutaneous flap of the fibula. Microsurgery 4(1):11e16
Serafin D, Villarreal-Rios A, Georgiade NG (1977) A rib containing free flap to reconstruct mandibular defects. Brit J Plast Surg 30:263–266
Taylor GI (1982) Reconstruction of the mandible with composite iliac bone grafts. Ann Plast Surg 9:361–376
Swartz WM, Banis JC, Newton ED et al (1986) The osteocutaneous scapular flap for mandibular and maxillary reconstruction. Plast Reconstr Surg 77:530–545
Soutar DS, Scheker LR, Tanner NSB, McGregor IA (1983) The radial forearm flap: a versatile method for intraoral reconstruction. Brit J Plast Surg 36:1–8
MacLeod AM, Robinson DW (1982) Reconstruction of mandible involving the mandible and floor of the mouth by free osteocutaneous flaps derived from the foot. Brit J Plast Surg 35:239–246
Horiuchi K, Hattori A, Inada I, Kamibayashi T, Sugimura M, Yajima H, Tamai S (1995) Mandibular reconstruction using the double barrel fibular graft. Microsurgery 16(7):450–454
Ortakoglu K, Suer BT, Ozyigit A et al (2006) Vertical distraction osteogenesis of fibula transplant for mandibular reconstruction: a case report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 102:e8
Bahr W, Stoll P, Wachter R (1998) Use of the “double barrel” free vascularized fibula in mandibular reconstruction. J Oral Maxillofac Surg 56:38
Salinas TJ, Desa VP, Katsnelson A et al (2010) Clinical evaluation of implants in radiated fibula flaps. J Oral Maxillofac Surg 68:524
Horiuchi K, Hattori A, Inada I et al (1995) Mandibular reconstruction using the double barrel fibula graft. Microsurgery 46:450
Yu Y, Zhang WB, Liu XJ, Guo CB, Yu GY, Peng X (2020) Double-barrel fibula flap versus vascularized iliac crest flap for mandibular reconstruction. J Oral Maxillofac Surg 78(5):844–850
Trilles J, Chaya BF, Daar DA, Anzai L, Boczar D, Rodriguez Colon R, Hirsch DL, Jacobson AS, Levine JP (2022) Double-barrel versus single-barrel fibula flaps for mandibular reconstruction: safety and outcomes. Laryngoscope 132(8):1576–1581
Massarelli O (2022) Chimeric LSMAP Double-barrel fibula free flap: goal-oriented surgical technique and tips for one-stage mandibular reconstruction. Plast Reconstr Surg Glob Open 10(1):e4040
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Institutional ethical committee approval was obtained for this clinical study (PLS 44/2015).
Conflict of interest
Balakrishnan Thalaivirithan Margabandu, Swetha Vedhanarayanan, Sethurajan Balasubramanian Sethurajan, and Jaganmohan Janardhanam declare no conflict of interest.
Patient consent
All patients recruited in this prospective cohort study had given their informed consent for both the surgical procedures and using the clinical data and photographs for research and publication purposes.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Margabandu, B.T., Vedhanarayanan, S., Sethurajan, S.B. et al. Aesthetic and functional outcomes of microvascular reconstruction of large post-excisional defects of the mandible by using the chimeric double-barrel free fibula flap. Eur J Plast Surg 46, 1027–1038 (2023). https://doi.org/10.1007/s00238-023-02101-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-023-02101-0