Abstract
Background
The number of performed deep inferior epigastric perforator (DIEP) flaps for post-mastectomy breast reconstructions (PMBR) has shown a dramatic increase over the past decade. As this increased demand requires a higher proportion of operative capacities worldwide, there is a need for increased efficiency. Introduction of lean strategies might form a solution. Therefore, the purpose of this study was to assess the effects and outcomes of practising lean strategies in DIEP flap surgery over six years by analysing operation time and complications.
Methods
In this retrospective cohort study, all patients who underwent a DIEP flap for PMBR between January 2013 and May 2019 were included. Patient- and surgery related characteristics were collected. Duration of surgery and complication rates were compared.
Results
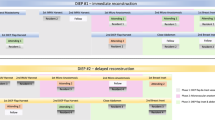
A total of 170 DIEP flaps for PMBR were performed in 139 patients. DIEP flaps were performed in an immediate (8 patients) or delayed (131 patients) setting. Mean operating time was 329 minutes for unilateral and 554 minutes for bilateral DIEP flap reconstruction. Over time, operating time decreased 19% in the unilateral, and 17.1% in the bilateral series. Also, more additional procedures during the initial DIEP flap procedure were performed over time. Total flap loss was seen in 1.2% of the cases. While surgical time decreased, the number of major complications decreased 9.3% in the unilateral and 20% in the bilateral series.
Conclusions
Using lean strategies can safely reduce surgical time in DIEP flap breast reconstructions, while achieving, a reduction of complications.
Level of evidence: Level IV, risk/prognostic study.


Similar content being viewed by others
References
Hofer SOP, Damen THC, Mureau MAM, Rakhorst HA, Roche NA (2007) A critical review of perioperative complications in 175 free deep inferior epigastric perforator flap breast reconstructions. Ann Plast Surg 59:137–142
Blondeel PN (1999) One hundred free DIEP flap breast reconstructions: a personal experience. Br J Plast Surg 52:104–111
Lindenblatt N, Gruenherz L, Farhadi J (2019) A systematic review of donor site aesthetic and complications after deep inferior epigastric perforator flap breast reconstruction. Gland Surg 8:389–398
Yueh JH, Slavin SA, Adesiyun T et al (2010) Patient satisfaction in postmastectomy breast reconstruction: A comparative evaluation of DIEP, TRAM, latissimus flap, and implant techniques. Plast Reconstr Surg 125:1585–1595
Grinsell DG, McCoubrey GW, Finkemeyer JP (2016) The deep inferior epigastric perforator learning curve in the current era. Ann Plast Surg 76:72–77
Ohno T, Norman B (1998) Toyota production system: beyond large-scale production, 1st edn. https://doi.org/10.4324/9780429273018
Busic V, Das-Gupta R, Mesic H, Begic A (2006) The deep inferior epigastric perforator flap for breast reconstruction, the learning curve explored. J Plast Reconstr Aesthetic Surg 59:580–584
Bodin F, Dissaux C, Lutz JC, Hendriks S, Fiquet C, Bruant-Rodier C (2015) The DIEP flap breast reconstruction: starting from scratch in a university hospital. Ann Chir Plast Esthet 60:171–178
Acosta R, Smit JM, Audolfsson T et al (2011) A clinical review of 9 years of free perforator flap breast reconstructions: an analysis of 675 flaps and the influence of new techniques on clinical practice. J Reconstr Microsurg 27:91–98
Sharma HR, Rozen WM, Mathur B, Ramakrishnan V (2019) 100 steps of a DIEP flap - a prospective comparative cohort series demonstrating the successful implementation of process mapping in microsurgery. Plast Reconstr Surg - Glob Open 7(1):e2006
Damen THC, Mureau MAM, Timman R, Rakhorst HA, Hofer SOP (2009) The pleasing end result after DIEP flap breast reconstruction: a review of additional operations. J Plast Reconstr Aesthetic Surg 62:71–76
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
The Dutch Healthcare Authority (2019) Declarations of microsurgical free flap reconstruction. www.opendisdata.nl. Accessed 10 Dec 2019
Gill PS, Hunt JP, Guerra AB et al (2004) A 10-year retrospective review of 758 DIEP flaps for breast reconstruction. Plast Reconstr Surg 113:1153–1160
Enajat M, Smit JM, Rozen WM et al (2010) Aesthetic refinements and reoperative procedures following 370 consecutive DIEP and SIEA flap breast reconstructions: important considerations for patient consent. Aesthetic Plast Surg 34:306–312
Dong J, Wang T, Zhang Y, Xu H, He J (2019) Staged immediate nipple reconstruction with tube flap in secondary autologous breast reconstruction. J Plast Surg Hand Surg 53:204–207
Pauchot J, Feuvrier D, Panouillères M, Pluvy I, Tropet Y (2015) Benefit of simultaneous contralateral breast symmetry procedure with unilateral breast reconstruction using DIEP flaps. About 33 cases. Ann Chir Plast Esthet. 60:472–477
Heathcote S, Duggan K, Rosbrugh J et al (2019) Enhanced recovery after surgery (ERAS) protocols expanded over multiple service lines improves patient care and hospital cost. Am Surg 85:1044–1050
Acknowledgements
Anaesthetists (A.J. Jansen; A.F. van der Meer), nurse practitioner (C. van Zuuren), theatre staff (P. Kammerman, T. Kruiper, R. Leis-Dorenbusch, M. Dosoe, M. Postmus-Folkes, G. Kouwenhoven-Voortman, R. van Ommen-Schipper, A. Aaldering, B. van der Horst), and nursing staff.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study was approved by the regional Medical Ethics Committee, registration no.: K20-15.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Patient consent
Patients signed informed consent regarding publishing their data.
Conflict of interest
Juliette E.D. Jacobs, Nikki Beudeker, Claudia A. Bargon, Sabine Siesling, Narda Hendriks-Brouwer, Oliver T. Zöphel, Ute Schmidbauer, Yvonne C.M.M. Smulders, Johan G. Wijbenga, and Hinne A. Rakhorst declare no conflict of interest. The authors alone are responsible for the content and writing of the paper.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jacobs, J.E.D., Beudeker, N., Bargon, C.A. et al. Lean DIEP flap surgery: saving time and reducing complications. Eur J Plast Surg 44, 793–800 (2021). https://doi.org/10.1007/s00238-021-01836-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00238-021-01836-y